In this informative article, you will gain a deeper understanding of Motor Neurone Disease (MND) – its causes, symptoms, and treatment options. MND, also known as Amyotrophic Lateral Sclerosis (ALS), affects the nerve cells responsible for controlling muscle movement. By exploring the causes, such as genetic and environmental factors, you will discover the potential risk factors associated with this progressive and debilitating disease. Furthermore, we will shed light on the common symptoms experienced by those affected by MND, ranging from muscle weakness and twitching to difficulty speaking and swallowing. Finally, we will explore the available treatment options and interventions that aim to manage the symptoms, improve quality of life, and provide support for individuals living with MND.
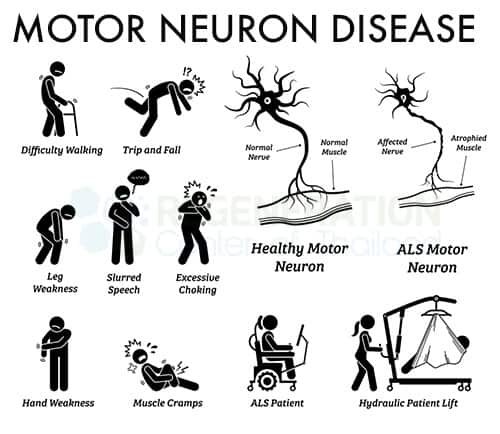
Overview of Motor Neurone Disease-MND
Definition and Background
Motor Neurone Disease (MND), also known as Amyotrophic Lateral Sclerosis (ALS), is a progressive neurological disorder that affects the motor neurones in the brain and spinal cord. These motor neurones are responsible for transmitting signals from the brain to the muscles, controlling voluntary muscle movements such as walking, speaking, and swallowing. MND leads to the degeneration and death of these motor neurones, resulting in muscle weakness, wasting, and eventually, paralysis.
Prevalence of Motor Neurone Disease
MND is a relatively rare condition, with an estimated prevalence of 2 to 5 per 100,000 individuals worldwide. It can affect people of any age, but it is most commonly diagnosed in individuals between the ages of 40 and 70. Men are slightly more likely to develop MND than women.
Understanding the Nervous System
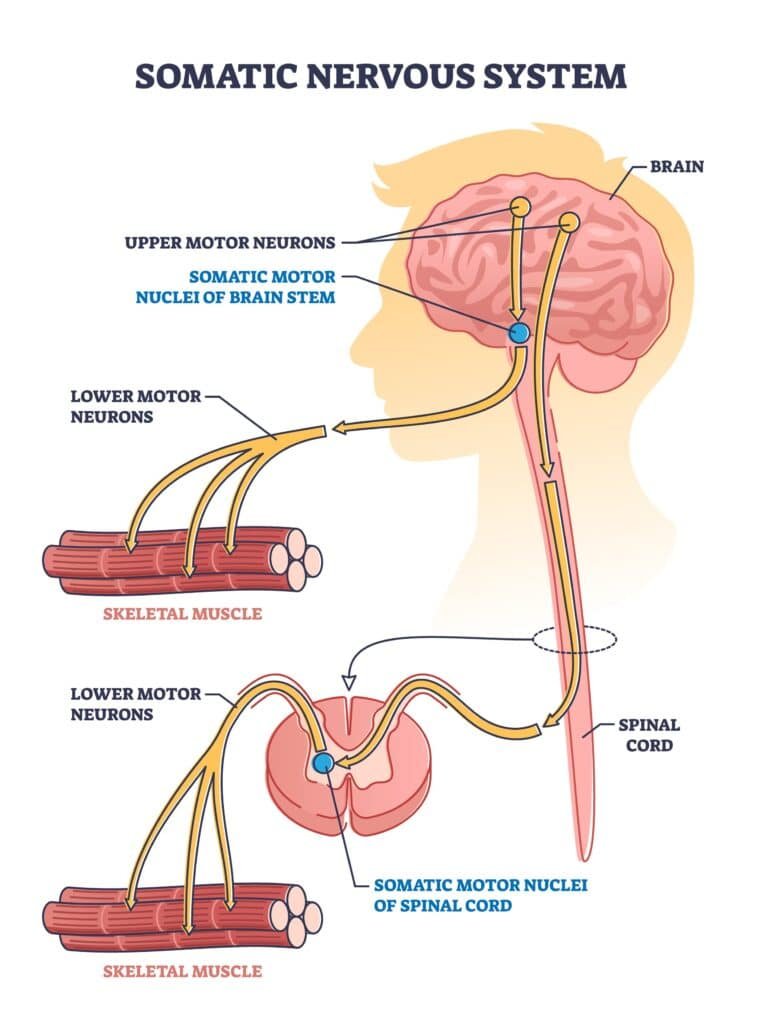
To understand MND, it is important to have a basic understanding of the nervous system. The nervous system consists of the central nervous system (brain and spinal cord) and the peripheral nervous system (nerves outside the brain and spinal cord). It plays a crucial role in regulating and coordinating the body’s functions. The motor neurones affected in MND are a part of the peripheral nervous system.
Function of Motor Neurones
Motor neurones are responsible for transmitting signals from the brain to the muscles throughout the body. They control voluntary muscle movements, allowing us to walk, talk, and perform various activities. In MND, the degeneration of these motor neurones disrupts the communication between the brain and muscles, leading to muscle weakness and eventually, paralysis.
