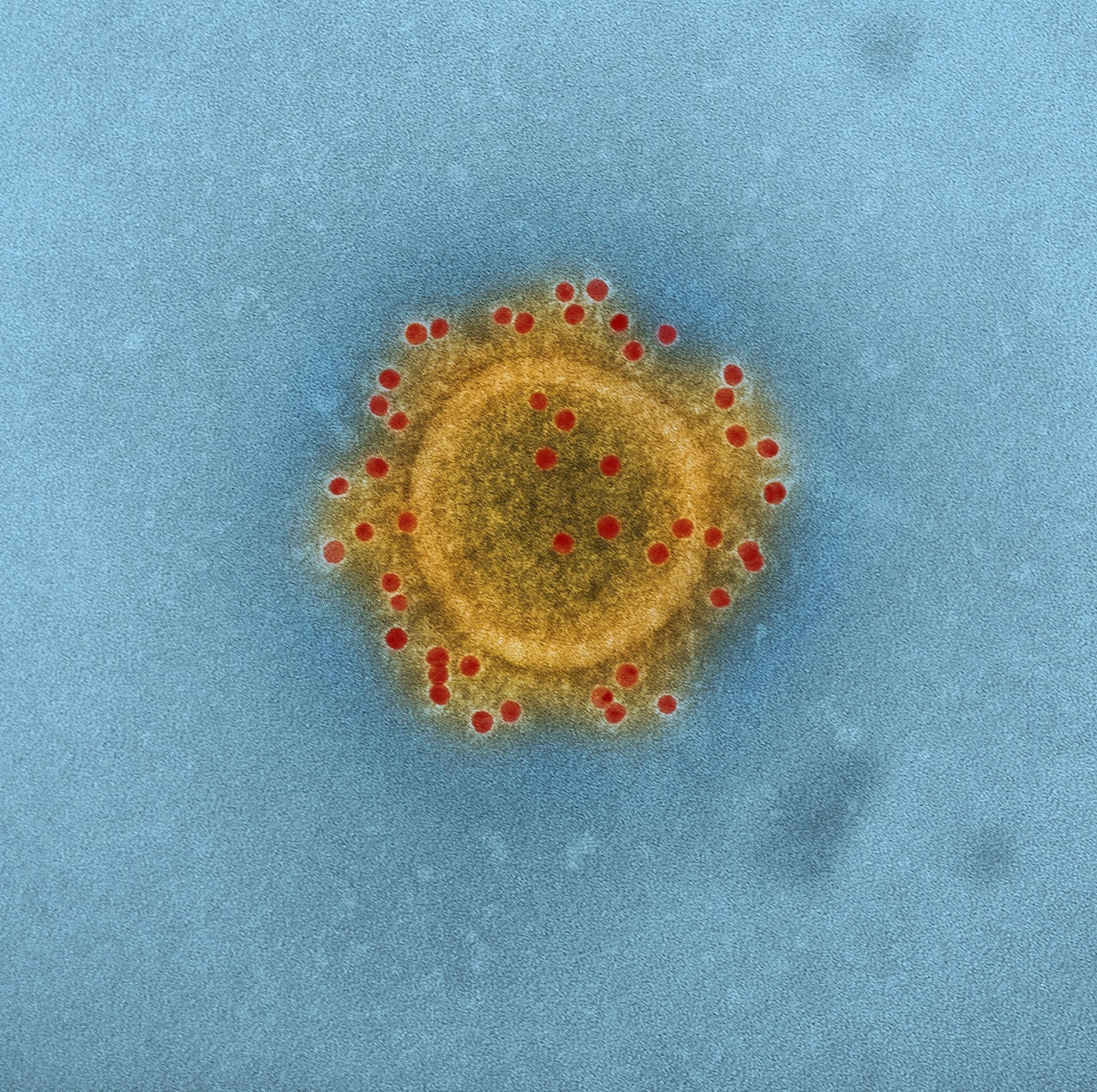
You’re about to discover the latest research findings on the Middle East Respiratory Syndrome Coronavirus (MERS-CoV). From the cutting-edge discoveries unraveling the origins of the virus to the ongoing efforts in developing effective treatments and preventive measures, this article delves into the ever-evolving landscape of MERS-CoV research. Brace yourself for a captivating journey into the world of science as we explore the latest breakthroughs and advancements in combatting this infectious disease. So, grab a cup of tea and get ready to delve into the fascinating world of MERS-CoV research!
