In “Preventing Disability Progression in Ankylosing Spondylitis: Key Strategies and Therapies,” you’ll discover the crucial approaches and treatments that can help in preventing the progression of disability in Ankylosing Spondylitis. With an emphasis on empowering individuals with the necessary tools, this article aims to provide valuable insights into managing this chronic inflammatory disease. By exploring key strategies and therapies, you’ll gain a better understanding of how to effectively combat the symptoms and maintain a fulfilling, active lifestyle.
Early Diagnosis and Treatment
Ankylosing Spondylitis (AS) is a chronic inflammatory disease that primarily affects the spine, causing pain, stiffness, and eventually leading to spinal fusion and deformities. Early diagnosis and prompt treatment play a crucial role in managing the symptoms and preventing long-term complications associated with AS.
Importance of early diagnosis
Early diagnosis of AS allows for early intervention and the implementation of appropriate treatment strategies to alleviate pain, improve mobility, and slow down the progression of the disease. Recognizing the signs and symptoms of AS in its early stages is key to preventing disability and enhancing the overall quality of life for individuals living with this condition.
Diagnostic criteria for ankylosing spondylitis
AS is diagnosed based on a combination of clinical history, physical examination, and imaging tests. The most commonly used diagnostic criteria is the modified New York criteria, which includes the presence of chronic back pain for more than three months, morning stiffness, improvement with exercise, and radiographic evidence of sacroiliitis.
Role of healthcare professionals in early detection
Healthcare professionals, including rheumatologists and primary care physicians, play a crucial role in the early detection of AS. By actively listening to patients’ concerns, conducting a thorough physical examination, and ordering appropriate diagnostic tests, healthcare professionals can identify AS in its early stages and initiate the appropriate treatment plan promptly.
Treatment options for managing symptoms
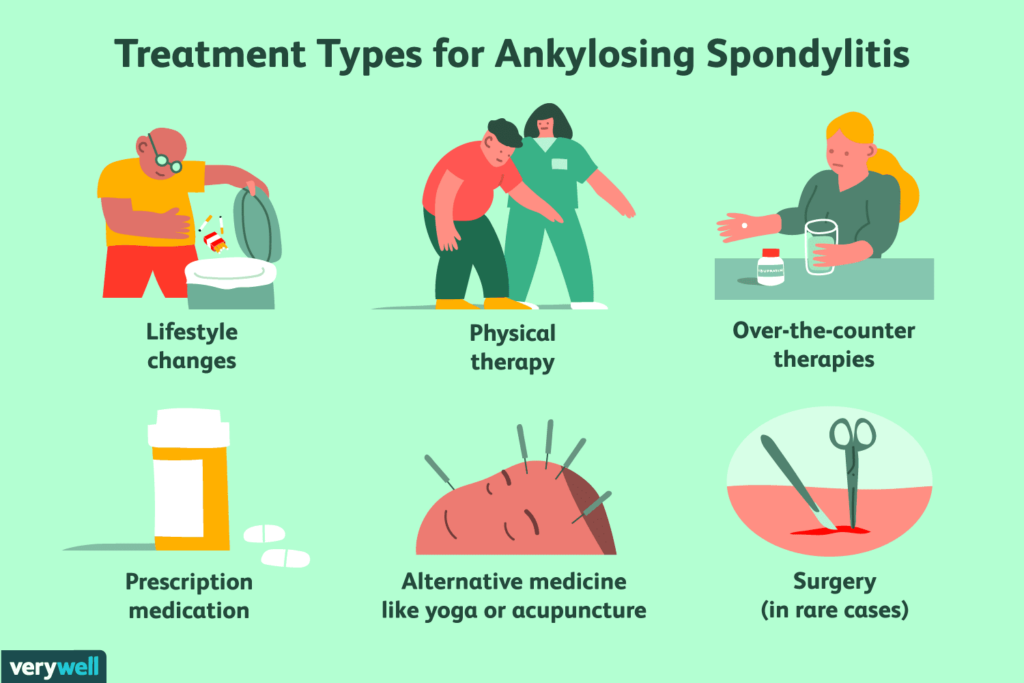
While there is currently no cure for AS, several treatment options are available to manage symptoms and slow down disease progression. The choice of treatment depends on the severity of symptoms and individual patient factors. The main treatment modalities for AS include exercise, physical therapy, medications, diet and nutrition, rest and sleep, stress management, posture and ergonomics, surgery (as a last resort), and a multidisciplinary approach.
