You’re about to embark on a journey of exploration into the intricate connection between Diabetes Mellitus and Eye Health. As you delve into this captivating article, you’ll uncover the profound impact that diabetes can have on your eyesight and discover preventative measures to safeguard your visual health. Get ready to unravel the fascinating relationship between these two elements and gain valuable insights to better care for your eyes in the face of diabetes. Your eyes hold the key to a vibrant world, and this article will equip you with the knowledge to protect and cherish that gift.
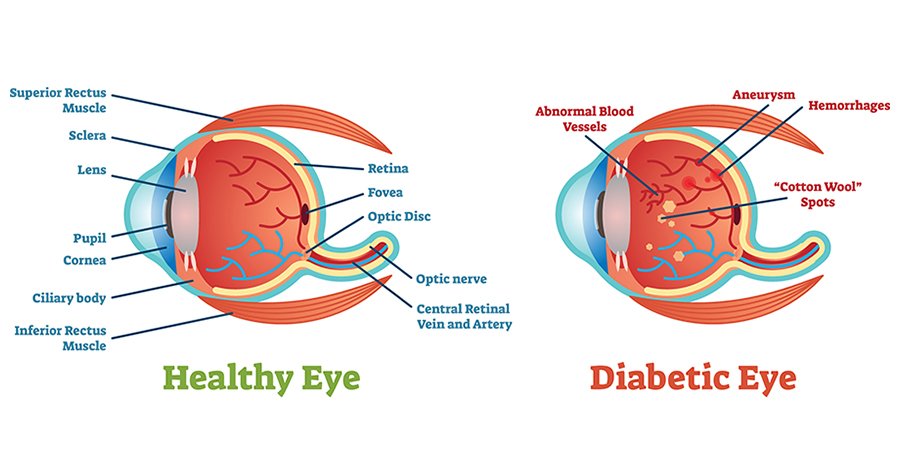
Overview of Diabetes Mellitus
Diabetes Mellitus is a chronic condition that affects the way your body utilizes glucose (sugar) from the food you eat. It occurs when your body either doesn’t produce enough insulin or cannot effectively use the insulin it produces. Insulin is a hormone that helps regulate blood sugar levels and allows glucose to enter cells, where it is used for energy. There are several types of diabetes mellitus, including Type 1, Type 2, and Gestational Diabetes.
Types of Diabetes Mellitus
Type 1 Diabetes
Type 1 diabetes, also known as insulin-dependent diabetes, is an autoimmune disease where the immune system mistakenly attacks the insulin-producing cells in the pancreas. This leads to a complete lack of insulin production in the body. Type 1 diabetes typically develops during childhood or adolescence and requires lifelong insulin therapy to manage blood sugar levels.
Type 2 Diabetes
Type 2 diabetes is the most common form of diabetes and usually occurs in adulthood, although it is increasingly being diagnosed in children and teenagers. In Type 2 diabetes, the body becomes resistant to the effects of insulin, or the pancreas may not produce enough insulin to meet the body’s needs. Lifestyle factors such as obesity, sedentary behavior, and poor diet can significantly increase the risk of developing Type 2 diabetes.
Gestational Diabetes
Gestational diabetes develops during pregnancy and usually resolves after the baby is born. It occurs when the body cannot produce enough insulin to meet the increased demands of pregnancy. Women who develop gestational diabetes are at higher risk of developing Type 2 diabetes later in life. Managing blood sugar levels during pregnancy is crucial to ensure the health of the mother and baby.
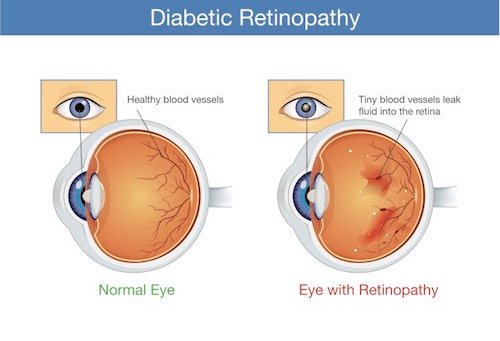
Diabetes Mellitus and Eye Health
Diabetes can have a significant impact on eye health, leading to various complications that can affect vision. It is important to be aware of these complications and take steps to prevent or manage them to maintain optimal eye health.
