In this article, you will discover the latest research findings on the Zoster-Herpes Virus and its clinical implications. With advancements in medical science, understanding this virus has become crucial in the field of healthcare. From its causes and transmission to its potential long-term effects on the human body, this article will provide you with comprehensive insights into this commonly encountered virus. So, get ready to uncover the fascinating world of the Zoster-Herpes Virus and its impact on our health.

Clinical Overview of Zoster-Herpes Virus
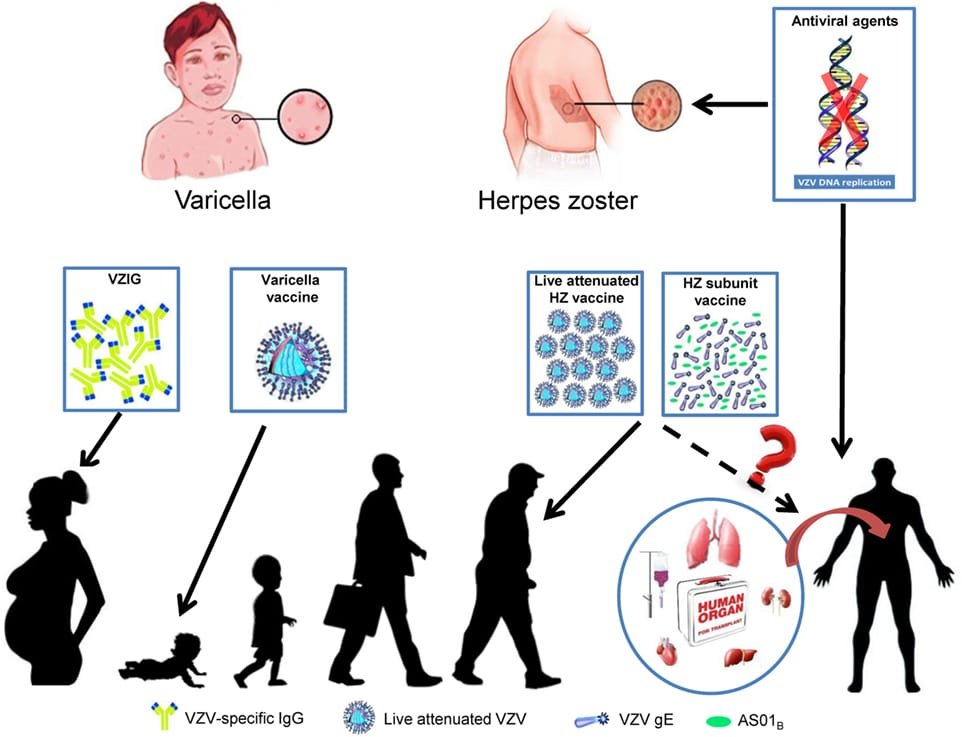
Zoster-Herpes Virus, also known as varicella-zoster virus (VZV), is a highly contagious virus that belongs to the herpesviridae family. This virus is responsible for causing two distinct clinical conditions: chickenpox (varicella) and shingles (herpes zoster). Once an individual is infected with VZV, the virus remains dormant in the sensory ganglia until it is reactivated later in life, leading to the development of shingles.
Pathophysiology of Zoster-Herpes Virus
The pathophysiology of the zoster-herpes virus involves a combination of viral reactivation and immune response. After the initial infection with VZV during childhood, the virus establishes latency in the sensory ganglia, specifically in the dorsal root or cranial nerve ganglia. Under certain conditions such as aging, stress, or immunosuppression, the virus can reactivate and travel along the sensory nerve fibers, resulting in the characteristic rash and pain associated with shingles.

Epidemiology of Zoster-Herpes Virus
Zoster-Herpes Virus is a widespread infection, with an estimated 1 million cases of shingles occurring annually in the United States alone. The risk of developing shingles increases with age, as the incidence rises sharply after the age of 50. It is important to note that individuals who have not been previously infected with VZV and have not received the varicella vaccine can develop chickenpox upon exposure to shingles.
Clinical Presentation and Symptoms of Zoster-Herpes Virus
The clinical presentation of zoster-herpes virus typically begins with the prodromal phase, consisting of nonspecific symptoms such as malaise, fatigue, and headache. This is followed by the characteristic dermatomal rash, which is a painful and vesicular eruption localized to a specific area. The rash usually lasts for 2-4 weeks, with the associated pain potentially persisting long after the rash has resolved, resulting in a condition known as postherpetic neuralgia.
