In this comprehensive overview of MERS-CoV, you will gain a deeper understanding of this relatively new and highly contagious respiratory illness. From its origins to its symptoms and transmission, this article will provide you with all the essential information you need to know about MERS-CoV and how it has affected communities worldwide. So fasten your seatbelt and get ready to dive into the world of MERS-CoV, where knowledge is key to staying safe.
Overview of MERS-CoV
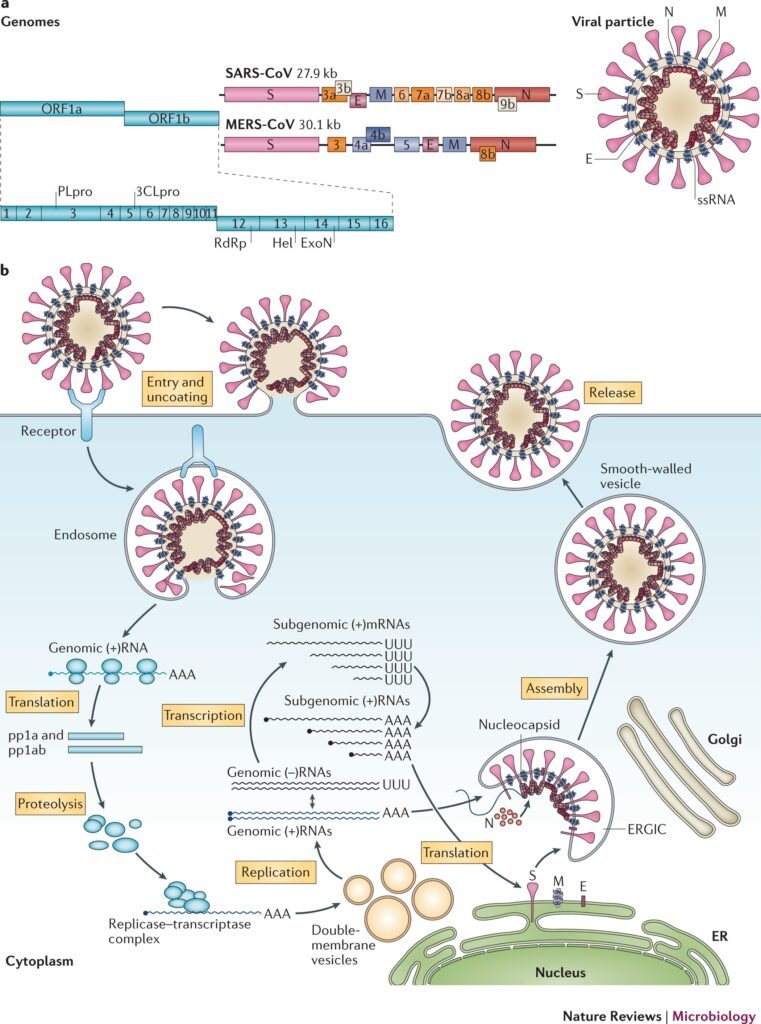
MERS-CoV, or Middle East Respiratory Syndrome Coronavirus, is a viral infection that was first identified in 2012 in Saudi Arabia. It belongs to the same family of viruses as the Severe Acute Respiratory Syndrome Coronavirus (SARS-CoV) and the more recent novel Coronavirus causing the COVID-19 pandemic. MERS-CoV is primarily transmitted from dromedary camels to humans, although limited human-to-human transmission has also been documented.
Definition and History of MERS-CoV
MERS-CoV is a highly contagious respiratory illness that can lead to severe respiratory distress and even death. The virus is believed to have originated in bats and was transmitted to camels, which then became a primary source of human infection. The first known case of MERS-CoV was reported in Saudi Arabia in 2012, and since then, sporadic cases and outbreaks have occurred primarily in the Middle East. However, cases have also been reported in other regions due to travel-related transmission.
