Imagine living with a condition where even small amounts of a commonly consumed protein could wreak havoc on your body. That’s the reality for those diagnosed with Celiac Disease, an autoimmune disorder triggered by gluten. The implications are not only physical but also extend to the emotional and social aspects of daily life. To manage this condition, a gluten-free diet becomes a crucial and necessary lifestyle change. In this article, we will explore the key aspects of a gluten-free diet for Celiac Disease, providing you with valuable insights and tips to navigate this dietary journey with confidence.

Celiac Disease Overview
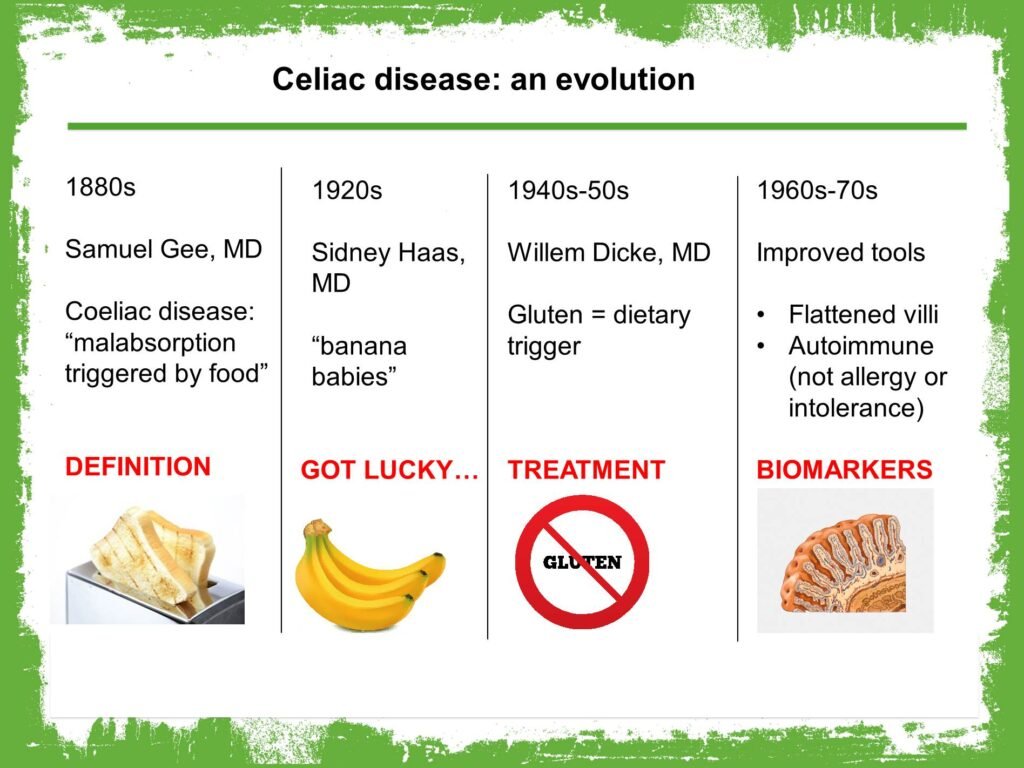
Celiac Disease is a serious autoimmune condition that affects approximately 1 in 100 people worldwide. When an individual with Celiac Disease consumes gluten, a protein found in wheat, barley, and rye, their immune system responds by attacking the lining of the small intestine. This immune response damages the villi, small finger-like projections that line the intestine and are responsible for nutrient absorption. As a result, individuals with Celiac Disease often experience a range of symptoms and potential complications.
Celiac Disease has a genetic component, meaning it tends to run in families. If you have a close relative, such as a parent or sibling, with Celiac Disease, you have a higher risk of developing the condition yourself. Other factors, such as certain infections and early introduction of gluten to an infant’s diet, may also contribute to the development of Celiac Disease. However, the exact causes are still not fully understood and further research is needed to shed more light on the disease.
