Imagine feeling perfectly healthy one day, and then suddenly being overcome by a severe form of pneumonia. This is the reality for thousands of people every year who are diagnosed with Legionnaires’ Disease. This article aims to provide a comprehensive understanding of this lesser-known but potentially life-threatening illness. From its origins to its symptoms and treatments, you will gain valuable insights into Legionnaires’ Disease and the precautions you can take to protect yourself. So, let’s explore this important topic together and arm ourselves with knowledge.

What is Legionnaires’ Disease?
Legionnaires’ Disease is a severe form of pneumonia caused by the Legionella bacteria. It was first recognized in 1976 when an outbreak occurred among attendees of an American Legion convention in Philadelphia. This disease is not contagious and is typically contracted by inhaling small droplets of water contaminated with Legionella bacteria. Legionnaires’ Disease can be life-threatening, especially for individuals with weakened immune systems or underlying health conditions. Understanding the causes, symptoms, risk factors, prevention, treatment, and impact of Legionnaires’ Disease is crucial for public health and individual well-being.
Overview of Legionnaires’ Disease
Legionnaires’ Disease is caused by Legionella bacteria, primarily Legionella pneumophila. This bacterium is commonly found in freshwater environments, such as rivers and lakes, as well as artificial water systems like hot tubs, cooling towers, and plumbing systems. When the Legionella bacteria multiply and are released into the air, they can be inhaled into the lungs, leading to infection.
Legionnaires’ Disease can manifest in various ways, ranging from mild respiratory problems to severe pneumonia. This can pose challenges in its diagnosis and treatment. Typically, symptoms appear within 2 to 10 days after exposure to the bacteria.
History of Legionnaires’ Disease
Legionnaires’ Disease gained public attention and its name from the infamous outbreak at the Bellevue-Stratford Hotel in Philadelphia in 1976. Over 200 attendees of the American Legion convention fell ill, resulting in 34 deaths. This event led to investigations and the discovery of a new bacterium, later named Legionella. Since then, numerous outbreaks have been reported worldwide, contributing to our understanding of the disease and the development of preventive measures.
Causes of Legionnaires’ Disease
The primary cause of Legionnaires’ Disease is the inhalation of Legionella-contaminated water droplets. Legionella bacteria can multiply in stagnant water environments with temperatures between 20 to 45 degrees Celsius (68 to 113 degrees Fahrenheit). These bacteria are more commonly found in man-made water systems with complex structures, such as hot water tanks, cooling towers, and plumbing systems. Factors such as water temperature, pH levels, and the presence of biofilms contribute to the growth and spread of Legionella bacteria.
Symptoms and Diagnosis
Common Symptoms
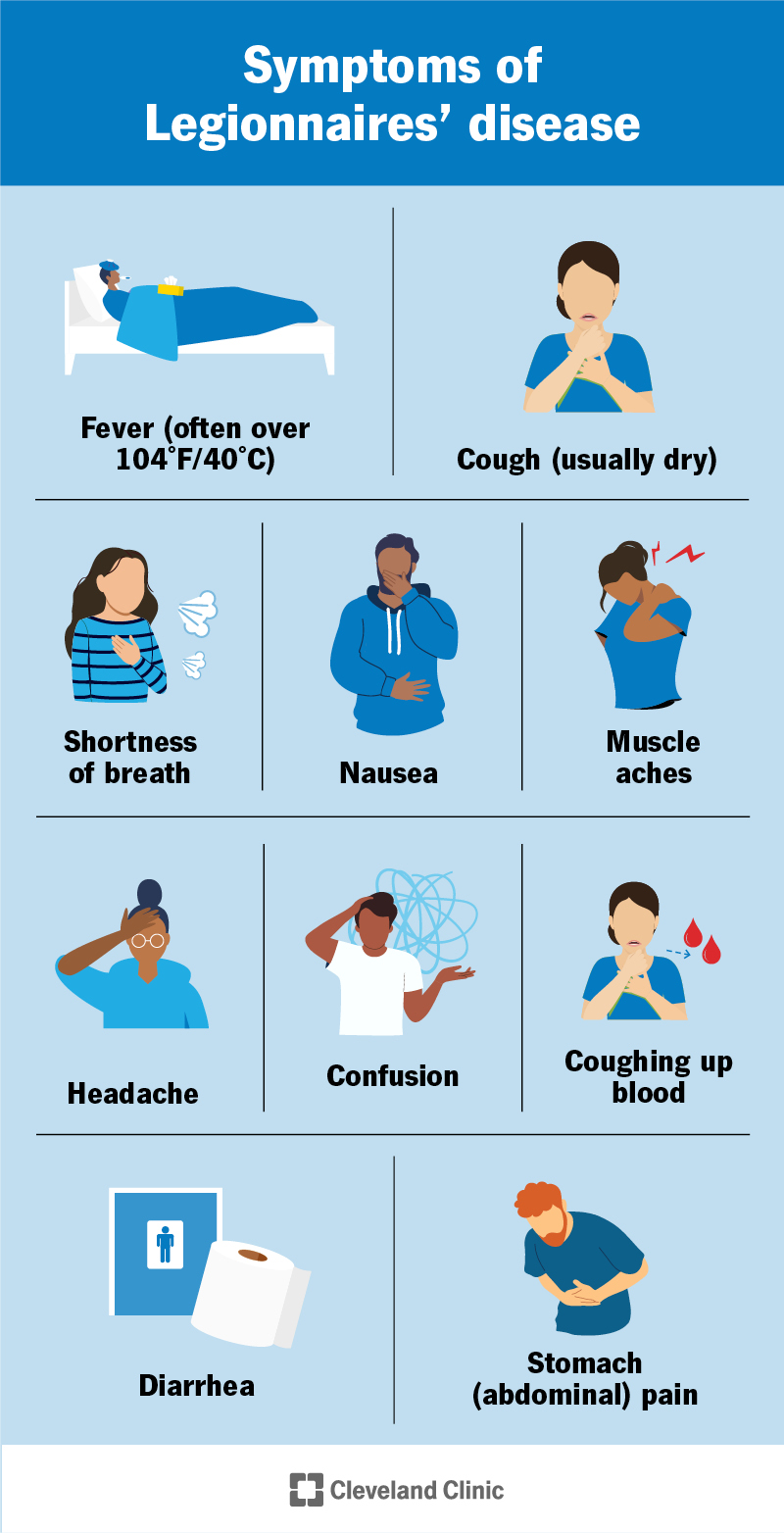
Legionnaires’ Disease can present with a range of symptoms, primarily affecting the respiratory system. The most common symptoms include fever, cough, shortness of breath, muscle aches, and headaches. Some individuals may also experience gastrointestinal symptoms like nausea, vomiting, and diarrhea. The severity of symptoms varies, with some individuals experiencing mild illness, while others may develop severe pneumonia.
Diagnostic Methods
