Leukemia can be a daunting diagnosis, but there is hope. When it comes to treating this blood cancer, there are several options available, including chemotherapy, radiation, and stem cell transplant. Each of these methods has its own benefits and considerations, and understanding them can help you navigate the path towards recovery and a better quality of life. In this article, we will explore these treatment options, providing you with the information you need to make informed decisions about your health. So, let’s dive in and discover the possibilities that lie ahead on your journey to overcoming leukemia.

Chemotherapy
Introduction to Chemotherapy
Chemotherapy is a common treatment option for leukemia, a type of cancer that affects the blood and bone marrow. It is a systemic treatment, which means that it targets cancer cells throughout the body. Chemotherapy drugs work by interfering with the growth and division of cancer cells, preventing them from multiplying and spreading. This treatment can be administered in various ways, including oral pills, intravenous injections, or infusions.
Types of Chemotherapy Drugs
There are different types of chemotherapy drugs that can be used to treat leukemia. These drugs can be classified into several categories based on their mechanisms of action and the stage of cancer they target. Some commonly used chemotherapy drugs for leukemia include anthracyclines, alkylating agents, antimetabolites, corticosteroids, and topoisomerase inhibitors. The choice of drugs will depend on the type and stage of leukemia, as well as the individual patient’s needs and treatment goals.
Administration of Chemotherapy
Chemotherapy can be administered in different ways, depending on the specific drug and the patient’s condition. It can be given orally, through pills or liquids that are swallowed. Intravenous chemotherapy involves injecting the drugs directly into a vein, either through a catheter or a needle. In some cases, chemotherapy may be administered directly into the spinal fluid through a lumbar puncture or intrathecal injection. The frequency and duration of chemotherapy treatments will vary depending on the individual treatment plan.
Side Effects of Chemotherapy
Chemotherapy drugs can have various side effects due to their impact on normal cells in addition to cancer cells. Common side effects of chemotherapy for leukemia include hair loss, nausea and vomiting, fatigue, decreased appetite, increased risk of infection, anemia, and increased susceptibility to bleeding. These side effects are usually temporary and can be managed with supportive care and medical interventions. It is important for patients to communicate any side effects they experience to their healthcare team so that appropriate measures can be taken to alleviate them.
Effectiveness of Chemotherapy
Chemotherapy can be an effective treatment option for leukemia, especially when used in combination with other therapies. The goal of chemotherapy is to induce remission, which means that there are no signs of leukemia cells in the blood or bone marrow. Achieving remission is a significant milestone in leukemia treatment, as it allows for consolidation therapy to further reduce the risk of relapse. While chemotherapy can be successful in treating leukemia, its effectiveness can vary depending on factors such as the type of leukemia, the stage of the disease, and individual patient characteristics.
Radiation
Introduction to Radiation Therapy
Radiation therapy is another treatment option for leukemia that involves the use of high-energy beams to target and kill cancer cells. It is a localized treatment, meaning it is focused on specific areas of the body where leukemia cells are present. Radiation therapy can be used alone or in combination with other treatments such as chemotherapy or stem cell transplant.
Types of Radiation Therapy
There are two main types of radiation therapy used in the treatment of leukemia: external beam radiation therapy and internal radiation therapy. External beam radiation therapy involves directing radiation beams from outside the body to the affected area, while internal radiation therapy (also known as brachytherapy) involves placing a radioactive source directly into the body near the leukemia cells. The choice of radiation therapy will depend on factors such as the type and stage of leukemia, as well as the patient’s overall health.
Administration of Radiation Therapy
Radiation therapy is typically delivered in multiple sessions called fractions. The total number of sessions and the duration of the treatment will depend on several factors, including the size and location of the leukemia cells being targeted. Each treatment session is painless and generally lasts only a few minutes. The radiation oncologist will carefully plan and monitor the treatment to ensure that the leukemia cells receive an adequate dose of radiation while minimizing exposure to healthy tissues.
