Imagine experiencing chronic back pain, stiffness, and fatigue that progressively worsens over time. These are some of the symptoms that individuals with Ankylosing Spondylitis (AS), a form of inflammatory arthritis that primarily affects the spine, may face. If left undiagnosed and untreated, AS can lead to severe complications and a significant reduction in quality of life. However, with early intervention and proper diagnosis, individuals with AS can manage their symptoms effectively and maintain an active and fulfilling lifestyle. In this article, we will explore the process of diagnosing AS and the importance of early intervention in managing this debilitating condition.
What is Ankylosing Spondylitis
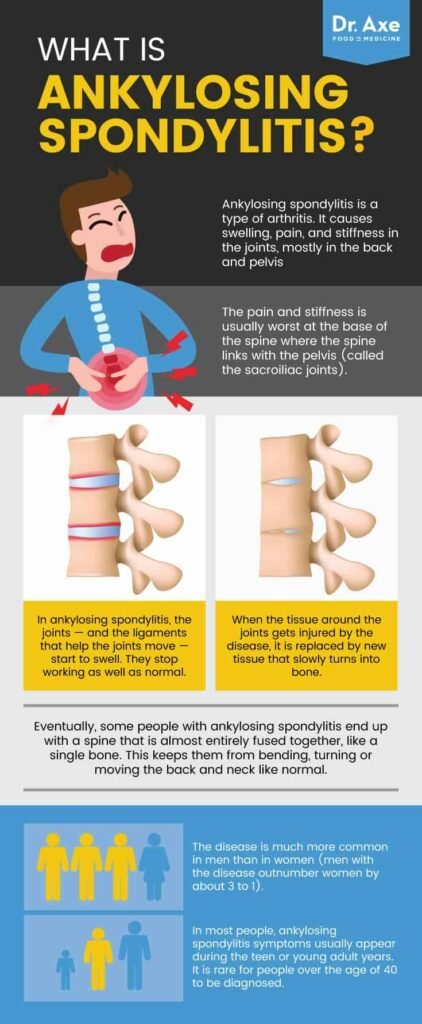
Overview of Ankylosing Spondylitis
Ankylosing Spondylitis is a chronic inflammatory disease that primarily affects the spine, causing pain, stiffness, and potentially leading to joint fusion. However, it can also affect other areas of the body such as the hips, shoulders, and knees. This condition falls under the category of rheumatic diseases, which are characterized by inflammation in the joints, ligaments, and tendons.
Causes and Risk Factors
The exact cause of Ankylosing Spondylitis is still unknown, but researchers believe that a combination of genetic and environmental factors play a role in its development. The HLA-B27 gene is strongly associated with the condition. Other risk factors include a family history of the disease, certain infections, and a history of traumatic injuries to the spine.
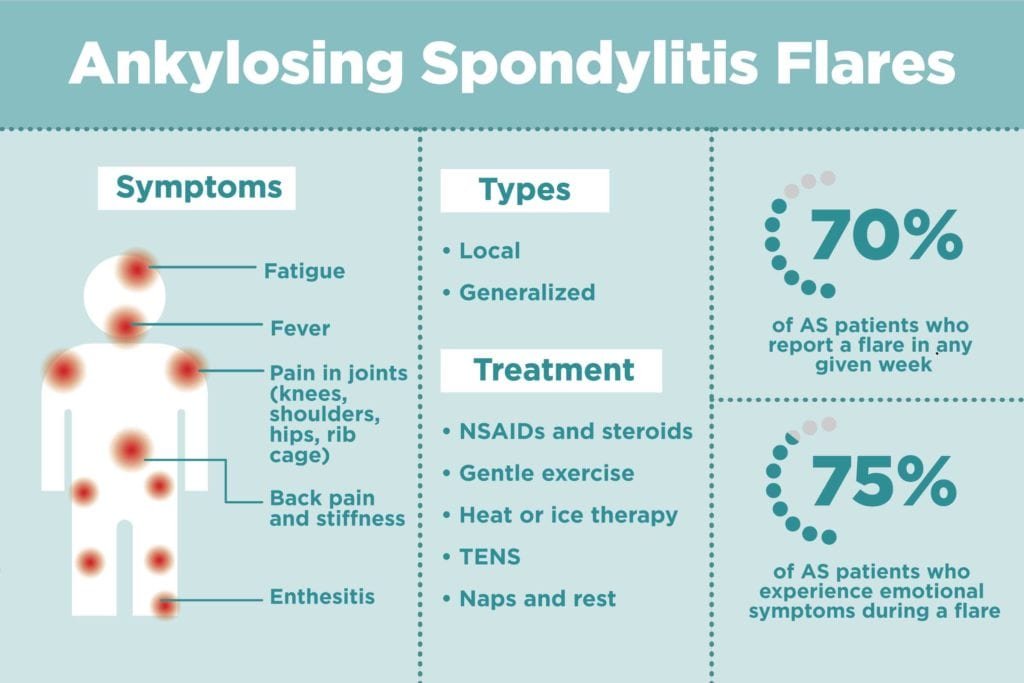
Symptoms and Impact on Quality of Life
The symptoms of Ankylosing Spondylitis can vary from person to person. The most common symptom is chronic back pain and stiffness that worsens with inactivity and improves with movement. Fatigue and sleep disturbances are also frequently reported. As the disease progresses, individuals may experience reduced range of motion in the affected joints and may have difficulty performing daily tasks. Ankylosing Spondylitis can significantly impact an individual’s quality of life, making it important to seek early intervention and management strategies.
