If you’ve ever wanted to learn more about multiple sclerosis (MS), then you’re in luck! This comprehensive guide is here to provide you with all the necessary information and insights you need to understand this complex neurological disorder. From its symptoms and causes to its treatment options and management techniques, this article aims to empower you with the knowledge and understanding to navigate through the world of multiple sclerosis with confidence. So, let’s embark on this informative journey together and unlock the secrets of MS!

What is Multiple Sclerosis?
Definition
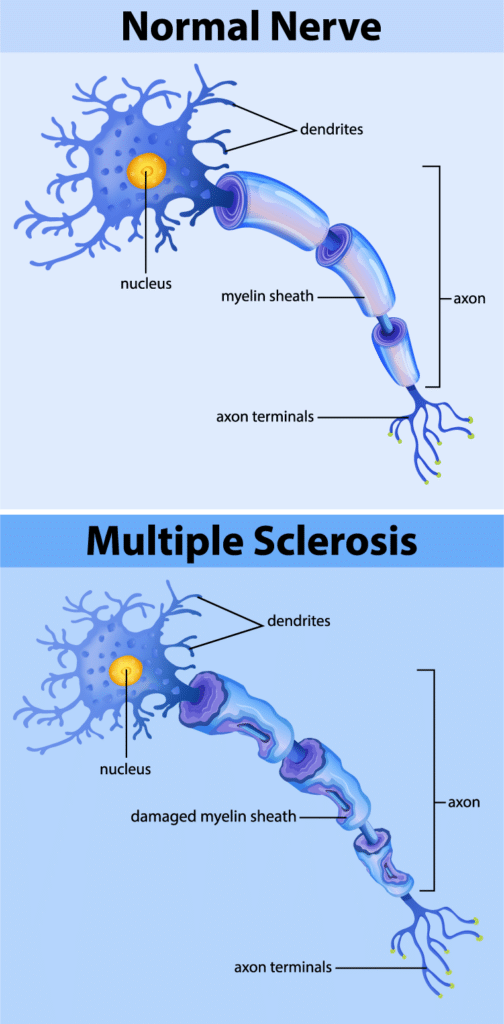
Multiple Sclerosis (MS) is a chronic autoimmune disease that affects the central nervous system (CNS). It occurs when the body’s immune system mistakenly attacks the protective covering of nerve fibers, known as myelin, in the CNS. This inflammation and damage disrupt the transmission of nerve signals between the brain and the rest of the body, leading to a wide range of physical and neurological symptoms.
Causes
The exact cause of multiple sclerosis is still unknown. However, researchers believe that a combination of genetic and environmental factors play a role in its development. It is thought that individuals with certain genes may be more susceptible to developing MS, and exposure to certain viruses or other environmental factors may trigger the immune system to attack the myelin in the CNS.
Symptoms
The symptoms of multiple sclerosis can vary widely between individuals and can also change over time. Some common symptoms include fatigue, numbness or tingling sensations, muscle weakness, balance and coordination problems, vision problems, and cognitive difficulties. These symptoms can significantly impact a person’s daily functioning and quality of life.
Diagnosis
Diagnosing multiple sclerosis can be complex, as there is no single test that can definitively confirm the condition. Medical professionals rely on a combination of medical history, physical examination, neurological examinations, magnetic resonance imaging (MRI) scans, cerebrospinal fluid analysis, evoked potential tests, and blood tests to make an accurate diagnosis. It is essential to consult with a healthcare professional who specializes in neurological disorders for an accurate diagnosis.
Types of Multiple Sclerosis
Relapsing-Remitting MS
Relapsing-Remitting MS (RRMS) is the most common form of multiple sclerosis, accounting for approximately 85% of cases. In RRMS, individuals experience episodes of new or worsening symptoms, known as relapses or flare-ups, followed by periods of remission, during which the symptoms partially or completely resolve. The disease progression in RRMS can vary between individuals, with some experiencing mild symptoms and others facing more frequent relapses and disability.