Causes of Motor Neurone Disease
Genetic Factors
While the exact cause of MND is still unknown, researchers have identified genetic factors that play a role in its development. In some cases, MND can be inherited through specific gene mutations. The most common genetic form of MND is caused by mutations in the C9orf72 gene. However, the majority of MND cases are not inherited and are believed to occur due to a combination of genetic and environmental factors.
Environmental Factors
Apart from genetic factors, certain environmental factors may contribute to the development of MND. Exposure to certain toxins, such as heavy metals, pesticides, and chemicals, has been implicated in the onset of MND. However, more research is needed to fully understand the connection between these environmental factors and MND.
Potential Risk Factors
Several potential risk factors have been identified for MND, although their impact on the development of the disease is not fully understood. These risk factors include age, gender (men are slightly more likely to develop MND), smoking, and exposure to viruses or other infections.
Role of Oxidative Stress
Oxidative stress is believed to play a role in the pathogenesis of MND. This occurs when there is an imbalance between the production of reactive oxygen species (free radicals) and the body’s ability to counteract their harmful effects. Oxidative stress can cause damage to cells and contribute to the degeneration of motor neurones in MND.
Excitotoxicity and Glutamate
Excitotoxicity, another potential mechanism in MND, involves the excessive release of the neurotransmitter glutamate. Normally, glutamate plays a crucial role in transmitting signals between nerve cells. However, in MND, there is an accumulation of glutamate, leading to overactivation of certain receptors in motor neurones. This overexcitation can contribute to the degeneration of motor neurones in MND.

Types of Motor Neurone Disease
Amyotrophic Lateral Sclerosis (ALS)
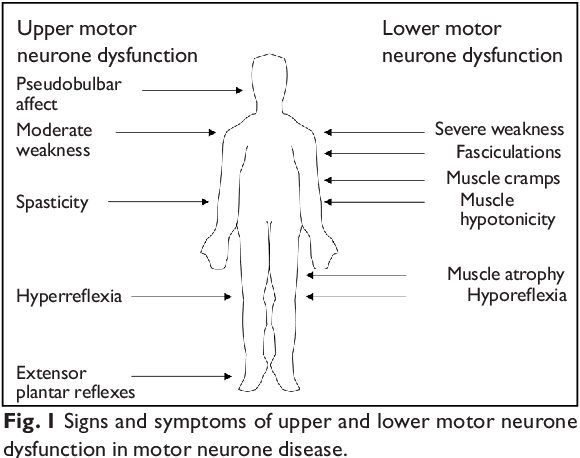
ALS is the most common form of MND, accounting for about 80-90% of all cases. It affects both the upper motor neurones (located in the brain) and the lower motor neurones (located in the spinal cord). ALS symptoms typically begin with muscle weakness and gradually progress to muscle wasting, difficulty speaking and swallowing, and ultimately, paralysis.