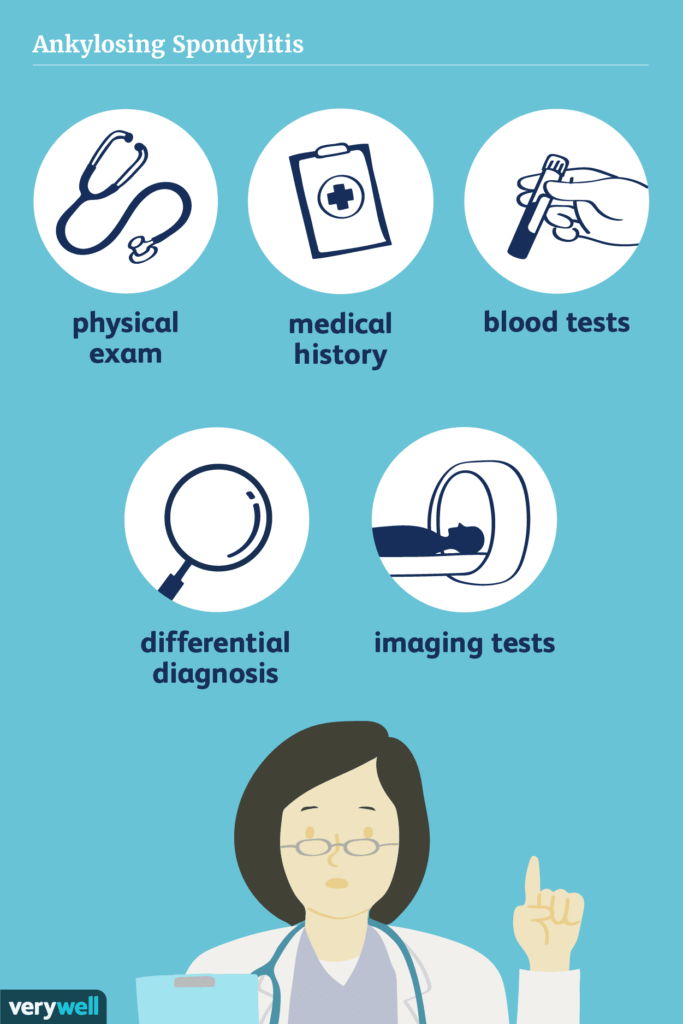
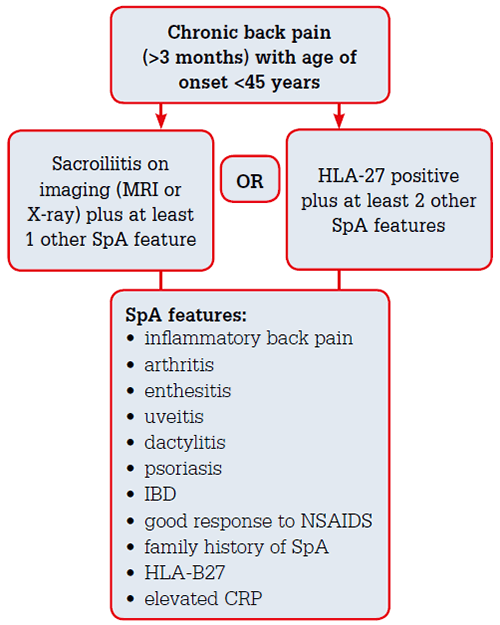
Diagnosing Ankylosing Spondylitis
Clinical Assessment
Ankylosing Spondylitis diagnosis often begins with a clinical assessment, where a healthcare professional will inquire about your symptoms, medical history, and conduct a physical examination. This assessment will help determine if further diagnostic tests are necessary.
