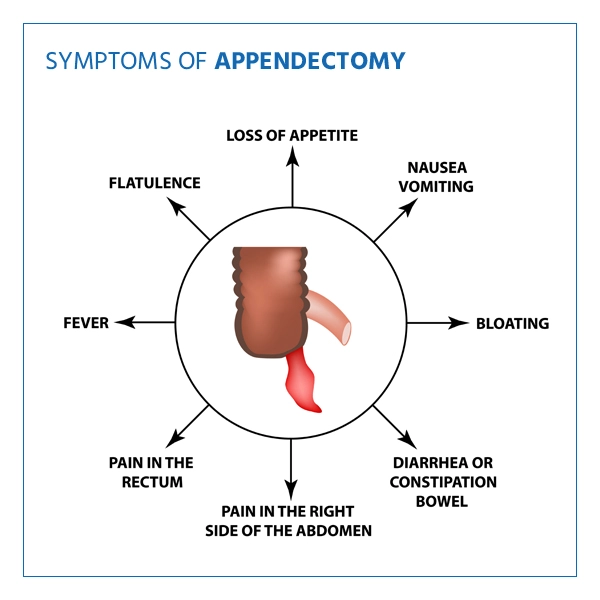
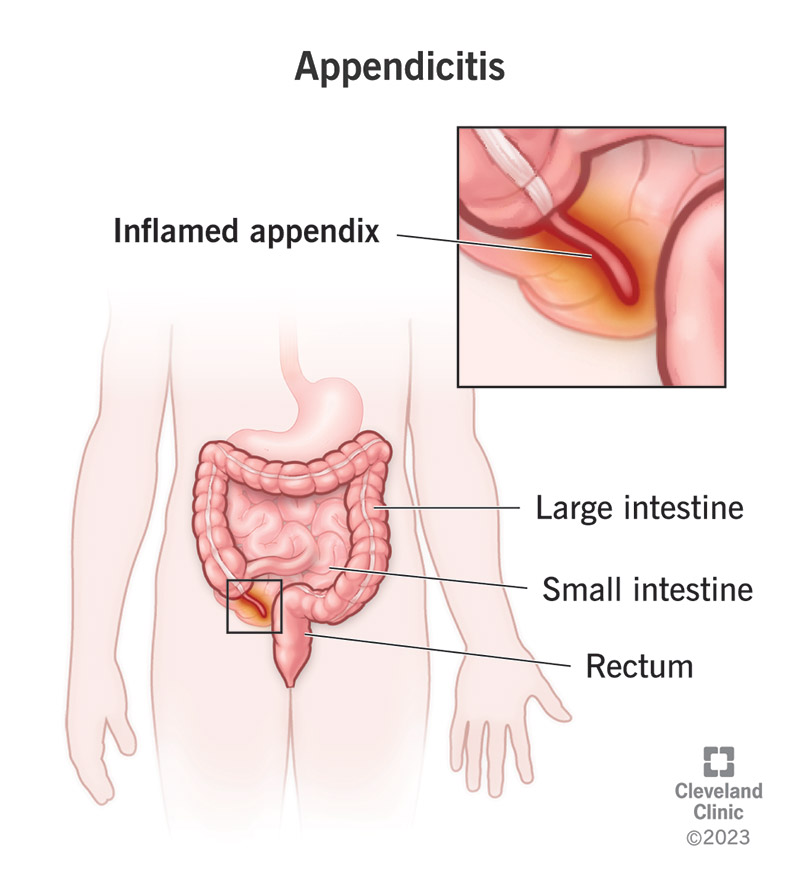
Hey there! Feeling a sharp pain in your abdomen that just won’t go away? It could be a sign of appendicitis, a condition that occurs when your appendix becomes inflamed. But here’s the real kicker – it doesn’t stop there. In this article, we’ll take a closer look at appendicitis complications and why it’s crucial for you to stay informed. So listen up, because when it comes to your health, knowledge is power!
