Are your nails looking a little less than fabulous lately? Well, it could be a sign of a fungal nail infection. This common condition, known as onychomycosis, occurs when a fungus invades the nail bed, causing a range of symptoms that can be unsightly and uncomfortable. From thickened nails to discoloration and crumbling, these signs shouldn’t be ignored. In this article, we will explore the signs and symptoms of fungal nail infections, providing you with the knowledge you need to take the necessary steps for treatment and prevention. So, don’t let those pesky fungi ruin your nail game – let’s get to the root of the problem together!
Overview
What are fungal nail infections?
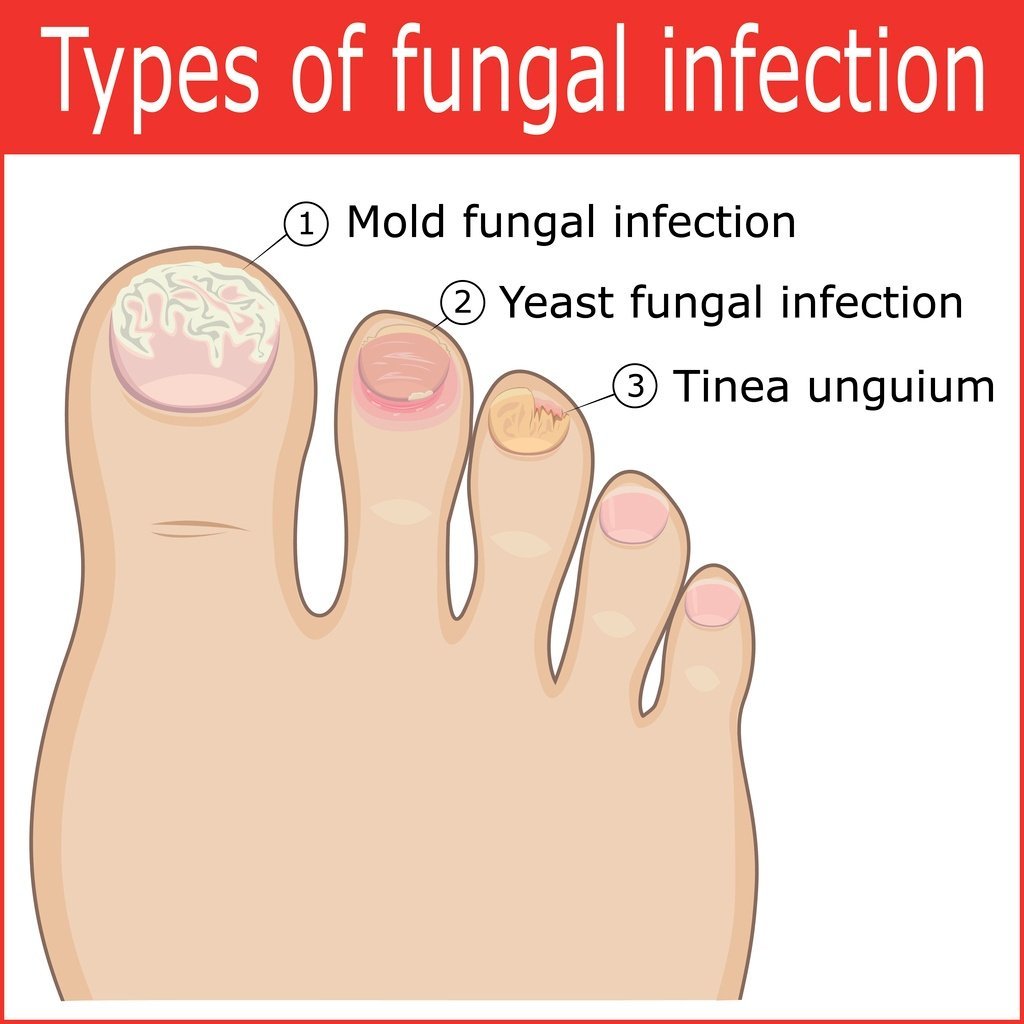
Fungal nail infections, also known as onychomycosis, are common fungal infections that affect the nails, most commonly the toenails. They are caused by fungi, such as dermatophytes, yeasts, or molds, that invade and grow in the nails. Fungal nail infections can cause various visible changes in the nails and may lead to discomfort or pain. If left untreated, they can cause permanent damage to the nails and may even spread to other parts of the body.