Side Effects of Radiation Therapy
Radiation therapy can cause certain side effects, which vary depending on the area of the body being treated. Common side effects of radiation therapy for leukemia may include fatigue, skin changes, hair loss in the treated area, loss of appetite, nausea, and diarrhea. These side effects are usually temporary and can be managed with supportive care provided by the healthcare team. It is important for patients to communicate any side effects they experience so that appropriate measures can be taken to alleviate them.
Effectiveness of Radiation Therapy
Radiation therapy can be an effective treatment option for leukemia, especially when used in combination with other therapies. It is commonly used in cases where leukemia cells have infiltrated specific areas or when there is a risk of relapse. The goal of radiation therapy is to eliminate or control the leukemia cells in the targeted area. The effectiveness of radiation therapy will depend on factors such as the type and stage of leukemia, the location of the leukemia cells, and individual patient characteristics.
Stem Cell Transplant
Introduction to Stem Cell Transplant
Stem cell transplant, also known as hematopoietic stem cell transplant, is a treatment approach that involves replacing damaged or diseased stem cells with healthy ones. It is used in the treatment of leukemia to restore the bone marrow’s ability to produce normal blood cells. Stem cell transplants can be performed using a patient’s own stem cells (autologous transplant) or stem cells from a donor (allogeneic transplant).
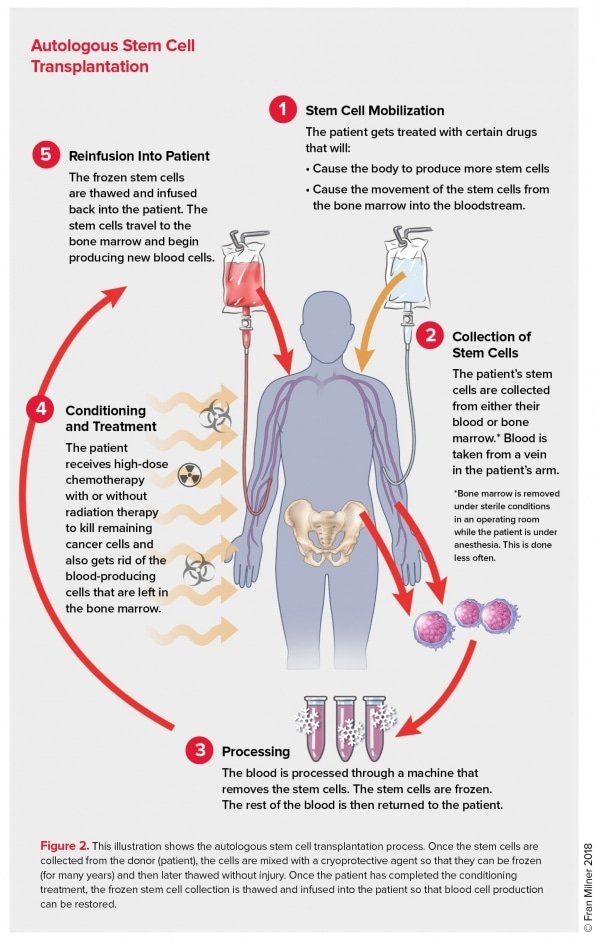
Types of Stem Cell Transplants
In autologous stem cell transplant, the patient’s own stem cells are collected before high-dose chemotherapy or radiation therapy. The stem cells are frozen and stored, and then re-infused back into the patient’s body after the intensive treatment to replenish the bone marrow. Allogeneic stem cell transplant, on the other hand, involves using stem cells from a compatible donor. The donor can be a sibling, a family member, or an unrelated matched donor identified through a bone marrow registry.
