You’ve probably heard of it before, but do you really know what Ankylosing Spondylitis is? In this article, we’ll shed some light on this chronic condition that affects the spine and other joints in the body. From exploring its causes to examining the symptoms to discussing the various treatment options available, we’ll provide you with all the information you need to better understand Ankylosing Spondylitis and how it can be managed. So, let’s dive in and get to know this condition a little better.

Understanding Ankylosing Spondylitis
Ankylosing Spondylitis (AS) is a chronic inflammatory disease that primarily affects the spine, causing pain and stiffness. It falls under the category of seronegative spondyloarthropathies, which refers to a group of conditions that affect the spine and joints. AS usually starts in early adulthood and can lead to significant disability if left untreated. It is important to understand the prevalence, risk factors, causes, symptoms, diagnosis, treatment options, and complications associated with this condition to effectively manage it and improve quality of life.
Overview of Ankylosing Spondylitis
AS primarily affects the spine, causing inflammation in the joints and ligaments. This leads to the fusion of the vertebrae, resulting in reduced mobility and flexibility. However, AS can also affect other parts of the body such as the hips, shoulders, and knees. The symptoms of AS can vary from person to person, with some individuals experiencing mild discomfort while others may suffer from severe pain and mobility limitations. Early diagnosis and appropriate treatment are crucial in minimizing the impact of AS on daily life.
Prevalence of Ankylosing Spondylitis
AS is not a widely known condition, but it is estimated that around 0.1% to 0.5% of the general population may have AS. It is more common in men than in women, with a male-to-female ratio of 2:1. The onset of symptoms typically occurs between the ages of 15 and 45, although it can also affect children and older adults. AS is more prevalent in certain ethnic groups, including Caucasians, Native Americans, and individuals of Asian descent. The exact cause of this disparity is still under investigation.
Risk Factors of Ankylosing Spondylitis
While the exact cause of AS is unknown, there are several risk factors that may increase the likelihood of developing the condition. These include genetic factors and environmental factors.
Genetic Factors
One of the strongest risk factors for AS is the presence of the HLA-B27 gene. HLA-B27 is a genetic marker that is found in 90-95% of individuals with AS, although it is important to note that not all individuals with this gene develop the condition. Having a family history of AS also increases the risk of developing the disease, suggesting a hereditary component.
Environmental Factors
Environmental factors may also play a role in the development of AS. Some studies have shown a potential link between bacterial infections, such as those caused by Klebsiella or Escherichia coli, and the onset of AS. Additionally, smoking has been identified as a potential environmental risk factor, as it can worsen the symptoms and progression of the disease.
Causes of Ankylosing Spondylitis
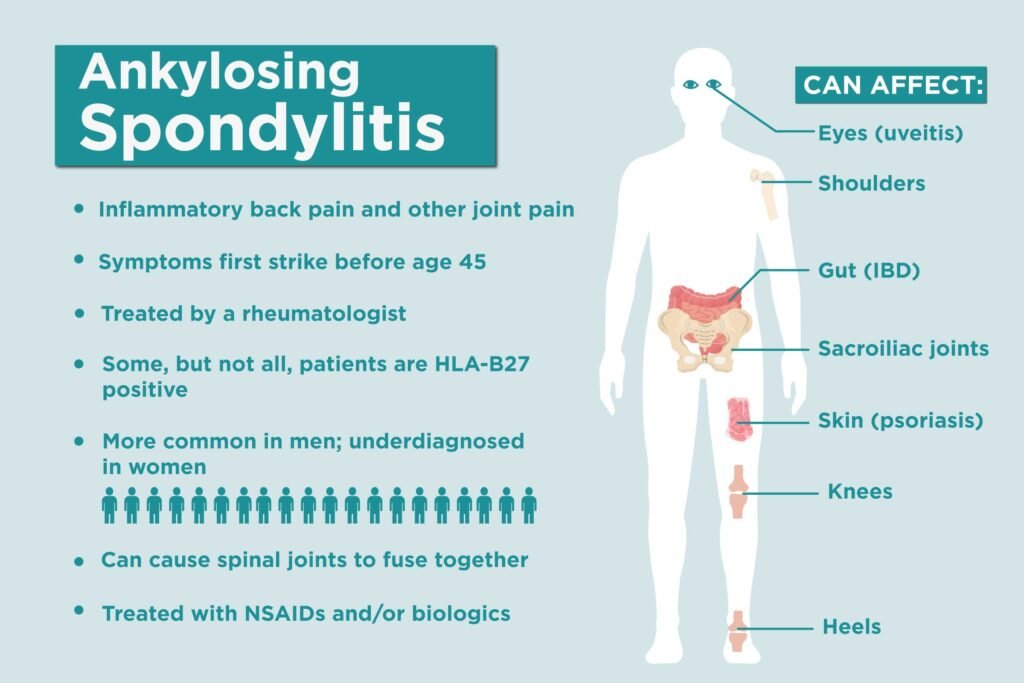
While the exact cause of AS remains unknown, research suggests that a combination of genetic and environmental factors contribute to its development. Three main factors are believed to be involved in the pathogenesis of AS: the HLA-B27 gene, an autoimmune response, and inflammation in the joints.