Progressive Bulbar Palsy (PBP)
PBP is a type of MND that primarily affects the muscles responsible for speech and swallowing. It is characterized by weakness and wasting of the bulbar muscles, which include the muscles of the face, tongue, and throat. Individuals with PBP often experience slurred speech, difficulty chewing and swallowing, and drooling.
Progressive Muscular Atrophy (PMA)
PMA is a rare type of MND that primarily affects the lower motor neurones in the spinal cord. It is characterized by muscle weakness and wasting, predominantly in the limbs. Unlike ALS, PMA does not typically affect the upper motor neurones in the brain. The progression of PMA is generally slower than that of ALS.
Primary Lateral Sclerosis (PLS)
PLS is a rare form of MND that primarily affects the upper motor neurones in the brain. It is characterized by muscle weakness, stiffness, and spasticity. PLS progresses more slowly than ALS and primarily affects the lower limbs. Individuals with PLS may experience difficulty walking, as well as problems with balance and coordination.
Progressive Multifocal Motor Neuropathy (MMN)
MMN is a rare form of MND that primarily affects the peripheral nerves, leading to muscle weakness and wasting. Unlike other forms of MND, MMN does not involve the degeneration of motor neurones. MMN is characterized by weakness in specific muscles, such as the hands or forearms, which may gradually progress over time.
Hereditary Spastic Paraplegia (HSP)
HSP is a genetic disorder that primarily affects the upper motor neurones in the brain and spinal cord. It is characterized by muscle stiffness and weakness, particularly in the lower limbs. Although it shares some similarities with PLS, HSP is generally considered a distinct condition.
Symptoms of Motor Neurone Disease
Early Symptoms
The early symptoms of MND can vary among individuals and may be subtle at first. Common early symptoms include muscle weakness, twitching, and cramps. These symptoms may initially affect one limb or one side of the body.
Motor Symptoms
As MND progresses, individuals may experience increasing muscle weakness and wasting, leading to difficulties with walking, gripping objects, and performing fine motor tasks. Muscle stiffness and spasticity may also be present, causing the muscles to become tight and resistant to movement.
Respiratory Symptoms
As MND affects the muscles involved in breathing, individuals may experience respiratory symptoms such as shortness of breath, difficulty taking deep breaths, and weak coughing. Severe respiratory complications can occur in advanced stages of the disease and may require ventilatory support.
Speech and Swallowing Difficulties
MND often leads to difficulties with speech and swallowing. Individuals may experience slurred speech, changes in voice quality, and difficulty articulating words. Swallowing difficulties, also known as dysphagia, may cause problems with chewing, swallowing liquids and solids, and increased risk of choking or aspirating.
Cognitive and Emotional Changes
While MND primarily affects the motor neurones, some individuals may also experience cognitive and emotional changes. These can include difficulties with cognition, such as problems with memory, concentration, and decision-making, as well as emotional changes such as mood swings, depression, and anxiety.

Diagnosing Motor Neurone Disease
Medical History and Physical Examination
To diagnose MND, a healthcare professional will start by taking a detailed medical history and conducting a thorough physical examination. They will evaluate the presence of symptoms, assess muscle strength and reflexes, and look for any signs of muscle wasting or fasciculations (muscle twitches).
Tests and Investigations
Various tests and investigations may be ordered to help diagnose MND and rule out other conditions with similar symptoms. These may include blood tests, electromyography (EMG), nerve conduction studies (NCS), magnetic resonance imaging (MRI), and genetic testing.