Prevalence of Diabetes Mellitus-Related Eye Complications
Diabetic Retinopathy
Diabetic retinopathy is the most common eye complication associated with diabetes. It occurs when high blood sugar levels damage the small blood vessels in the retina, which is the light-sensitive tissue at the back of the eye. If left untreated, diabetic retinopathy can lead to vision loss or even blindness.
Diabetic Macular Edema
Diabetic macular edema (DME) is a specific complication of diabetic retinopathy. It occurs when fluid leaks into the macula, the central part of the retina responsible for sharp, detailed vision. DME can cause blurry or distorted vision and may lead to vision loss if left untreated.
Cataracts
Cataracts are a common eye condition where the lens of the eye becomes cloudy, causing vision problems. People with diabetes are at an increased risk of developing cataracts at an earlier age and may experience more rapid progression of the condition. Cataracts can be successfully treated with surgery to replace the cloudy lens with an artificial one.
Glaucoma
Glaucoma refers to a group of eye conditions that damage the optic nerve, which connects the eye to the brain. People with diabetes are at a higher risk of developing glaucoma. If left untreated, glaucoma can lead to permanent vision loss. Early detection and treatment are crucial in managing this condition.
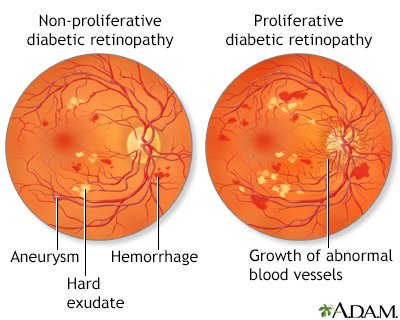
Understanding Diabetic Retinopathy
Definition and Symptoms
Diabetic retinopathy is a complication of diabetes that affects the blood vessels in the retina. It often develops gradually and may not cause noticeable symptoms in the early stages. As the condition progresses, symptoms may include blurred or fluctuating vision, dark or empty areas in the vision, difficulty seeing colors, and vision loss.
Causes and Risk Factors
High blood sugar levels over an extended period are the primary cause of diabetic retinopathy. Other risk factors include long duration of diabetes, poor blood sugar control, high blood pressure, high cholesterol levels, and smoking.
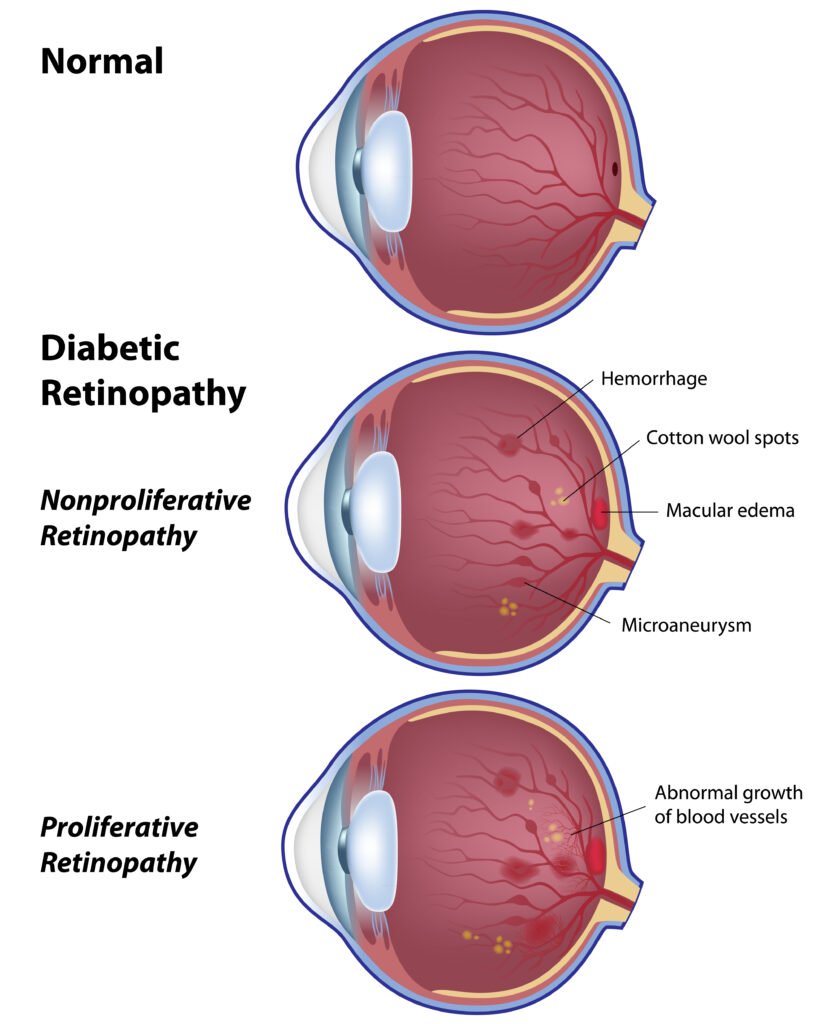
Stages of Diabetic Retinopathy
Diabetic retinopathy is classified into four stages: mild nonproliferative retinopathy, moderate nonproliferative retinopathy, severe nonproliferative retinopathy, and proliferative retinopathy. The severity of the condition is determined by the presence of specific changes in the blood vessels and the extent of damage to the retina.
