Have you ever wondered about the connection between the Zoster-Herpes Virus and shingles? This article seeks to unravel the mystery behind this intriguing link. By delving into the world of viral infections, we will explore how the Zoster-Herpes Virus plays a pivotal role in the development of shingles. Prepare to uncover fascinating insights into this complex relationship and gain a deeper understanding of the causes and symptoms of shingles.

Overview of Zoster-Herpes Virus
Definition of Zoster-Herpes Virus
The Zoster-Herpes Virus, also known as the Varicella-Zoster Virus (VZV), belongs to the family of herpes viruses. It is responsible for causing two distinct clinical presentations – chickenpox (varicella) and shingles (herpes zoster). This virus can remain dormant in the body after an initial infection and reactivate later in life, resulting in the development of shingles.
Causes of Zoster-Herpes Virus
The primary cause of the Zoster-Herpes Virus is an initial infection with varicella, commonly known as chickenpox. Once a person has recovered from chickenpox, the virus remains in the body, specifically in nerve tissues. Factors such as aging, weakened immune system, stress, or certain medications can trigger the reactivation of the virus, leading to shingles.
Symptoms and Clinical Presentation
The symptoms and clinical presentation of the Zoster-Herpes Virus vary depending on whether it manifests as chickenpox or shingles. Chickenpox typically starts with a rash that progresses into itchy, fluid-filled blisters all over the body. On the other hand, shingles presents as a painful, blistering rash that is usually localized to one side of the body and follows the distribution of specific nerve roots.
Risk Factors for Zoster-Herpes Virus
Certain factors increase the risk of developing shingles. Advanced age is one of the primary risk factors, with the incidence of shingles increasing significantly after the age of 50. Other risk factors include a weakened immune system due to diseases like HIV/AIDS, undergoing chemotherapy or organ transplantation, and taking immunosuppressive medications. Additionally, individuals who have had chickenpox at a young age are also at risk of developing shingles later in life.
Understanding Shingles
Definition of Shingles
Shingles, also known as herpes zoster, is a viral infection caused by the reactivation of the Zoster-Herpes Virus. It is characterized by the development of a painful rash that typically appears in a band or stripe along one side of the body. The rash usually lasts for a few weeks, and the pain can persist even after the rash has healed.
Connection between Zoster-Herpes Virus and Shingles
Shingles is directly linked to the Zoster-Herpes Virus, as it occurs when the virus reactivates in the body after a period of dormancy. The Zoster-Herpes Virus remains in nerve tissues, and when it reactivates, it travels along nerve pathways, causing inflammation and the characteristic rash associated with shingles. This connection between the virus and shingles underlines the importance of understanding and managing the Zoster-Herpes Virus for the prevention and treatment of shingles.
Signs and Symptoms of Shingles
The signs and symptoms of shingles can vary between individuals, but common manifestations include a painful, burning or tingling sensation before the rash develops. The rash then appears as clusters of small, fluid-filled blisters that gradually crust over. Other symptoms may include fever, headache, sensitivity to light, and fatigue. It is crucial to consult a healthcare professional if shingles is suspected, as early diagnosis and treatment can help manage symptoms and prevent complications.
Complications Associated with Shingles
While shingles typically resolves within a few weeks, there are potential complications that can arise from the infection. One of the most common complications is postherpetic neuralgia (PHN), which is characterized by persistent pain in the area affected by the shingles rash. Shingles can also lead to more severe neurological complications, such as facial paralysis or inflammation of the brain. Ophthalmic complications, including eye infections and vision loss, are also possible in cases where the rash involves the eye area.
