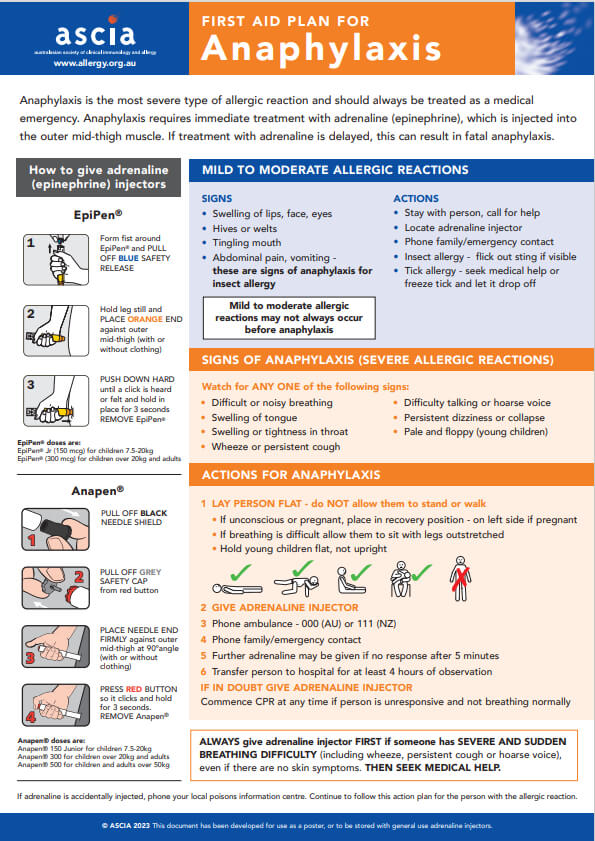
In “Anaphylaxis Treatment: A Comprehensive Guide,” this article provides a comprehensive overview of the management and treatment options available for anaphylaxis. This life-threatening condition can occur rapidly and requires immediate attention. From recognizing the symptoms to administering proper treatment, this guide aims to equip you with the knowledge and understanding necessary to take prompt action in the face of an anaphylactic reaction. With a friendly and approachable tone, we will navigate through the various steps and strategies needed to effectively respond to this medical emergency.
Emergency Procedures
Recognizing Anaphylaxis Symptoms
In order to effectively manage anaphylaxis, it is crucial to be able to recognize its symptoms. Anaphylaxis is a severe and potentially life-threatening allergic reaction that requires immediate medical attention. Common symptoms of anaphylaxis include difficulty breathing, wheezing, swelling of the face or throat, hives, itching, and a sudden drop in blood pressure. It is important to remember that anaphylaxis symptoms can vary from person to person, so it is essential to be vigilant and seek help immediately if any signs of an allergic reaction occur.
Calling Emergency Services
As soon as you suspect anaphylaxis or witness someone experiencing severe allergic symptoms, it is of utmost importance to call emergency services right away. Anaphylaxis requires immediate medical attention, and delaying the call for emergency assistance can be life-threatening. Provide the operator with as much information as possible, including the nature of the allergic reaction, any known allergies, and the individual’s current condition. Stay on the line with the operator and follow any instructions given to you until help arrives.
Administering Epinephrine
Administering epinephrine is a crucial step in managing anaphylaxis. Epinephrine is a medication that helps reverse the symptoms of an allergic reaction and can be the difference between life and death during an anaphylactic episode. If the individual has been prescribed an epinephrine auto-injector, carefully follow the instructions provided with the device. Remember to remove the safety cap, hold the auto-injector firmly against the outer thigh, and press down firmly to release the medication. Once the injection is complete, hold the auto-injector in place for a few seconds before removing it. It is important to seek immediate medical attention even after administering epinephrine.
Laying the Individual Down
When someone is experiencing anaphylaxis, it is crucial to lay the individual down on their back. Elevating their legs can help improve blood flow and prevent a sudden drop in blood pressure. Gently support the person’s head and neck to maintain an open airway. Do not allow the person to stand or sit up as it can further complicate their breathing and potentially worsen the symptoms.