Symptoms and Diagnosis
The symptoms of Celiac Disease can vary widely from person to person, making diagnosis a complex process. Common symptoms include bloating, diarrhea, constipation, abdominal pain, and fatigue. Some individuals may also experience weight loss, anemia, bone or joint pain, depression, and skin rashes. In children, Celiac Disease can result in growth problems, delayed puberty, and dental enamel defects.
To diagnose Celiac Disease, your doctor will first perform a physical examination and review your medical history. They may then recommend blood tests to look for specific antibodies associated with the disease. These antibodies include anti-tissue transglutaminase (tTG) and anti-endomysial antibodies (EMA). If the blood tests suggest Celiac Disease, your doctor may proceed with an intestinal biopsy to confirm the diagnosis. During a biopsy, a small sample of the small intestine is taken and examined for damage to the villi.
Prevalence and Demographics
Celiac Disease can affect people of all ages and ethnicities. While it was once considered a rare condition, it is now recognized as one of the most common genetic autoimmune disorders worldwide. It is estimated that around 1% of the global population has Celiac Disease, with higher prevalence rates observed in certain populations, such as those of European descent.
Interestingly, Celiac Disease affects women more frequently than men. Studies have shown that women are diagnosed with Celiac Disease at a ratio of nearly 2 to 1 compared to men. The reason for this gender disparity is not fully understood but may be related to hormonal factors or differences in immune response.
Understanding Gluten
What is Gluten?
Gluten is a protein composite found in several grains, including wheat, barley, and rye. It provides elasticity to dough, helping it rise and giving it a chewy texture. Gluten is also commonly used as a food additive in processed foods to enhance texture and flavor.
Sources of Gluten
Gluten can be found in a wide variety of foods, making it important for individuals with Celiac Disease to be vigilant about their dietary choices. Foods that commonly contain gluten include bread, pasta, cereals, cookies, cakes, pies, and beer. It can also be found in less obvious sources, such as soups, sauces, dressings, and even some medications and vitamins.
In addition to foods, individuals with Celiac Disease must be cautious about cross-contamination. This occurs when gluten-containing foods come into contact with gluten-free foods or preparation surfaces. For example, using the same toaster for gluten-free and regular bread can lead to cross-contamination.
Gluten Intolerance vs. Celiac Disease
It’s important to note that Celiac Disease is different from gluten intolerance, also known as non-celiac gluten sensitivity. While both conditions involve an adverse reaction to gluten, the underlying mechanisms and potential complications can differ.
Celiac Disease is an autoimmune condition, where the body’s immune system mistakenly attacks gluten, causing damage to the small intestine. Gluten intolerance, on the other hand, is a less well-defined condition characterized by gastrointestinal symptoms, such as bloating and diarrhea, that improve when gluten is eliminated from the diet. Unlike Celiac Disease, gluten intolerance does not involve an autoimmune response or damage to the small intestine.

Gluten-Free Diet Basics
The Importance of a Gluten-Free Diet for Celiac Disease
Following a strict gluten-free diet is the only known treatment for Celiac Disease. By eliminating gluten from your diet, you can reduce inflammation in the small intestine and allow the villi to heal. This, in turn, can alleviate symptoms and prevent further complications.
Failure to adhere to a gluten-free diet can have serious consequences for individuals with Celiac Disease. Prolonged exposure to gluten can result in nutritional deficiencies, weakened immune function, osteoporosis, infertility, and an increased risk of certain cancers, such as lymphoma.
What Foods to Avoid
The most crucial step in managing Celiac Disease is to avoid foods that contain gluten. This means eliminating all sources of wheat, barley, and rye from your diet. As mentioned earlier, this includes foods like bread, pasta, cakes, and cookies. It’s essential to read food labels carefully, as gluten can sometimes be hidden under different names, such as modified food starch or malt.
In addition to these grains, individuals with Celiac Disease must be cautious about cross-contamination. This means avoiding foods that may have come into contact with gluten during processing or preparation. For example, oats are naturally gluten-free, but they are often processed in facilities that also handle wheat, resulting in possible cross-contamination.