Complications of Zoster-Herpes Virus
While most cases of zoster-herpes virus resolve without any complications, certain individuals may experience complications that can be debilitating. One of the most common complications is postherpetic neuralgia (PHN), which is characterized by persistent pain lasting for more than three months after the rash has healed. Other potential complications include herpes zoster ophthalmicus (involvement of the eye), meningoencephalitis (inflammation of the brain and meninges), and neurological sequelae such as facial paralysis.
Diagnostic Methods for Zoster-Herpes Virus
The diagnosis of zoster-herpes virus is primarily based on clinical presentation and physical examination. However, specific laboratory tests can aid in confirming the diagnosis and guiding appropriate management.
Physical Examination
During physical examination, healthcare providers will carefully examine the rash, noting its distribution and characteristics. The presence of a unilateral and dermatomal rash is highly suggestive of zoster-herpes virus. In some cases, additional symptoms such as fever and lymphadenopathy may also be present.
Viral Culture and Polymerase Chain Reaction (PCR)
Viral culture and PCR are two laboratory techniques used to detect VZV in skin lesions or other bodily fluids. These tests can provide a definitive diagnosis by identifying the presence of viral DNA or isolating the live virus from the sample. However, it is important to note that these tests need to be performed within a specific timeframe, ideally within 72 hours of rash onset, to yield accurate results.
Serologic Testing
Serologic testing involves evaluating blood samples for the presence of VZV-specific antibodies. While serologic tests can confirm past VZV infection, they are not very helpful in the acute phase of the disease. Serologic testing can be particularly useful in cases where the clinical presentation is atypical or if there is uncertainty about the patient’s vaccination status.
Antibody Testing
Antibody testing, specifically the varicella-zoster virus glycoprotein-based enzyme immunoassay (EIA), can assess an individual’s immunity to VZV. This type of testing is often performed in situations where the patient’s immune status is uncertain, such as in healthcare workers or immunocompromised individuals.

Pharmacological Treatment of Zoster-Herpes Virus
Treatment for zoster-herpes virus aims to alleviate symptoms, shorten the duration of the illness, and prevent complications. It primarily comprises antiviral medications, analgesics, topical agents, and occasionally, corticosteroids or immunomodulatory therapy.
Antiviral Medications
Antiviral medications, such as acyclovir, valacyclovir, and famciclovir, are the mainstay of treatment for zoster-herpes virus. These medications work by inhibiting viral replication and reducing the severity and duration of symptoms. Prompt initiation of antiviral therapy within 72 hours of rash onset is essential to achieve the best outcomes.
Analgesics and Topical Agents
Pain management plays a crucial role in the treatment of zoster-herpes virus. Over-the-counter analgesics such as acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs) can be used to relieve mild to moderate pain. Additionally, topical agents like lidocaine patches, capsaicin cream, and antiviral creams can provide localized pain relief and aid in the healing process of the rash.
Corticosteroids
Corticosteroids, such as prednisone, can be used in combination with antiviral therapy to reduce inflammation and alleviate pain. However, their use should be carefully considered, as the evidence supporting their efficacy is mixed, and they can potentially delay viral clearance.
Immunomodulatory Therapy
In certain cases, particularly in immunocompromised individuals, the use of immunomodulatory therapies like intravenous immunoglobulin (IVIG) or monoclonal antibodies may be considered. These treatments aim to modulate the immune response and prevent complications associated with zoster-herpes virus.
Non-Pharmacological Treatment of Zoster-Herpes Virus
In addition to pharmacological interventions, non-pharmacological treatments can also help manage the symptoms of zoster-herpes virus and improve the overall well-being of the affected individuals.
Cool Compresses and Soothing Baths
Cool compresses and soothing baths can provide relief from the itching and discomfort associated with the rash. Cold, wet compresses applied to the affected area can help alleviate pain and reduce inflammation. Similarly, taking cool baths or using colloidal oatmeal-based products can soothe the skin and alleviate itching.