Overview of Appendicitis Complications
Appendicitis, a condition characterized by the inflammation of the appendix, can sometimes lead to various complications. These complications can arise if appendicitis is not promptly diagnosed and treated. It is important to understand the potential complications of appendicitis to ensure timely medical intervention and prevent further health issues. In this article, we will discuss four common complications of appendicitis: perforation, abscess formation, peritonitis, and intestinal obstruction.
Perforation
Perforation refers to the occurrence of a hole or rupture in the appendix. This complication usually arises when appendicitis is left untreated or if there is a delay in seeking medical help. When the appendix perforates, its contents, including bacteria, can leak into the abdominal cavity, leading to infection and other health problems.
Abscess Formation
Abscess formation is another possible complication of appendicitis. An abscess is a localized collection of pus that can develop around the appendix if the infection spreads. This can occur as a result of a ruptured appendix or when the body’s immune response is unable to contain the infection. Abscesses can cause pain, swelling, and fever, and may require drainage or surgical intervention for proper treatment.
Peritonitis
Peritonitis is a severe and potentially life-threatening complication of appendicitis. It occurs when the infection spreads throughout the lining of the abdominal cavity, known as the peritoneum. Peritonitis can lead to severe abdominal pain, fever, nausea, vomiting, and a generalized feeling of illness. Prompt medical attention is crucial in cases of suspected peritonitis, as immediate intervention is necessary to prevent further complications.
Intestinal Obstruction
Intestinal obstruction can occur as a result of appendicitis complications. The inflammation and swelling caused by appendicitis can lead to the obstruction or blockage of the intestines, causing digestive problems. Symptoms of intestinal obstruction may include severe abdominal pain, bloating, nausea, vomiting, and an inability to pass gas or have a bowel movement. It is important to address intestinal obstruction promptly to prevent further complications and restore normal intestinal function.
Diagnosis and Assessment
To accurately diagnose appendicitis complications, healthcare professionals employ various diagnostic methods and assessments. These include physical examination, laboratory tests, and imaging studies.
Physical Examination
During a physical examination, your healthcare provider will assess your abdomen for tenderness, rigidity, and signs of inflammation. They may also perform a test known as the rebound tenderness test, where pressure is applied to the abdomen and released quickly to check for pain upon release. Additionally, your healthcare provider may check for other signs, such as an elevated heart rate or fever, which may indicate an infection or complications.
Laboratory Tests
Laboratory tests are commonly used to aid in the diagnosis of appendicitis complications. Blood tests, such as a complete blood count (CBC), can reveal elevated white blood cell counts, indicating an infection. Urinalysis may be performed to rule out urinary tract infection as the cause of abdominal pain. In some cases, additional tests, such as C-reactive protein (CRP) levels or imaging markers, may be utilized to assess the severity of the infection or inflammation.
Imaging Studies
Imaging studies play a crucial role in the diagnosis and assessment of appendicitis complications. These may include ultrasound, computed tomography (CT) scan, or magnetic resonance imaging (MRI). These imaging techniques allow healthcare professionals to visualize the appendix and surrounding structures, helping to identify any abnormalities or complications such as perforation, abscess formation, or intestinal obstruction. These diagnostic tools are especially valuable when the diagnosis is unclear or in cases of suspected complications.

Perforation
Definition
Perforation occurs when the appendix develops a hole or ruptures. This can be a serious complication of appendicitis and requires immediate medical attention. When the appendix perforates, its contents, including bacteria and fecal matter, can spill into the abdominal cavity, leading to infection and inflammation.
Causes
Perforation most commonly occurs when appendicitis is left untreated. The inflammation and swelling of the appendix can cause increased pressure, ultimately leading to rupture. Other factors that can contribute to perforation include delayed diagnosis, delayed surgical intervention, or an atypical presentation of appendicitis.
Signs and Symptoms
The signs and symptoms of perforation may differ from those of uncomplicated appendicitis. While some individuals may experience a sudden and intense worsening of abdominal pain, others may notice a sudden relief of pain. Other symptoms can include a high fever, rapid heart rate, chills, nausea, vomiting, and a generalized feeling of illness.