Physical Therapy and Exercise
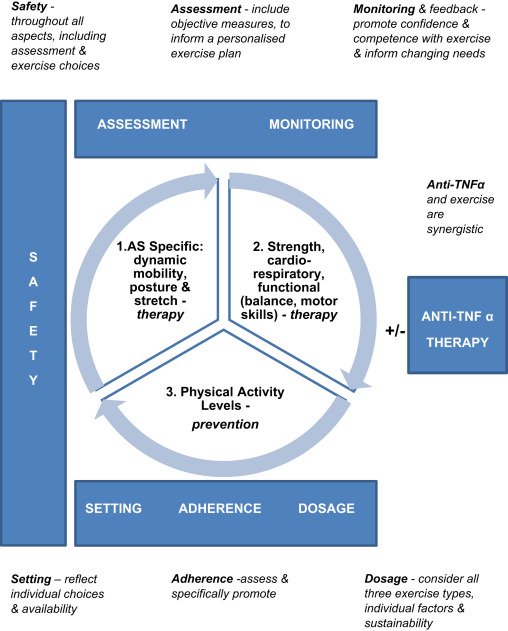
Physical therapy and regular exercise are vital components in managing ankylosing spondylitis. These interventions aim to improve flexibility, posture, and overall physical functioning while reducing pain and stiffness associated with AS.
Role of physical therapy in managing ankylosing spondylitis
Physical therapy plays a crucial role in the management of AS by focusing on reducing pain, improving posture, increasing flexibility, and enhancing overall physical functioning. Physical therapists design individualized exercise programs tailored to the specific needs of AS patients, ensuring optimal outcomes and enhancing their overall quality of life.
Benefits of exercise for ankylosing spondylitis patients
Exercise offers numerous benefits for individuals with AS. Regular physical activity helps maintain joint flexibility, reduce stiffness, improve muscle strength, enhance posture, and promote overall cardiovascular health. Exercise also plays a pivotal role in managing and reducing pain, improving mood, and increasing energy levels.
Types of exercises recommended
A combination of stretching, strengthening, and cardiovascular exercises is typically recommended for individuals with AS. Stretching exercises help maintain and improve joint flexibility, while strengthening exercises target the muscles surrounding the affected joints, enhancing stability and support. Additionally, cardiovascular exercises such as swimming or cycling can improve cardiovascular fitness without putting excessive stress on the joints.
Best practices for physical therapy sessions
When undergoing physical therapy for AS, it is important to communicate openly with your physical therapist about your symptoms, limitations, and goals. This enables them to tailor the exercise program, make adjustments as needed, and address any concerns or challenges you may be experiencing. It is also crucial to follow the prescribed exercise regimen diligently and attend therapy sessions regularly for maximum benefit.
Medication Options
In addition to exercise and physical therapy, medications are often prescribed to manage pain and inflammation associated with ankylosing spondylitis. Various types of medications can be used, either individually or in combination, to alleviate symptoms and improve overall well-being.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly used to manage pain, stiffness, and inflammation in AS. They work by reducing the production of prostaglandins, which are responsible for pain and inflammation. NSAIDs can provide short-term relief and improve overall mobility, allowing individuals with AS to engage in physical activity and maintain a better quality of life.
Biologic medicines
Biologic medicines, also known as biologic response modifiers, are a type of medication that targets specific components of the immune system involved in the inflammatory process of AS. They are typically administered via injections or infusions and may help reduce pain, inflammation, and disease activity. Biologics have shown promising results in managing symptoms and slowing down the progression of AS in individuals who have not responded adequately to NSAIDs.