Topical Calamine Lotion or Oatmeal Baths
Topical calamine lotion can be applied to the rash to provide relief from itching and help dry out the blisters. Oatmeal baths, either commercial products or homemade preparations, can also help soothe the itchiness and inflammation associated with the rash.
Pain Management Techniques
Various pain management techniques, including relaxation exercises, distraction techniques, and transcutaneous electrical nerve stimulation (TENS), can be employed to alleviate the pain associated with zoster-herpes virus. These techniques aim to reduce pain perception and improve overall quality of life during the illness.
Psychosocial Support
The impact of zoster-herpes virus extends beyond the physical symptoms, as it can also have significant psychosocial implications. It is important to provide adequate psychosocial support to individuals affected by the virus, as they may experience anxiety, depression, and social isolation. Counseling, support groups, and education about the condition can help individuals cope with the emotional and psychological aspects of the disease.

Prevention and Vaccination for Zoster-Herpes Virus
Prevention of zoster-herpes virus relies on vaccination, effective infection control measures, and post-exposure prophylaxis in certain situations.
Varicella-Zoster Virus Vaccination
Vaccination against varicella-zoster virus is the best strategy to prevent both chickenpox and shingles. The varicella vaccine is recommended for children and adults who have not been previously vaccinated or infected with the virus. Additionally, a shingles vaccine, specifically the recombinant zoster vaccine (RZV), is recommended for individuals aged 50 years and older to prevent the development of shingles and its associated complications.
Preventing Transmission to Vulnerable Populations
To prevent the transmission of zoster-herpes virus to vulnerable populations, such as infants, pregnant women, and individuals with weakened immune systems, it is important to implement strict infection control measures. This includes avoiding contact with individuals who have active shingles, ensuring good hand hygiene, and maintaining a clean environment.
Post-Exposure Prophylaxis
In specific situations where individuals who are at high risk of severe disease come into close contact with someone with shingles, post-exposure prophylaxis with varicella zoster immunoglobulin (VZIG) may be considered. This treatment can help reduce the severity and duration of illness in vulnerable individuals.
Immunocompromised Individuals
Immunocompromised individuals, including those with HIV/AIDS, transplant recipients, and individuals receiving immunosuppressive therapy, should be closely monitored and managed to prevent the development of severe shingles. Vaccination against varicella-zoster virus should be considered in eligible individuals to strengthen their immune response.
The Relationship Between Zoster-Herpes Virus and Cancer
Recent research has shed light on the potential link between zoster-herpes virus and certain types of cancer. While the association between these two is still being studied, several cancer types have been found to have an increased incidence in individuals with a history of zoster infection.
Association with Certain Cancer Types
Studies have shown an increased risk of developing certain cancers, such as lymphoma, leukemia, and solid tumors, in individuals with a history of zoster infection. The underlying mechanisms behind this association are not fully understood and require further investigation.
Viral Factors Influencing Carcinogenesis
There is evidence to suggest that certain viral factors, such as specific VZV strains and genetic variants, may play a role in the development of cancer. These factors could potentially alter the immune response and contribute to the carcinogenic process.
Potential Therapeutic Implications
Understanding the relationship between zoster-herpes virus and cancer can have significant therapeutic implications. It might open doors to the development of targeted therapies that aim to prevent or treat certain cancers by targeting viral factors or modulating the immune response.
Zoster-Herpes Virus in Special Populations
Zoster-herpes virus can have unique clinical implications in certain populations, including pregnant women, children, immunocompromised patients, and the elderly.
Zoster in Pregnancy
Zoster infection during pregnancy is relatively rare but can lead to serious complications for both the mother and the developing fetus. The use of antiviral medications should be carefully considered, taking into account the potential risks and benefits. Vaccination against varicella-zoster virus should ideally take place before pregnancy to minimize the risk of vertical transmission.
Pediatric Zoster
While zoster is more commonly seen in older individuals, it can also occur in children. The clinical presentation and management of zoster in children are similar to those in adults, with antiviral therapy being the mainstay of treatment. However, the vaccination against varicella-zoster virus remains the best preventive measure to reduce the risk of zoster in children.
Zoster in Immunocompromised Patients
Immunocompromised individuals, such as those with HIV/AIDS, organ transplant recipients, and individuals receiving immunosuppressive therapy, are at an increased risk of developing severe and disseminated zoster. Prompt diagnosis and aggressive management are crucial in this population, often necessitating a multidisciplinary approach involving infectious disease specialists, dermatologists, and immunologists.