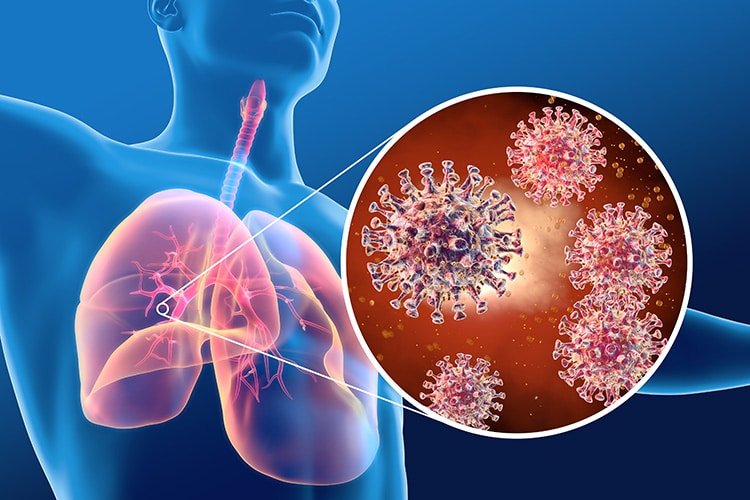
Symptoms of Middle East Respiratory Syndrome Coronavirus (MERS-CoV)
Typical Symptoms
When it comes to Middle East Respiratory Syndrome Coronavirus (MERS-CoV), the symptoms can vary from mild to severe. In most cases, individuals infected with MERS-CoV experience typical symptoms, which include fever, cough, shortness of breath, and muscle aches. These symptoms usually develop within two to 14 days after exposure to the virus. It is important to note that these symptoms are similar to those of other respiratory illnesses, such as the flu or common cold. Thus, it is crucial to seek medical attention if you experience these symptoms, especially if you have a history of travel to regions where MERS-CoV is prevalent.
Severe Symptoms
While most cases of MERS-CoV infection result in mild symptoms, some individuals may develop severe complications. Severe symptoms of MERS-CoV include pneumonia, acute respiratory distress syndrome (ARDS), kidney failure, and even death. These severe symptoms usually occur in individuals who have underlying medical conditions or compromised immune systems. It is important to be aware of the potential for severe symptoms and seek immediate medical attention if you or someone you know experiences them.
Asymptomatic Cases
In addition to typical and severe symptoms, it is worth noting that some individuals infected with MERS-CoV may be asymptomatic. This means that they do not experience any noticeable symptoms despite being infected with the virus. Asymptomatic cases pose a challenge as individuals may unknowingly transmit the virus to others. This highlights the importance of practicing good hygiene and taking preventative measures to reduce the risk of transmission, even if you feel well.
Transmission and Spread of MERS-CoV
Primary Transmission Routes
The primary route of transmission for MERS-CoV is believed to be from animals to humans. The virus is zoonotic in nature, meaning it originates in animals and can be transmitted to humans. Camels, in particular, have been identified as a primary source of transmission. Direct contact with infected animals, such as camels, or consumption of raw camel products, are potential routes of transmission.
Zoonotic Transmission
Zoonotic transmission occurs when the virus jumps from infected animals to humans. This can happen through close contact with infected animals, such as camels, or through consumption of their raw milk or meat. It is important to note that not all individuals who come into contact with infected animals will develop symptoms or get infected. However, individuals who work closely with animals, such as farmers or veterinarians, may be at a higher risk of exposure.
Human-to-Human Transmission
While zoonotic transmission is the primary route of MERS-CoV transmission, there have been instances of human-to-human transmission as well. This typically occurs within close contact settings, such as households or healthcare facilities. Respiratory droplets produced when an infected individual coughs or sneezes can contain the virus, making it possible for transmission to occur. It is crucial to practice good respiratory hygiene, such as covering your mouth and nose when coughing or sneezing, to minimize the risk of transmission.