HLA-B27 Gene
The presence of the HLA-B27 gene is strongly associated with AS, suggesting a genetic predisposition to the disease. HLA-B27 is an antigen-presenting molecule that plays a key role in the immune system. It is believed that individuals with the HLA-B27 gene have an abnormal immune response, leading to the inflammation and joint damage characteristic of AS.
Autoimmune Response
AS is considered an autoimmune disorder, which means that the immune system mistakenly attacks its own healthy tissues. In AS, the immune system targets the joints and ligaments of the spine, causing inflammation and damage. The exact triggers for this autoimmune response are still under investigation.
Inflammation in Joints
Inflammation in the joints is a hallmark feature of AS. The immune system produces proteins called cytokines, which stimulate inflammation in the affected joints. This inflammation leads to the release of enzymes that cause damage to the bone and cartilage, eventually leading to the fusion of the vertebrae.
Symptoms of Ankylosing Spondylitis
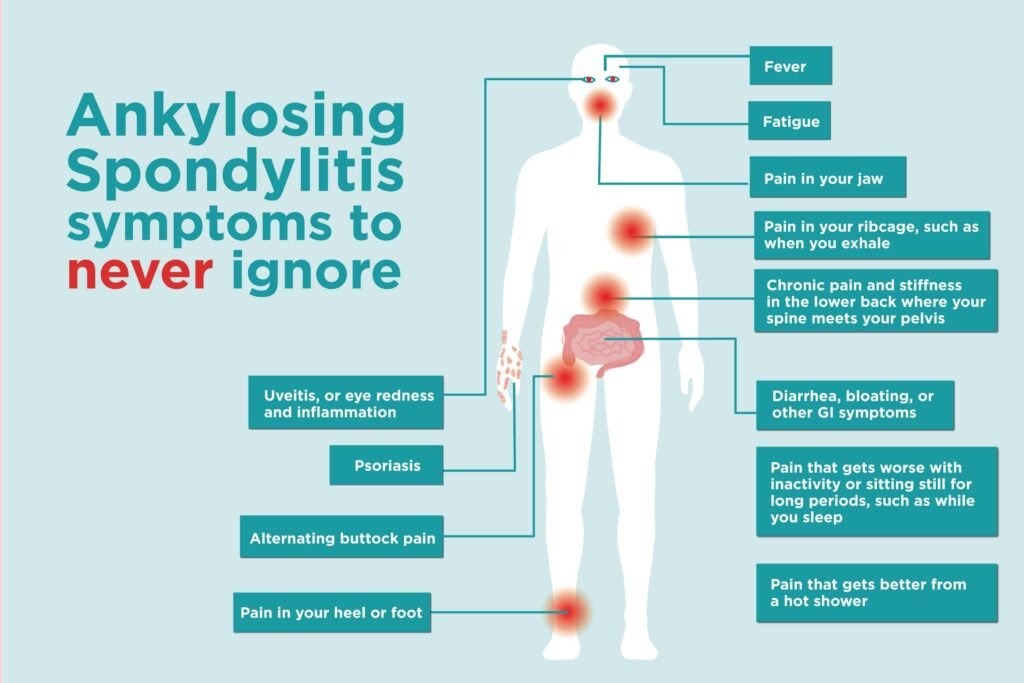
AS can cause a wide range of symptoms, which can vary from person to person. The symptoms can be divided into three categories: early symptoms, chronic symptoms, and extra-articular symptoms.