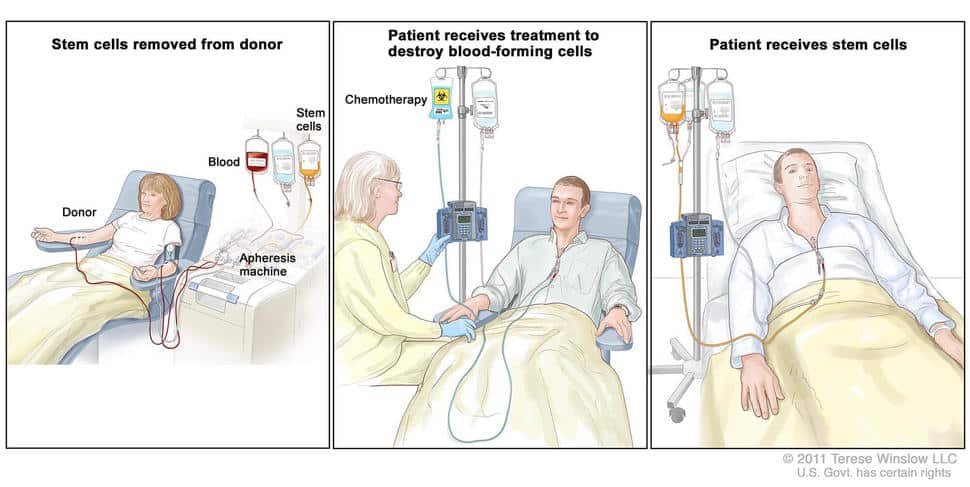
Procedure of Stem Cell Transplant
Stem cell transplant is a complex procedure that involves several steps. In autologous stem cell transplant, the patient’s stem cells are collected either through a process called apheresis or by extracting bone marrow through a surgical procedure. The collected stem cells are then frozen and stored until the patient is ready for the transplant. In allogeneic stem cell transplant, the donor’s stem cells are collected using apheresis. The stem cells are then infused into the patient’s bloodstream through a vein, similar to a blood transfusion.
Side Effects of Stem Cell Transplant
Stem cell transplant can have significant side effects due to the high-dose chemotherapy or radiation therapy that precedes it. Common side effects of stem cell transplant for leukemia include nausea, vomiting, hair loss, fatigue, increased risk of infection, anemia, bleeding, and graft-versus-host disease (GVHD) in allogeneic transplants. GVHD occurs when the donor’s immune cells attack the recipient’s tissues and can cause various complications. Close monitoring and supportive care are essential during the recovery phase to manage and minimize these side effects.
Effectiveness of Stem Cell Transplant
Stem cell transplant can be a curative treatment option for some patients with leukemia. It offers the potential for long-term remission and survival, especially in cases of high-risk or relapsed leukemia. The effectiveness of stem cell transplant will depend on factors such as the type and stage of leukemia, the availability of a suitable donor, and the patient’s overall health. Close follow-up and ongoing monitoring are essential after a stem cell transplant to assess the patient’s response and manage any potential complications.
Combined Treatment Approaches
Combining Chemotherapy and Radiation Therapy
Combining chemotherapy and radiation therapy can be an effective treatment approach for certain types and stages of leukemia. This combined treatment approach is often referred to as chemoradiation. Chemotherapy is typically administered first to shrink the leukemia cells and make them more susceptible to radiation. After chemotherapy, radiation therapy is used to target the remaining leukemia cells in specific areas of the body. This combination can increase the effectiveness of treatment and improve the chances of achieving remission.
Combining Chemotherapy and Stem Cell Transplant
The combination of chemotherapy and stem cell transplant can be a potent treatment option for leukemia. Prior to the transplant, high-dose chemotherapy is used to eliminate leukemic cells from the bone marrow. The stem cell transplant is then performed to restore the bone marrow with healthy stem cells. This combined approach allows for intensive treatment of the leukemia while replacing damaged cells with healthy ones. It improves the chances of achieving long-term remission and offers the potential for a cure in some cases.
Combining Radiation Therapy and Stem Cell Transplant
For certain types and stages of leukemia, combining radiation therapy and stem cell transplant can be an effective treatment strategy. Radiation therapy is often used to target specific areas of the body affected by leukemia cells, followed by stem cell transplant to restore the bone marrow. This combined treatment approach maximizes the impact of localized radiation therapy while ensuring the regeneration of healthy blood cells through the transplant process. It is an intensive treatment option that can increase the chances of long-term remission and survival.