Loosening Tight Clothing
During an anaphylactic episode, it is common for the individual to experience swelling and difficulty breathing. To alleviate any restrictions, it is important to loosen any tight clothing such as collars, belts, or waistbands. This will help provide the person with the necessary space to breathe more easily and reduce the chances of additional discomfort.
Recovery Position
After administering epinephrine and ensuring the individual’s airway is clear, it may be beneficial to place them in the recovery position. This position involves turning the person on their side, with one arm extended and the other bent at the elbow to support their head. The recovery position helps prevent choking and allows any fluids to drain from the mouth, reducing the risk of aspiration. However, if the person is experiencing severe breathing difficulties, it is best to prioritize maintaining an open airway over putting them in the recovery position.
Medications for Anaphylaxis
Epinephrine Auto-Injectors
As mentioned earlier, epinephrine is the first-line medication for managing anaphylaxis. Epinephrine auto-injectors, such as EpiPen or Auvi-Q, are designed for easy and quick administration by individuals or their caretakers during an allergic emergency. These auto-injectors contain a pre-measured dose of epinephrine, ready to be injected into the outer thigh. It is crucial to always carry an epinephrine auto-injector if you or someone you care for has a history of severe allergies. Make sure to check the expiration date regularly and replace it before it expires.
Antihistamines
Antihistamines are commonly used as a secondary treatment for anaphylaxis. They work by blocking the effects of histamine, a chemical released during an allergic reaction that causes symptoms like itching, hives, and nasal congestion. Although antihistamines can help relieve milder allergy symptoms, they are not a substitute for epinephrine in severe cases of anaphylaxis. However, taking antihistamines after administering epinephrine can help provide additional relief and prevent the recurrence of symptoms.
Corticosteroids
Corticosteroids, such as prednisone or methylprednisolone, are another medication commonly used in the management of anaphylaxis. While they do not provide immediate relief, corticosteroids help reduce inflammation and prevent a potentially delayed allergic response. They are usually prescribed to be taken orally after the initial treatment with epinephrine and antihistamines. Corticosteroids can help ensure sustained control of symptoms and prevent a potential rebound reaction.
Bronchodilators
Bronchodilators, such as albuterol, are medications that help relax and open up the airways. They are typically used to treat asthma but can also be beneficial during an anaphylactic episode, especially if the individual experiences wheezing or difficulty breathing. While epinephrine is the primary treatment for anaphylaxis, bronchodilators can be administered if the symptoms persist or if the person has a known history of asthma. It is important to consult with a healthcare professional to determine the appropriate use and dosage of bronchodilators in an emergency situation.

Prevention Strategies
Identifying and Avoiding Triggers
The first step in preventing anaphylaxis is to identify the triggers that may cause an allergic reaction. Common triggers include certain foods, insect stings, medications, and latex. Allergists can perform tests, such as skin prick tests or blood tests, to help identify specific allergens. Once the triggers are identified, it is important to avoid them as much as possible. This may involve reading labels carefully, staying away from known allergens, and making lifestyle adjustments to minimize exposure.
Reading Labels and Checking Food Ingredients
One of the most effective ways to prevent anaphylaxis is to carefully read labels and check food ingredients. Food allergies are a common cause of anaphylaxis, and many allergic reactions occur due to accidental ingestion of allergens. When grocery shopping, always read food labels and look for any potential allergens that may be present. This includes checking for allergen warnings, cross-contamination risks, and hidden sources of allergens. When in doubt, reach out to manufacturers for clarification or choose products that clearly state they are suitable for individuals with allergies.
Carrying an Epinephrine Auto-Injector
Carrying an epinephrine auto-injector at all times is crucial for individuals with a history of severe allergies. Accidental exposure to allergens can happen unexpectedly, and having immediate access to epinephrine can be life-saving. Make it a routine to always have an epinephrine auto-injector readily available in your purse, backpack, or pocket. Inform your family, friends, and coworkers about the importance of recognizing the signs of an allergic reaction and how to use the auto-injector in case of an emergency.