Treatment and Prevention
The management of diabetic retinopathy involves controlling blood sugar levels, blood pressure, and cholesterol levels. Regular eye examinations are essential for early detection and timely treatment. Laser therapy, intravitreal injections, and surgery may be recommended, depending on the stage and severity of the disease.
Diabetic Macular Edema
Definition and Symptoms
Diabetic macular edema is characterized by the accumulation of fluid in the macula, the central part of the retina. This results in the swelling of the macula and can cause blurred or distorted central vision. Other symptoms may include color perception changes, difficulty reading, and an overall decrease in visual acuity.
Causes and Risk Factors
The main cause of diabetic macular edema is the leakage of fluid from damaged blood vessels within the retina. Poor blood sugar control, high blood pressure, high cholesterol levels, and the duration of diabetes are some of the risk factors associated with the development of this condition.
Diagnosis and Treatment
Diabetic macular edema can be detected through a comprehensive eye examination, including a dilated eye exam and imaging tests such as optical coherence tomography (OCT). Treatment options aim to reduce macular edema and improve vision. These may include laser therapy, intravitreal injections, or in some cases, surgical intervention.
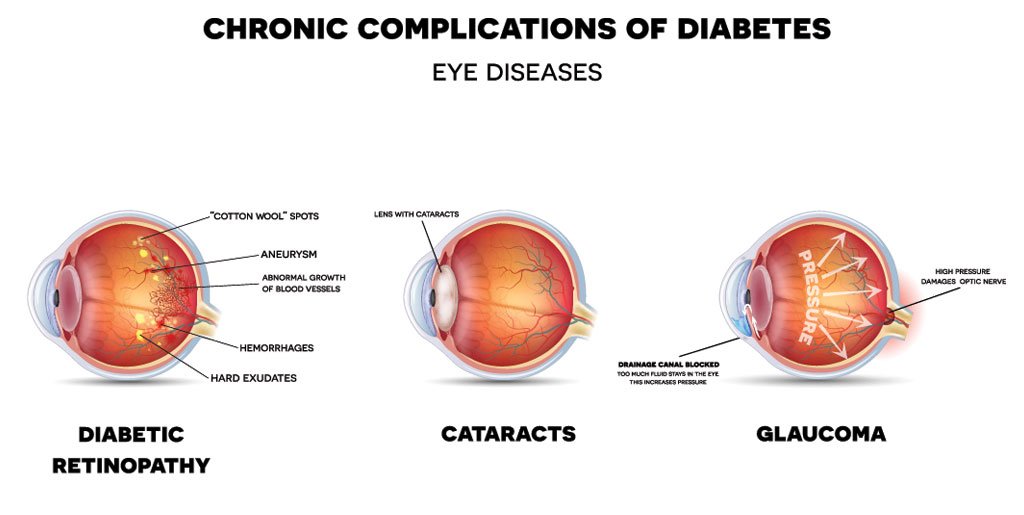
Cataracts and Diabetes
Definition and Symptoms
Cataracts refer to the clouding of the natural lens of the eye, which leads to a progressive decline in vision. Symptoms may include blurry or hazy vision, increased sensitivity to glare, difficulty with night vision, and frequent changes in eyeglass prescription.