What Foods Are Safe to Eat
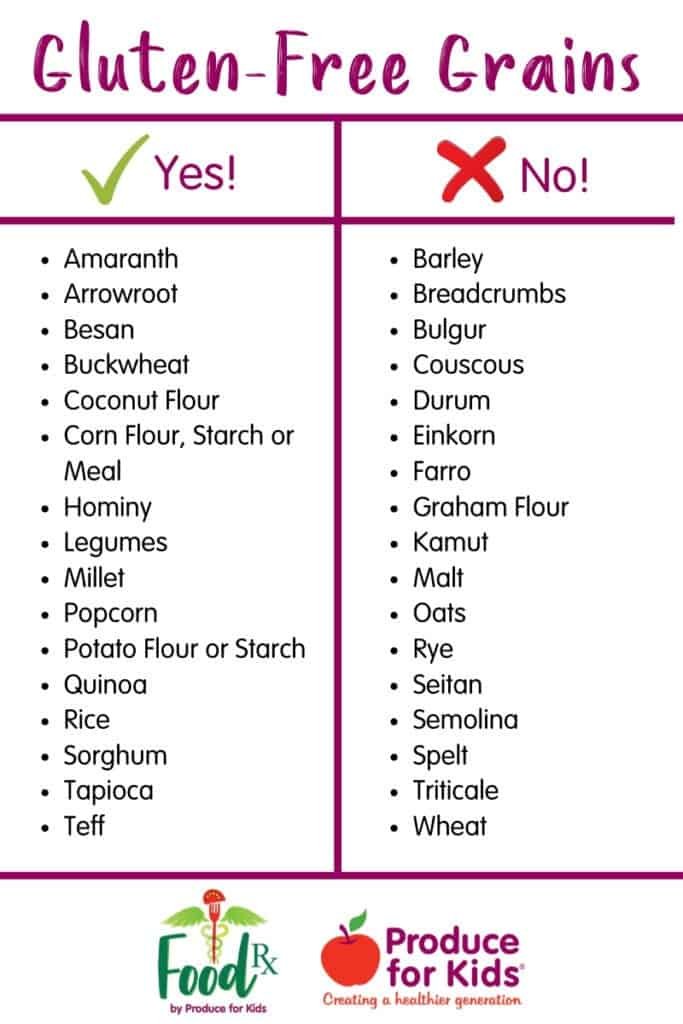
Although many staple foods are off-limits on a gluten-free diet, there are still plenty of options available. Naturally gluten-free grains, such as rice, quinoa, millet, and buckwheat, can be incorporated into your meals. Fruits, vegetables, lean meats, fish, eggs, and dairy products are also safe to consume.
Fortunately, there is an increasing availability of gluten-free versions of popular foods, such as bread, pasta, and cookies. These products are made from alternative grains and flours, such as almond flour, coconut flour, or cassava flour. It’s important to note that while these gluten-free alternatives are suitable for individuals with Celiac Disease, they may not be suitable for those with gluten intolerance, as they can still contain other potential triggers.
Gluten-Free Food Substitutes
Grains and Flours Substitutes
When it comes to finding alternatives for grains and flours, there is a wide variety of options available. Rice flour, cornmeal, potato flour, and tapioca flour are all gluten-free alternatives that can be used in baking or cooking. These substitutes can help recreate the texture and taste of gluten-containing foods.
Additionally, there are alternative grains and flours that are naturally gluten-free and provide a range of nutritional benefits. For example, quinoa is a complete protein and high in fiber, while almond flour and coconut flour are rich in healthy fats. Experimenting with these substitutes can open up a whole new world of culinary possibilities.
Bread and Pasta Alternatives
One of the most challenging aspects of following a gluten-free diet is finding suitable bread and pasta alternatives. Fortunately, there are now many gluten-free options available in stores or online. These products are typically made from alternative grains or flours, such as rice flour, tapioca starch, or chickpea flour.