Similarities and Differences between MERS-CoV and SARS-CoV
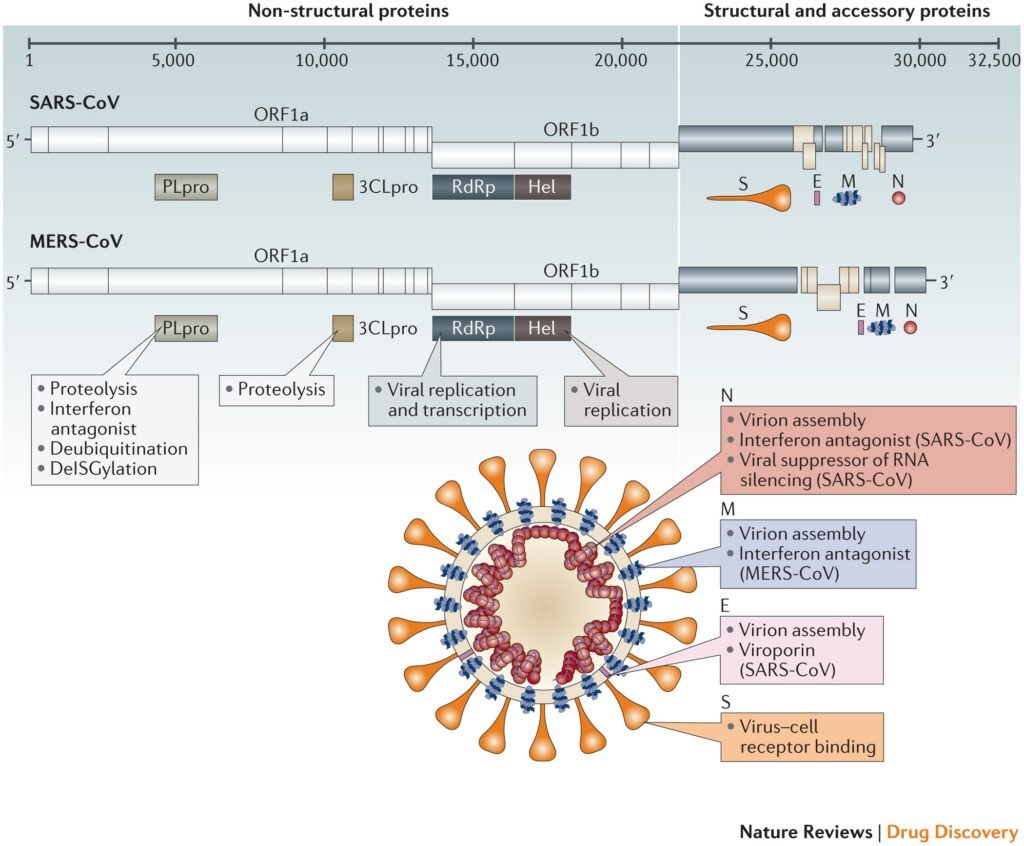
MERS-CoV and SARS-CoV share similarities in terms of their origins, as both viruses are believed to have originated in bats and crossed over to other animal species before infecting humans. However, there are some key differences between the two viruses. MERS-CoV has a higher fatality rate compared to SARS-CoV, but it is less easily transmitted between humans. Both viruses can cause severe respiratory illness, but MERS-CoV has a lower overall case count compared to SARS-CoV and COVID-19.
Global Prevalence of MERS-CoV
While MERS-CoV primarily affects countries in the Middle East, sporadic cases and outbreaks have also been reported in other regions due to travel-related transmission. As of the most recent data, over 2,500 laboratory-confirmed cases of MERS-CoV have been reported, with the majority occurring in Saudi Arabia. The global prevalence of MERS-CoV is relatively low compared to other viral respiratory illnesses, but it requires ongoing surveillance and public health measures to prevent its spread.
Transmission and Spread of MERS-CoV
Modes of Transmission
MERS-CoV is primarily transmitted from dromedary camels to humans through close contact or consumption of raw or undercooked camel products, such as milk or meat. Limited human-to-human transmission has been documented, primarily in healthcare settings and within households. The virus is mainly spread through respiratory droplets when an infected person coughs or sneezes, but it can also be transmitted through contact with contaminated surfaces.
Risk Factors for MERS-CoV Transmission
Certain factors increase the risk of MERS-CoV transmission. Direct exposure to camels or camel products, particularly in countries where the virus is prevalent, increases the risk of infection. Healthcare workers and individuals in close contact with MERS-CoV patients are also at a higher risk of transmission. Additionally, poor infection control practices and crowded environments can facilitate the spread of the virus.
Outbreaks and Pandemics
Although MERS-CoV outbreaks have occurred sporadically since its discovery, the virus has not caused a widespread pandemic like SARS-CoV or COVID-19. Most MERS-CoV outbreaks have been contained through effective public health measures, including surveillance, contact tracing, and isolation of cases. However, ongoing surveillance and preparedness efforts are crucial to prevent future outbreaks and ensure a prompt response if the virus evolves to become more transmissible.