Causes and Risk Factors
In people with diabetes, high blood sugar levels can cause changes in the lens of the eye and lead to the development of cataracts. Other risk factors include age, prolonged exposure to sunlight, smoking, and certain medications.
Treatment and Prevention
The treatment for cataracts is surgical removal of the cloudy lens and replacement with a clear artificial intraocular lens. Maintaining good blood sugar control, wearing sunglasses to protect the eyes from UV radiation, and avoiding smoking can help reduce the risk of developing cataracts.
Diabetes and Glaucoma
Definition and Types of Glaucoma
Glaucoma refers to a group of eye conditions that cause damage to the optic nerve, resulting in progressive vision loss. The most common type of glaucoma is primary open-angle glaucoma, which develops slowly over time. Angle-closure glaucoma, on the other hand, occurs when the drainage angle of the eye becomes blocked suddenly, leading to a rapid increase in eye pressure.
Causes and Risk Factors
The exact cause of glaucoma is still unknown, but several risk factors have been identified. These include age, race (people of African, Hispanic, and Asian descent are at higher risk), family history of glaucoma, and certain medical conditions such as diabetes.
Diagnosis and Treatment
Glaucoma is diagnosed through a comprehensive eye examination, including measuring intraocular pressure, evaluating the optic nerve, and checking the visual field. Treatment options aim to lower intraocular pressure and can include eye drops, laser therapy, or surgery, depending on the type and stage of glaucoma.
Importance of Regular Eye Examinations
Frequency of Eye Examinations
Regular eye examinations are crucial for people with diabetes to detect and monitor any diabetes mellitus-related eye complications. The American Diabetes Association recommends annual comprehensive dilated eye examinations for people with Type 1 and Type 2 diabetes. Pregnant women with gestational diabetes should also have an eye examination during pregnancy.
Early Detection and Management of Diabetes Mellitus-Related Eye Complications
Regular eye examinations help in the early detection and timely management of diabetes mellitus-related eye complications such as diabetic retinopathy, diabetic macular edema, cataracts, and glaucoma. Early intervention and treatment can help prevent or minimize vision loss and maintain optimal eye health.
Preventing Diabetes Mellitus-Related Eye Complications
Preventing or minimizing the risk of diabetes mellitus-related eye complications is possible through various lifestyle and health management strategies.
Maintaining Healthy Blood Sugar Levels
Keeping blood sugar levels within the target range recommended by your healthcare provider is crucial for preventing or slowing the progression of diabetes mellitus-related eye complications. Regular monitoring of blood sugar levels, adherence to prescribed medications or insulin therapy, and adopting a healthy lifestyle can help achieve and maintain target levels.
Managing Blood Pressure and Cholesterol
Maintaining normal blood pressure and cholesterol levels is essential for overall cardiovascular health, which plays a significant role in eye health. Regular monitoring, following a heart-healthy diet, engaging in regular physical activity, and taking prescribed medications can help manage blood pressure and cholesterol levels.
Quitting Smoking
Smoking is detrimental to eye health and can significantly increase the risk and progression of diabetes mellitus-related eye complications. Quitting smoking and avoiding exposure to secondhand smoke can help protect your eyes and overall health.
Eating a Balanced Diet
Adopting a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can support overall health and eye health. Including foods with antioxidants, omega-3 fatty acids, and nutrients like vitamins C and E in your diet can help protect against diabetes mellitus-related eye complications.
Exercising Regularly
Engaging in regular physical activity, such as walking, swimming, or cycling, can help control blood sugar levels, manage weight, and improve overall cardiovascular health. Aim for at least 150 minutes of moderate-intensity aerobic activity per week, along with strength-training exercises twice a week.
Monitoring and Managing Overall Health
Regular health check-ups, monitoring of blood sugar, blood pressure, and cholesterol levels, and following your healthcare provider’s recommendations are crucial for managing diabetes and preventing or minimizing its complications on eye health.
In conclusion, understanding the types of diabetes mellitus and their impact on eye health is essential for individuals living with diabetes. Regular eye examinations, maintaining healthy blood sugar levels, managing blood pressure and cholesterol, quitting smoking, adopting a balanced diet, exercising regularly, and monitoring overall health are key in preventing and managing diabetes mellitus-related eye complications. Taking proactive steps can help preserve vision and promote overall well-being in individuals with diabetes.