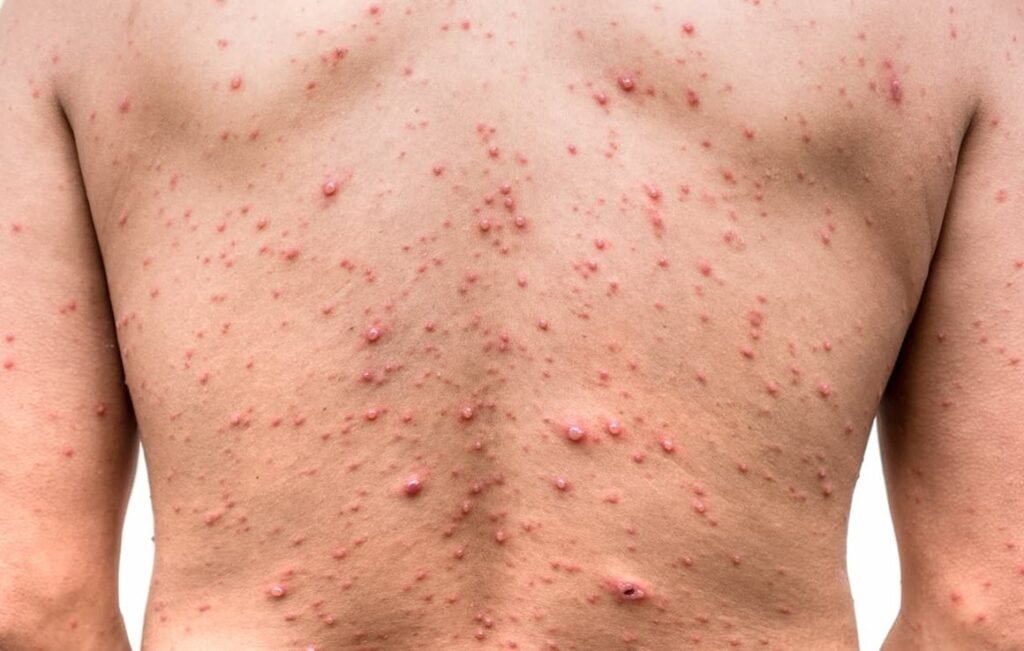
Transmission of Zoster-Herpes Virus and Shingles
Modes of Transmission
The Zoster-Herpes Virus and shingles can be transmitted through various modes, primarily involving direct contact with fluid from the blisters of an infected individual. However, it is important to note that while chickenpox is highly contagious, shingles itself is not as readily transmissible. Understanding the different modes of transmission is crucial in implementing preventive measures and reducing the risk of spreading the virus.
Person-to-Person Transmission
Person-to-person transmission of the Zoster-Herpes Virus is primarily through direct contact with the rash or fluid from the blisters of an infected individual. It is important to avoid contact with the rash or blisters to prevent transmission. Individuals with shingles should also take precautions such as covering the rash with a sterile bandage and practicing good hand hygiene to minimize the risk of spreading the virus to others.
Airborne Transmission
Unlike chickenpox, shingles is not typically transmitted through the airborne route in a casual setting. The virus is not present in respiratory secretions, thus reducing the risk of transmission through coughing or sneezing. However, in rare cases, shingles involving the respiratory tract or lungs can potentially result in airborne transmission, primarily in healthcare settings or in individuals with compromised immune systems.
Transmission from Varicella-Zoster Virus
The transmission of the Zoster-Herpes Virus can also occur from an individual with shingles to someone who has not had chickenpox before. Exposure to the shingles rash can lead to the development of chickenpox in individuals who are not immune to the Varicella-Zoster Virus. It is important to be aware of this potential transmission route, especially when shingles occurs in close contact with individuals who have never had chickenpox or been vaccinated against it.
Diagnosis and Testing for Zoster-Herpes Virus and Shingles
Clinical Examination and Medical History
Diagnosing the Zoster-Herpes Virus and shingles typically involves a clinical examination and a thorough medical history review. Healthcare professionals will examine the rash, take note of the distribution and characteristics, and inquire about any preceding symptoms. They will also consider the patient’s medical history, including previous varicella or shingles infections, to aid in the diagnosis.
Laboratory Tests for Zoster-Herpes Virus
In some cases, laboratory tests may be performed to confirm the presence of the Zoster-Herpes Virus. This can involve obtaining a sample from the rash or blister fluid for viral culture or polymerase chain reaction (PCR) testing. However, these tests are not always necessary for the diagnosis of shingles, as the clinical presentation is often sufficient to make an accurate diagnosis.
Imaging Studies for Shingles Diagnosis
Imaging studies, such as magnetic resonance imaging (MRI), may be utilized in certain situations to aid in the diagnosis of shingles. MRI can provide detailed images of the affected nerve roots, helping to confirm the diagnosis and determine the extent of nerve involvement. These imaging studies are typically reserved for cases where there is concern for complications or when the diagnosis is uncertain based on clinical examination alone.
Differentiating Zoster-Herpes Virus from Other Conditions
It is important to differentiate the Zoster-Herpes Virus and shingles from other similar conditions to ensure appropriate management. Conditions that can present with similar symptoms include herpes simplex virus infections, dermatitis, and allergic reactions. Thorough clinical evaluation, medical history review, and, if necessary, laboratory testing can help in making an accurate diagnosis and ruling out other potential causes.

Treatment Options for Shingles
Antiviral Medications
Antiviral medications are a cornerstone of shingles treatment and aim to reduce the severity and duration of the infection. These medications, such as acyclovir, valacyclovir, and famciclovir, work by inhibiting viral replication. Early initiation of antiviral therapy is crucial to optimize its effectiveness. Individuals with severe symptoms, those at high risk of complications, or those with involvement of the facial or eye area may require hospitalization for intravenous antiviral treatment.
