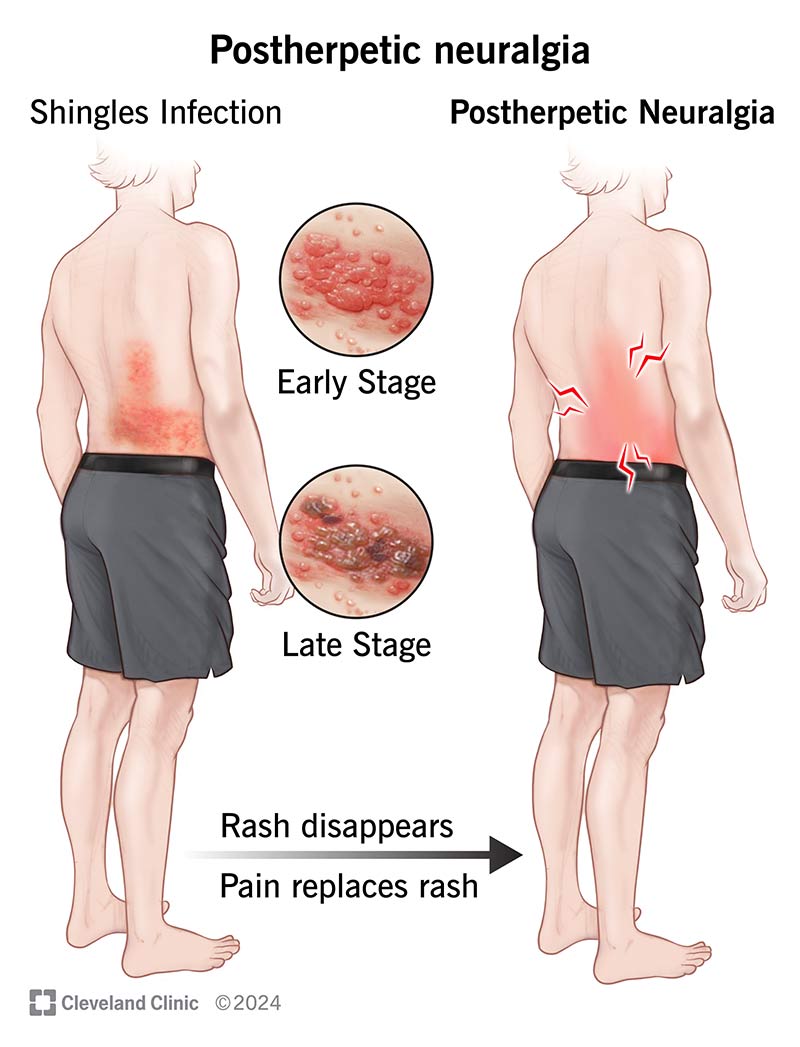
Imagine this scenario: you’ve recently recovered from a bout of shingles, the painful rash caused by the Zoster-Herpes Virus. Although you’ve beaten the infection, you start experiencing an unexpected lingering pain known as postherpetic neuralgia. Curious to find out why this is happening, you begin to wonder about the role of the Zoster-Herpes Virus in causing this discomfort. In this article, we will explore the connection between the virus and postherpetic neuralgia, shedding light on the link between your past infection and the lingering pain you’re currently experiencing.
Overview of Zoster-Herpes Virus
Zoster-Herpes Virus is a highly contagious viral infection caused by the Varicella-Zoster Virus (VZV), belonging to the family Herpesviridae. This virus is responsible for two distinct clinical entities: varicella (commonly known as chickenpox) and herpes zoster (also known as shingles). Both varicella and herpes zoster are characterized by a rash consisting of vesicles, but they differ in their clinical presentation and epidemiology.
Definition
Zoster-Herpes Virus refers to the infection caused by the Varicella-Zoster Virus (VZV). Varicella, also called chickenpox, occurs primarily in children, while herpes zoster, or shingles, is commonly seen in adults. The primary infection causes varicella, during which the virus establishes latency in the dorsal root ganglia and cranial nerve ganglia. Reactivation of the latent virus later in life leads to the development of herpes zoster.
Epidemiology
Varicella is a highly contagious disease that spreads through respiratory droplets or direct contact with the fluid from the vesicles. It is more prevalent in children but can affect individuals of any age. Conversely, herpes zoster occurs mainly in adults, particularly those over the age of 50 or individuals with compromised immune systems. It is estimated that approximately one in three people will experience herpes zoster during their lifetime.
Clinical Features
The clinical presentation of varicella is characterized by a pruritic rash, initially consisting of macules that progress into vesicles and eventually crust over. The rash typically starts on the trunk and spreads to other parts of the body. In contrast, herpes zoster presents as a painful rash that follows the distribution of the affected sensory nerve. The rash is typically unilateral and is characterized by grouped vesicles on an erythematous base. The pain associated with herpes zoster can be severe and long-lasting, leading to debilitating complications such as postherpetic neuralgia.