Super-Spreading Events
Super-spreading events refer to instances where one individual spreads the virus to a disproportionately large number of people. These events can occur in various settings, such as hospitals or social gatherings, and play a significant role in the spread of MERS-CoV. Identifying and containing super-spreading events is crucial in preventing further transmission and controlling outbreaks.
Risk Factors and Vulnerable Populations
Age and Gender
When it comes to MERS-CoV, age and gender can influence the risk of infection and the severity of symptoms. Older individuals, particularly those over the age of 60, are more likely to develop severe symptoms and experience complications compared to younger individuals. Men have been found to be at a higher risk of MERS-CoV infection and severe illness compared to women. However, it is important to note that anyone can become infected with MERS-CoV, regardless of age or gender.
Pre-existing Medical Conditions
Individuals with pre-existing medical conditions, such as diabetes, chronic lung disease, kidney disease, and immunosuppression, are at a higher risk of developing severe symptoms if infected with MERS-CoV. These underlying medical conditions can weaken the immune system and make it more difficult for the body to fight off the virus. It is essential for individuals with such conditions to take extra precautions to reduce their risk of exposure to MERS-CoV.
Healthcare Settings
Healthcare settings, including hospitals and clinics, can pose an increased risk of MERS-CoV transmission. Healthcare workers who come into close contact with infected individuals are at a higher risk of infection if proper infection prevention and control measures are not in place. It is crucial for healthcare facilities to implement strict protocols and guidelines to minimize the risk of transmission within these settings.
Epidemiology and Global Impact
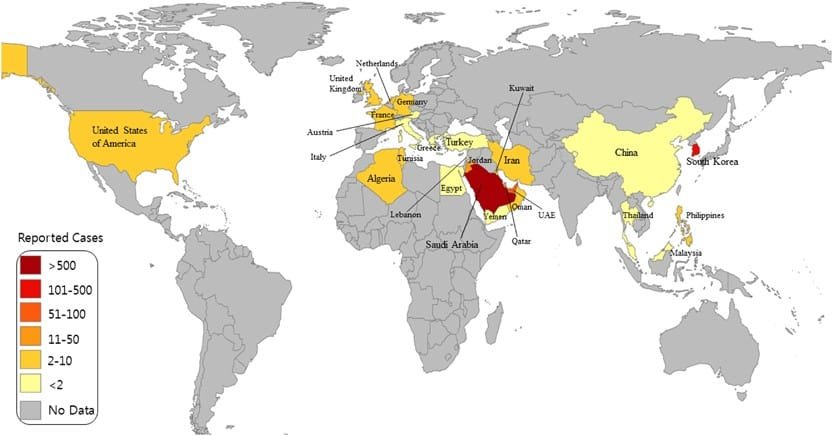
Geographical Distribution
MERS-CoV was first identified in 2012 in the Middle East, and since then, it has spread to other countries. The majority of cases have been reported in Saudi Arabia, but MERS-CoV has also been identified in other regions, including the United States, South Korea, and European countries. The geographical distribution of MERS-CoV highlights the importance of global surveillance and collaboration in monitoring and responding to the virus.
Outbreaks and Case Fatality Rate
Although MERS-CoV is not as widespread as other respiratory viruses, it has caused several outbreaks, leading to a significant number of infections and deaths. The case fatality rate of MERS-CoV varies depending on factors such as age, underlying health conditions, and the quality of healthcare received. On average, the case fatality rate is estimated to be around 35%, which is higher compared to other coronaviruses such as SARS-CoV and SARS-CoV-2 (COVID-19).
Sporadic Cases and Imported Infections
In addition to outbreaks, sporadic cases of MERS-CoV continue to occur, often linked to travel from regions where the virus is prevalent. Imported infections refer to cases where individuals become infected in one region and then travel to other countries while infected. These sporadic cases and imported infections highlight the need for robust surveillance systems and effective preventive measures in healthcare and travel settings.