Pain medications and muscle relaxants
For individuals experiencing severe pain and muscle spasms, pain medications and muscle relaxants may be prescribed to provide temporary relief. These medications can help alleviate pain and promote relaxation, allowing individuals to engage in physical therapy and exercise more comfortably.
Steroids
Steroids, such as corticosteroids, are occasionally used in the treatment of AS to quickly suppress inflammation and relieve pain. However, their long-term use is generally not recommended due to potential side effects and limited efficacy in managing the disease.
DMARDs (Disease-Modifying Antirheumatic Drugs)
Disease-Modifying Antirheumatic Drugs (DMARDs) are a class of medications used to slow down the progression of AS and prevent joint damage. DMARDs work by modulating the immune system and targeting the underlying mechanisms of the disease. Methotrexate, sulfasalazine, and leflunomide are some examples of DMARDs that may be prescribed in certain cases of AS.
Diet and Nutrition
Although diet alone cannot cure ankylosing spondylitis, adopting a healthy and anti-inflammatory diet can contribute to symptom management and overall well-being. Proper nutrition plays a crucial role in supporting the immune system, reducing inflammation, and maintaining optimal weight.
Anti-inflammatory diet
An anti-inflammatory diet focuses on consuming whole, unprocessed foods that are rich in nutrients and have anti-inflammatory properties. This typically includes fresh fruits and vegetables, lean proteins, healthy fats, whole grains, and limited consumption of processed foods, refined sugars, and saturated fats.
Importance of a well-balanced diet
Eating a well-balanced diet is crucial for individuals with AS as it provides essential nutrients needed for overall health and well-being. A well-balanced diet that includes a variety of nutrient-dense foods can support the immune system, reduce inflammation, promote healthy weight management, and improve overall energy levels.
Foods to avoid
Certain foods may trigger inflammation or worsen symptoms in individuals with AS. It is advisable to limit or avoid foods high in saturated fats, trans fats, refined sugars, and processed ingredients. Additionally, some people with AS may be sensitive to specific foods such as nightshade vegetables (e.g., tomatoes, peppers, and eggplants) and gluten, and may benefit from eliminating or reducing their consumption.
Nutritional supplements
In some cases, nutritional supplements may be recommended to ensure adequate intake of essential nutrients. Omega-3 fatty acids, vitamin D, and calcium supplements are commonly advised for individuals with AS to support joint health, reduce inflammation, and promote bone density.
Rest and Sleep
Adequate rest and quality sleep are essential for individuals with ankylosing spondylitis. Resting allows the body to recuperate, while proper sleep is crucial for overall health, pain management, and disease control.
Importance of rest in managing ankylosing spondylitis
Rest is essential for individuals with AS to manage their symptoms and prevent fatigue. While regular physical activity and exercise are important, it is equally important to listen to your body’s signals and allow yourself sufficient rest to manage pain and reduce the risk of flare-ups.
Creating a conducive sleep environment
Creating a conducive sleep environment can significantly impact the quality of sleep for individuals with AS. This includes ensuring a comfortable mattress and pillows that provide adequate support, maintaining a cool and dark sleeping environment, and minimizing noise and distractions.
Sleep hygiene practices
Adopting good sleep hygiene practices can help individuals with AS achieve restful sleep. This includes establishing a regular sleep schedule, avoiding stimulants like caffeine before bedtime, engaging in relaxing activities before sleep, and practicing relaxation techniques, such as deep breathing or meditation.
Benefits of rest and adequate sleep
Adequate rest and quality sleep have numerous benefits for individuals with AS. They help reduce pain, improve mood and mental health, enhance cognitive function, boost energy levels, and support overall immune system function. Prioritizing rest and sleep can contribute to better disease management and an improved quality of life.
Stress Management
Stress can significantly impact AS symptoms, triggering flare-ups and worsening pain and inflammation. Therefore, it is crucial for individuals with AS to develop effective stress management techniques to reduce the impact of stress on their physical and mental well-being.