In recent years, there has been a surge in popularity of gluten-free baking, resulting in a wider availability of gluten-free bread and pasta recipes. Many gluten-free cookbooks and online resources offer recipes for homemade bread and pasta, allowing you to tailor them to your taste preferences and dietary needs.
Gluten-Free Baking Tips
Baking without gluten can be a bit of a learning curve, but with practice and the right techniques, you can achieve delicious results. Here are a few tips to help you navigate gluten-free baking:
-
Use a mix of gluten-free flours: Combining different gluten-free flours, such as rice, almond, and tapioca flour, can help mimic the texture of gluten-containing treats.
-
Add binding agents: Gluten provides elasticity and structure to baked goods. To achieve similar results in gluten-free baking, you can include binding agents like xanthan gum or guar gum.
-
Increase moisture: Gluten-free flours tend to absorb more moisture than their gluten-containing counterparts. It’s important to add extra moisture, such as additional eggs or apple sauce, to prevent dryness.
-
Experiment and have fun: Have patience and be willing to experiment with different ingredients and techniques. Gluten-free baking is a journey of trial and error, but the reward is creating delicious treats that are safe for individuals with Celiac Disease.
Meal Planning and Grocery Shopping
Creating a Gluten-Free Meal Plan
Meal planning is a valuable tool for individuals with Celiac Disease, as it ensures that you have a variety of safe and nutritious meals throughout the week. When creating a gluten-free meal plan, start by identifying gluten-free sources of carbohydrates, such as rice, quinoa, or potatoes. Then, select lean proteins, such as chicken, fish, or tofu, and incorporate a range of fruits and vegetables.
It can be helpful to prepare a weekly shopping list based on your meal plan. This ensures that you have all the necessary ingredients on hand, reducing the temptation to rely on convenience foods or risk consuming gluten-containing foods.
Tips for Shopping Gluten-Free
Grocery shopping for a gluten-free diet requires careful attention to detail. Here are some tips to help you navigate the aisles and make informed choices:
-
Familiarize yourself with gluten-free labels: Look for the “gluten-free” label on products. This indicates that the product has been tested and is considered safe for individuals with Celiac Disease.
-
Review ingredient lists: Even if a product doesn’t have a gluten-free label, carefully read the ingredient list. Avoid anything containing wheat, barley, rye, or any ingredients with gluten-derived names.
-
Shop the perimeter: The perimeter of the grocery store is often where you’ll find fresh produce, lean meats, and other naturally gluten-free foods. This can help guide your shopping and reduce the temptation to browse processed food aisles.
-
Be cautious with processed foods: Many processed foods, such as ready-made meals, sauces, and snacks, can contain hidden sources of gluten. Always read the ingredient list or choose certified gluten-free options when available.
Reading Food Labels
Understanding food labels is crucial for individuals with Celiac Disease, as it allows you to identify potential sources of gluten in packaged foods. When reading labels, focus on the following key points:
-
Look for the “gluten-free” label: As mentioned earlier, this label is an easy way to identify products that are safe for individuals with Celiac Disease.
-
Check for allergen warnings: Manufacturers often include allergen warnings, such as “Contains: wheat” or “May contain traces of wheat.” These alerts can help you determine if a product is safe to consume.
-
Learn to identify gluten-derived ingredients: Familiarize yourself with common ingredients that contain gluten, such as modified food starch, malt, or hydrolyzed vegetable protein. If you come across any of these ingredients on a food label, it’s best to avoid the product or seek clarification from the manufacturer.
-
Check for safe handling practices: Some food labels may state that the product is processed in a facility that also handles wheat. This indicates a risk of cross-contamination, making it important to assess your personal tolerance for such products.
-
Reach out to manufacturers if unsure: If you have any doubts about a particular product or its suitability for your gluten-free diet, don’t hesitate to contact the manufacturer directly. They can provide more detailed information and help address your concerns.
