Have you ever experienced a sudden onset of itchy, red welts appearing out of nowhere on your skin? It can be incredibly frustrating to deal with these mysterious hives and not know the cause. Fortunately, in this article, we will uncover the mystery behind hives and explore the possible triggers that may be causing them. By understanding the underlying causes, you can find relief and take steps to prevent these irritating welts from appearing in the first place. Stay tuned as we delve into the fascinating world of hives and discover the secrets behind their appearance.
Introduction
Welcome to our comprehensive guide on hives! Whether you’re experiencing hives yourself or seeking information for a loved one, we’re here to provide you with all the information you need to understand, manage, and treat this common skin condition. Hives can be a source of discomfort and distress, but with the right knowledge and resources, you can take control and find relief.
What are Hives?
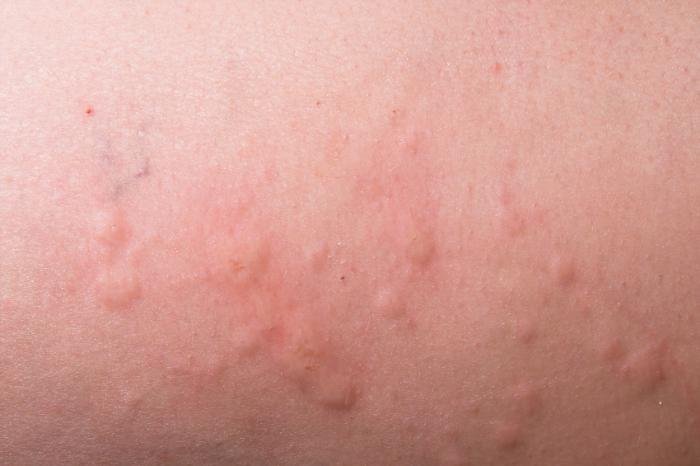
Hives, also known as urticaria, are characterized by itchy, red, and raised welts on the skin. They can vary in size and shape and often appear suddenly. Hives occur when certain cells in the skin release histamine and other substances, causing an allergic reaction. This reaction leads to the characteristic symptoms associated with hives.
Symptoms
The primary symptom of hives is the appearance of raised, itchy bumps on the skin. These bumps, known as wheals, can range in size from small spots to larger welts and may change shape and location on the body. Hives can also be accompanied by other symptoms, such as swelling (angioedema), itching, a burning sensation, and even pain in some cases.
Causes
Hives can have various underlying causes, and identifying the trigger can be essential for effective management. Some common causes of hives include:
-
Allergens: Exposure to allergens such as pet dander, pollen, dust mites, or certain foods can trigger an allergic reaction and lead to hives.
-
Food: Certain foods, including nuts, shellfish, eggs, and dairy products, can cause hives in susceptible individuals.
-
Medications: Some medications, such as antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), and aspirin, have been known to induce hives as an adverse reaction.
-
Infections: Viral or bacterial infections, including the common cold or urinary tract infections, can sometimes result in hives.
-
Physical Factors: External factors like pressure, cold temperature, heat, sunlight, or exercise can trigger hives in some individuals.
-
Emotional Stress: Stress and emotional factors can contribute to the development of hives in some cases.
Diagnosis
If you suspect you have hives, it is important to consult a healthcare professional for an accurate diagnosis. Your doctor will perform a physical examination, review your medical history, and may conduct allergy testing or other diagnostic tests to determine the underlying cause of your hives. By identifying the trigger, your healthcare provider can develop an appropriate treatment plan tailored to your specific needs.

Types of Hives
Hives can be classified into different types based on their duration and underlying causes. Understanding the different types of hives can help guide your treatment and management approach.
Acute Urticaria
Acute urticaria refers to hives that last for less than six weeks. This form of hives is often triggered by allergens or other identifiable causes. Acute urticaria is the most common type and usually resolves spontaneously within a few days or weeks.
Chronic Urticaria
Chronic urticaria is characterized by hives that persist or recur for more than six weeks. Unlike acute urticaria, the exact cause of chronic hives is often difficult to determine. In some cases, chronic urticaria may be related to an underlying autoimmune or systemic disease. It is important to work closely with your healthcare provider to manage and treat chronic hives effectively.
Physical Urticaria
Physical urticaria refers to hives that are triggered by physical stimuli such as pressure, cold, heat, exercise, or sunlight. This type of hives occurs in response to specific physical factors and can vary in severity and duration. Identifying and avoiding these triggers is crucial in managing physical urticaria.
Triggers of Hives
Hives can be triggered by a wide range of factors. Understanding and identifying your triggers can help prevent and manage future episodes of hives. Here are some common triggers to be aware of:
Allergens
Exposure to allergens such as pollen, pet dander, dust mites, or certain medications can lead to an allergic reaction and trigger hives in susceptible individuals. If you suspect an allergen is causing your hives, allergy testing can help identify the specific culprit and guide your management plan.
Food
Certain foods have been known to cause hives in susceptible individuals. Common culprits include nuts, shellfish, eggs, dairy products, and certain food additives. Keeping a food diary can help identify potential triggers and guide dietary modifications to manage your hives.
Medications
Some medications can cause hives as an adverse reaction. Antibiotics, NSAIDs, aspirin, and other drugs have been associated with hives in certain individuals. If you suspect a medication is triggering your hives, it is important to consult your doctor for alternative treatment options.
Infections
Viral or bacterial infections can sometimes lead to the development of hives. The common cold, sinus infections, and urinary tract infections are examples of infections that may cause hives. Treating the underlying infection is crucial for effectively managing hives in these cases.
Physical Factors
Physical factors such as pressure, cold temperature, heat, exercise, or exposure to sunlight can trigger hives in individuals with physical urticaria. Avoiding these triggers or taking preventive measures, such as wearing protective clothing or using sunscreen, can help manage physical urticaria.
Emotional Stress
Stress and emotional factors have been associated with the development or worsening of hives in some individuals. Engaging in stress management techniques such as meditation, exercise, or therapy can be beneficial in reducing the frequency and severity of stress-induced hives.