Clinical Presentation and Symptoms
Incubation Period
The incubation period for MERS-CoV typically ranges from 2 to 14 days, with an average of 5-6 days. During this period, an infected individual may not exhibit any symptoms but can still transmit the virus to others, making early detection and isolation crucial in controlling its spread.
Common Symptoms
The symptoms of MERS-CoV infection can vary from mild to severe and may include fever, cough, shortness of breath, and muscle pain. Some individuals may also experience gastrointestinal symptoms such as diarrhea. In severe cases, MERS-CoV can lead to pneumonia and acute respiratory distress syndrome (ARDS), requiring intensive medical care.
Complications and Severe Cases
MERS-CoV infections can progress rapidly in certain individuals, particularly those with underlying health conditions such as diabetes, renal disease, or compromised immune systems. Severe cases of MERS-CoV can result in respiratory failure, organ failure, and death. The fatality rate for MERS-CoV is approximately 35%, but the actual mortality rate may be lower due to underreporting of mild cases.
Diagnosis and Laboratory Testing
MERS-CoV Testing Methods
Laboratory testing is essential for diagnosing MERS-CoV infection. The most common method is the real-time reverse transcription-polymerase chain reaction (RT-PCR) test, which detects the presence of viral RNA in respiratory samples. Serological testing, which looks for antibodies against MERS-CoV, can also be used to confirm prior infection. These tests are typically conducted in specialized laboratories approved for high-level containment.
Diagnostic Challenges and Limitations
Diagnosing MERS-CoV infection can be challenging due to the similarity of symptoms with other respiratory illnesses and the need for specialized laboratory testing. In addition, the availability of testing facilities may vary in different regions, leading to delays in diagnosis and potential underreporting of cases. To address these challenges, ongoing research and improvements in diagnostic technologies are needed.
Treatment and Management
Current Treatment Options
There is currently no specific antiviral treatment for MERS-CoV infection. Supportive care, including hydration, supplemental oxygen, and treatment of complications such as pneumonia, is the mainstay of management. In severe cases, patients may require hospitalization and intensive care support, including mechanical ventilation. Experimental antiviral therapies are being investigated, but their efficacy and safety are still under evaluation.
Supportive Care
Supportive care is crucial in managing MERS-CoV infection, particularly in severe cases. Maintaining hydration, providing respiratory support, and treating secondary infections are essential components of supportive care. Multidisciplinary teams involving healthcare professionals from various specialties work together to monitor and manage the symptoms and complications associated with MERS-CoV.
Experimental Therapies and Vaccines
Research is ongoing to develop effective therapies and vaccines for MERS-CoV. Several experimental antiviral drugs are being studied in clinical trials, aimed at inhibiting the replication of the virus or modulating the host immune response. Vaccine development efforts are also underway, with promising candidates in preclinical and early clinical stages. However, it will take time to determine their safety and efficacy before they can be made widely available.
Prevention and Control Measures
Infection Prevention Practices
The key to preventing MERS-CoV infection is practicing good hygiene and adopting infection prevention measures. These include regular handwashing with soap and water or using alcohol-based hand sanitizers, covering the mouth and nose with a tissue or elbow when coughing or sneezing, and avoiding close contact with sick individuals. Individuals at higher risk, such as healthcare workers and individuals in contact with camels, should take additional precautions.
Public Health Interventions
Public health interventions play a crucial role in preventing and controlling the spread of MERS-CoV. These include active surveillance of cases and contacts, contact tracing, isolation and quarantining of cases, and implementing appropriate infection control measures in healthcare settings. Public health authorities also provide guidance and resources to communities and healthcare professionals to ensure effective prevention and control of MERS-CoV.
Travel Advisories and Restrictions
International travel advisories and restrictions may be implemented in response to MERS-CoV outbreaks. These measures aim to reduce the risk of transmission across borders and prevent the introduction of the virus into new regions. Travelers to countries or areas with known MERS-CoV activity should stay updated with the latest travel advisories and follow recommended preventive measures to protect themselves and limit the spread of the virus.
Surveillance and Reporting
Global Surveillance Systems
Global surveillance systems are essential for monitoring the spread and impact of MERS-CoV. These systems enable the timely detection, reporting, and response to cases and outbreaks. International organizations, such as the World Health Organization (WHO), collaborate with member countries to enhance surveillance capacities and facilitate the sharing of information and best practices.
Case Reporting and Notification
Prompt and accurate case reporting and notification are crucial for effective disease control. Healthcare professionals and laboratories play a key role in reporting suspected or confirmed MERS-CoV cases to local health authorities. Timely reporting allows for early intervention, contact tracing, and implementation of appropriate public health measures to prevent further transmission and protect the community.