Pain Management Strategies
Pain management is an essential aspect of shingles treatment, as the infection can result in significant discomfort. Over-the-counter pain relievers, such as acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs), can be used to alleviate mild to moderate pain. In more severe cases, prescription pain medications or nerve blocks may be necessary to manage the pain effectively. Additionally, topical numbing agents, such as lidocaine creams or patches, can provide localized relief.
Topical Treatments for Shingles
Topical treatments can also be employed to aid in the healing process and alleviate symptoms associated with shingles. Calamine lotion or menthol-containing creams can help soothe the itching and irritation caused by the rash. Additionally, keeping the affected area clean and dry can promote healing, prevent secondary infections, and contribute to overall symptom relief.
Alternative Therapies and Home Remedies
Some individuals may choose to supplement conventional treatment with alternative therapies or home remedies to help manage the symptoms of shingles. While these approaches may provide symptomatic relief for some, it is essential to consult with a healthcare professional before initiating any alternative therapies, as they may interact with prescribed medications or have limited effectiveness in managing the infection.
Prevention of Zoster-Herpes Virus and Shingles
Vaccination
Vaccination is a crucial strategy for preventing both varicella (chickenpox) and shingles. The varicella vaccine is routinely administered to children to prevent primary varicella infection. Additionally, a separate vaccine specifically targeting shingles (herpes zoster vaccine) is available for individuals over the age of 50 to reduce the risk of developing shingles and its associated complications.
Vaccination Schedule and Recommendations
The vaccination schedule for varicella and shingles varies depending on individual factors and age. Children typically receive the varicella vaccine as part of their routine immunization schedule, and a two-dose regimen is recommended for optimal protection. The shingles vaccine is generally recommended for individuals aged 50 and older, with a single booster dose often administered around the age of 60 to enhance long-term protection.
Post-Exposure Prophylaxis
Post-exposure prophylaxis is another preventive measure that can be used to reduce the risk of developing shingles in certain individuals who have been in close contact with an individual diagnosed with shingles. Administration of antiviral medications within a specified timeframe after exposure can help mitigate the severity of the infection or prevent it altogether.
Preventing Shingles Transmission to Others
To prevent the transmission of shingles to others, individuals with active shingles should avoid close contact with individuals who have never had varicella or been vaccinated against it. Implementing good hand hygiene practices, covering the rash with a sterile bandage, and refraining from touching or scratching the blisters can help minimize the risk of spreading the virus to others.

Complications and Long-Term Effects of Shingles
Postherpetic Neuralgia
Postherpetic neuralgia (PHN) is one of the most commonly reported complications of shingles. It is characterized by persistent pain in the affected area, even after the rash has healed. PHN can last for weeks, months, or even years and can significantly impact an individual’s quality of life. Early intervention, including the use of antiviral medications and pain management strategies, is crucial to minimize the risk of developing PHN.
Neurological Complications
In some cases, shingles can lead to more severe neurological complications. These can include encephalitis, meningitis, or even stroke. These complications are relatively rare but can occur, particularly in individuals with compromised immune systems or when the virus affects critical areas of the nervous system. Timely diagnosis and appropriate treatment can help minimize the risk of these severe neurological complications.
Ophthalmic Complications
Shingles can also affect the eye, leading to potentially serious ophthalmic complications. When the rash involves the ophthalmic branch of the trigeminal nerve, it can cause inflammation of the eye (herpes zoster ophthalmicus). This can result in eye pain, redness, vision changes, and, in severe cases, permanent vision loss. Immediate medical attention is crucial to prevent long-term damage and preserve vision in cases involving the eye.
Impact on Quality of Life
Shingles and its complications can have a significant impact on an individual’s quality of life. The pain associated with shingles can be debilitating, affecting an individual’s ability to perform daily activities and negatively impacting their emotional well-being. The risk of developing chronic pain, such as postherpetic neuralgia, can also lead to long-term challenges in managing pain and maintaining a desirable quality of life. Early diagnosis, appropriate treatment, and comprehensive supportive care can help mitigate the impact on an individual’s daily life.
Epidemiology of Zoster-Herpes Virus and Shingles
Global Prevalence
The Zoster-Herpes Virus is highly prevalent worldwide, with individuals at risk of developing shingles, particularly as they age. Varicella prevalence varies globally, with some regions reporting high rates of primary varicella infection during childhood. Risk factors, socioeconomic conditions, and vaccination practices influence the overall prevalence of the virus and subsequent development of shingles in different populations.