Educating Others about Anaphylaxis
Educating others about anaphylaxis is essential for creating a safe and supportive environment. This includes family members, friends, coworkers, teachers, and anyone who may be in a situation where they need to respond to an allergic emergency. Share information about anaphylaxis, its symptoms, and the appropriate emergency procedures to follow. Provide resources and training materials to help others understand the importance of prompt action and the potentially life-saving impact they can have during an anaphylactic episode.
Managing Anaphylaxis in a Healthcare Setting
Supplemental Oxygen Therapy
In a healthcare setting, supplemental oxygen therapy may be provided to individuals experiencing anaphylaxis. Supplemental oxygen helps ensure the body receives an adequate amount of oxygen, easing breathing difficulties and reducing the risk of complications. Oxygen can be administered through various methods, such as a nasal cannula, a mask, or a headbox, depending on the severity of the symptoms and the individual’s condition. Healthcare professionals will closely monitor the oxygen saturation levels and adjust the oxygen delivery accordingly.
Intravenous Fluids
During severe anaphylaxis cases, intravenous (IV) fluids may be administered to maintain blood pressure and hydration. The drop in blood pressure, known as anaphylactic shock, can lead to organ failure and other life-threatening complications. IV fluids help replenish fluid volume and provide necessary medications, such as corticosteroids and antihistamines, directly into the bloodstream. The administration of IV fluids is typically performed in a hospital or emergency department under the supervision of healthcare professionals.
Continuous Monitoring of Vital Signs
Continuous monitoring of vital signs is crucial in managing anaphylaxis in a healthcare setting. Vital signs, including heart rate, blood pressure, respiratory rate, and oxygen saturation, are essential indicators of an individual’s overall condition. Healthcare professionals will closely monitor these vital signs to assess the effectiveness of the treatment provided and make any necessary adjustments. Continuous monitoring allows for early detection of any potential complications and ensures prompt intervention.
Allergen Immunotherapy
Allergen immunotherapy, commonly known as allergy shots, may be recommended for individuals with severe allergies that frequently trigger anaphylaxis. Immunotherapy involves the gradual exposure to small amounts of specific allergens to desensitize the immune system over time. This treatment can help reduce the severity of allergic reactions and lower the risk of anaphylaxis. It is typically administered under the supervision of an allergist or immunologist and requires regular visits over a period of several years.

Dealing with Anaphylaxis Aftercare
Post-Attack Assessment
After experiencing an anaphylactic episode, it is important to undergo a post-attack assessment to evaluate the severity of the reaction, address any residual symptoms, and identify potential triggers. This assessment may involve follow-up visits with an allergist or other healthcare professionals to review the incident, discuss any remaining concerns or questions, and develop an appropriate aftercare plan. The post-attack assessment helps ensure comprehensive management of anaphylaxis and reduces the risk of future episodes.
Follow-up with Allergist
Following an anaphylactic episode, it is crucial to schedule a follow-up appointment with an allergist. The allergist will review the details of the episode, perform any necessary tests or evaluations, and assess the effectiveness of the current treatment plan. They may recommend adjustments to the management approach or suggest additional preventive measures based on the individual’s specific needs. Regular follow-up appointments with an allergist help ensure ongoing care and support in the management of anaphylaxis.
Anaphylaxis Action Plan
An anaphylaxis action plan is a personalized document that outlines the steps to take in case of an allergic emergency. This plan is typically developed in collaboration with an allergist and includes details about the individual’s specific triggers, emergency contact information, medication dosages, and emergency procedures. An anaphylaxis action plan should be shared with family members, friends, teachers, and anyone who may be responsible for the person’s care to ensure a prompt and appropriate response during an allergic emergency.