Medical History and Physical Examination
During the medical history interview, you will be asked about your symptoms, family history, and any previous injuries or illnesses. This information helps to paint a clearer picture for the healthcare provider and aids in the diagnostic process. A physical examination may involve assessing your range of motion, examining joint tenderness and swelling, and evaluating your overall posture and spine alignment.
Imaging Techniques for Diagnosis
Imaging techniques such as X-rays, magnetic resonance imaging (MRI), and computed tomography (CT) scans may be used to assist in the diagnosis of Ankylosing Spondylitis. These tests can help to visualize inflammation, joint damage, and signs of fusion in the affected areas. They provide valuable insights into the progression and severity of the condition.
Laboratory Tests for Ankylosing Spondylitis
Erythrocyte Sedimentation Rate (ESR)
An Erythrocyte Sedimentation Rate (ESR) blood test can indicate the presence of inflammation in the body. Elevated levels of ESR can be an indication of Ankylosing Spondylitis, although this test alone cannot provide a definitive diagnosis. It is often used in conjunction with other diagnostic tools to help support a diagnosis.
C-reactive Protein (CRP) Level
Similar to the ESR test, the C-reactive protein (CRP) level test measures the presence of inflammation in the body. Elevated levels of CRP can be indicative of active disease activity in Ankylosing Spondylitis. Again, this test is typically used alongside other diagnostic methods to strengthen the diagnostic process.
Human Leukocyte Antigen B27 (HLA-B27) Testing
HLA-B27 testing is a genetic test that can help identify the presence of the HLA-B27 gene, which is strongly associated with Ankylosing Spondylitis. However, it’s important to note that not all individuals with Ankylosing Spondylitis have the HLA-B27 gene, and not all individuals with the gene will develop the condition. Therefore, this test alone cannot provide a definitive diagnosis.
Early Signs and Symptoms of Ankylosing Spondylitis
Back Pain and Stiffness
One of the earliest and most common symptoms of Ankylosing Spondylitis is chronic back pain and stiffness. This pain is often worse in the morning or after periods of inactivity and improves with movement and exercise. Individuals may find relief by engaging in regular physical activity and practicing good posture.
Reduced Range of Motion
As Ankylosing Spondylitis progresses, individuals may experience a reduced range of motion in the affected joints. This limitation can affect daily activities such as bending, twisting, and reaching. Engaging in exercises that target flexibility and range of motion can help maintain joint function and prevent further limitation.
Fatigue and Sleep Disturbances
Fatigue is a common symptom experienced by individuals with Ankylosing Spondylitis. The chronic inflammation and pain associated with the condition can lead to poor sleep quality, making individuals feel tired and drained. It is important to prioritize adequate rest and seek assistance from healthcare professionals if sleep disturbances become a significant issue.

Differential Diagnosis of Ankylosing Spondylitis
Other Causes of Back Pain
While Ankylosing Spondylitis is a common cause of chronic back pain, it is not the only possibility to consider. Other potential causes of back pain include muscle strains, herniated discs, osteoarthritis, and other inflammatory conditions. Seeking an accurate diagnosis is essential to ensure appropriate treatment and management strategies.
Differentiating Ankylosing Spondylitis from Other Rheumatic Diseases
Ankylosing Spondylitis shares similarities with other rheumatic diseases such as psoriatic arthritis, reactive arthritis, and inflammatory bowel disease-associated arthritis. Healthcare professionals will consider various factors, including symptom presentation, medical history, and diagnostic tests, to differentiate between these conditions and accurately diagnose Ankylosing Spondylitis.
Early Intervention Strategies
Education and Awareness
Raising awareness about Ankylosing Spondylitis is crucial for early intervention. Educating individuals about the signs and symptoms of the condition, as well as the importance of seeking medical attention, can lead to earlier diagnoses and improved outcomes. Public health campaigns, outreach programs, and patient resources play key roles in achieving this goal.
Pharmacological Treatments
Pharmacological treatments may be recommended for the management of Ankylosing Spondylitis. Nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly prescribed to alleviate pain and reduce inflammation. Disease-modifying antirheumatic drugs (DMARDs) and biologic therapies may also be utilized to control disease progression and minimize symptoms. It is important to work closely with a healthcare professional to determine the most appropriate treatment plan for individual needs.