Primary Progressive MS
Primary Progressive MS (PPMS) is a less common form of multiple sclerosis, affecting approximately 10-15% of individuals with MS. Unlike RRMS, PPMS is characterized by a gradual worsening of symptoms over time, without distinct relapses and remissions. The progression of PPMS can be slow but steady, and individuals often experience a higher level of disability compared to other forms of MS.
Secondary Progressive MS
Secondary Progressive MS (SPMS) typically develops in individuals who initially had RRMS. After a certain period, the disease transition from RRMS to SPMS, resulting in a gradual worsening of symptoms and disability, with or without distinct relapses. The transition to SPMS can occur at different times and rates for each individual.
Progressive-Relapsing MS
Progressive-Relapsing MS (PRMS) is the least common form of MS, affecting fewer than 5% of people with MS. In PRMS, individuals experience a steady progression of symptoms along with occasional relapses or flare-ups. This form of MS tends to have a more severe disease course, leading to significant disability over time.

Risk Factors
Age
Multiple sclerosis can affect individuals of any age, but it commonly develops between the ages of 20 and 50. Nevertheless, it can also occur in children and older adults.
Gender
Women are approximately two to three times more likely to develop multiple sclerosis compared to men. The reasons for this gender disparity are still not fully understood.
Genetics
There is evidence to suggest that genetics play a role in the development of multiple sclerosis. Having a first-degree relative, such as a parent or sibling, with MS increases the risk of developing the condition.
Ethnicity
MS is more prevalent in individuals of Northern European descent, including those with Scandinavian, Scottish, or English ancestry. However, it can affect people of all ethnic backgrounds.
Environmental Factors
Exposure to certain environmental factors, such as viral infections, low vitamin D levels, smoking, and lack of sun exposure, have been linked to an increased risk of developing multiple sclerosis. However, the exact relationship between these factors and MS is still being studied.
Pathophysiology of Multiple Sclerosis
Immune System Involvement
In multiple sclerosis, the immune system mistakenly identifies the myelin, a protective covering of nerve fibers, as foreign and launches an immune response against it. This immune response involves the activation of immune cells, such as T-cells and B-cells, which release inflammatory molecules that damage the myelin and the underlying nerve fibers.
Demyelination
The inflammation caused by the immune system leads to the breakdown of myelin, a process known as demyelination. As the myelin is damaged, the nerve fibers become exposed and are unable to transmit electrical signals effectively. This disruption in the transmission of nerve signals contributes to the development of MS symptoms.
Lesions in the Central Nervous System
The inflammation and demyelination in multiple sclerosis result in the formation of lesions or scar tissue in the CNS, including the brain and spinal cord. These lesions disrupt the normal flow of nerve signals, leading to the wide range of neurological symptoms observed in MS.

Common Symptoms of Multiple Sclerosis
Fatigue
Fatigue is one of the most common symptoms of multiple sclerosis. It is a profound, overwhelming sense of tiredness that is not relieved by rest. Fatigue can significantly impact daily functioning and quality of life for individuals living with MS.
Numbness or Tingling Sensations
Many individuals with multiple sclerosis experience sensations of numbness or tingling, often in the limbs or face. These sensations can range from mild to severe and can be temporary or long-lasting.
Muscle Weakness
Muscle weakness is commonly seen in individuals with multiple sclerosis. It can affect various muscle groups, leading to difficulties with walking, balance, and coordination. This weakness is a result of both the loss of nerve signals and the damage to the myelin that affects the transmission of signals to the muscles.
Balance and Coordination Problems
The disruption in nerve signal transmission caused by MS can result in balance and coordination problems. Individuals may experience difficulty walking, unsteadiness, and a decrease in fine motor control.
Vision Problems
Vision problems are a common symptom of multiple sclerosis. These can include blurry vision, double vision, pain or discomfort in the eyes, and even temporary or permanent loss of vision in severe cases. These vision problems occur due to the involvement of the optic nerves in MS.
Cognitive Difficulties
In addition to physical symptoms, MS can also cause cognitive difficulties. Individuals may experience problems with memory, attention, problem-solving, and processing speed. These cognitive changes can significantly impact daily life and require appropriate management strategies.