Preparation for Future Episodes
While it is impossible to predict when an anaphylactic episode may occur, being prepared can help minimize the impact and ensure swift action. It is important to always carry an epinephrine auto-injector, regularly check its expiration date, and replace it promptly when needed. Consider keeping a backup auto-injector at home, work, or school to account for unexpected situations. Additionally, it may be beneficial to inform close contacts, such as family members, friends, and coworkers, about the nature of your allergies and teach them how to effectively respond to an allergic emergency.
Alternative and Complementary Therapies
Acupuncture
Acupuncture is an alternative therapy that aims to promote balance and harmony in the body. While there is limited scientific evidence specifically supporting acupuncture for anaphylaxis, some individuals find it beneficial for managing their overall health and well-being. It is important to note that acupuncture should not be used as a substitute for standard medical care or emergency treatment during an anaphylactic episode. If considering acupuncture as a complementary therapy, consult with a qualified acupuncturist and inform them about your history of anaphylaxis.
Probiotics
Probiotics are live microorganisms that can provide health benefits when consumed in adequate amounts. While research on the effects of probiotics on anaphylaxis prevention is still evolving, some studies suggest that specific strains of probiotics may have a modulating effect on the immune system. Probiotics are commonly found in fermented foods, such as yogurt, sauerkraut, and kefir, as well as in supplement form. It is important to consult with a healthcare professional before starting any new dietary supplements, especially if you have a history of anaphylaxis.
Herbal Remedies
Herbal remedies have been used for centuries in various cultures to treat various ailments. However, when it comes to managing anaphylaxis, it is important to exercise caution. Some herbal remedies may interact with medications or exacerbate allergies, potentially leading to severe reactions. It is crucial to consult with a qualified herbalist or a healthcare professional knowledgeable in herbal medicine before considering any herbal remedies for anaphylaxis management. Always disclose your history of anaphylaxis and any medications you are currently taking to ensure safe and appropriate guidance.
Mindfulness Techniques
Mindfulness techniques, such as meditation, deep breathing exercises, and relaxation exercises, can help manage stress and anxiety associated with anaphylaxis. While they may not directly impact the physical symptoms of anaphylaxis, they can support overall well-being and provide emotional resilience. Practicing mindfulness techniques regularly can help individuals better cope with the anxiety and fear that can arise from living with severe allergies. Consider incorporating mindfulness techniques into your daily routine or explore guided mindfulness apps or programs to assist you on your journey.
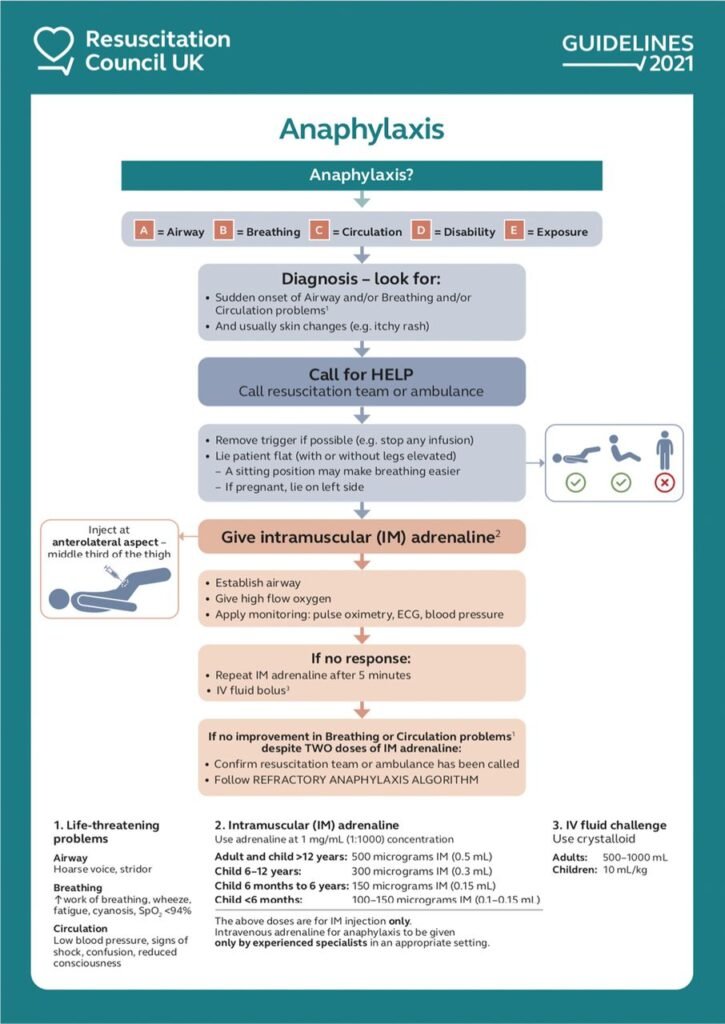
Emerging Treatment Options
Omalizumab (Xolair)