Impact of stress on ankylosing spondylitis symptoms
Stress can exacerbate AS symptoms by increasing muscle tension, promoting inflammation, and compromising the immune system. It is important to recognize the connection between stress levels and AS symptoms, and actively manage stress to minimize its impact on the disease.
Techniques for stress reduction
There are various stress reduction techniques that can be beneficial for individuals with AS. These include deep breathing exercises, meditation, mindfulness, yoga, tai chi, and other relaxation techniques. Engaging in activities that promote relaxation and provide an outlet for stress, such as hobbies, socializing, or listening to music, can also help alleviate stress.
Mind-body therapies
Mind-body therapies, such as cognitive-behavioral therapy (CBT) and relaxation techniques, can be effective in managing stress and improving coping mechanisms for individuals with AS. These therapies focus on identifying and modifying negative thought patterns, promoting positive behaviors, and enhancing overall emotional well-being.
Support groups and counseling
Joining support groups or seeking counseling can provide individuals with AS an opportunity to connect with others who understand their experiences, share strategies for managing stress, and offer emotional support. Counseling can be particularly beneficial in addressing any emotional or psychological challenges that may arise from living with a chronic condition like AS.
Posture and Ergonomics
Maintaining good posture and ensuring ergonomic adaptations in both work and home environments are essential for individuals with AS. Proper posture and ergonomic practices help minimize strain on the spine, reduce pain, and prevent the development of spinal deformities.
Maintaining good posture
Maintaining good posture involves aligning the spine in a neutral position during various activities. This includes sitting up straight with the shoulders relaxed, avoiding excessive slouching or hunching, and maintaining proper alignment while standing and walking. Regularly practicing good posture can help reduce back pain and contribute to overall spinal health.
Ergonomic adaptations for work and home environments
Making ergonomic adaptations in work and home environments can significantly improve comfort and reduce strain on the spine. This can include using ergonomic chairs and adjustable desks, positioning computer monitors at eye level, using supportive cushions or lumbar rolls, and arranging workspaces to minimize unnecessary reaching or twisting motions.
Assistive devices for improved posture
Assistive devices, such as lumbar supports, orthotic shoe inserts, and back braces, can provide additional support and improve posture for individuals with AS. These devices can help alleviate pain, reduce pressure on the spine, and promote proper alignment during activities of daily living.
Preventing spinal deformities
Maintaining good posture, regularly engaging in exercises that promote spinal mobility and flexibility, and utilizing ergonomic adaptations can help prevent the development of spinal deformities in individuals with AS. Early intervention and proactive measures can significantly impact the long-term prognosis and overall quality of life for those living with this condition.
Surgery as a Last Resort
In some cases, surgery may be considered for individuals with ankylosing spondylitis when conservative treatment options have been exhausted or when severe joint damage or debilitating symptoms occur. Surgical intervention aims to improve function, reduce pain, correct deformities, and enhance overall quality of life.
When surgery may be considered
Surgery may be considered in individuals with AS when conservative treatment options fail to provide adequate relief and symptoms significantly impact daily life. Surgical intervention is typically reserved for cases involving severe joint damage, spinal fusion, instability, or disabling symptoms that significantly impact mobility and quality of life.
Types of surgical procedures
Different surgical procedures may be performed depending on the specific needs of the individual. Total hip replacement or knee replacement may be necessary to address severe joint damage, while spinal fusion surgery aims to stabilize the spine and correct deformities. Surgical correction of kyphosis or scoliosis may also be performed to improve posture and alleviate pain.
Risks and benefits of surgery
Like any surgical procedure, there are risks and benefits associated with surgery for ankylosing spondylitis. While surgery can provide significant relief and improve overall functionality, potential risks include infection, bleeding, complications related to anesthesia, and prolonged recovery periods. It is crucial for individuals considering surgery to thoroughly discuss the potential risks and benefits with their healthcare provider.
