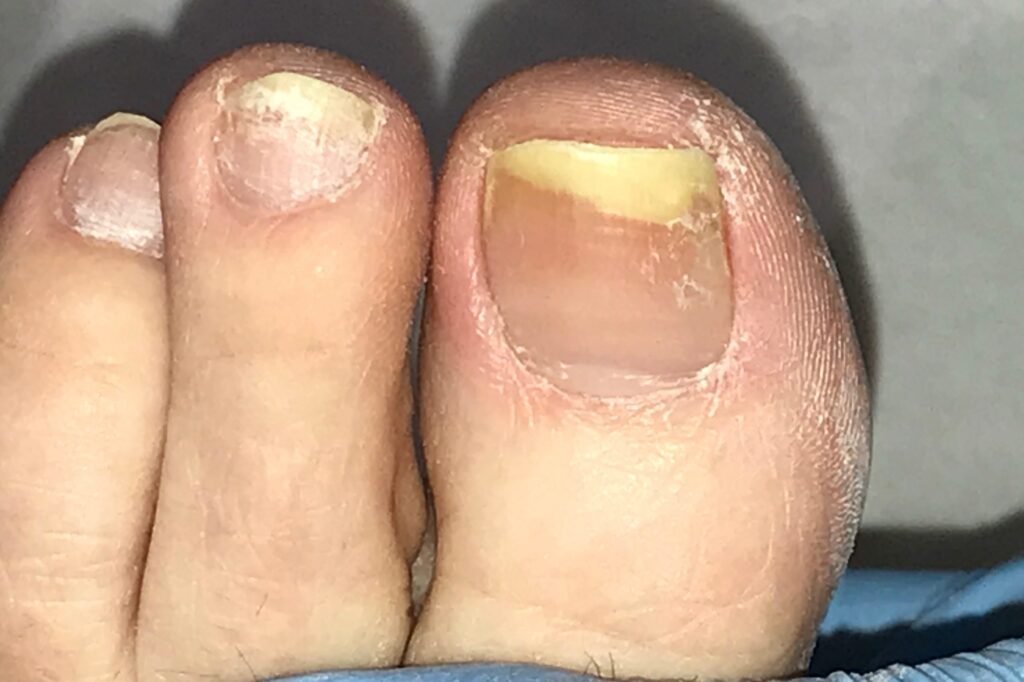
Are you experiencing discoloration, thickening, or brittleness in your toenails? If so, you may be dealing with a fungal nail infection. This common condition occurs when fungus infects the nails and can be both uncomfortable and embarrassing. In this article, we will explore the causes, symptoms, and treatment options for fungal nail infections, helping you understand how to effectively manage this pesky condition. So, if you’re ready to take the first step towards healthier, happier feet, let’s dive into the world of fungal nail infections together.
Causes of Fungal Nail Infections
Fungal pathogens
Fungal nail infections, also known as onychomycosis, are primarily caused by various types of fungi. The most common culprits include dermatophytes, which are found in soil and on the skin and nails of infected individuals. Yeast and molds can also lead to fungal nail infections, although they are less prevalent. The fungi thrive in warm, moist environments, making nails susceptible to infection.
Risk factors
Certain factors increase the likelihood of developing a fungal nail infection. These include aging, as fungal infections become more common in older individuals. People with compromised immune systems, such as those with HIV/AIDS or undergoing cancer treatment, are also at higher risk. Athletes and individuals with diabetes, who often have sweaty feet or poor circulation, respectively, are more susceptible to infections. Additionally, wearing tight-fitting shoes or synthetic socks, as well as walking barefoot in public places like swimming pools or locker rooms, can contribute to the development of fungal nail infections.
Transmission methods
Fungal nail infections can be easily transmitted from person to person. Direct contact with an infected person’s nails or skin can spread the fungus. Sharing personal items like nail clippers or towels, which may harbor fungal spores, can also lead to infection. Furthermore, walking barefoot in public areas and using communal showers or pools can increase the risk of picking up fungi that cause nail infections.
Conditions that promote infection
Various conditions can create an environment that promotes fungal nail infections. These include warm and humid climates, excessive sweating of the feet, and prolonged exposure to moisture. Wearing shoes and socks that do not allow proper ventilation can create a favorable breeding ground for fungi. Additionally, having a history of nail trauma, such as injury or repeated microtrauma from tight footwear, can weaken the nail’s natural defense mechanisms, making it more susceptible to infection.