Omalizumab, marketed as Xolair, is a medication approved for the treatment of allergic asthma and chronic idiopathic urticaria. It works by inhibiting the binding of immunoglobulin E (IgE), an antibody involved in allergic reactions. While not specifically approved for anaphylaxis, omalizumab has shown promise in certain cases of severe allergic reactions. It may be considered as an off-label treatment option for individuals with frequent life-threatening anaphylaxis episodes that are not adequately controlled with traditional medications. It is essential to consult with an allergist or immunologist to determine the appropriateness and potential benefits of omalizumab for your specific situation.
Mepolizumab (Nucala)
Mepolizumab, sold under the brand name Nucala, is an injectable medication approved for the treatment of severe eosinophilic asthma and certain eosinophilic granulomatosis with polyangiitis conditions. Eosinophils are a type of white blood cell that is often elevated in individuals with severe allergies and asthma. By targeting and reducing eosinophil levels, mepolizumab can help prevent asthma exacerbations and potentially mitigate the risk of anaphylaxis. As with any emerging treatment options, mepolizumab should only be considered under the guidance of a healthcare professional familiar with the management of anaphylaxis.
Dupilumab (Dupixent)
Dupilumab, known by its brand name Dupixent, is an injectable medication approved for the treatment of moderate to severe atopic dermatitis and certain types of asthma. While it is not specifically indicated for anaphylaxis, dupilumab has shown promise in some studies involving individuals with chronic spontaneous urticaria, a condition characterized by recurrent hives. As an emerging treatment option, the use of dupilumab for anaphylaxis management should be assessed on a case-by-case basis by an allergist or immunologist familiar with the individual’s specific conditions and needs.
Future Research Directions
Anaphylaxis research is an ever-evolving field, with ongoing efforts to improve diagnosis, prevention, and treatment options. Future research directions include exploring novel therapies, identifying biomarkers for risk assessment, and developing targeted interventions. Researchers are investigating potential vaccines for specific allergens, oral immunotherapy for food allergies, and other innovative approaches. Collaboration between researchers, clinicians, and individuals affected by anaphylaxis is essential in advancing our understanding of this severe allergic reaction and developing more effective strategies for prevention and management.
Support and Coping Strategies
Joining Support Groups
Living with anaphylaxis can be challenging and may significantly impact an individual’s daily life. Joining support groups can provide a valuable sense of community, where individuals can share experiences, exchange coping strategies, and receive emotional support. Support groups can be in-person or online, offering a safe space to connect with others who understand the unique challenges of managing severe allergies. Organizations such as the Food Allergy Research and Education (FARE) and Allergy and Asthma Network offer resources and can help individuals find local support groups.
Seeking Psychological Support
Anaphylaxis and severe allergies can have a substantial psychological impact on individuals and their loved ones. Anxiety, fear, and stress can be common emotions experienced by those living with anaphylaxis. Seeking psychological support, such as therapy or counseling, can help individuals cope with the emotional toll of managing severe allergies. Mental health professionals can provide guidance, coping strategies, and support tailored to the specific needs of individuals dealing with anaphylaxis.