Targeted Therapy
Introduction to Targeted Therapy
Targeted therapy is a relatively newer approach in the treatment of leukemia that focuses on attacking specific molecules or pathways involved in the growth and survival of cancer cells. Unlike chemotherapy, which affects both cancer cells and normal cells, targeted therapy specifically targets leukemia cells while sparing healthy tissues. This approach aims to disrupt the abnormal signaling that drives leukemia cell growth, leading to the inhibition or destruction of the cancer cells.
Types of Targeted Therapy
There are several types of targeted therapy drugs used in the treatment of leukemia. Some of the commonly used targeted therapies include tyrosine kinase inhibitors (TKIs), which block the action of specific enzymes involved in leukemia cell signaling; monoclonal antibodies, which recognize and bind to specific proteins on the surface of leukemia cells; and immune checkpoint inhibitors, which enhance the immune system’s ability to recognize and destroy cancer cells. The choice of targeted therapy will depend on the specific type of leukemia and genetic mutations present in the cancer cells.
Administration of Targeted Therapy
Targeted therapy drugs can be administered orally, in the form of pills or capsules, or intravenously through injections or infusions. The frequency and duration of targeted therapy treatment will depend on the specific drug and the patient’s response. Targeted therapy is often used as a long-term maintenance treatment after achieving remission or as a targeted therapy option for patients who may not be suitable candidates for intensive chemotherapy or radiation therapy.
Side Effects of Targeted Therapy
Targeted therapy drugs can have specific side effects depending on the drug and its mechanism of action. Common side effects of targeted therapy for leukemia may include fatigue, skin rashes, diarrhea, nausea, vomiting, and liver or kidney problems. Some targeted therapy drugs may also have cardiovascular or respiratory side effects. It is important for patients receiving targeted therapy to be closely monitored by their healthcare team and to report any side effects to ensure timely management and adjustment of treatment if necessary.
Effectiveness of Targeted Therapy
Targeted therapy has shown promising results in the treatment of certain types of leukemia, particularly those with specific genetic mutations or molecular abnormalities. It offers the potential for more precise and personalized treatment options, as targeted therapy drugs can be tailored to individual patients based on the molecular characteristics of their cancer cells. The effectiveness of targeted therapy will depend on factors such as the specific type of leukemia, the presence of targetable mutations, and the patient’s response to treatment. Ongoing research and clinical trials are continuously advancing the field of targeted therapy for leukemia treatment.
Immunotherapy
Introduction to Immunotherapy
Immunotherapy is an innovative approach in the treatment of leukemia that harnesses the power of the immune system to recognize and destroy cancer cells. It involves using drugs or other therapies that stimulate or enhance the body’s natural ability to fight cancer. Immunotherapy for leukemia aims to activate and strengthen the immune response against leukemia cells, providing a targeted and potentially long-lasting treatment option.
Types of Immunotherapy
There are several types of immunotherapy used in the treatment of leukemia. These include monoclonal antibodies, which can recognize and bind to specific proteins on the surface of leukemia cells, leading to their destruction; immune checkpoint inhibitors, which remove the brakes on the immune system, allowing it to attack cancer cells more effectively; and adoptive cell therapy, which involves modifying and reinfusing the patient’s own immune cells, such as T cells, to target and kill leukemia cells. The choice of immunotherapy will depend on the specific type of leukemia and the patient’s individual characteristics.
Administration of Immunotherapy
Immunotherapy can be administered through different routes, depending on the specific type of therapy. Some immunotherapy drugs are given intravenously through injections or infusions, while others can be administered orally as pills or capsules. Immunotherapy treatments can have varying durations and frequencies, depending on the specific drug and the patient’s response. In some cases, immunotherapy may be given in cycles, with breaks in between to allow the immune system to recover and prevent potential side effects.