Causes of fungal nail infections
Fungal nail infections are primarily caused by the overgrowth of fungi in the nails. The most common culprits are dermatophytes, a group of fungi that thrive in warm and moist environments, such as swimming pools, public showers, and locker rooms. These fungi can enter the nails through small cuts or gaps between the nail and the nail bed. Other types of fungi, such as yeasts and molds, can also cause fungal nail infections, although they are less common.
Risk factors for fungal nail infections
Several factors can increase your risk of developing a fungal nail infection. These include:
- Age: Older adults are more prone to fungal nail infections due to reduced blood circulation, slower nail growth, and weakened immune systems.
- Poor hygiene: Not keeping your nails clean and dry can create a favorable environment for fungal growth.
- Nail damage: Any injury to the nail, such as a stubbed toe or repetitive trauma, can create openings for fungi to invade.
- Nail conditions: Certain conditions, such as psoriasis or nail psoriasis, can increase the risk of developing fungal nail infections.
- Sweating: Excessive sweating can create a moist environment that promotes fungal growth.
- Weakened immune system: Conditions that weaken the immune system, such as diabetes, HIV/AIDS, or certain medications, can make you more susceptible to fungal infections.
- Poor circulation: Conditions that affect blood flow, such as peripheral arterial disease, can hinder the body’s ability to fight off fungal infections.
Symptoms
Fungal nail infections can cause a range of symptoms, which can vary in severity from person to person. Here are some common symptoms to look out for:
Visible changes in the nails
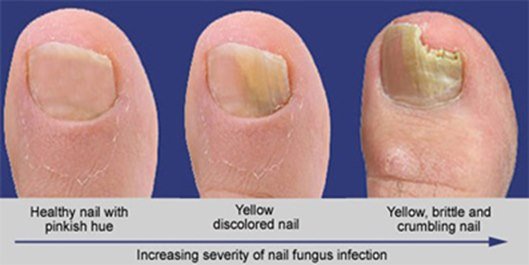
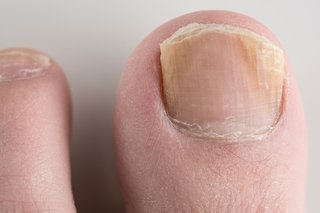
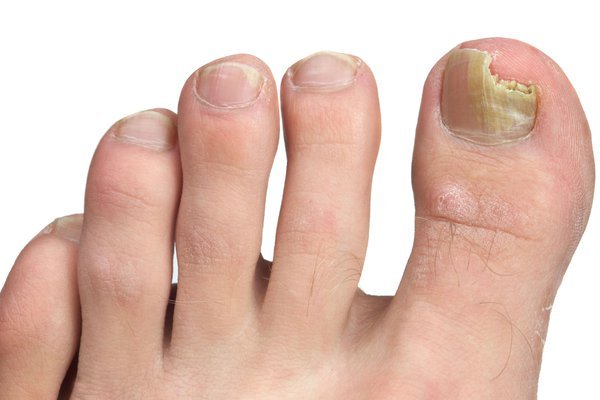
One of the first signs of a fungal nail infection is visible changes in the appearance of the nails. This can include the nails becoming discolored, turning yellow, brown, or white. The affected nails may also appear dull, thickened, or distorted in shape.
Thickened nails
Fungal nail infections can cause the nails to thicken and become more brittle. The nails may become difficult to trim and may even start to separate from the nail bed.
Discolored nails
Fungal nail infections can cause the nails to change color. They may turn yellow, brown, green, or white. In some cases, the infection can cause the entire nail to become discolored, while in others, only parts of the nail may be affected.
Brittle or crumbly nails
When a fungal infection affects the nails, they can become brittle or crumbly. The nails may break easily or develop a rough texture. They may also start to flake or chip at the edges.
Distorted nail shape
As the fungal infection progresses, it can cause the nails to become distorted in shape. They may become curved, wavy, or have an irregular surface. In severe cases, the nails may even lift off the nail bed or crumble completely.
Foul odor
Fungal nail infections can produce an unpleasant odor. This odor is often caused by the accumulation of debris and fungal growth underneath the nails.
Pain or discomfort
Some people with fungal nail infections may experience pain or discomfort. This can range from a mild, occasional discomfort to a more severe, persistent pain.
Itching or irritation
Fungal nail infections can cause itching or irritation around the affected nails. This can be particularly bothersome, especially if the infection spreads to multiple nails.
Tenderness around the nails
In some cases, fungal nail infections can cause tenderness or sensitivity around the nails. The affected nails may feel tender to the touch, and pressure on the nails may trigger pain or discomfort.