Educating Family and Friends
Educating family and friends about anaphylaxis is crucial for creating a supportive environment and reducing the risk of accidental exposure to allergens. Ensure that those close to you understand the severity of the condition, recognize the signs of an allergic reaction, and know how to respond in case of an emergency. Teach them how to use an epinephrine auto-injector and communicate any specific triggers or precautions necessary to keep you safe. Open and honest communication can help foster understanding, empathy, and active participation in your care.
Adapting to Lifestyle Changes
Living with anaphylaxis may require significant lifestyle adjustments to minimize exposure to allergens and mitigate the risk of severe allergic reactions. This may involve changes in dietary habits, reading food labels meticulously, and exploring alternative food options. It may also require avoidance of certain environments, such as pet-owning households or areas with high insect populations. Adaptations like carrying emergency medication at all times, practicing diligent hygiene, and effectively communicating your needs with others can help navigate daily life while managing anaphylaxis.
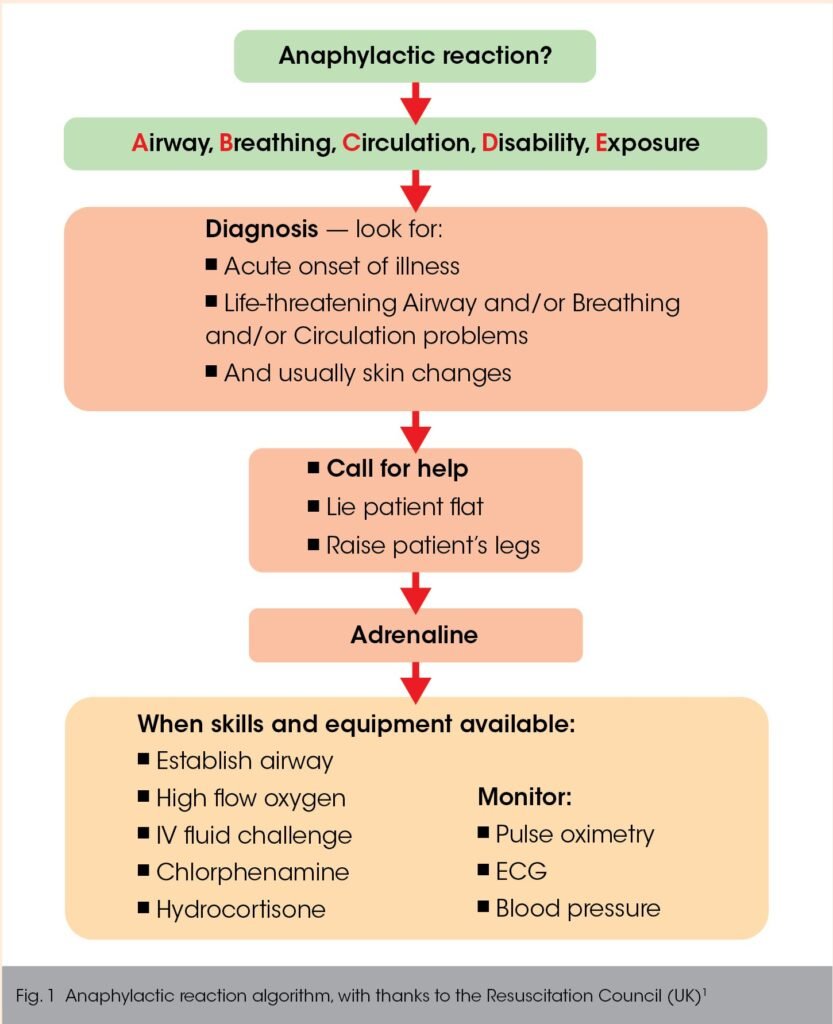
Training on Anaphylaxis Management
First Aid Courses
First aid courses provide invaluable knowledge and skills for managing emergencies, including anaphylaxis. These courses teach participants how to recognize the signs of an allergic reaction, administer epinephrine auto-injectors, and perform life-saving techniques, such as CPR. Taking a first aid course equips individuals with the confidence and competence to respond effectively in emergency situations. Many organizations and healthcare facilities offer first aid courses, and it is recommended for individuals to renew their certification periodically to stay updated on the latest guidelines and techniques.