Electromyography (EMG)
EMG is a diagnostic test used to assess the electrical activity of muscles and the health of motor neurones. During an EMG, a small needle electrode is inserted into the muscle to measure the electrical signals produced by the muscles and the motor neurones that control them. Abnormalities in the EMG findings can indicate motor neurone damage and support a diagnosis of MND.
Nerve Conduction Studies (NCS)
NCS is another diagnostic test that evaluates the function and integrity of peripheral nerves. It involves delivering small electrical impulses to specific nerves and measuring how quickly the impulses travel and the strength of the response. NCS can help identify any abnormalities in the peripheral nerves, which can be associated with certain types of MND.
MRI and Other Imaging Techniques
MRI scans and other imaging techniques, such as magnetic resonance spectroscopy (MRS), may be used to rule out other conditions that may mimic MND. These imaging tests can provide detailed images of the brain and spinal cord, helping to identify any structural abnormalities or signs of alternative causes of the symptoms.
Genetic Testing
In cases where there is a family history of MND or when a genetic form of the disease is suspected, genetic testing may be performed. This involves analyzing an individual’s DNA to detect specific gene mutations associated with MND. Genetic testing can help confirm a diagnosis and provide valuable information for genetic counseling and further management of the condition.
Progression and Prognosis
Stages of Motor Neurone Disease
MND is a progressive disease that follows a general pattern of advancement. It typically starts with mild symptoms and gradually progresses over time. The rate and pattern of progression can vary among individuals. The progression of MND is often divided into three stages: early, middle, and advanced stages. Understanding these stages can help individuals and their caregivers prepare and plan for the challenges that lie ahead.
Factors Affecting Disease Progression
Several factors can influence the progression of MND. These include the type of MND, the age of onset, the rate of disease progression, and individual variations. In general, individuals with ALS tend to have a more rapid disease progression compared to those with other forms of MND.
Prognosis and Life Expectancy
MND is a life-limiting condition, and the prognosis varies depending on the type of MND and individual factors. On average, individuals with ALS have a life expectancy of 2 to 5 years from the time of diagnosis. However, some individuals may live longer, while others may experience a more aggressive disease course. It is important to note that prognosis and life expectancy can be highly individualized, and each person’s journey with MND is unique.
Quality of Life and Supportive Care
While MND is a progressive and debilitating disease, there are various interventions available to support individuals and improve their quality of life. Supportive care plays a crucial role in managing the symptoms and complications of MND, as well as addressing the physical, emotional, and social aspects of the condition. A multidisciplinary approach involving healthcare professionals from different specialties can provide comprehensive care and support tailored to the individual’s needs.
Available Treatment Options
Managing Symptoms and Complications
There is currently no cure for MND, but several treatment options are available to manage the symptoms and complications associated with the disease. These may include medications, non-drug therapies, supportive care, and palliative treatment.
Riluzole and Edaravone
The two main medications approved for the treatment of MND are riluzole and edaravone. Riluzole is believed to slow down the progression of the disease by reducing the release of glutamate, while edaravone is thought to have antioxidant and neuroprotective effects. These medications can help delay disease progression and prolong survival, although their effects vary among individuals.
Ventilation and Breathing Assistance
As MND progresses, respiratory function may become compromised, and individuals may require assistance with breathing. Non-invasive ventilation (NIV) is a commonly used therapy that involves wearing a mask or nasal interface to deliver pressurized air to support breathing. In some cases, invasive ventilation, such as tracheostomy, may be necessary.
Physical and Occupational Therapy
Physical and occupational therapy play a crucial role in maintaining mobility, preventing joint stiffness, and improving overall function in individuals with MND. These therapies focus on exercises, stretches, and adaptive techniques to maximize independence and quality of life. They may also involve the use of assistive devices, such as braces, splints, and wheelchairs.