Diagnosis
If you suspect you have a fungal nail infection, it is important to consult a healthcare professional for a proper diagnosis. They will assess your symptoms and may perform various tests to confirm the presence of a fungal infection. Some common diagnostic methods include:
Physical examination
During a physical examination, a healthcare professional will inspect the affected nails and look for visible signs of a fungal infection. They may also inquire about your medical history and any underlying health conditions that may contribute to the infection.
Nail clippings or scrapings
To confirm the presence of a fungal infection, a healthcare professional may collect nail clippings or scrapings from the affected nails. These samples will be sent to a laboratory for further analysis.
Fungal culture
A fungal culture involves placing the collected nail samples in a special medium that promotes the growth of fungi. This allows healthcare professionals to identify the specific type of fungus causing the infection.
Microscopic examination
Microscopic examination involves examining the nail samples under a microscope. This allows healthcare professionals to detect the presence of fungal elements, such as hyphae or spores, which confirm the diagnosis of a fungal infection.
Wood’s lamp examination
A Wood’s lamp examination is a diagnostic test that uses ultraviolet light to detect fungal infections. However, this method is not always reliable for diagnosing fungal nail infections and is often used in conjunction with other diagnostic techniques.
Complications
While fungal nail infections may seem harmless at first, if left untreated, they can lead to various complications. Some common complications include:
Permanent nail damage
If a fungal nail infection is not treated promptly, it can cause permanent damage to the nails. The nails may become thickened, discolored, or deformed, which can impact their appearance and overall health.
Spread of infection
Without proper treatment, fungal nail infections can spread to other nails or even to other parts of the body. This can lead to multiple infected nails and increase the difficulty of treatment.
Cellulitis
In some cases, untreated fungal nail infections can lead to cellulitis, a bacterial skin infection. Cellulitis can cause redness, swelling, pain, and warmth in the affected area. If left untreated, cellulitis can lead to more serious complications, such as abscess formation or blood infection.
Bone infection
In rare cases, severe and untreated fungal nail infections can spread to the underlying bones, leading to a bone infection (osteomyelitis). Bone infections can be challenging to treat and may require surgical intervention.
Prevention
Preventing fungal nail infections is important to reduce the risk of developing this common fungal infection. Here are some preventive measures you can take:
Keep nails clean and dry
Keeping your nails clean and dry is crucial to prevent the growth of fungi. After washing your hands or feet, thoroughly dry them, paying special attention to the spaces between the toes and fingers.
Trim nails properly
Proper nail trimming can prevent the accumulation of debris and reduce the risk of a fungal infection. Trim your nails straight across and avoid rounding the edges, as this can cause the nails to grow into the skin.
Avoid sharing personal items
Avoid sharing personal items, such as nail clippers, socks, or shoes, as this can increase the risk of spreading fungal infections. If you visit a nail salon, make sure they follow strict hygiene practices and disinfect their tools properly.
Use protective footwear
When using public showers, locker rooms, or swimming pools, wear protective footwear, such as flip-flops or shower shoes. This can reduce the risk of coming into contact with fungi that thrive in moist environments.
Avoid walking barefoot in public places
Walking barefoot in public places, such as gyms or communal showers, can expose your feet to fungal infections. Always wear shoes or sandals to protect your feet from coming into direct contact with contaminated surfaces.
Choose breathable footwear and socks
Opt for breathable footwear made from materials such as leather or canvas. These materials allow air circulation and reduce the likelihood of moisture buildup. Additionally, wear moisture-wicking socks to further prevent excessive sweating.
Use antifungal sprays or powders
Consider using antifungal sprays or powders on your feet or in your shoes to inhibit the growth of fungi. These products can create an inhospitable environment for fungal growth and reduce the risk of infection.
Wear gloves when handling chemicals or water for extended periods
When working with chemicals or immersing your hands in water for extended periods, such as during household chores or while swimming, wear protective gloves. This helps minimize the exposure of your nails to moisture and potential fungal contamination.
Avoid prolonged contact with water
Prolonged exposure to water can weaken the nails and make them more prone to fungal infections. If your hands or feet are frequently submerged in water, consider wearing waterproof gloves or using protective creams to create a barrier.
Treatment
If you have been diagnosed with a fungal nail infection, various treatment options are available. The choice of treatment depends on the severity of the infection and individual factors. Some common treatment options include:
Topical antifungal medications
For mild to moderate fungal nail infections, topical antifungal medications, such as creams, gels, or nail lacquers, are often prescribed. These medications are applied directly to the affected nails and are generally used for several weeks or months. It is important to follow the prescribed regimen consistently for effective treatment.