Early Symptoms
The early symptoms of AS often include persistent low back pain and stiffness that are worse in the morning or after periods of rest. This pain and stiffness can gradually develop over several months and may be accompanied by fatigue. Some individuals may experience pain and stiffness in the neck or other joints, such as the hips or shoulders.
Chronic Symptoms
As AS progresses, it can lead to chronic pain and stiffness in the spine and other affected joints. The pain may worsen with prolonged inactivity or when resting. Decreased mobility and flexibility are common, making it difficult to perform daily activities. In severe cases, the spine may become fused, resulting in a stooped posture and limited movement.
Extra-articular Symptoms
In addition to joint-related symptoms, AS can also cause extra-articular symptoms that affect other parts of the body. These may include inflammation in the eyes (uveitis), chest pain caused by inflammation of the rib joints (costochondritis), and bowel inflammation (inflammatory bowel disease).

Diagnosis of Ankylosing Spondylitis
Diagnosing AS can be challenging due to its variable and overlapping symptoms. A combination of medical history, physical examination, blood tests, imaging tests, and HLA-B27 testing is typically used to reach a diagnosis.
Medical History
The doctor will gather information about your symptoms, including the location, duration, and severity of pain or stiffness. They will also inquire about any family history of AS or other autoimmune diseases.
Physical Examination
During a physical examination, the doctor will assess your range of motion, flexibility, and the presence of specific signs associated with AS, such as limited chest expansion. They may also examine your joints, including the spine, to check for tenderness or swelling.
Blood Tests
Blood tests may be conducted to check for inflammation markers, such as erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP). The HLA-B27 gene may also be tested, although it is important to note that a positive result does not confirm the diagnosis, as some individuals without AS also have this gene.
Imaging Tests
Imaging tests, such as X-rays and magnetic resonance imaging (MRI), can help visualize the inflammation and damage to the joints and spine. X-rays may show changes in the sacroiliac joints, while MRI can provide more detailed images of the affected areas.
HLA-B27 Testing
HLA-B27 testing may be used as a supportive tool in the diagnosis of AS. However, it should be interpreted in conjunction with other clinical findings, as a positive result does not necessarily mean that you have AS.
Treatment of Ankylosing Spondylitis
While there is currently no cure for AS, treatment options are available to manage symptoms, improve mobility, and slow down the progression of the disease.
Medications
Nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly prescribed to reduce pain and inflammation in AS. They can help relieve symptoms and improve joint mobility. In some cases, disease-modifying antirheumatic drugs (DMARDs) may be prescribed to slow down the progression of joint damage. In severe cases, biologic therapies, which target specific immune system proteins, may be considered.
Physical Therapy
Physical therapy plays a crucial role in managing AS. A physical therapist can design an exercise program tailored to your specific needs, focusing on improving posture, flexibility, and strength. They may also teach you techniques to improve mobility and manage pain.
Exercise
Regular exercise is important for individuals with AS, as it helps maintain joint flexibility, improve posture, and alleviate stiffness. Low-impact activities such as swimming, walking, and cycling are recommended. It is important to consult with a healthcare professional before starting any exercise program.
Surgery
In rare cases, surgery may be considered for individuals with severe AS who do not respond to other treatment options. Surgical interventions, such as joint replacement or spinal fusion, can help improve mobility and reduce pain.
Pain Management in Ankylosing Spondylitis
Managing pain in AS is a key aspect of treatment. Various medications and pain relief techniques can be used to alleviate discomfort and improve quality of life.
Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
NSAIDs, such as ibuprofen and naproxen, are often the first line of treatment for pain management in AS. They help reduce pain and inflammation in the affected joints. However, long-term use of NSAIDs should be monitored, as they can have potential side effects on the gastrointestinal system.