Food Preparation and Cross Contamination
Preventing Cross-Contamination in the Kitchen
In a shared kitchen, preventing cross-contamination is crucial to ensure the safety of individuals with Celiac Disease. Here are some steps you can take to minimize the risk:
-
Designate gluten-free areas: If possible, designate specific areas or countertops for gluten-free food preparation. This reduces the chance of gluten coming into contact with gluten-free ingredients.
-
Use separate cooking utensils and cutting boards: It’s important to use separate cooking utensils, such as knives and spoons, for gluten-free and gluten-containing foods. The same applies to cutting boards.
-
Clean and sanitize surfaces: Thoroughly clean and sanitize all surfaces, utensils, and equipment before and after use. This removes any potential residual gluten and reduces the risk of cross-contamination.
-
Avoid shared condiments: Sharing condiments that may have come into contact with gluten can lead to cross-contamination. It’s best to have separate jars or bottles for gluten-free options.
Safe Food Handling Practices
Safe food handling practices are essential to ensure the safety of individuals with Celiac Disease. Here are some guidelines to follow:
-
Wash your hands: Always wash your hands thoroughly before and after handling gluten-free ingredients. This prevents the transfer of gluten or other potential contaminants.
-
Use separate cooking utensils: As mentioned earlier, using separate utensils, such as spoons or tongs, for gluten-free and gluten-containing foods is crucial to prevent cross-contamination.
-
Avoid double-dipping: Double-dipping with utensils that have touched gluten can contaminate gluten-free foods. It’s best to use separate utensils or pour condiments into a separate dish.
-
Store gluten-free foods separately: When storing food, keep gluten-free items separate from gluten-containing ones to avoid accidental cross-contamination.
Eating Out Safely
Eating out can present challenges for individuals with Celiac Disease, as it can be more difficult to control and ensure the avoidance of gluten. However, with careful planning and communication, it is possible to dine out safely. Here are some tips to consider:
-
Research restaurants in advance: Prior to dining out, research restaurants that offer gluten-free options and have a good understanding of cross-contamination prevention. Many restaurants now have gluten-free menus available, either online or upon request.
-
Speak to the restaurant staff: When you arrive at the restaurant, inform the staff about your dietary requirements. Ask questions about their gluten-free offerings, preparation methods, and cross-contamination protocols.
-
Be detailed when ordering: Clearly communicate your dietary restrictions to your server and be specific about what you can and cannot eat. Ask for your meal to be prepared separately and for any sauces or dressings to be served on the side.
-
Be cautious with buffets and self-serve stations: Buffets and self-serve stations pose a higher risk of cross-contamination. Assess the situation carefully and, if necessary, speak with the staff to ensure the safety of your meal.
By being proactive and taking precautions, you can enjoy dining out without compromising your health.

Nutritional Considerations
Potential Nutrient Deficiencies in a Gluten-Free Diet
Following a gluten-free diet can sometimes lead to nutritional deficiencies, as it restricts several food groups that are important sources of certain nutrients. Here are some potential nutrient deficiencies to be aware of:
-
Fiber: Many gluten-free products lack the fiber content found in whole wheat products. To ensure an adequate intake of fiber, focus on incorporating naturally gluten-free sources, such as fruits, vegetables, and gluten-free grains like quinoa or brown rice.
-
B vitamins: Fortified wheat products are a significant source of B vitamins, including folate, riboflavin, and thiamine. It is important to look for gluten-free products that are fortified with these essential nutrients or consider taking supplements.
-
Iron: Iron deficiency anemia is relatively common in individuals with Celiac Disease. This is due to the damage to the small intestine, which can impair iron absorption. Include iron-rich foods such as lean meats, seafood, legumes, and leafy green vegetables in your diet. Additionally, consuming vitamin C-rich foods alongside iron-rich foods can enhance iron absorption.
-
Calcium and Vitamin D: Some individuals with Celiac Disease may experience low bone density, putting them at an increased risk of osteoporosis. Dairy products fortified with calcium and vitamin D, as well as leafy green vegetables and fortified plant-based milk alternatives, can help support bone health.