Diagnosis of Multiple Sclerosis
Medical History and Physical Examination
A comprehensive medical history is an essential part of the diagnostic process for multiple sclerosis. The healthcare professional will inquire about any symptoms experienced, their duration and frequency, as well as family history of MS or other autoimmune conditions. A thorough physical examination may also reveal signs of central nervous system dysfunction.
Neurological Examinations
Neurological examinations are crucial for evaluating the function of the central nervous system. These examinations may include tests to assess reflexes, coordination, muscle strength, sensation, and balance. The results of these evaluations can provide valuable insights into the presence and progression of MS.
Magnetic Resonance Imaging (MRI)
MRI scans are commonly used to detect the presence of lesions in the central nervous system. These scans produce detailed images of the brain and spinal cord and can help identify areas of inflammation, demyelination, and scarring. MRI is a key tool in diagnosing and monitoring the progression of multiple sclerosis.
Cerebrospinal Fluid Analysis
Obtaining a sample of cerebrospinal fluid through a lumbar puncture can provide valuable information for diagnosing multiple sclerosis. The analysis of this fluid can reveal the presence of certain immune system markers, including an increased number of certain white blood cells and antibodies.
Evoked Potential Tests
Evoked potential tests measure the electrical activity of the brain or spinal cord in response to specific stimuli, such as visual or auditory cues. These tests can help assess the speed and efficiency of nerve signal transmission and detect any abnormalities that may suggest the presence of MS.
Blood Tests
Blood tests are helpful in ruling out other conditions that may mimic the symptoms of multiple sclerosis. These tests can also check for certain antibodies that may be present in MS, although no specific blood marker confirms the diagnosis.
Treatment Options for Multiple Sclerosis
Disease-Modifying Therapies
Disease-modifying therapies (DMTs) are a cornerstone in the management of multiple sclerosis. These medications aim to modify the course of the disease by reducing the frequency and severity of relapses, slowing disease progression, and minimizing the accumulation of new lesions. Several types of DMTs are available, each with its own mechanism of action and potential side effects.
Steroids
Corticosteroids, such as oral prednisone or intravenous methylprednisolone, are often prescribed during acute MS relapses. These medications have powerful anti-inflammatory properties and can help reduce the duration and severity of relapse symptoms. However, long-term use of steroids is generally not recommended due to their potential side effects.
Physical Therapy
Physical therapy plays a crucial role in managing multiple sclerosis. A physical therapist can develop an exercise program tailored to an individual’s abilities and needs, helping improve strength, flexibility, balance, and coordination. Physical therapy can also provide strategies to manage fatigue and optimize mobility.
Occupational Therapy
Occupational therapy focuses on helping individuals with multiple sclerosis maintain independence and improve their ability to perform daily activities. An occupational therapist can provide recommendations on adaptive equipment, energy conservation techniques, and modifications to the home and work environment.
Speech Therapy
Speech therapy can be beneficial for individuals with MS who experience difficulties with speech and swallowing. A speech therapist can provide exercises and strategies to improve speech clarity, swallowing safety, and overall communication skills.
Medications for Symptom Management
Various medications can help manage the symptoms of multiple sclerosis. For example, muscle relaxants can alleviate muscle spasticity, while medications for fatigue can improve energy levels. Other symptom-specific medications target bladder and bowel dysfunction, pain, and depression.
Living with Multiple Sclerosis
Developing a Supportive Network
Living with multiple sclerosis can be challenging, both physically and emotionally. It is essential to cultivate a supportive network of friends, family, and healthcare professionals who can provide understanding, encouragement, and practical assistance. Support groups and online communities can also offer valuable connections and resources.
Adopting a Healthy Lifestyle
Maintaining a healthy lifestyle can be beneficial for individuals with multiple sclerosis. This includes consuming a balanced diet, engaging in regular physical activity, getting enough sleep, and avoiding smoking and excessive alcohol consumption. Following these lifestyle recommendations can help support overall well-being and potentially improve MS symptoms.
Managing Stress
Stress can exacerbate multiple sclerosis symptoms and lead to relapses. Developing effective stress management techniques, such as relaxation exercises, mindfulness, and engaging in enjoyable activities, can help individuals better cope with the challenges of living with MS.