Corticosteroids
Corticosteroids may be used to provide short-term pain relief in individuals with severe pain or inflammation. They can be administered orally, intravenously, or through injections directly into the affected joints.
Disease-Modifying Antirheumatic Drugs (DMARDs)
DMARDs, such as sulfasalazine or methotrexate, may be prescribed to individuals with AS who do not respond adequately to NSAIDs. These medications help slow down the progression of joint damage and reduce inflammation.
Biologic Therapies
Biologic therapies, also known as biologics, are a newer class of medications used to target specific immune system proteins involved in the inflammatory process. They are often reserved for individuals with moderate to severe AS who do not respond to other treatments.
Pain Relief Techniques
In addition to medications, various pain relief techniques can be used to manage the symptoms of AS. These may include hot or cold therapy, massage, acupuncture, and relaxation techniques such as deep breathing exercises.
Managing Ankylosing Spondylitis in Daily Life
Managing AS in daily life involves making certain lifestyle adjustments and practicing self-care techniques. The following strategies can help improve overall well-being and minimize the impact of the disease.
Posture and Spinal Care
Maintaining good posture is essential for individuals with AS, as it helps reduce strain on the spine and joints. Practicing proper body mechanics, using supportive cushions and chairs, and avoiding prolonged sitting or standing can help alleviate discomfort.
Exercise and Stretching
Regular exercise and stretching are important for maintaining joint flexibility and mobility. Engaging in activities such as yoga or Pilates can help improve posture, strengthen the muscles, and alleviate stiffness.
Ergonomics
Ensuring proper ergonomics in the workplace and at home can help minimize strain on the joints. Using ergonomic chairs, keyboards, and standing desks can promote better posture and reduce the risk of developing pain or discomfort.
Heat and Cold Therapy
Applying heat or cold to the affected areas can provide temporary relief from pain and stiffness. Warm showers, heating pads, or ice packs can be used depending on personal preference and the specific symptoms experienced.
Stress Management
Stress can worsen the symptoms of AS, so it is important to practice stress management techniques. Engaging in activities such as meditation, deep breathing exercises, or hobbies that promote relaxation can help reduce stress levels and improve overall well-being.
Complications Associated with Ankylosing Spondylitis
If left untreated or poorly managed, AS can lead to several complications that can significantly impact a person’s health and quality of life.
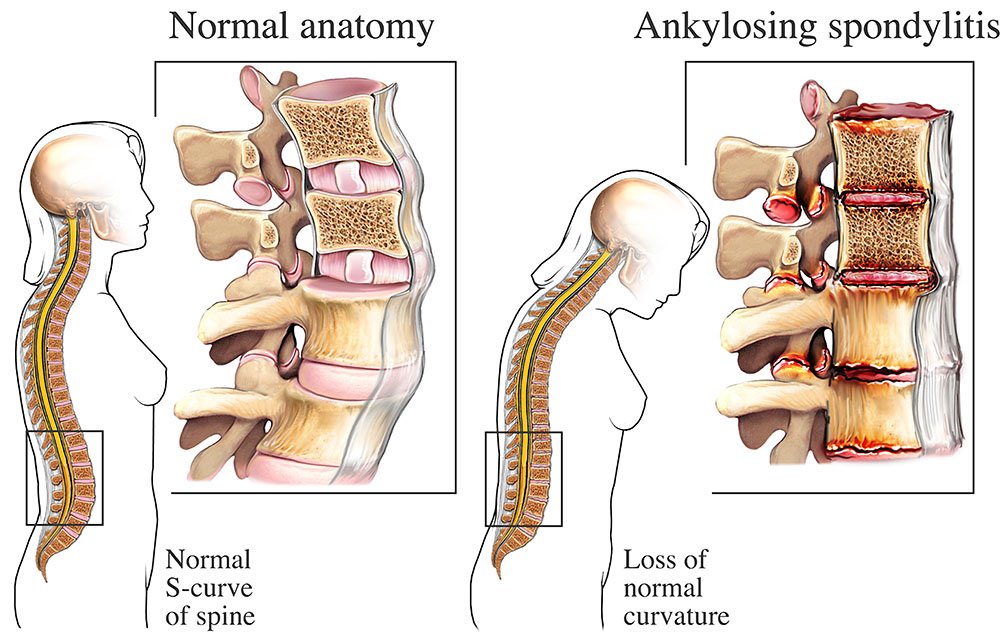
Spinal Fusion
Over time, AS can cause the vertebrae in the spine to fuse together, leading to a loss of mobility and flexibility. This can result in a stooped posture and limited range of motion.