Epinephrine Auto-Injector Training
Proper training on the use of epinephrine auto-injectors is essential for individuals at risk of anaphylaxis and their caregivers. Understanding how to safely and effectively administer emergency medication can make a significant difference in managing anaphylactic episodes. Seek guidance from healthcare professionals, including allergists or pharmacists, on the correct storage, handling, and administration of epinephrine auto-injectors. Various resources, such as instructional videos and practice devices, are available to ensure individuals feel confident and comfortable using their auto-injectors in an emergency.
Allergy and Immunology Symposia
Allergy and immunology symposia provide an opportunity for medical professionals, researchers, and individuals affected by anaphylaxis to come together and share knowledge and experiences. These events often cover the latest advancements in anaphylaxis management, emerging treatments, and research findings. Attending symposia allows healthcare professionals to stay updated on best practices and individuals to connect with experts in the field. Local medical associations, universities, and professional organizations often host these symposia, offering a wealth of information and networking opportunities.
Medical Professional Education
Medical professionals, including doctors, nurses, and emergency responders, play a critical role in the management of anaphylaxis. Continuing education on anaphylaxis guidelines and protocols is essential to ensure up-to-date and effective care. Medical professional education may include seminars, workshops, and online courses specifically focused on anaphylaxis management. These educational opportunities help healthcare providers remain knowledgeable about the latest research, guidelines, and treatment options, enabling them to deliver optimal care to individuals experiencing anaphylaxis.
Emergency Preparedness for Anaphylaxis
Creating an Emergency Action Plan
An emergency action plan is a personalized document that outlines the steps to take in case of an anaphylactic emergency. It should include information about an individual’s specific triggers, emergency contact details, and clear instructions on how to administer emergency medication, such as an epinephrine auto-injector. Create an emergency action plan in collaboration with an allergist or healthcare professional who understands your specific needs. Ensure that copies of the plan are readily accessible at home, school, work, and any other relevant locations.
Ensuring Accessibility of Epinephrine
Ensuring the accessibility of epinephrine is crucial in managing anaphylaxis emergencies. Make sure that your epinephrine auto-injectors are easily accessible and stored in locations where they can be quickly retrieved. For example, keep auto-injectors in easily identifiable pouches or cases attached to a keychain, backpack, or purse. When transitioning between locations, such as from home to work or school, verify that your emergency medication is with you. Regularly check the expiration dates of your auto-injectors and replace them promptly before they expire.
Educating Schools and Daycares
For individuals with severe allergies, it is essential to educate schools and daycares about anaphylaxis management. Communicate with teachers, administrators, and support staff to ensure they are aware of your specific triggers, symptoms, and emergency procedures. Provide them with a copy of your emergency action plan, including instructions on when and how to administer epinephrine. Establish open lines of communication and maintain regular updates to address any changes or concerns related to your allergies. Collaboration between families, schools, and healthcare providers is key in ensuring a safe and supportive environment for individuals with anaphylaxis.
Emergency Medical Identification
Wearing emergency medical identification, such as a bracelet or necklace, is an important safety measure for individuals with anaphylaxis. Medical identification jewelry should specify the individual’s allergies, the need for epinephrine, and any other pertinent medical information. In case of an emergency, the medical identification helps emergency responders or bystanders quickly identify the individual’s condition and provide appropriate care. Medical identification can be easily obtained from various providers and should be worn at all times, especially when away from home. Regularly update the information on the medical identification to reflect any changes in your medical condition or emergency contact details.