Speech and Swallowing Therapy
Speech and swallowing therapy, also known as speech and language therapy, can help individuals with MND manage their communication and swallowing difficulties. These therapies may involve techniques and exercises to improve speech clarity, swallowing function, and safe eating.
Nutritional Support
Nutritional support is essential for individuals with MND, as the disease can affect the ability to eat, chew, and swallow. A dietitian or nutritionist can provide guidance on maintaining adequate calorie intake, optimizing nutrition, and managing swallowing difficulties. In some cases, a feeding tube may be recommended to ensure proper nutrition and hydration.
Assistive Devices and Adaptations
Assistive devices and adaptations can help individuals with MND maintain independence and carry out daily activities. These may include mobility aids, such as walking frames or powered wheelchairs, as well as adaptive equipment for eating, dressing, grooming, and other tasks. Occupational therapists and assistive technology specialists can provide guidance and recommendations based on individual needs.
Medication for Motor Neurone Disease
Riluzole as a Disease-Modifying Drug
Riluzole is the only medication currently approved for the treatment of MND that has disease-modifying effects. It works by reducing the release of glutamate, a neurotransmitter that can be toxic to motor neurones in excessive amounts. Riluzole has been shown to modestly prolong survival in individuals with MND and is typically prescribed early in the disease course.
Edaravone as a New Treatment Option
Edaravone is a recently approved medication for the treatment of MND. It is believed to have antioxidant and free radical-scavenging effects, potentially protecting motor neurones from oxidative stress. Clinical trials have shown that edaravone can slow down the decline in functional abilities in certain individuals with MND. It is typically administered intravenously.
Other Medications for Symptom Control
In addition to riluzole and edaravone, several other medications may be used to manage specific symptoms and complications of MND. These may include medications to control muscle cramps, alleviate spasticity, reduce excess saliva production, and manage other symptoms such as pain, sleep disturbances, and mood changes. Individualized treatment plans are essential to address the unique needs of each individual with MND.
Supportive Care and Palliative Treatment
Multidisciplinary Care Team
Supportive care for MND involves a multidisciplinary approach, with healthcare professionals from different specialties working together to provide comprehensive care. This care team may include neurologists, physiotherapists, occupational therapists, speech and language therapists, dietitians, respiratory therapists, social workers, psychologists, and palliative care specialists. Each member of the care team plays a vital role in addressing the physical, emotional, and psychosocial needs of individuals with MND.
Respiratory Support
Respiratory support is a crucial component of supportive care in MND. As the disease progresses, the respiratory muscles may weaken, leading to breathing difficulties. Non-invasive ventilation (NIV) is commonly used to support breathing by delivering pressurized air through a mask or nasal interface. In some cases, invasive ventilation may be required, which involves the surgical creation of a tracheostomy and the use of a ventilator.
Palliative Care and Symptom Control
Palliative care aims to improve the quality of life for individuals with life-limiting conditions, including MND. It focuses on providing relief from symptoms, managing pain, addressing emotional and psychosocial needs, and supporting individuals and their families throughout the disease journey. Palliative care can be initiated at any stage of MND, working alongside other treatments and interventions to provide holistic care.
End-of-Life Care and Advance Directives
End-of-life care becomes an important consideration as MND progresses. Advance care planning, including the creation of advance directives and discussions about end-of-life preferences, ensures that an individual’s wishes regarding medical interventions, life-sustaining treatments, and other considerations are respected. Hospice care may be provided in the final stages of MND to provide comfort and support for both the individual and their loved ones.
In conclusion, Motor Neurone Disease (MND) is a complex neurological condition that affects the motor neurones responsible for controlling voluntary muscle movements. It can have a significant impact on the physical, emotional, and social well-being of individuals affected by the disease. Understanding the causes, symptoms, and available treatment options for MND is crucial in providing comprehensive care and support for those living with this challenging condition. With ongoing research and advancements in medical care, there is hope for improving the management and outcomes for individuals with MND.