Maintaining a Balanced Diet
A nutritious and balanced diet can support overall health and well-being for individuals with multiple sclerosis. A diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can provide essential nutrients and antioxidants. Some MS-specific dietary approaches, such as the Mediterranean diet, have shown potential benefits in managing symptoms.
Exercise and Physical Activity
Regular exercise and physical activity can improve strength, flexibility, cardiovascular fitness, and overall mood in individuals with multiple sclerosis. Engaging in activities such as walking, swimming, yoga, or Tai Chi can be particularly helpful. It is important to work with healthcare professionals to develop an exercise plan that is suitable for individual abilities and limitations.
Coping Strategies
Living with multiple sclerosis can involve numerous physical and emotional challenges. Developing coping strategies, such as maintaining a positive mindset, seeking emotional support, practicing self-care, and setting realistic goals, can help individuals navigate the ups and downs of life with MS.

Potential Complications of Multiple Sclerosis
Mobility Issues
As multiple sclerosis progresses, mobility may become increasingly affected. Individuals may experience difficulties with walking, balance, and coordination, which can impact independence and daily activities. Assistive devices, physical therapy, and other interventions can help manage these mobility issues.
Cognitive Decline
Cognitive difficulties are common in multiple sclerosis and can range from mild to severe. Some individuals may experience problems with memory, attention, information processing, and problem-solving. Regular cognitive exercises, rehabilitation programs, and strategies for memory and task management can assist in managing these cognitive challenges.
Emotional and Mental Health Challenges
Living with multiple sclerosis can have a significant impact on emotional and mental well-being. Depression, anxiety, and mood swings are common. Seeking professional help, engaging in psychotherapy, and developing healthy coping mechanisms can be fundamental in managing the emotional aspects of MS.
Bladder and Bowel Problems
Multiple sclerosis can affect the nerves that control bladder and bowel function, resulting in bladder urgency, frequency, or incontinence, as well as constipation or bowel incontinence. Medications, bladder retraining, dietary modifications, and other strategies can help manage these symptoms.
Sexual Dysfunction
Sexual dysfunction is not uncommon in individuals with multiple sclerosis. Issues such as reduced libido, erectile dysfunction, and difficulties with arousal or orgasm can occur. Open communication with healthcare professionals and exploring sexual aids or techniques can help address these concerns.
Depression and Anxiety
Depression and anxiety are prevalent among individuals with multiple sclerosis. The emotional impact of the disease, combined with the physical challenges, can contribute to these mental health conditions. It is essential to seek appropriate support and treatment, which can include therapy, medication, and lifestyle changes.
Frequently Asked Questions (FAQs)
Can multiple sclerosis be cured?
Currently, there is no cure for multiple sclerosis. Treatment focuses on managing symptoms, preventing relapses, and slowing disease progression. Ongoing research continues to explore potential new treatments and therapeutic approaches.
What is the life expectancy of someone with multiple sclerosis?
Multiple sclerosis does not typically shorten life expectancy significantly. Many individuals with MS have a normal lifespan. However, the impact of MS on quality of life can vary widely, and certain complications or comorbidities associated with the disease may affect life expectancy.
Can pregnancy affect multiple sclerosis?
Pregnancy can have a variable effect on multiple sclerosis symptoms. Some women experience a decrease in relapses and symptom severity during pregnancy, while others may experience worsening symptoms. It is important for women with MS to work closely with their healthcare team to manage their condition both during and after pregnancy.
Is multiple sclerosis hereditary?
Although there is a genetic component to multiple sclerosis, it is not purely hereditary. Having a family member with MS does increase the risk of developing the disease, but the overall genetic contribution to MS is complex, involving multiple genes and interactions with environmental factors.
Can multiple sclerosis cause death?
While multiple sclerosis is typically not fatal in itself, the complications associated with the disease can sometimes lead to severe disability and secondary health issues that may contribute to mortality. However, with advancing knowledge and treatment options, the overall outlook for individuals with multiple sclerosis has improved significantly in recent years.