Diagnosing Legionnaires’ Disease can be challenging due to its similarity to other respiratory illnesses. Healthcare professionals rely on several diagnostic methods to confirm a Legionella infection. These include laboratory tests such as urine antigen testing, sputum culture, and serology tests. Additionally, chest X-rays or computed tomography (CT) scans may be utilized to assess lung health and detect any abnormalities.
Differences from Other Respiratory Illnesses
Legionnaires’ Disease can be distinguished from other respiratory illnesses, such as the common cold or flu, based on several factors. While the common cold and flu are usually caused by viruses, Legionnaires’ Disease is caused by bacteria. The severity and persistence of symptoms, such as high fever and pneumonia, are also indicators of Legionnaires’ Disease. Prompt diagnosis and treatment are crucial to prevent complications and ensure a better prognosis.
Risk Factors
Individual Risk Factors
Certain individuals are more susceptible to contracting Legionnaires’ Disease. Those with weakened immune systems, such as the elderly, individuals with chronic illnesses, or those undergoing immunosuppressive therapies, have a higher risk of infection. Smokers and individuals with lung diseases or compromised respiratory function are also more vulnerable to severe illness if exposed to Legionella bacteria.
Environmental Risk Factors
The presence of Legionella bacteria is closely associated with specific environmental conditions. Buildings with complex water systems, poor maintenance practices, and inadequate water treatment measures are at a higher risk of harboring Legionella bacteria. Additionally, stagnant water, water sources with high temperatures, and the formation of biofilms provide favorable conditions for Legionella growth. Understanding and mitigating these environmental risk factors are essential for preventing Legionnaires’ Disease outbreaks.
Prevention
Water Management and Treatment
Effective water management and treatment play a crucial role in preventing Legionnaires’ Disease. Regular monitoring and maintenance of water systems, including cooling towers, hot tubs, and plumbing systems, are essential to minimize the risk of Legionella growth. Implementing measures such as disinfection, temperature control, and periodic cleaning can help control bacterial growth and reduce the transmission risk.
Legionella Testing
Regular testing for Legionella bacteria is an important preventive measure, especially in high-risk environments. Water samples from various points in the water system can be analyzed for the presence of Legionella. Testing can identify areas of concern, allowing for targeted interventions and the implementation of control measures to prevent outbreaks.
Air Quality Control
Improving air quality is an additional preventive measure that can reduce the transmission of Legionella bacteria. Proper ventilation, air filtration, and humidification systems can help minimize the dissemination of contaminated water droplets carrying Legionella bacteria. Adequate airflow and filtration are particularly important in healthcare facilities, hotels, and other public spaces where individuals may be at a higher risk of exposure.

Treatment and Prognosis
Medical Interventions
Early diagnosis and timely treatment are vital for improving outcomes in Legionnaires’ Disease. Antibiotics, such as fluoroquinolones or macrolides, are commonly prescribed to fight the Legionella infection. The specific antibiotic regimen may vary based on the severity of the illness and individual patient factors. In severe cases, hospitalization may be required, and supportive care, such as oxygen therapy, may be provided.