Age and Gender Distribution
Shingles primarily affects older individuals, with the incidence increasing substantially after the age of 50. Aging is associated with a natural decline in immune function, making older adults more susceptible to viral reactivation. While shingles can occur in individuals of any gender, some studies suggest a slightly higher incidence in women, although the reasons for this difference are not yet fully understood.
Factors Affecting Shingles Incidence
Several factors can influence the incidence of shingles. As previously mentioned, age is a significant risk factor, with older individuals being more susceptible to the reactivation of the Zoster-Herpes Virus. Additionally, certain medical conditions, such as HIV/AIDS or cancer, can weaken the immune system and increase the risk of developing shingles. Stress, particularly chronic or severe stress, is also known to be a trigger for viral reactivation and the development of shingles.
Trends and Patterns of Zoster-Herpes Virus Infection
The incidence of shingles has been on the rise in recent years, likely due to multiple factors, including aging populations and changes in epidemiological patterns. Furthermore, improved surveillance, diagnostic techniques, and awareness have contributed to a better understanding of the disease burden and its impact on individuals and healthcare systems. Continued monitoring and research are essential to track trends and patterns of Zoster-Herpes Virus infection, which can aid in the development of effective prevention and treatment strategies.

Research and Developments in Zoster-Herpes Virus and Shingles
Advances in Vaccines and Preventive Strategies
Significant advancements have been made in the development of vaccines and preventive strategies for the Zoster-Herpes Virus. Improvements in the shingles vaccine have led to the availability of highly effective vaccines that provide long-term protection against shingles and its complications. Ongoing research aims to further enhance vaccine efficacy and explore the possibility of developing a universal herpes vaccine, which could provide broader protection against multiple strains of herpes viruses.
Understanding the Virus Replication Cycle
Continued research efforts have focused on deepening our understanding of the virus replication cycle of the Zoster-Herpes Virus. By deciphering the molecular mechanisms involved in the reactivation of the virus and its interactions with host cells, researchers strive to identify potential therapeutic targets. This knowledge can guide the development of novel antiviral agents that may be more effective in treating and preventing shingles.
Investigational Therapies
Various investigational therapies are being explored for the treatment of shingles, particularly in high-risk populations or cases with severe complications. These therapies may include novel antiviral agents, immune modulators, or targeted therapies aimed at minimizing viral replication and inflammation. Clinical trials and ongoing research are essential for evaluating the safety and efficacy of these potential therapeutic options.
The Link between Zoster-Herpes Virus and Other Diseases
Research is also uncovering potential links between the Zoster-Herpes Virus and other diseases beyond shingles. Studies have suggested associations between the Zoster-Herpes Virus infection and an increased risk of cardiovascular disease, stroke, and certain neurological conditions. Further investigations are needed to better understand these connections and their implications for disease prevention and management strategies.
Conclusion
Summary of Zoster-Herpes Virus and Shingles
In conclusion, the Zoster-Herpes Virus, also known as the Varicella-Zoster Virus, is responsible for causing both chickenpox and shingles. Shingles, which occurs due to the reactivation of the virus later in life, is characterized by the development of a painful rash. Prompt diagnosis and appropriate treatment are crucial to managing symptoms and preventing complications associated with shingles.
Key Takeaways
Key takeaways from this comprehensive article include understanding the causes, symptoms, and risk factors associated with the Zoster-Herpes Virus and shingles. Recognizing the modes of transmission and the importance of vaccination and preventive strategies is essential for reducing the incidence and impact of shingles. Lastly, ongoing research and advancements in treatment options and understanding the virus’s replication cycle hold promise for improved prevention and management of shingles.
Future Directions for Research
In the future, research efforts should continue to focus on developing more effective vaccines, exploring novel therapeutic options, and deepening our understanding of the complex interactions between the Zoster-Herpes Virus and the human host. Furthermore, the investigation of potential links between the virus and other diseases can contribute to a more comprehensive approach to disease prevention and management.
Potential Impact of Effective Prevention and Treatment
Effective prevention and treatment strategies for the Zoster-Herpes Virus and shingles can have a significant impact on individuals and communities. By reducing the incidence of shingles, the burden of pain, complications, and long-term effects can be minimized. Furthermore, the prevention and management of shingles can lead to improved quality of life for individuals, particularly older adults who are more vulnerable to the virus’s reactivation.
In conclusion, understanding the Zoster-Herpes Virus and shingles is vital for prevention, early diagnosis, and effective management. By staying informed, implementing preventive measures, and seeking appropriate medical care, individuals can mitigate the impact of the Zoster-Herpes Virus and shingles on their health and well-being.