Transmission
Varicella is primarily transmitted through respiratory droplets or direct contact with the vesicular fluid of an infected individual. It is highly contagious and can easily spread in close-knit communities, such as schools or households. Herpes zoster, on the other hand, is caused by reactivation of the VZV from its latent form. The virus reactivates when the immune system becomes compromised or weakened, allowing the virus to travel along the affected sensory nerve and cause a new outbreak of shingles. Herpes zoster is not directly contagious, but a person with active shingles can transmit the virus to individuals who have not had varicella or have not been vaccinated against it, leading to the development of varicella in those individuals.
Pathogenesis of Zoster-Herpes Virus
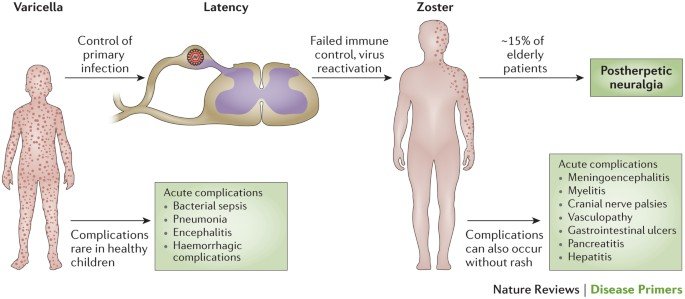
The pathogenesis of Zoster-Herpes Virus involves three key stages: primary infection, latency, and reactivation. Understanding these stages is crucial in comprehending the development of postherpetic neuralgia, a common complication of herpes zoster.
Primary Infection
Primary infection with VZV occurs when an individual without prior exposure to varicella or vaccination becomes infected. The virus enters the body through the respiratory tract and replicates in the regional lymph nodes. It then disseminates throughout the body via the bloodstream, leading to the characteristic generalized rash and systemic symptoms of varicella. During primary infection, the virus establishes latency in the dorsal root ganglia and cranial nerve ganglia.
Latency and Reactivation
Following primary infection, the VZV enters a latent phase in the sensory ganglia, where it remains dormant within the neurons. The reasons for viral reactivation are not fully understood, but it is believed to be related to age-related declines in immune function, immunosuppression, or other factors that compromise the host’s immune system. Reactivation involves viral replication and spread along the sensory nerve, leading to the clinical manifestations of herpes zoster.
Immune Response
The immune response plays a critical role in controlling the initial infection, maintaining viral latency, and limiting the severity and duration of reactivated disease. Both cellular and humoral immune responses are involved in the defense against VZV. T cells, particularly CD4+ T cells, play a vital role in controlling VZV infection by producing antiviral cytokines and promoting the cytotoxic activity of CD8+ T cells. Antibodies generated during primary infection or vaccination also contribute to the immune response against VZV.
Diagnosis of Zoster-Herpes Virus
The diagnosis of Zoster-Herpes Virus is primarily based on clinical assessment, supported by laboratory tests and imaging studies in certain cases.
Clinical Assessment
The clinical assessment of Zoster-Herpes Virus involves a detailed history and physical examination. The characteristic rash of varicella or herpes zoster, along with the associated symptoms, is often sufficient for clinical diagnosis. The distribution of the rash and the presence of pain are important features that can help differentiate herpes zoster from other dermatologic conditions.
Laboratory Tests
Laboratory tests can aid in the diagnosis of Zoster-Herpes Virus, particularly in cases where the clinical presentation is atypical or when complications are suspected. Viral culture, polymerase chain reaction (PCR), and serological assays, such as enzyme immunoassay (EIA), can be used to detect the presence of VZV and determine the immune status of the individual.
Imaging
Imaging studies, such as magnetic resonance imaging (MRI) or computed tomography (CT), are not routinely performed for the diagnosis of Zoster-Herpes Virus. However, they may be considered in certain cases, particularly when there are concerns about complications or involvement of specific anatomical structures, such as the central nervous system.
Postherpetic Neuralgia: Definition and Prevalence
Postherpetic neuralgia is a chronic neuropathic pain syndrome that occurs following an episode of herpes zoster. It is characterized by persistent pain in the affected dermatome that persists for more than three months after the rash has healed.
Definition of Postherpetic Neuralgia
Postherpetic neuralgia is defined as pain that persists for more than three months after the resolution of the herpes zoster rash. The pain is typically described as burning, aching, or shooting and is often accompanied by abnormal sensations, such as tingling or hypersensitivity, in the affected area.