Data Collection and Analysis
Data collection and analysis are essential components of understanding the epidemiology and impact of MERS-CoV. Surveillance systems gather information on demographics, clinical characteristics, and outcomes of MERS-CoV cases. This data helps identify trends, assess the effectiveness of control measures, and inform public health policies and strategies.
Epidemiology and Public Health Implications
Epidemiological Patterns
MERS-CoV has shown a sporadic pattern of occurrence, with periodic outbreaks in countries primarily in the Middle East. The exact reasons for the sporadic nature of the virus are not fully understood. The majority of cases are reported in Saudi Arabia, with occasional cases and small outbreaks occurring in other countries due to travel-related transmission. Continuous surveillance and investigation are necessary to identify any changes in the epidemiology of MERS-CoV.
Mortality and Morbidity
MERS-CoV has a higher fatality rate compared to other respiratory viruses, with an estimated case fatality rate of around 35%. However, it is important to note that milder cases of MERS-CoV may be underreported, resulting in an overestimation of the fatality rate. Severe cases of MERS-CoV can lead to long-term complications and increased morbidity, particularly among individuals with underlying health conditions.
Social and Economic Impact
The social and economic impact of MERS-CoV extends beyond the health consequences. The fear of the virus and its potential to cause severe illness and death can disrupt communities, strain healthcare systems, and negatively affect local economies, particularly in countries heavily reliant on tourism. The implementation of effective prevention and control measures, along with public awareness campaigns, can help mitigate the social and economic impact of MERS-CoV.
One Health Approach in MERS-CoV
Link Between Animal and Human Health
The One Health approach recognizes the interconnectedness of human, animal, and environmental health. In the case of MERS-CoV, the link between animal and human health is evident through the transmission of the virus from dromedary camels to humans. Understanding the dynamics of the virus in animal populations is vital for preventing future zoonotic spillover events and controlling its spread.
Zoonotic Origins and Animal Reservoirs
MERS-CoV is primarily a zoonotic disease, meaning it originates in animals and can be transmitted to humans. Dromedary camels have been identified as the main reservoir of MERS-CoV, with evidence of widespread infection in camel populations in the Middle East and Africa. Studies are ongoing to understand the mechanisms of viral transmission and the potential for other animal species to serve as reservoirs or intermediate hosts.
Preventing Future Spillover Events
Preventing future spillover events of MERS-CoV requires a multifaceted approach. This includes enhancing surveillance systems in animal populations, improving control measures in animal husbandry practices, promoting responsible consumption of animal products, and raising awareness among the public and healthcare professionals about the risks associated with zoonotic diseases. Collaborative efforts between human and animal health sectors are essential for successfully preventing future spillover events.
Research and Future Directions
Current Research Efforts
Ongoing research efforts focus on various aspects of MERS-CoV, including its epidemiology, transmission dynamics, clinical presentation, diagnostics, treatment, and prevention. These research endeavors aim to deepen our understanding of the virus and contribute to the development of more effective control and prevention strategies. Collaboration between researchers and stakeholders at the regional and global levels fosters knowledge sharing and accelerates progress in MERS-CoV research.
Knowledge Gaps and Research Priorities
Despite significant advancements in our understanding of MERS-CoV, several knowledge gaps remain. For instance, the precise mechanisms of viral transmission from camels to humans and the factors that influence the sporadic nature of outbreaks require further investigation. Research priorities include the development of effective treatment options, the evaluation of the potential for human-to-human transmission, and the improvement of diagnostic capabilities in resource-limited settings.
Potential Future Risks
MERS-CoV continues to pose a potential risk to global public health. While the virus has not caused a widespread pandemic like SARS-CoV or COVID-19, the possibility of future mutations or genetic reassortments could lead to increased transmissibility and a higher risk of global spread. Continuous surveillance, research, and preparedness efforts are necessary to monitor the evolution of the virus and respond effectively to any potential future risks.
In conclusion, MERS-CoV is a viral respiratory illness with high morbidity and mortality rates. While the global prevalence of MERS-CoV is relatively low compared to other respiratory viruses, ongoing surveillance, prevention measures, and research efforts are crucial to prevent outbreaks and safeguard public health. The One Health approach, focusing on the interconnectedness of human, animal, and environmental health, is key in preventing future spillover events and controlling the spread of MERS-CoV. By staying vigilant, implementing effective prevention and control measures, and supporting ongoing research, we can mitigate the impact of MERS-CoV and protect the well-being of individuals and communities worldwide.