Supplements and Fortified Foods
In some cases, dietary changes alone may not be sufficient to meet your nutritional needs. Your healthcare provider may recommend certain supplements or fortified foods to address specific nutrient deficiencies. Here are some commonly recommended supplements for individuals with Celiac Disease:
-
Multivitamin/mineral supplement: A daily multivitamin/mineral supplement can help ensure you are getting a broad range of essential nutrients. Look for gluten-free options and consult with your healthcare provider for guidance on the appropriate dosage.
-
Vitamin B12: Vitamin B12 is primarily found in animal-based foods, making it important for individuals following a strict gluten-free and plant-based diet to consider supplementation. Speak to your healthcare provider to determine if you would benefit from B12 supplementation.
-
Probiotics: Probiotics are beneficial bacteria that support gut health. They may be particularly helpful for individuals with Celiac Disease, as their gut microbiome may be imbalanced due to long-term gluten exposure. Consult with your healthcare provider to select a suitable probiotic supplement.
-
Calcium and vitamin D: Supplementing with calcium and vitamin D may be necessary if you are unable to meet your requirements through diet alone. Your healthcare provider can guide you on the appropriate dosage and duration of supplementation.
Fortified foods, such as gluten-free bread and cereals, can also be a valuable source of additional nutrients. Look for products that are fortified with vitamins and minerals, such as iron, calcium, and B vitamins, to help bridge any potential nutritional gaps.
Balancing Nutrient Intake
Maintaining a well-balanced diet is essential for individuals with Celiac Disease to ensure they are getting all the necessary nutrients. Here are some general guidelines to help you balance your nutrient intake:
-
Diversify your diet: Aim to incorporate a wide variety of foods from different food groups. This helps ensure you are getting a range of essential nutrients.
-
Eat nutrient-dense foods: Choose foods that pack a nutritional punch, such as fruits, vegetables, lean proteins, and healthy fats. These foods provide vitamins, minerals, and other important nutrients without unnecessary additives.
-
Monitor portion sizes: Be mindful of portion sizes to avoid overeating or under-eating. Balancing your plate with appropriate portions of carbohydrates, proteins, and fats can help ensure you are meeting your nutrient needs.
-
Consult with a registered dietitian: If you’re unsure about meeting your specific nutrient requirements or have concerns about your nutrition, consider consulting with a registered dietitian who specializes in Celiac Disease. They can provide personalized guidance and support to help you optimize your diet.
Managing Celiac Disease in Social Settings
Navigating Parties and Gatherings
Attending parties and gatherings can be challenging when you have Celiac Disease, as it’s often difficult to know if the food being served is gluten-free. Here are some strategies to navigate social events successfully:
-
Communicate with the host: Reach out to the host in advance and explain your dietary needs. Offer to bring a gluten-free dish to share, ensuring there will be at least one safe option available.
-
Eat before you go: Consider having a meal or snack before attending an event, especially if you’re uncertain about the food that will be served. This can help prevent hunger and reduce the temptation to eat potentially unsafe foods.
-
BYOGF (Bring Your Own Gluten-Free): If you’re unsure about the food options, bring your own gluten-free snacks or treats to enjoy. This way, you can still participate in the social gathering without compromising your health.
Communicating Dietary Needs
Open and effective communication about your dietary needs is key to ensuring your safety and well-being when dining with others. Here are some tips for communicating your dietary needs:
-
Be clear and concise: Clearly explain your dietary restrictions to others, emphasizing that consuming even small amounts of gluten can have serious consequences for your health.
-
Offer alternatives or suggestions: If someone is preparing a meal for you, offer alternative ingredients or suggest simple gluten-free recipes that they can follow.
-
Educate others about cross-contamination: Many people may not be aware of the concept of cross-contamination. Explain how even a small trace of gluten can trigger an immune response, and ask for their support in preventing cross-contamination during food preparation and serving.
-
Be appreciative: Show gratitude whenever someone goes out of their way to accommodate your dietary needs. A simple thank you can go a long way in fostering understanding and support.