Oral antifungal medications
For more severe or persistent fungal nail infections, oral antifungal medications may be recommended. These medications, such as terbinafine or itraconazole, are taken orally and work systemically to eliminate the fungal infection. Oral antifungal medications are typically taken for several weeks or months and require regular monitoring for potential side effects.
Surgical intervention
In some cases, surgical intervention may be necessary to treat fungal nail infections. Surgical options include removing the affected nail (partial or complete nail avulsion) or surgical removal of the nail bed (matrixectomy). These procedures are usually reserved for severe or recurrent infections that do not respond to other treatment methods.
Laser therapy
Laser therapy is a relatively new treatment option for fungal nail infections. This non-invasive procedure uses laser energy to target and destroy the fungi without damaging the surrounding tissues. The effectiveness of laser therapy may vary, and multiple sessions may be required for optimal results.
Nail removal
In severe cases of fungal nail infections that do not respond to other treatments, removing the affected nail completely may be necessary. This allows for direct treatment of the nail bed and prevents the spread of the infection. However, nail removal is generally considered a last resort due to the permanent loss of the nail.
Home remedies
Several home remedies can complement medical treatments for fungal nail infections. These include regularly soaking the affected nails in a mixture of warm water and vinegar, using tea tree oil or coconut oil, or applying antifungal creams or ointments over the counter. While these remedies may provide some relief, they are often not as effective as medical treatments alone.
At-Home Care
In addition to medical treatments and preventive measures, there are steps you can take at home to care for your nails and prevent further complications. Here are some recommendations:
Keep nails clean and dry
Maintain good hygiene by keeping your nails clean and dry. Thoroughly dry your nails after washing, and avoid prolonged exposure to moisture. This helps create an unfavorable environment for fungal growth.
Clip and file nails properly
Proper nail care includes regular trimming and filing. Trim your nails straight across and file any rough edges. Avoid cutting the nails too short, as this can increase the risk of nail trauma and fungal infection.
Apply antifungal creams or ointments
As part of your at-home care routine, consider applying antifungal creams or ointments recommended by your healthcare professional. These topical treatments can help inhibit the growth of fungi and support the effectiveness of medical treatments.
Use over-the-counter treatments
Over-the-counter antifungal treatments, such as creams, gels, or sprays, may provide temporary relief from the symptoms of fungal nail infections. However, they are generally less potent than prescription medications and may not eliminate the infection completely.
Practice good foot hygiene
In addition to keeping your nails clean, practice good foot hygiene to prevent the spread of fungal infections. Wash your feet regularly, dry them thoroughly, and wear clean socks made of moisture-wicking materials.
Use medicated nail polish
Medicated nail polish containing an antifungal agent can be used as a preventive measure or as part of the treatment plan for fungal nail infections. Apply the medicated nail polish as directed by your healthcare professional to help inhibit fungal growth.
When to See a Doctor
While you can often manage mild fungal nail infections at home, it is important to consult a healthcare professional if you experience any of the following:
Severe nail infection
If the fungal nail infection is severe and causing significant pain, discomfort, or interference with daily activities, it is advisable to seek medical attention. The healthcare professional can assess the severity of the infection and recommend appropriate treatment options.
Painful infection
If you experience severe pain or throbbing in the affected nails, it may indicate an advanced or spreading infection. Prompt medical evaluation is necessary to prevent further complications and manage the pain effectively.
Persistent or recurring infection
If the fungal nail infection persists or keeps coming back despite treatment, it is important to consult a healthcare professional. They may need to reassess the diagnosis, modify the treatment plan, or explore underlying causes that contribute to the recurrent infection.
Spreading infection
If the infection spreads to other nails or to other parts of your body, it is essential to seek medical attention. This suggests an aggressive or widespread infection that may require more intensive treatment.
Underlying health conditions
If you have an underlying health condition, such as diabetes or a weakened immune system, it is crucial to monitor and manage fungal nail infections. These conditions can increase the risk of complications and require specialized care.
Conclusion
Fungal nail infections are common but treatable conditions that can affect the appearance and health of your nails. By understanding the causes, symptoms, diagnosis, and treatment options, you can take appropriate measures to prevent fungal nail infections and seek prompt medical attention when needed. Remember to maintain good hygiene, practice preventive measures, and consult a healthcare professional for proper diagnosis and treatment. With proper care, you can help protect your nails from permanent damage and enjoy healthy, fungus-free nails.