Prevalence and Risk Factors
Postherpetic neuralgia is the most common complication of herpes zoster, affecting approximately 10-15% of individuals who experience an episode of shingles. The risk of developing postherpetic neuralgia increases with age, with individuals over the age of 60 being at the highest risk. Other risk factors include the severity of the acute herpes zoster infection, the presence of severe pain during the acute phase, and the involvement of certain dermatomes, such as the ophthalmic division of the trigeminal nerve.
Clinical Presentation
The clinical presentation of postherpetic neuralgia is characterized by chronic pain in the affected dermatome. The pain may be constant or intermittent and can range in severity from mild to excruciating. In addition to pain, individuals may also experience sensory abnormalities, such as numbness or hypersensitivity, as well as functional impairments and psychological distress.

Pathophysiology of Postherpetic Neuralgia
The pathophysiology of postherpetic neuralgia is multifactorial and involves a combination of nerve damage, persistent inflammation, and neurochemical imbalances.
Nerve Damage
Nerve damage is thought to play a crucial role in the development of postherpetic neuralgia. The Varicella-Zoster Virus can directly damage neurons, resulting in altered neural signaling and the generation of abnormal pain signals. Additionally, the inflammatory response triggered by the virus can lead to further damage to the nerves, contributing to the persistence of pain.
Persistent Inflammation
The inflammatory response induced by the Varicella-Zoster Virus during the acute phase of herpes zoster can persist even after the resolution of the rash. This chronic inflammation can contribute to the ongoing sensitization of the nerves, leading to prolonged pain and the development of postherpetic neuralgia.
Neurochemical Imbalance
In individuals with postherpetic neuralgia, there may be imbalances in certain neurotransmitters and neuropeptides involved in modulating pain signals. These imbalances can contribute to the amplification and persistence of pain signals, resulting in the chronic pain experienced in postherpetic neuralgia.
Role of Zoster-Herpes Virus in Postherpetic Neuralgia
The involvement of the Zoster-Herpes Virus in the development of postherpetic neuralgia is complex and multifactorial. Several mechanisms have been proposed to explain the relationship between the virus and the development of chronic pain.
Virus Persistence at Dorsal Root Ganglia
Following the primary infection, the Varicella-Zoster Virus establishes latency within the neurons of the dorsal root ganglia. During reactivation, the virus replicates and spreads along the sensory nerve, causing inflammation and damage to the nerve fibers. This persistent viral presence and the associated inflammatory response are believed to contribute to the development and maintenance of postherpetic neuralgia.
Neuronal Apoptosis
Apoptosis, or programmed cell death, of sensory neurons is thought to be involved in the pathogenesis of postherpetic neuralgia. It is believed that the Varicella-Zoster Virus infection leads to the activation of apoptotic pathways in the sensory neurons, resulting in the loss of these neurons and the disruption of normal sensory processing. The loss of sensory neurons can contribute to the altered pain signaling and the development of chronic pain in postherpetic neuralgia.
Inflammatory Responses
The inflammatory responses triggered by the Varicella-Zoster Virus, both during the acute phase of herpes zoster and in the persistent inflammation seen in postherpetic neuralgia, play a significant role in the development and maintenance of chronic pain. The release of pro-inflammatory molecules, such as cytokines and chemokines, can sensitize the peripheral nerves and contribute to the amplification of pain signals.

Clinical Manifestations of Postherpetic Neuralgia
Postherpetic neuralgia is characterized by a range of clinical manifestations that go beyond chronic pain in the affected dermatome.
Pain Characteristics
The pain in postherpetic neuralgia is typically described as burning, aching, or shooting. It may be constant or intermittent and can vary in intensity. The pain is often severe and can significantly impact the quality of life of affected individuals.
Sensory Abnormalities
In addition to pain, individuals with postherpetic neuralgia may experience sensory abnormalities in the affected area. These abnormalities can include numbness, tingling, itching, or increased sensitivity to touch or temperature changes.
Functional Impairments
The chronic pain and sensory abnormalities associated with postherpetic neuralgia can lead to functional impairments. Activities such as dressing, bathing, or even simple movements may be challenging or painful to perform, affecting the individual’s independence and overall quality of life.
Psychological Impact
The constant pain and functional limitations caused by postherpetic neuralgia can have a significant psychological impact on affected individuals. It is not uncommon for individuals with postherpetic neuralgia to experience depression, anxiety, social isolation, and a reduced overall quality of life.
Diagnostic Criteria and Assessment of Postherpetic Neuralgia
The diagnosis and assessment of postherpetic neuralgia involve a combination of clinical criteria and various assessment tools.
International Association for the Study of Pain (IASP) Criteria
The International Association for the Study of Pain (IASP) has established diagnostic criteria for postherpetic neuralgia. According to these criteria, the pain must persist for more than three months following the resolution of the herpes zoster rash, be located within the dermatome affected by the shingles, and be neuropathic in nature.