Signs and Symptoms
Nail discoloration
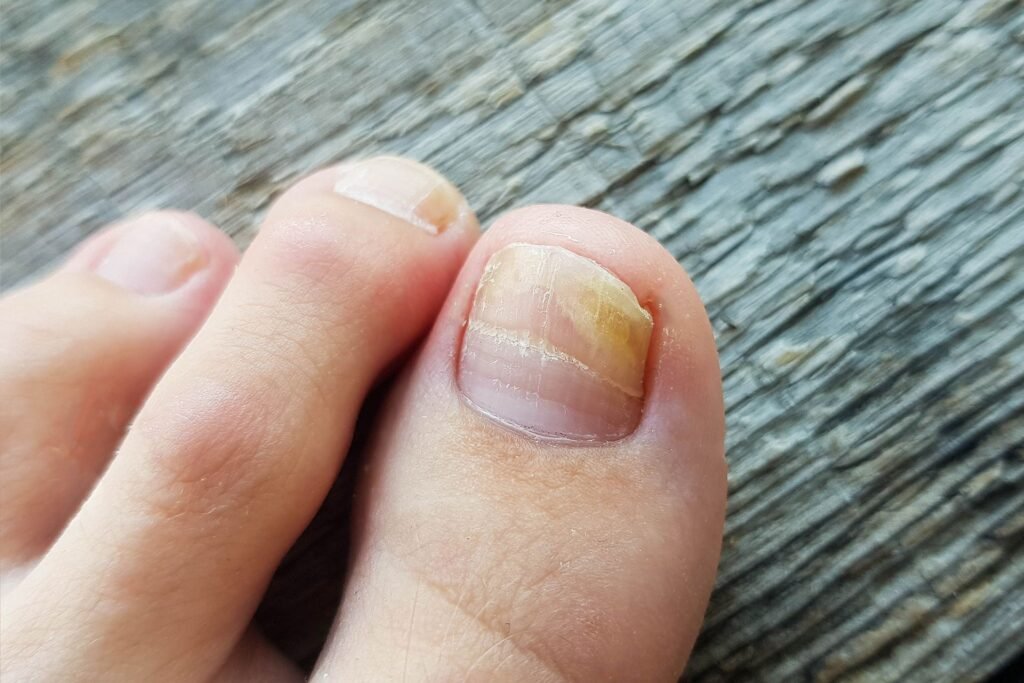
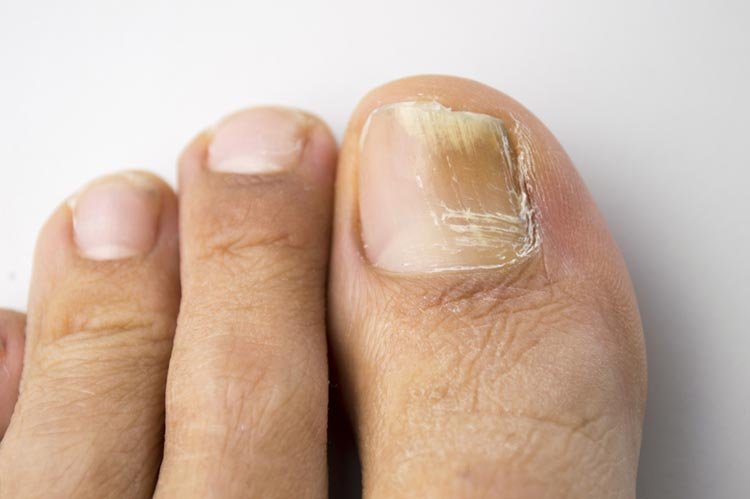
One of the primary signs of a fungal nail infection is nail discoloration. Infected nails may turn yellow, brown, or even green. The discoloration often starts at the edges or the tip of the nail and gradually spreads towards the cuticle.
Thickening and deformity
As the fungal infection progresses, the infected nail can become thicker and distorted in shape. The nail may become brittle and crumbly, making it difficult to trim or maintain proper nail hygiene. The nail’s texture may also change, becoming rough or pitted.
Brittleness and crumbling
Fungal nail infections can lead to brittle and crumbly nails that easily break or separate from the nail bed. This can cause significant discomfort and make it challenging to engage in regular activities that involve manual dexterity.
Foul odor
Some individuals with fungal nail infections may notice a foul smell emanating from their infected nails. This odor is often a result of the byproducts produced by the fungi as they multiply and grow within the nail.
Pain and discomfort
In advanced stages of fungal nail infections, individuals may experience pain and discomfort. The infected nail may cause pressure and irritation, leading to discomfort while walking or wearing certain types of shoes.