Complications
Perforation can lead to various complications, including the formation of abscesses, peritonitis, and intestinal obstruction. The presence of perforation increases the risk of infection and can result in systemic inflammation or sepsis. These complications highlight the importance of promptly diagnosing and treating appendicitis to prevent the development of more severe issues.
Treatment
When perforation is suspected, immediate surgical intervention is often necessary. The aim of surgery is to remove the inflamed appendix, clean the abdominal cavity, and address any associated complications, such as abscesses or peritonitis. Antibiotic therapy is typically administered before and after surgery to prevent or treat infection. Recovery following perforation may involve drainage of abscesses and a longer hospital stay to monitor for any further complications.
Abscess Formation
Definition
Abscess formation is a common complication of appendicitis. It occurs when an infected appendix causes the formation of a localized collection of pus. Abscesses can develop either within the appendix or in the surrounding tissues.
Causes
Abscess formation can occur when the infection spreads from the inflamed appendix. This can happen due to a ruptured appendix or when the body’s immune response is unable to contain the infection. Additionally, delayed diagnosis or delayed surgical intervention can increase the likelihood of abscess formation.
Signs and Symptoms
The signs and symptoms of an abscess may include localized pain, swelling, and tenderness in the lower right abdomen. Fever, chills, fatigue, and a general feeling of illness can also be present. If the abscess has migrated to other areas, there may be pain in different parts of the abdomen.
Complications
If left untreated, abscesses can lead to further complications. These include the spread of infection to other parts of the body, such as peritonitis or sepsis. Furthermore, abscesses can impede the normal function of organs and cause pain and discomfort. Timely intervention is important to prevent these complications and facilitate proper healing.
Treatment
The treatment of an abscess often involves drainage to remove the accumulated pus. This can include surgical drainage or the insertion of a catheter or tube to drain the abscess. Antibiotic therapy is usually administered to treat the infection. In some cases, once the abscess has been drained, a follow-up surgery to remove the appendix may be performed to prevent future abscess formation.

Peritonitis
Definition
Peritonitis is a severe and potentially life-threatening complication of appendicitis. It occurs when the infection spreads throughout the lining of the abdominal cavity, known as the peritoneum.
Causes
Peritonitis usually arises due to a perforated or ruptured appendix. The rupture allows bacteria and other infectious agents to enter the peritoneal cavity, causing widespread inflammation. Delayed diagnosis or surgical intervention can also increase the risk of peritonitis.
Signs and Symptoms
The signs and symptoms of peritonitis are often severe and require urgent medical attention. These may include severe abdominal pain, tenderness, rigidity, and distention. Additional symptoms may include fever, chills, nausea, vomiting, and a general feeling of illness. The abdomen may become rigid and sensitive to touch.
Complications
Without prompt treatment, peritonitis can lead to serious complications. These can include the development of abscesses, sepsis, organ failure, and even death. The spread of infection and inflammation can also affect other organs and systems in the body. Immediate medical intervention is required to minimize the risk of severe complications.
Treatment
The treatment of peritonitis involves a combination of medical and surgical interventions. Surgical intervention is often necessary to remove the appendix, drain abscesses, and clean the abdominal cavity. Antibiotic therapy is administered to combat the infection. In severe cases, intensive care and monitoring may be necessary to manage complications and support organ function.
Intestinal Obstruction
Definition
Intestinal obstruction refers to the blockage or partial blockage of the intestines. Appendicitis can sometimes lead to intestinal obstruction as a result of inflammation and swelling.
Causes
The swelling and inflammation associated with appendicitis can lead to the obstruction of the intestines. The appendix, during an inflamed state, may adhere to nearby organs or tissues, causing a blockage. In severe cases, the appendix itself may become twisted, leading to further obstruction.