Resources for Support
Living with Celiac Disease can sometimes feel overwhelming, but there are numerous resources available to help you navigate the challenges. Here are some valuable sources of support:
-
Celiac support groups: Joining a support group can provide an opportunity to connect with others who are living with Celiac Disease. These groups often offer a wealth of information, resources, and emotional support.
-
Online communities and forums: There are many online communities and forums where individuals with Celiac Disease can share their experiences, ask questions, and offer support to one another. These platforms can be a valuable source of information and a place to find encouragement.
-
Registered dietitians: Consulting with a registered dietitian who specializes in Celiac Disease can provide personalized guidance and support. They can help you navigate dietary challenges and develop strategies to optimize your nutrition.
-
Celiac Disease organizations: There are several reputable organizations that provide comprehensive information and support for individuals with Celiac Disease. These organizations often have websites, educational materials, and helplines where you can seek assistance and gather reliable information.
Celiac Disease and Other Health Conditions
Link between Celiac Disease and Other Autoimmune Disorders
Celiac Disease is closely associated with other autoimmune disorders, meaning conditions in which the immune system mistakenly attacks healthy tissues. Some of the autoimmune disorders that have a higher prevalence in individuals with Celiac Disease include:
-
Type 1 diabetes: There is a strong link between Celiac Disease and type 1 diabetes. Studies have shown that individuals with type 1 diabetes have a higher risk of developing Celiac Disease, and vice versa.
-
Autoimmune thyroid diseases: Conditions such as Hashimoto’s thyroiditis and Graves’ disease are more common in individuals with Celiac Disease. It is thought that shared genetic factors and the presence of an autoimmune response contribute to this association.
-
Rheumatoid arthritis: Celiac Disease and rheumatoid arthritis share certain genetic factors, leading to an increased risk of developing both conditions.
-
Dermatitis herpetiformis: Dermatitis herpetiformis is a skin condition characterized by itchy, blistering rashes. It is often associated with Celiac Disease, with gluten triggering the immune response that leads to these skin symptoms.
While there is a correlation between Celiac Disease and other autoimmune disorders, it’s important to note that having one condition does not necessarily mean you will develop another. Regular medical check-ups are crucial for early detection and management of any potential associated health conditions.
Associated Health Conditions
In addition to autoimmune disorders, Celiac Disease is associated with several other health conditions. These conditions may occur concurrently or arise as a result of undiagnosed or untreated Celiac Disease. Some of the health conditions associated with Celiac Disease include:
-
Osteoporosis: Celiac Disease can impair calcium absorption, leading to decreased bone density and an increased risk of osteoporosis. Adequate calcium and vitamin D intake, along with a gluten-free diet, can help minimize this risk.
-
Infertility and miscarriages: Women with undiagnosed or untreated Celiac Disease may be more likely to experience infertility or recurrent miscarriages. Adhering to a strict gluten-free diet can improve fertility outcomes in these cases.
-
Lactose intolerance: Damage to the small intestine can impair the production of lactase, the enzyme needed to digest lactose, leading to lactose intolerance in some individuals with Celiac Disease.
-
Neurological disorders: Celiac Disease has been associated with various neurological complications, including peripheral neuropathy, migraines, ataxia, and epilepsy. These conditions often improve or resolve with a gluten-free diet.
It’s important to work closely with your healthcare provider to monitor and manage any associated health conditions that may arise as a result of Celiac Disease.
Importance of Regular Medical Check-ups
Regular medical check-ups are essential for individuals with Celiac Disease to monitor their health and address any potential complications. Here’s why regular check-ups are important:
-
Monitoring gluten-free diet adherence: Regular check-ups provide an opportunity for healthcare providers to assess how well you are adhering to a gluten-free diet. They can review your dietary habits and address any challenges or questions you may have.
-
Assessing nutritional status: Regular check-ups allow healthcare professionals to monitor your nutritional status and identify any nutrient deficiencies or imbalances. They can provide guidance on optimizing your diet or recommend appropriate supplements if needed.