Diagnosis and Laboratory Testing
Clinical Features
The clinical features of MERS-CoV infection can vary from mild respiratory symptoms to severe respiratory distress. In addition to fever, cough, and shortness of breath, individuals may also experience gastrointestinal symptoms such as diarrhea and vomiting. It is important for healthcare providers to be aware of these clinical features to promptly diagnose and manage cases of MERS-CoV.
Molecular Testing
Molecular testing, such as polymerase chain reaction (PCR), is the main method used to diagnose MERS-CoV infection. This testing involves detecting the genetic material of the virus in respiratory samples or other bodily fluids. Rapid and accurate molecular testing is crucial in identifying individuals infected with MERS-CoV and implementing appropriate infection control measures.
Serological Testing
Serological testing involves detecting antibodies specific to MERS-CoV in blood samples. This type of testing is useful in determining past infections or assessing an individual’s immune response to the virus. However, serological testing alone may not be sufficient for diagnosing acute cases of MERS-CoV infection. It is often used in conjunction with molecular testing for a comprehensive diagnosis.
Treatment and Management Options for MERS-CoV
Symptomatic Treatment
Currently, there is no specific antiviral treatment available for MERS-CoV. Treatment primarily focuses on managing symptoms and providing supportive care. This may include measures such as fever reduction, hydration, and supplemental oxygen for individuals experiencing respiratory distress. It is important to consult with healthcare professionals for appropriate symptomatic treatment and management options.
Experimental Therapies
Due to the lack of specific antiviral treatments, various experimental therapies have been explored for the treatment of MERS-CoV. These include the use of antiviral drugs, convalescent plasma therapy, and experimental monoclonal antibodies. While these therapies show promise, further research and clinical trials are necessary to evaluate their effectiveness and safety.
Supportive Care
Supportive care plays a crucial role in the management of MERS-CoV cases. This includes providing adequate hydration, maintaining respiratory support when necessary, and addressing complications such as pneumonia or kidney failure. The goal of supportive care is to relieve symptoms, prevent complications, and promote recovery.
Infection Prevention and Control
Preventing the spread of MERS-CoV is a key aspect of management. In healthcare settings, strict infection prevention and control measures should be implemented to minimize the risk of transmission. This includes proper hand hygiene, use of personal protective equipment, and adherence to respiratory hygiene practices. In community settings, practicing good respiratory hygiene and following public health guidelines are essential in preventing the spread of MERS-CoV.
Current Vaccination Strategies and Progress
Challenges in MERS-CoV Vaccine Development
Developing a vaccine for MERS-CoV poses several challenges. The virus has a unique genetic makeup, and there are limited animal models available for testing vaccine candidates. Furthermore, the sporadic nature of MERS-CoV outbreaks makes it difficult to conduct large-scale clinical trials. These challenges have hindered the progress in developing a widely available and effective MERS-CoV vaccine.
Experimental Vaccines
Despite the challenges, there have been efforts to develop MERS-CoV vaccines. Several experimental vaccines have shown promise in pre-clinical and early-stage clinical trials. These vaccines aim to induce an immune response against the virus and prevent infection or reduce the severity of the disease. Ongoing research and development efforts continue to explore the potential of these experimental vaccines.
Vaccination Recommendations
Currently, there are no licensed vaccines available for MERS-CoV. However, certain high-risk groups, such as healthcare workers or individuals with frequent exposure to camels in endemic regions, may be considered for vaccination if and when a vaccine becomes available. Vaccination recommendations will be based on the results of ongoing research, safety, and efficacy studies.
Surveillance and Response Measures
Case Reporting and Surveillance
Effective surveillance systems play a crucial role in monitoring the spread of MERS-CoV and providing timely information for public health responses. Timely and accurate reporting of cases, including laboratory-confirmed cases and suspected cases, is essential for understanding the epidemiology and implementing appropriate control measures.
Contact Tracing
Contact tracing involves identifying individuals who may have come into contact with an infected person and monitoring them for symptoms or infection. This process is vital in breaking the chain of transmission and preventing further spread of MERS-CoV. Contact tracing often involves identifying and monitoring close contacts, such as family members, healthcare workers, or individuals who shared close spaces with an infected person.