Side Effects of Immunotherapy
Immunotherapy drugs can have specific side effects, known as immune-related adverse events, which occur due to the stimulation of the immune system. Common side effects of immunotherapy for leukemia may include fatigue, flu-like symptoms, skin rashes, diarrhea, fever, and liver or kidney problems. Some immunotherapy drugs can also cause immune-related inflammation in different organs, leading to specific side effects. It is important for patients receiving immunotherapy to be closely monitored by their healthcare team to detect and manage any potential side effects promptly.
Effectiveness of Immunotherapy
Immunotherapy has shown promising results in the treatment of certain types of leukemia, particularly those with specific molecular targets that can be recognized by the immune system. It offers the potential for durable responses and long-term remission, even in cases where traditional treatments may have been ineffective. However, the effectiveness of immunotherapy can vary depending on factors such as the specific type of leukemia, the immunotherapy approach used, and the patient’s individual response to treatment. Ongoing research and clinical trials are continuously expanding the possibilities of immunotherapy as a treatment option for leukemia.
Clinical Trials
Importance of Clinical Trials
Clinical trials play a crucial role in advancing the field of leukemia treatment and improving patient outcomes. These trials aim to evaluate the safety and effectiveness of new treatments, including novel drugs, combination therapies, and innovative approaches. By participating in clinical trials, patients with leukemia can potentially access cutting-edge treatments that are not yet widely available. Clinical trials also contribute to expanding scientific knowledge and guiding the development of future treatment strategies.
Types of Clinical Trials
There are different types of clinical trials conducted in the field of leukemia treatment. These include phase I trials, which evaluate the safety and dosage of a new treatment; phase II trials, which assess the effectiveness of a treatment in a larger group of patients; and phase III trials, which compare the new treatment to standard treatments to determine its efficacy. Additionally, there are also observational trials that aim to collect data on treatment outcomes and patient experiences to improve future care.
Process of Joining a Clinical Trial
Joining a clinical trial involves several steps. Patients who are interested in participating in a clinical trial should consult with their healthcare team to explore available options. The healthcare team will provide detailed information about the trial, including the potential risks and benefits. Patients will undergo a screening process to determine their eligibility for the trial, including an assessment of their medical history, current health status, and any specific inclusion or exclusion criteria defined by the trial protocol. Informed consent is a crucial component of participating in a clinical trial, and patients should have a clear understanding of the trial procedures, participation requirements, and potential implications.
Risks and Benefits of Clinical Trials
Participating in a clinical trial has both risks and potential benefits. The experimental treatment being tested may have unknown side effects or be less effective than standard treatments. However, patients in clinical trials often receive close monitoring and comprehensive care from the healthcare team, which can lead to earlier detection of any potential complications or side effects. The benefits of clinical trials can include access to cutting-edge treatments, contributing to scientific knowledge, and potentially improved outcomes for future patients. Each clinical trial has specific risks and benefits, which should be carefully considered and discussed with the healthcare team.
Supportive Care
Symptom Management Strategies
Supportive care plays a critical role in the comprehensive treatment of patients with leukemia. Symptom management strategies aim to alleviate the physical and emotional burden associated with leukemia and its treatments. These strategies can include medications to manage specific symptoms such as pain, nausea, fatigue, or sleep disturbances. Additionally, non-pharmacological interventions such as relaxation techniques, acupuncture, or massage therapy may also be used to address symptom burden and improve overall well-being.
Pain Management Techniques
Pain is a common symptom experienced by patients with leukemia, often resulting from the disease itself or as a side effect of treatments. Effective pain management techniques can significantly improve patients’ quality of life. These may include the use of pain medications, both over-the-counter and prescription strength, as well as non-pharmacological interventions such as heat or cold therapy, physical therapy, or cognitive-behavioral techniques. Personalized pain management plans are developed in collaboration with healthcare professionals to address each patient’s unique needs and preferences.