Signs and Symptoms
The signs and symptoms of intestinal obstruction can include severe abdominal pain, bloating, abdominal distention, nausea, vomiting, and an inability to pass gas or have a bowel movement. In some cases, there may be visible signs of a “tense” abdomen, where the abdomen feels rigid and sensitive to touch.
Complications
If left untreated, intestinal obstruction can result in serious complications, such as bowel perforation or ischemia (lack of blood supply to the intestines). These conditions can be life-threatening and require immediate medical intervention.
Treatment
The treatment of intestinal obstruction involves addressing the underlying cause, which in this case is appendicitis. This usually requires surgical intervention to remove the appendix and relieve the obstruction. In some cases, additional procedures may be necessary to repair or remove any damaged portions of the intestines. In cases where the obstruction is partial or temporary, non-surgical interventions such as bowel rest, fluid management, and medication may be employed.
Management of Appendicitis Complications
When it comes to managing appendicitis complications, a multidisciplinary approach involving surgery, antibiotic therapy, and drainage procedures is commonly employed.
Surgical Intervention
Surgical intervention is often the primary treatment for appendicitis complications, such as perforation, abscess formation, peritonitis, and intestinal obstruction. The goal of surgery is to remove the inflamed appendix, clean the abdominal cavity, and address any associated complications. This can involve draining abscesses, repairing damaged tissue, or removing sections of the intestines if necessary.
Antibiotic Therapy
Antibiotic therapy is an essential component in the management of appendicitis complications. It is typically administered before and after surgery to prevent or treat infection. The selection of antibiotics will be based on the type and severity of the infection, and may be adjusted as needed.
Drainage Procedures
In cases where abscesses have formed, drainage procedures may be necessary. This involves the insertion of a drain or catheter to remove the accumulated pus and fluid. Drainage procedures can be performed either surgically or under imaging guidance, depending on the location and size of the abscess.
Long-term Effects and Recurrence
Long-term Health Complications
While the timely diagnosis and treatment of appendicitis complications can significantly minimize long-term health consequences, there is a potential for certain complications to arise. These include the development of adhesions (scar tissue), which can cause bowel obstructions in the future. Additionally, individuals who have undergone surgery for appendicitis may have a slightly increased risk of developing certain gastrointestinal disorders, such as inflammatory bowel disease or irritable bowel syndrome.
Recurrence of Appendicitis
Recurrence of appendicitis is a rare occurrence, but it is possible. It is estimated that the risk of recurrent appendicitis after an initial episode is less than 5%. However, in cases where there has been a delay in seeking medical attention or a history of complications, the risk of recurrence may be higher. Prompt medical attention and appropriate treatment are essential in reducing the risk of recurrent appendicitis.

Prevention and Outlook
Preventive Measures
While it is not always possible to prevent appendicitis, there are certain measures that can reduce the risk of complications. Seeking medical attention at the onset of symptoms, such as abdominal pain, can help ensure timely diagnosis and treatment. It is also important to follow medical advice and complete the prescribed course of antibiotics, even after surgical intervention.
Prognosis and Outlook
The prognosis for appendicitis complications can vary depending on the severity and extent of the condition. With prompt medical intervention and appropriate management, the outlook for individuals with appendicitis complications is generally favorable. However, the presence of complications can increase the risk of more serious health issues and may require more extensive treatment. Close monitoring and follow-up care are important in achieving a successful recovery.
Conclusion
Appendicitis complications can arise if the condition is not promptly diagnosed and treated. Perforation, abscess formation, peritonitis, and intestinal obstruction are potential complications that can occur. It is crucial to be aware of the signs and symptoms of these complications to seek immediate medical attention. Diagnosis may involve physical examination, laboratory tests, and imaging studies. Early intervention and proper management, including surgical intervention, antibiotic therapy, and drainage procedures, are key in preventing further complications and promoting recovery. Regular follow-up care is important to monitor for long-term effects and any risk of recurrence. By understanding the complications of appendicitis and taking preventative measures, individuals can ensure better overall health and well-being.