Osteoporosis
AS can increase the risk of developing osteoporosis, a condition characterized by weakened bones. This can lead to an increased risk of fractures and other complications.
Heart Problems
Individuals with AS may have an increased risk of developing certain heart problems, including aortitis (inflammation of the aorta) and aortic valve disease. Regular monitoring of heart health is important for early detection and management of these conditions.
Inflammation in the Eyes
AS can cause inflammation in the eyes, known as uveitis or iritis. This can lead to redness, pain, sensitivity to light, and blurred vision. Prompt medical attention is necessary to prevent complications and preserve vision.
Inflammatory Bowel Disease
Some individuals with AS may also develop inflammatory bowel disease, such as Crohn’s disease or ulcerative colitis. This can cause symptoms such as abdominal pain, diarrhea, and rectal bleeding.
Support and Resources for Ankylosing Spondylitis
Living with AS can be challenging, but there are numerous support and educational resources available to help individuals manage their condition effectively.
Support Groups
Joining a support group for AS can provide valuable emotional support and a sense of community. Connecting with others who understand the challenges of living with AS can be empowering and help individuals navigate their journey more effectively.
Patient Education
Educating yourself about AS can empower you to actively participate in your treatment and make informed decisions. Reliable sources of information include reputable websites, books, and educational materials provided by healthcare professionals.
Online Communities
Online communities and forums dedicated to AS provide an opportunity to connect with individuals from around the world who share similar experiences. These communities can offer support, advice, and a platform for sharing personal stories and insights.
Institutional Resources
Medical institutions and hospitals often have specialized clinics or departments dedicated to rheumatology, where individuals with AS can receive comprehensive care. These resources may include access to specialized healthcare professionals, research opportunities, and patient support programs.
Research Organizations
Research organizations focused on AS are continually working towards better understanding the disease and developing new treatment options. Keeping up-to-date with the latest advancements and participating in research studies can contribute to the progress in the field of AS.
Promising Research and Future Developments
The field of AS research is continuously evolving, with ongoing studies and advancements. Several areas of research show promise for improving the understanding and management of AS.
Immunotherapy
Immunotherapy, also known as targeted therapy, focuses on modifying the immune response to reduce inflammation and slow progression in AS. This approach aims to target specific immune system molecules that play a role in the disease process.
Genetic Studies
Genetic studies are unraveling the complex interactions between genetic factors and AS. By identifying specific genes that influence the development and progression of the disease, researchers hope to gain insights into potential therapeutic targets.
Biomarker Discoveries
Biomarkers are molecules or characteristics that can be measured and indicate the presence or progression of a disease. Ongoing research aims to identify biomarkers specific to AS, which could aid in early diagnosis, monitoring disease activity, and evaluating treatment responses.
Advancements in Biologics
Biologic therapies have revolutionized the treatment of various autoimmune conditions, including AS. Researchers continue to explore novel biologic agents and optimize treatment protocols to improve outcomes for individuals living with AS.
As research and clinical trials progress, it is hoped that new treatment options and personalized approaches will emerge, allowing for more effective management and improved quality of life for individuals with AS.
In conclusion, understanding the various aspects of Ankylosing Spondylitis, including its prevalence, risk factors, causes, symptoms, diagnosis, treatment options, complications, and available resources, is crucial for effective management and support. By raising awareness and promoting research, individuals with AS can receive proper care and lead fulfilling lives despite the challenges of this chronic condition. With advancements in research and a collaborative effort in the medical community, the future holds promise for improved understanding, personalized therapies, and better outcomes for individuals with AS.