-
Screening for associated health conditions: Healthcare providers will often perform routine screenings for associated health conditions, such as autoimmune disorders or deficiencies. Early detection and intervention can lead to better management and improved outcomes.
-
Reviewing disease management: Regular visits enable your healthcare provider to assess how well your Celiac Disease is being managed and make adjustments to your treatment plan if necessary. They can also address any new symptoms or concerns you may have.
Keeping up with regular medical check-ups is an important aspect of managing Celiac Disease and maintaining your overall health and wellbeing.
Living Well with Celiac Disease
Tips for Maintaining a Positive Mindset
Adjusting to a gluten-free lifestyle can be challenging, especially in the beginning. Here are some tips to help you maintain a positive mindset:
-
Educate yourself: Learn as much as you can about Celiac Disease, gluten-free living, and available resources. Empower yourself with knowledge, as this can help you feel more confident in managing your condition.
-
Connect with others: Reach out to others living with Celiac Disease or join support groups to connect with individuals who understand your experience. Sharing your journey, challenges, and successes with others can provide encouragement and support.
-
Focus on what you can eat: Instead of dwelling on foods you can’t have, focus on exploring new gluten-free recipes and discovering delicious alternatives. This can help you appreciate the diverse range of foods available to you.
-
Celebrate milestones and achievements: Recognize and celebrate your achievements along the way. Whether it’s successfully avoiding gluten in a social setting or trying a new gluten-free recipe, give yourself credit for your efforts.
Educating Family and Friends
Educating your family and friends about Celiac Disease is crucial to gaining their support and understanding. Here’s how you can effectively educate your loved ones:
-
Provide reliable information: Share reputable resources or literature about Celiac Disease to help others understand the condition better. Point them to credible websites or suggest brochures and books that explain the disease.
-
Explain your symptoms and dietary needs: Clearly communicate your symptoms, dietary restrictions, and the seriousness of gluten exposure. Help your loved ones understand the potential consequences of cross-contamination or accidental gluten ingestion.
-
Offer guidance: Educate your family and friends on how they can support you. This may involve discussing safe food preparation practices, labeling gluten-free items in shared kitchen spaces, or being mindful of cross-contamination when eating together.
-
Encourage open communication: Foster an environment where open communication is encouraged. Encourage loved ones to ask questions and express any concerns they may have so that you can address them together.
By involving your family and friends and educating them about Celiac Disease, you can create a supportive network that will help you navigate the challenges you may face.
Future Research and Advancements
Research in the field of Celiac Disease is ongoing, aiming to improve diagnosis, treatment, and the overall management of the condition. Here are some areas of future research and potential advancements:
-
Improved diagnostic methods: Researchers are exploring alternative diagnostic tools and techniques that may be more accurate, sensitive, and convenient for diagnosing Celiac Disease. This includes investigations into non-invasive tests, such as saliva or blood tests.
-
Development of gluten-detectors: Efforts are underway to develop portable gluten-detectors that can detect trace amounts of gluten in food. These devices would significantly aid individuals with Celiac Disease in verifying the safety of their meals.
-
Advancements in gluten-free products: Manufacturers are constantly innovating to improve the taste, texture, and variety of gluten-free products. Future advancements may include the development of gluten-free alternatives that closely resemble gluten-containing foods.
-
Potential treatment options: Researchers are exploring various treatment options for Celiac Disease, such as medications that act on the immune response or enzymes that can break down gluten in the digestive system. These treatments may potentially reduce the impact of accidental gluten exposure or offer additional support alongside a gluten-free diet.
As research progresses, individuals with Celiac Disease can look forward to continued advancements that will enhance their quality of life and make managing the condition easier.
Living with Celiac Disease requires commitment, education, and a positive mindset. By understanding the disease, adhering to a gluten-free diet, and seeking support when needed, you can lead a healthy and fulfilling life. Remember, you are not alone on this journey. Reach out to healthcare professionals, support groups, and loved ones for guidance and encouragement. With the right tools and resources, you can navigate the challenges of Celiac Disease and thrive.