Diagnosis
Physical examination
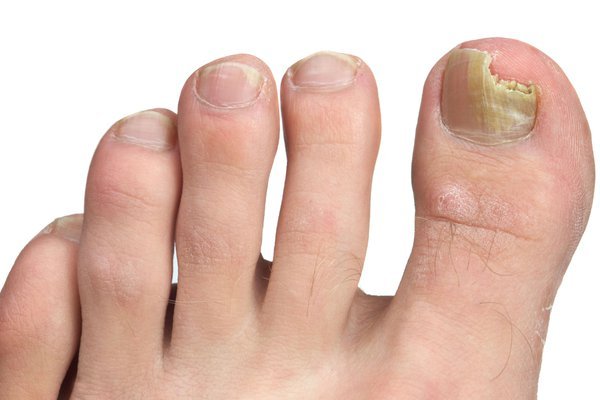
To diagnose a fungal nail infection, a healthcare provider will perform a physical examination of the affected nails. They will look for characteristic signs, such as discoloration, thickening, and deformation. It is important to mention any symptoms or concerns to the healthcare provider during the examination.
Microscopic examination
Microscopic examination involves collecting a nail clipping or scraping to examine under a microscope. This allows the healthcare provider to identify the presence of fungi or other infectious agents. They will look for telltale signs such as hyphae (strand-like structures) or spores.
Fungal culture
A fungal culture involves collecting a sample of the infected nail and placing it in a laboratory dish to encourage fungal growth. The fungi are then identified and characterized, helping to determine the most appropriate antifungal treatment.
Biopsy
In rare cases where the diagnosis is not clear, a nail biopsy may be performed. During a biopsy, a small piece of the infected nail is removed and sent to a laboratory for further analysis. This helps to confirm the presence of fungal infection and rule out other underlying conditions that may mimic the symptoms.
Types of Fungal Nail Infections
Distal subungual onychomycosis
Distal subungual onychomycosis is the most common type of fungal nail infection. It typically begins at the end of the nail bed and progresses towards the cuticle. The infection may cause the nail to become discolored, thickened, and brittle.
White superficial onychomycosis
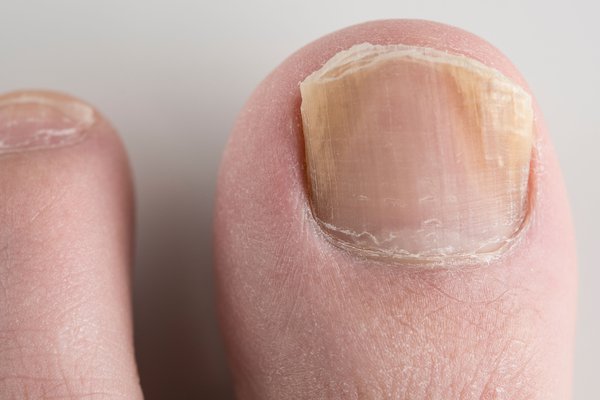
White superficial onychomycosis is characterized by white, powdery patches on the surface of the nail. The infection typically affects the top layers of the nail and can cause it to become rough and crumbly.
Proximal subungual onychomycosis
Proximal subungual onychomycosis is less common and usually occurs in individuals with compromised immune systems. The infection starts at the base of the nail and progresses towards the tip. It may cause the nail to lift from the nail bed and become discolored.
Candidal onychomycosis
Candidal onychomycosis is caused by Candida species of yeast. It primarily affects the fingernails and can cause separation of the nail from the nail bed, redness, and swelling. This type of fungal nail infection is more common in individuals who frequently immerse their hands in water.
Prevention
Maintaining proper hygiene
Maintaining good nail hygiene is essential in preventing fungal nail infections. Keep your nails clean and dry, regularly trim them, and avoid cutting or tearing the skin around the nails. It is also important to wash your hands and feet regularly with soap and water.
Using antifungal sprays/powders
To prevent fungal infections, consider using antifungal sprays or powders on your feet or in your shoes. These products can help reduce the moisture and inhibit the growth of fungi. It is best to apply them after showering or bathing and before wearing socks or shoes.
Avoiding prolonged exposure to moisture
Moisture is a breeding ground for fungi, so it is important to avoid prolonged exposure to wet environments. After activities that cause your feet to become sweaty or wet, dry them thoroughly. If possible, change into dry socks and footwear. It is also helpful to alternate your shoes to allow them to fully dry between uses.
Wearing breathable shoes and socks
Choose shoes and socks that allow air circulation and moisture evaporation. Opt for breathable materials such as leather or canvas, as they are less likely to trap moisture. Avoid wearing tight-fitting shoes or synthetic socks, as they can contribute to sweaty feet and create a suitable environment for fungal growth.
Home Remedies
Vinegar soak
A vinegar soak can help fight fungal nail infections due to its acidic properties. Mix equal parts of white vinegar and warm water in a basin and soak the affected nails for 15-20 minutes daily. This can help inhibit fungal growth and restore the natural pH balance of the nails.