How to Treat Hives
Managing and treating hives often involves a combination of medications, lifestyle modifications, and home remedies. Here are some commonly used approaches:
Antihistamines
Antihistamines are a common treatment for hives as they help block the effects of histamine, a chemical released during an allergic reaction. Over-the-counter antihistamines such as cetirizine or loratadine can provide relief from mild to moderate hives. If your hives are severe or require stronger management, your doctor may prescribe stronger antihistamines or a combination of medications.
Corticosteroids
In cases of severe hives or when other treatments fail, corticosteroids may be prescribed. These medications work by reducing inflammation and suppressing the immune system. Corticosteroids can provide quick relief but are generally prescribed for short-term use due to potential side effects with long-term use.
Other Medications
For individuals with chronic hives or hives caused by underlying conditions, additional medications may be prescribed. These may include immune modulators, antifungal medications, or medications that target specific immune system molecules involved in the development of hives.
Home Remedies
In addition to medications, there are various home remedies that can help alleviate symptoms and promote healing. Applying a cold compress to the affected areas, taking oatmeal baths, using soothing lotions or creams, and avoiding irritants or triggers can provide temporary relief from hives. However, it is important to consult your healthcare provider to ensure that these remedies are appropriate for your specific situation.
Prevention and Management
While it may not be possible to completely prevent hives, there are steps you can take to minimize your risk and manage the condition effectively.
Avoidance of Triggers
Identifying and avoiding your triggers is key to preventing hives. Keep a record of potential triggers and try to eliminate or minimize exposure to them. If you are unsure of the trigger, allergy testing can be helpful in identifying specific allergens.
Stress Management
Stress can worsen or trigger hives in some individuals. Engaging in stress management techniques such as exercising, mindfulness, deep breathing, or seeking professional support can help reduce stress levels and minimize the occurrence of stress-induced hives.
Maintaining a Healthy Lifestyle
Adopting a healthy lifestyle can contribute to overall well-being and potentially reduce the frequency and severity of hives. This includes eating a balanced diet, getting regular exercise, ensuring adequate sleep, and managing other underlying health conditions.

Complications of Hives
In most cases, hives are not dangerous and do not cause any significant complications. However, in rare instances, severe hives or angioedema can lead to life-threatening allergic reactions, known as anaphylaxis. Anaphylaxis requires immediate medical attention and can present with symptoms such as difficulty breathing, swelling of the lips or tongue, dizziness, and loss of consciousness. It is important to be aware of these symptoms and seek emergency care if they occur.
When to See a Doctor
While most cases of hives can be managed at home, it is important to consult a healthcare professional in certain situations. Seek medical attention if:
-
Your hives are severe or accompanied by difficulty breathing, swelling, or other signs of anaphylaxis.
-
The hives last longer than 6 weeks and are interfering with your daily life.
-
You have underlying health conditions or are taking medications that may complicate the management of your hives.
-
The hives are spreading rapidly and affecting a larger area of your body.

Myths and Misconceptions
There are several myths and misconceptions surrounding hives that can lead to confusion and misinformation. Let’s debunk a couple of the most common ones:
Hives are Contagious
Hives are not contagious. They are not caused by an infection or a communicable disease. Hives result from an allergic reaction or other underlying causes and cannot be transmitted from person to person.
Hives are Always a Sign of an Allergic Reaction
While many cases of hives are triggered by an allergic reaction, hives can also be caused by non-allergic factors such as infections, physical stimuli, or emotional stress. It is essential to work with your healthcare provider to identify the specific cause of your hives and develop an appropriate treatment plan.
FAQs about Hives
Here are answers to some frequently asked questions about hives:
Can stress cause hives?
Yes, stress can trigger or worsen hives in some individuals. Emotional stress releases certain chemicals in the body that can lead to the development of hives. It is important to manage stress levels and engage in stress reduction techniques to minimize the occurrence of stress-induced hives.
Can hives be dangerous?
In most cases, hives are not dangerous and do not cause significant harm. However, severe hives or angioedema can lead to life-threatening allergic reactions, known as anaphylaxis. It is crucial to seek immediate medical attention if you experience symptoms of anaphylaxis, such as difficulty breathing or swelling.
Can hives be a symptom of an underlying condition?
Yes, hives can be a symptom of an underlying condition, particularly in cases of chronic urticaria. Autoimmune diseases, thyroid disorders, or systemic conditions may manifest as hives. It is important to work closely with your healthcare provider to identify and manage any underlying conditions contributing to your hives.
In conclusion, hives can be an uncomfortable and distressing condition, but with the right knowledge and management strategies, you can find relief. Identifying and avoiding triggers, seeking appropriate medical care when necessary, and adopting a healthy lifestyle can help prevent the occurrence and minimize the impact of hives on your life. Remember, you don’t have to face hives alone – reach out to your healthcare provider for guidance and support.