Post-surgical rehabilitation
Following surgery, rehabilitation plays a vital role in the recovery process. Physical therapy and specific rehabilitation exercises are typically prescribed to improve strength, flexibility, and mobility. Post-surgical rehabilitation programs are individually tailored to the needs and limitations of the individual and are designed to optimize the surgical outcomes and promote a swift return to daily activities.
Combining Therapies for Optimal Results
An integrated and multidisciplinary approach that combines various therapeutic strategies is often the most effective way to manage ankylosing spondylitis. Combining therapies allows for a comprehensive and personalized approach that targets different aspects of the disease.
Multidisciplinary approach in treating ankylosing spondylitis
A multidisciplinary approach involves collaboration between healthcare professionals from different specialties, including rheumatologists, physiotherapists, occupational therapists, nutritionists, and mental health professionals. This approach ensures a holistic assessment and addresses the diverse needs of individuals with AS, resulting in a more comprehensive and effective treatment plan.
Creating an individualized treatment plan
Each individual with AS is unique, and an individualized treatment plan is essential to address specific symptoms, limitations, and preferences. By considering a person’s medical history, symptom severity, lifestyle factors, and treatment goals, healthcare professionals can develop a personalized treatment plan that optimizes outcomes and improves overall quality of life.
Collaboration between healthcare professionals
Collaboration between healthcare professionals is critical in managing ankylosing spondylitis effectively. Regular communication and coordination between rheumatologists, physical therapists, occupational therapists, and other healthcare providers ensure that all aspects of an individual’s condition are addressed, and treatment strategies are adjusted as needed.
Monitoring and adjusting treatment strategies
Regular monitoring and evaluation of treatment outcomes allow healthcare professionals to assess the effectiveness of different interventions and make necessary adjustments to the treatment plan. This ensures that individuals with AS receive the most appropriate and up-to-date care and enables healthcare professionals to optimize treatment strategies as needed.
Regular Monitoring and Follow-Up
Regular check-ups and assessments are essential for individuals with ankylosing spondylitis to track disease progression, identify early signs of disability, and modify treatment plans accordingly. Monitoring and follow-up appointments allow healthcare professionals to closely monitor the status of the disease and make timely interventions if necessary.
Importance of regular check-ups and assessments
Regular check-ups and assessments enable healthcare professionals to monitor disease activity, evaluate the response to treatment, and identify any early signs of complications. These appointments also serve as an opportunity for individuals with AS to discuss any concerns or changes in their condition and receive appropriate guidance and support.
Monitoring disease progression
Through regular monitoring, healthcare professionals can track disease progression, assess joint involvement, and identify any potential complications associated with ankylosing spondylitis. Monitoring typically involves physical examinations, imaging studies, and laboratory tests to evaluate disease activity and determine the impact on physical functioning.
Detecting early signs of disability
Detecting early signs of disability is crucial in preventing long-term complications and maintaining functional independence for individuals with AS. Regular monitoring allows healthcare professionals to identify any limitations in physical functioning, assess mobility and posture, and formulate appropriate strategies to minimize disability.
Modifying treatment plan based on evaluation results
Regular monitoring and follow-up visits provide an opportunity to evaluate the effectiveness of the current treatment plan and make any necessary adjustments. Healthcare professionals can modify the treatment plan based on evaluation results, such as changes in disease activity, symptom severity, or the individual’s response to medications or physical therapy.
In conclusion, the comprehensive management of ankylosing spondylitis involves early diagnosis, multidisciplinary treatment approaches, regular physical therapy and exercise, appropriate medication options, a healthy diet, sufficient rest and sleep, effective stress management, proper posture and ergonomics, a last resort involving surgery, and combining therapies for optimal results. With a proactive and personalized approach to treatment, individuals with ankylosing spondylitis can better manage their symptoms, slow down disease progression, and improve their overall quality of life. Regular monitoring and follow-up appointments are essential to track disease progression, detect early signs of disability, and modify treatment plans accordingly. By implementing these strategies, individuals with AS can enhance their well-being and prevent disability progression.