Tea tree oil application
Tea tree oil has natural antifungal properties and can be used as a topical treatment for fungal nail infections. Dilute tea tree oil with a carrier oil, such as coconut oil, and apply it directly to the affected nails two times a day. Continue this treatment until the infection clears up.
Garlic paste
Garlic has antimicrobial properties that can help combat fungal infections. Crush a few garlic cloves into a paste and apply it directly to the affected nails. Leave it on for 30 minutes and rinse thoroughly. Repeat this process daily until the infection improves.
Oregano oil
Oregano oil contains compounds that exhibit antifungal properties. Mix a few drops of oregano oil with a carrier oil and apply it to the affected nails two times a day. Be sure to let the oil penetrate the nail and surrounding skin.
Baking soda scrub
A baking soda scrub can help exfoliate and cleanse the affected nails. Mix baking soda with water to form a paste and gently scrub it onto the nails using a soft brush or toothbrush. Rinse thoroughly and repeat regularly for best results.
Medical Treatments
Topical antifungal medications
Topical antifungal medications, such as creams or ointments, are often the first-line treatment for fungal nail infections. These medications are applied directly to the infected nails and surrounding skin. It is important to follow the prescribed treatment regimen, which may span several weeks or months, to achieve successful results.
Oral antifungal medications
In cases of severe or resistant fungal nail infections, oral antifungal medications may be necessary. These medications work from within the body to fight the fungal infection. They are typically taken for a specified duration, often several months, and require periodic monitoring by a healthcare provider.
Nail debridement
Nail debridement involves the removal of the infected nail material using specialized tools. This procedure can be performed by a healthcare provider and is often combined with other treatment methods to enhance the effectiveness of antifungal medications.
Laser therapy
Laser therapy is a relatively new treatment option for fungal nail infections. It involves using a laser device to heat and kill the fungi without damaging the surrounding tissues. Multiple sessions may be required to achieve optimal results.
Surgical nail removal
In severe cases of fungal nail infections that do not respond to other treatments, surgical nail removal may be considered. This procedure involves removing all or part of the infected nail. It is usually reserved as a last resort option when other treatments have failed.
Complications
Secondary bacterial infection
If left untreated, fungal nail infections can lead to secondary bacterial infections. The damaged and weakened nail provides an entry point for bacteria, which can cause redness, swelling, and pus formation. Prompt treatment of fungal nail infections can help prevent the development of secondary complications.
Permanent nail damage
Advanced fungal nail infections can cause permanent damage to the nails. This may result in permanent thickening, deformity, or discoloration of the affected nails. Treatment at an early stage can help minimize the risk of permanent nail damage.
Functional limitations
Fungal nail infections can affect the functionality of the affected nails. Thickened, brittle, or crumbly nails can make it difficult to engage in activities that require fine motor skills or involve contact with objects. This can impact daily activities and decrease overall quality of life.
Emotional distress
The visible signs of fungal nail infections, such as discolored or deformed nails, can cause emotional distress and lower self-esteem. Individuals may feel self-conscious about the appearance of their nails, leading to social anxiety or avoidance of certain activities. Providing emotional support and seeking treatment can help alleviate these feelings.
Risk Groups
Elderly individuals
Fungal nail infections are more prevalent in the elderly population due to natural changes in nail structure and decreased blood circulation. Furthermore, aging can weaken the immune system, making older individuals more susceptible to fungal infections.
People with compromised immunity
Individuals with compromised immune systems, such as those with HIV/AIDS or undergoing cancer treatment, have a higher risk of developing fungal nail infections. Weakened immune defenses make it more difficult for the body to fend off fungal pathogens.
Athletes
Athletes, particularly those involved in sports that require close contact with moisture or sweaty footwear, are prone to fungal nail infections. The constant exposure to moist environments and repetitive trauma can create an ideal breeding ground for fungi.
Individuals with diabetes
People with diabetes often have poor circulation and nerve function in their feet. This can lead to decreased resistance to infections, including fungal nail infections. It is essential for individuals with diabetes to maintain good foot hygiene and seek prompt treatment for any signs of infection.
Conclusion
Fungal nail infections can be both bothersome and cosmetically displeasing. However, with proper understanding and preventive measures, the risk of developing such infections can be significantly reduced. Maintaining good nail hygiene, avoiding prolonged exposure to moisture, and wearing breathable shoes and socks are key preventive measures. If an infection does occur, various treatment options are available, ranging from home remedies to medical interventions. Seeking prompt medical attention and following recommended treatment guidelines can help alleviate symptoms, prevent complications, and restore the health and appearance of the nails. Remember, prevention is always better than cure when it comes to fungal nail infections.