Pain Assessment Scales
To assess the severity and impact of pain in postherpetic neuralgia, various pain assessment scales can be used. These scales, such as the Numerical Rating Scale (NRS) or the Visual Analog Scale (VAS), allow individuals to rate their pain intensity on a scale from 0 to 10. Additionally, pain assessment tools that evaluate pain-related interference in daily activities, such as the Brief Pain Inventory (BPI), can provide a more comprehensive understanding of the individual’s pain experience.
Functional and Psychological Assessments
Assessing the functional impairments and the psychological impact of postherpetic neuralgia can be achieved through the use of validated questionnaires and interviews. These assessments help determine the individual’s level of disability, the impact of pain on daily activities, and the presence of psychological distress, allowing for a more holistic approach to the management of postherpetic neuralgia.

Treatment Strategies for Postherpetic Neuralgia
The management of postherpetic neuralgia aims to alleviate pain, improve function, and enhance the overall quality of life. Treatment strategies often involve a multimodal approach, combining pharmacological, interventional, and psychological interventions.
Antiviral Therapy
Antiviral therapy, such as oral acyclovir, valacyclovir, or famciclovir, may be prescribed during the acute phase of herpes zoster to reduce viral replication and potentially mitigate the severity and duration of postherpetic neuralgia. However, the effectiveness of antiviral therapy in preventing or treating postherpetic neuralgia remains a topic of debate.
Analgesics and Adjuvants
Pharmacological interventions for postherpetic neuralgia typically include the use of analgesics, such as nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, or anticonvulsants. These medications can help relieve pain and improve functional outcomes. Additionally, adjuvant medications, such as tricyclic antidepressants or serotonin-norepinephrine reuptake inhibitors (SNRIs), may be prescribed to target neuropathic pain.
Interventional Procedures
In cases where pain is severe and refractory to pharmacological therapies, interventional procedures may be considered. These procedures, such as nerve blocks, neurolytic blocks, or spinal cord stimulation, aim to interrupt or modulate the pain signals and provide long-term pain relief.
Psychological Interventions
Psychological interventions, such as cognitive-behavioral therapy (CBT) or mindfulness-based stress reduction, can help individuals with postherpetic neuralgia cope with chronic pain, improve their psychological well-being, and enhance their overall quality of life. These interventions focus on changing thought patterns, developing coping skills, and promoting relaxation techniques to reduce pain-related distress.
Prevention and Vaccination
Prevention of Zoster-Herpes Virus and its complications, including postherpetic neuralgia, is possible through vaccination.
Varicella-Zoster Virus (VZV) Vaccination
Varicella-Zoster Virus (VZV) vaccination is highly effective in reducing the incidence and severity of varicella. The vaccine contains attenuated live VZV, which stimulates the immune system to produce a protective immune response. By preventing primary infection, VZV vaccination can also reduce the risk of herpes zoster and subsequently postherpetic neuralgia.
Vaccination Recommendations
Vaccination against VZV is recommended for individuals who have not had varicella or have not been previously vaccinated. The vaccine is routinely administered to children at specific ages, but individuals who have reached adolescence or adulthood and have not been vaccinated can also benefit from vaccination. Additionally, a specifically formulated vaccine, known as the zoster vaccine, is available for adults aged 50 and older to prevent herpes zoster and reduce the risk of postherpetic neuralgia.
Effectiveness of Vaccination
VZV vaccination has proven to be highly effective in preventing varicella and reducing the risk of herpes zoster. Studies have demonstrated that vaccination significantly decreases the incidence of varicella and its complications, including postherpetic neuralgia. Additionally, the zoster vaccine has been shown to reduce the risk of herpes zoster and postherpetic neuralgia in adults aged 50 and older.
In conclusion, Zoster-Herpes Virus, caused by the Varicella-Zoster Virus, is a significant infectious disease that can manifest as varicella or herpes zoster. While varicella primarily affects children, herpes zoster predominantly affects adults, particularly those over the age of 50 or with compromised immune systems. Herpes zoster can lead to the development of postherpetic neuralgia, a chronic neuropathic pain syndrome. The pathogenesis of postherpetic neuralgia involves nerve damage, persistent inflammation, and neurochemical imbalances. The Zoster-Herpes Virus is directly implicated in the development of postherpetic neuralgia through virus persistence, neuronal apoptosis, and the inflammatory response. Postherpetic neuralgia is characterized by chronic pain, sensory abnormalities, functional impairments, and psychological distress. Diagnosis and assessment of postherpetic neuralgia involve clinical criteria, pain assessment scales, and functional and psychological assessments. Treatment strategies for postherpetic neuralgia include antiviral therapy, analgesics and adjuvants, interventional procedures, and psychological interventions. Vaccination against the Varicella-Zoster Virus is an effective measure for preventing varicella, herpes zoster, and postherpetic neuralgia, particularly in susceptible populations.