Geriatric Zoster
Zoster infection in the elderly population can have significant clinical implications, including a higher risk of complications such as postherpetic neuralgia and ophthalmic involvement. Vaccination against varicella-zoster virus is recommended in individuals aged 50 years and older to reduce the risk of developing zoster and its associated complications.
Long-Term Complications and Sequelae
Zoster-herpes virus can lead to various long-term complications and sequelae, which may significantly impact the quality of life of affected individuals.
Postherpetic Neuralgia (PHN)
Postherpetic neuralgia (PHN) is the most common long-term complication of zoster infection, characterized by persistent pain that lasts for months or even years after the resolution of the rash. Management of PHN involves a multimodal approach, including medications targeting neuropathic pain, topical agents, and interventional procedures.
Herpetic Meningoencephalitis
Herpetic meningoencephalitis is a rare but serious complication of zoster infection, characterized by inflammation of the brain and meninges. Early diagnosis and prompt treatment with antiviral medications are crucial to prevent severe neurological sequelae.
Ophthalmic Zoster
Ophthalmic zoster, involving the trigeminal nerve and the eye, can have potentially devastating consequences if left untreated. Prompt referral to an ophthalmologist is necessary to prevent or manage ocular complications, such as corneal scarring, glaucoma, and vision loss.
Neurological Complications
In rare cases, zoster infection can lead to neurological complications, such as stroke, cranial nerve palsies, and myelitis. These complications require specialized care and management by neurologists and other relevant specialists.
Interactions of Zoster-Herpes Virus with the Immune System
Zoster-herpes virus interacts closely with the immune system, and understanding these interactions is essential for the development of effective preventive and therapeutic strategies.
Cellular and Humoral Immune Response
The immune response to zoster-herpes virus involves both cellular and humoral components. T cells play a crucial role in the control and clearance of the virus, while antibody production helps prevent reinfection. Dysregulation of the immune response can result in viral reactivation and the development of clinical disease.
Immunosenescence
Immunosenescence, the gradual decline in immune function with age, is an important factor contributing to the increased risk of zoster infection in older individuals. Vaccination against varicella-zoster virus in older adults can help bolster the immune response and reduce the risk of developing zoster and its complications.
Implications for Vaccine Development
A deeper understanding of the immune response to zoster-herpes virus can guide the development of more effective vaccines. Research into novel vaccine formulations, including adjuvants and booster strategies, aims to enhance the immune response and provide longer-lasting protection against zoster.
Immunotherapy Approaches
Immunotherapy approaches, such as adoptive T cell therapy and antibody-based therapies, are being explored as potential treatments for zoster-herpes virus. These therapies aim to boost the immune response and improve clinical outcomes, particularly in individuals with severe or recurrent infections.
Recent Advances in Zoster-Herpes Virus Research
Recent research on zoster-herpes virus has provided valuable insights into the genomic studies, novel antiviral therapies, immunological aspects, and pain management innovations related to the disease.
Genomic Studies and Viral Evolution
Advancements in genomic studies have enabled researchers to better understand the molecular characteristics and evolution of zoster-herpes virus. This knowledge has important implications for our understanding of viral pathogenesis, transmission patterns, and potential drug targets.
Novel Antiviral Therapies
The development of novel antiviral therapies holds promise for the management of zoster-herpes virus. Research into new antiviral agents and targeted therapies is ongoing, with the aim of improving treatment outcomes and reducing the risk of complications.
Immunological Insights
Advances in immunological research have revealed intriguing insights into the immune response to zoster-herpes virus and its implications for disease progression and management. This knowledge can potentially guide the development of immunotherapies and vaccines.
Pain Management Innovations
Pain management is a crucial aspect of zoster-herpes virus treatment. Recent innovations in pain management techniques, including the use of neuropathic pain medications, topical agents, and neuromodulation, have improved pain control and quality of life for individuals with zoster.
In conclusion, zoster-herpes virus is a widespread and clinically significant infection that can cause chickenpox and shingles. Understanding the pathophysiology, clinical presentation, diagnostic methods, and treatment options for this virus is essential for healthcare professionals. Preventive measures, vaccination, and ongoing research are key in managing and mitigating the impact of this virus on public health.