Infection Control Measures
Infection control measures in healthcare settings are crucial in preventing the spread of MERS-CoV. These measures include proper hand hygiene, use of personal protective equipment, and adherence to respiratory hygiene practices. Healthcare facilities should have robust infection prevention and control protocols in place to reduce the risk of transmission within these settings.
Global Preparedness and Response
MERS-CoV is a global concern, and preparedness and response efforts require collaborations and coordination on an international scale. This includes sharing information, research findings, and best practices among countries, as well as providing support to affected regions in terms of resources, expertise, and capacity building. Global preparedness and response efforts are crucial in mitigating the impact of MERS-CoV outbreaks and preventing future spread.
Lessons Learned from MERS-CoV Epidemics
Lessons for Public Health Systems
MERS-CoV epidemics have highlighted the importance of strong and resilient public health systems. This includes having effective surveillance systems, preparedness plans, and rapid response mechanisms in place. Improving public health infrastructure, investing in research and development, and enhancing collaboration between countries are key lessons learned from MERS-CoV epidemics.
Risk Communication and Preparedness
Clear and timely risk communication is crucial in managing MERS-CoV epidemics. Providing accurate information to the public, healthcare professionals, and policymakers is essential in fostering trust and cooperation. Additionally, proactive preparedness measures, such as educating healthcare workers and the public about MERS-CoV, practicing infection prevention and control, and maintaining supplies of essential medical resources, can help minimize the impact of future outbreaks.
Inter-sectoral Collaboration
Addressing the complex challenges posed by MERS-CoV requires collaboration across sectors, including health, agriculture, and environment. Recognizing the interconnectedness between human and animal health, as well as the social and environmental determinants of health, is essential in formulating comprehensive and effective response strategies. Inter-sectoral collaboration ensures a holistic approach and better preparedness for future outbreaks.
Comparative Analysis with Other Coronaviruses
MERS-CoV vs. SARS-CoV
MERS-CoV and SARS-CoV (Severe Acute Respiratory Syndrome Coronavirus) are both zoonotic coronaviruses that can cause severe respiratory illness in humans. However, there are several differences between the two viruses. MERS-CoV is believed to have a higher case fatality rate compared to SARS-CoV. The primary animal reservoir for MERS-CoV is camels, whereas the reservoir for SARS-CoV was believed to be masked palm civets and certain species of bats. The modes of transmission and the geographical distribution of the two viruses also differ.
MERS-CoV vs. SARS-CoV-2 (COVID-19)
MERS-CoV and SARS-CoV-2, the virus that causes COVID-19, are both coronaviruses but have distinct characteristics. MERS-CoV has a higher case fatality rate compared to SARS-CoV-2, but SARS-CoV-2 has caused a much larger global pandemic with widespread transmission. MERS-CoV is primarily transmitted from animals to humans, whereas SARS-CoV-2 is mainly transmitted through respiratory droplets from person to person. The clinical presentation and symptoms of MERS-CoV and SARS-CoV-2 also differ, although there may be some overlap.
In conclusion, Middle East Respiratory Syndrome Coronavirus (MERS-CoV) is a respiratory illness that can cause mild to severe symptoms, including pneumonia and kidney failure. The primary transmission route of MERS-CoV is from animals to humans, with camels being a major source of infection. However, there have been instances of human-to-human transmission, particularly in close contact settings such as healthcare facilities. Age, pre-existing medical conditions, and healthcare settings are risk factors for severe disease. Effective surveillance, prompt diagnosis through laboratory testing, supportive care, and infection prevention and control measures are crucial in managing MERS-CoV cases. While there are currently no licensed vaccines, experimental vaccines are being developed and researched. Lessons learned from MERS-CoV epidemics include the need for strong public health systems, risk communication, and inter-sectoral collaboration. Comparative analysis with other coronaviruses, such as SARS-CoV and SARS-CoV-2, helps to understand the unique characteristics and impact of MERS-CoV.