Prognosis and Recovery
The prognosis for individuals with Legionnaires’ Disease can vary depending on various factors, including the individual’s age, overall health, and the presence of underlying medical conditions. With prompt diagnosis and appropriate treatment, most individuals recover fully. However, severe cases can lead to complications, such as respiratory failure or septic shock, which may increase the risk of mortality. Long-term effects, such as persistent cough or fatigue, can also occur in some cases.
Outbreaks and Public Health Response
Famous Outbreaks
Legionnaires’ Disease has been associated with various well-known outbreaks over the years. Apart from the initial outbreak in Philadelphia in 1976, other notable outbreaks include the outbreak in Murcia, Spain, in 2001 during a regional festival, and the outbreak at the Playboy Mansion in 2011. These outbreaks have highlighted the importance of public health response and the need for effective prevention and control measures.
Role of Public Health Authorities
Public health authorities and organizations play a critical role in preventing and responding to Legionnaires’ Disease outbreaks. Their responsibilities include surveillance, investigating outbreaks, communicating with the public, and promoting preventive measures. Public health authorities work closely with healthcare providers, water management professionals, and other stakeholders to develop guidelines, regulations, and educational materials to prevent and control Legionnaires’ Disease.
Legal Implications
Legionnaires’ Disease outbreaks can have legal implications, especially when they result from negligence or non-compliance with regulations. In some cases, affected individuals or their families have pursued legal action against responsible parties for financial compensation. Understandably, legal cases involving Legionnaires’ Disease outbreaks are complex, requiring thorough investigation and expertise to determine liability and reach a fair resolution.

Impact on Specific Populations
Elderly and Immunocompromised Individuals
Elderly individuals and those with compromised immune systems are at a higher risk of developing severe forms of Legionnaires’ Disease. Their weakened immune response can lead to more severe pneumonia and increase the likelihood of complications. As such, extra precautions should be taken to protect these vulnerable populations, including regular water system maintenance, improved air quality control, and heightened surveillance in healthcare facilities.
Travelers and Tourists
Legionnaires’ Disease can affect travelers and tourists who are exposed to contaminated water sources, such as hotels, resorts, and cruise ships. Individuals may become exposed during showers, while using hot tubs, or through the inhalation of aerosolized water droplets. Travelers are advised to be cautious and seek accommodations with proper water management practices and maintenance. Raising awareness among travelers about the risks and preventive measures can help reduce the incidence of Legionnaires’ Disease in this population.
Global Impact and Research
Prevalence Worldwide
Legionnaires’ Disease is a global health concern, with outbreaks reported in various countries around the world. Exact prevalence rates are challenging to determine due to underdiagnosis and underreporting. However, it is estimated that tens of thousands of cases occur annually. Improved surveillance systems and increased awareness are crucial for accurately determining the disease burden and implementing effective preventive measures worldwide.
Ongoing Research Efforts
The scientific community continues to conduct research to enhance our understanding of Legionnaires’ Disease. Ongoing studies aim to uncover insights into the transmission dynamics, optimal treatment strategies, and preventive measures. Researchers are exploring innovative approaches, such as the development of vaccines and improved diagnostic tools, to combat this disease. Continued collaboration and investment in research are essential to further our knowledge and improve the prevention and management of Legionnaires’ Disease.

Comparison with COVID-19
Differences and Similarities
While both Legionnaires’ Disease and COVID-19 are respiratory illnesses, there are notable differences between the two. COVID-19 is caused by the SARS-CoV-2 virus, whereas Legionnaires’ Disease is caused by Legionella bacteria. COVID-19 has demonstrated significantly higher transmissibility, leading to a global pandemic. Both diseases can present with fever and respiratory symptoms, but COVID-19 may also cause loss of taste and smell, which are not common in Legionnaires’ Disease.
Impact on Legionnaires’ Disease Cases
The COVID-19 pandemic has had an indirect impact on Legionnaires’ Disease cases. The strain on healthcare systems, diversion of resources, and changes in care-seeking behavior during the pandemic may have affected the diagnosis and reporting of Legionnaires’ Disease cases. Additionally, preventive measures implemented to combat COVID-19, such as increased hand hygiene and changes in building occupancy, may have influenced the occurrence and transmission of Legionella bacteria. Monitoring and addressing these impacts are crucial to maintain effective preventive strategies for Legionnaires’ Disease.
Future Outlook and Awareness
Education and Awareness Programs
Raising awareness about Legionnaires’ Disease is essential to promote prevention, early diagnosis, and timely treatment. Education programs targeting healthcare professionals, water management professionals, building owners, and the general public can help disseminate knowledge about Legionnaires’ Disease, its risk factors, and preventive measures. These programs can also facilitate the sharing of best practices and help maintain a proactive approach to public health.
Improved Safety Measures
Continued advancements in water management and treatment technologies can contribute to preventing Legionnaires’ Disease outbreaks. Developing more efficient and sustainable methods of disinfecting water systems, promoting the use of antimicrobial materials, and incorporating Legionella control measures into building design are areas of focus. Collaborative efforts between experts, policymakers, and industry stakeholders are vital to further enhance safety measures and reduce the risk of Legionnaires’ Disease.