Exercise and Physical Therapy
Engaging in regular exercise and physical therapy is essential for individuals with Ankylosing Spondylitis. These interventions can help maintain joint flexibility, improve posture, and reduce pain and stiffness. A combination of strengthening and stretching exercises, along with specialized physical therapy techniques, can significantly enhance overall quality of life and functional ability.
Role of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
Benefits and Risks
Non-steroidal anti-inflammatory drugs (NSAIDs) are commonly used to manage pain and inflammation in Ankylosing Spondylitis. These medications can provide significant relief, allowing individuals to carry out daily activities more comfortably. However, as with any medication, NSAIDs do have potential side effects and risks. These may include gastrointestinal issues, increased risk of cardiovascular events, and kidney problems. It is crucial to discuss these concerns with a healthcare professional and ensure appropriate monitoring.
Appropriate Use and Monitoring
When using NSAIDs, it is important to follow the prescribed dosage and frequency. Regular check-ups and monitoring are essential to assess the effectiveness of the medication, gauge any potential side effects, and make adjustments if necessary. Healthcare professionals will guide individuals on the appropriate use of NSAIDs to achieve the optimal balance between pain relief and risk management.
Biologic Therapies for Ankylosing Spondylitis
Tumor Necrosis Factor (TNF) Blockers
Biologic therapies, specifically tumor necrosis factor (TNF) blockers, have revolutionized the treatment of Ankylosing Spondylitis. These medications target specific molecules in the immune system, reducing inflammation and slowing down disease progression. TNF blockers have been shown to effectively manage symptoms, improve physical function, and enhance overall quality of life for individuals with Ankylosing Spondylitis.
Other Targeted Therapies
In addition to TNF blockers, there are other targeted therapies available for the management of Ankylosing Spondylitis. These include medications that block interleukin-17 (IL-17) and Janus kinase (JAK) inhibitors. While these therapies have shown promising results, it is important to discuss the potential benefits and risks with a healthcare professional to determine the most suitable treatment approach.
Importance of Regular Exercise and Physical Therapy
Strengthening and Stretching Exercises
Regular exercise, particularly strengthening and stretching exercises, plays a crucial role in managing Ankylosing Spondylitis. Strengthening exercises help to build muscle strength and support the affected joints, while stretching exercises improve flexibility and joint mobility. A well-rounded exercise program designed by a physical therapist can help alleviate pain, improve posture, and maintain functional ability.
Posture Correction and Spinal Mobility
Ankylosing Spondylitis can significantly affect posture and spinal mobility. It is important to focus on maintaining proper posture and spinal alignment to reduce the risk of deformities and further limitations. Physical therapists can provide guidance on posture correction techniques and exercises to improve spinal mobility, allowing individuals to maintain an active and independent lifestyle.
Preventing Structural Damage
Early intervention through exercise and physical therapy can help prevent long-term damage caused by Ankylosing Spondylitis. By maintaining joint mobility, muscle strength, and proper posture, individuals can reduce the risk of structural abnormalities such as spinal fusion. Collaboration with healthcare professionals is key in developing a personalized exercise plan that addresses individual needs and goals.
Psychosocial Support and Coping Strategies
Impact on Mental Health
Living with a chronic condition like Ankylosing Spondylitis can have a significant impact on mental health. The physical limitations, pain, and potential lifestyle adjustments can lead to feelings of frustration, anxiety, and depression. It is important to prioritize mental well-being and seek appropriate support when needed.
Support Groups and Counseling
Joining a support group or seeking counseling can provide individuals with Ankylosing Spondylitis the opportunity to connect with others who understand their experiences. Sharing challenges, coping strategies, and success stories within a supportive community can help alleviate feelings of isolation and provide a sense of belonging. Healthcare professionals can also provide valuable guidance and counseling to address psychological concerns.
Stress Management Techniques
Stress can worsen the symptoms of Ankylosing Spondylitis and impact overall well-being. Developing effective stress management techniques is essential for individuals with the condition. Techniques such as deep breathing exercises, mindfulness meditation, and engaging in hobbies and activities that promote relaxation can help reduce stress levels and improve overall mental health.
In conclusion, Ankylosing Spondylitis is a chronic inflammatory disease that primarily affects the spine, causing pain and stiffness. Early intervention through a combination of medication, exercise, and physical therapy plays a vital role in managing symptoms, preventing structural damage, and improving overall quality of life. By seeking prompt diagnosis, appropriate treatment, and psychosocial support, individuals with Ankylosing Spondylitis can effectively manage the condition and enjoy a fulfilling lifestyle. Remember, you are not alone in this journey, and with the right support and care, you can effectively navigate the challenges posed by Ankylosing Spondylitis.