Counseling and Psychological Support
Leukemia and its treatments can have a significant emotional impact on patients and their caregivers. Counseling and psychological support services are essential components of supportive care to address the emotional and psychological well-being of patients and help them navigate the challenges associated with their diagnosis and treatment. These services may include individual counseling, support groups, psychotherapy, or other interventions to address anxiety, depression, fear, grief, or adjustment difficulties.
Diet and Nutrition Guidelines
Maintaining a healthy diet is important for patients with leukemia to support their overall health, well-being, and treatment outcomes. Diet and nutrition guidelines for patients with leukemia aim to optimize nutritional status, manage treatment-related side effects, and support the body’s healing and recovery processes. These guidelines often involve consuming a balanced diet of fruits, vegetables, whole grains, lean protein sources, and healthy fats. In some cases, specialized diets or nutritional supplements may be recommended to address specific needs or side effects.
Physical Exercise and Rehabilitation
Physical exercise and rehabilitation are increasingly recognized as important components of supportive care for patients with leukemia. Regular physical activity can help improve strength, endurance, and overall physical function, which may be compromised due to the disease or its treatments. Exercise programs tailored to individual patients’ capabilities and needs can help reduce fatigue, improve mood, enhance quality of life, and promote physical recovery. Rehabilitation interventions, such as physiotherapy or occupational therapy, may also be recommended to optimize physical function and independence.

Relapse and Refractory Leukemia
Causes and Risk Factors for Relapse
Relapse in leukemia refers to the return of cancer cells after a period of remission or successful treatment. Several factors can contribute to the risk of relapse in leukemia, including the specific type and stage of the disease, the presence of specific genetic mutations, and the effectiveness of prior treatments. Patients who have relapsed leukemia may require additional therapies or alternative treatment approaches to achieve remission again.
Treatment Options for Relapse
Treatment options for relapsed leukemia will depend on different factors, including the type and stage of leukemia, the location and extent of relapse, and the patient’s overall health. Options may include additional chemotherapy, radiation therapy, targeted therapy, immunotherapy, stem cell transplant, or participation in clinical trials. The choice of treatment will be individualized to each patient’s situation and may involve a combined treatment approach to maximize the chances of achieving remission again.
Managing Refractory Leukemia
Refractory leukemia refers to a type of leukemia that does not respond to initial treatments or fails to achieve remission. Managing refractory leukemia can be challenging, and treatment options may be limited. In some cases, alternative therapies, such as immunotherapy or targeted therapy, may be considered to target specific genetic mutations or molecular targets. Palliative care, which focuses on improving quality of life and managing symptoms, may also be an important component of care for patients with refractory leukemia.
Hospice and End-of-Life Care
In cases where leukemia becomes unresponsive to treatment or complications arise, hospice and end-of-life care provide essential support to patients and their families. Hospice care aims to provide comfort and support to patients during the final stages of life, with a focus on pain and symptom management, emotional well-being, and psychosocial support for patients and their loved ones. End-of-life care ensures that the patient’s wishes are honored and that supportive care is provided to ensure a dignified and peaceful transition.
Impact on Quality of Life
Emotional and Psychological Impact
Leukemia and its treatments can have a significant emotional and psychological impact on patients and their families. The diagnosis of leukemia can evoke feelings of fear, anxiety, sadness, or anger, and patients may experience a range of emotional challenges throughout their treatment journey. The support of healthcare professionals, counseling services, support groups, and the involvement of loved ones are crucial in addressing these emotional and psychological needs to improve overall quality of life.
Financial Burdens and Assistance Programs
Leukemia treatment can be associated with significant financial burdens, including medical expenses, medication costs, transportation, and other related expenses. These financial burdens can add stress and emotional strain to patients and their families. However, there are various financial assistance programs available to help alleviate some of these burdens. Healthcare institutions, nonprofit organizations, and government programs may provide financial aid, medication assistance, transportation support, or other resources to help patients access the necessary treatment and support services.
Coping Strategies for Patients and Caregivers
Coping with leukemia can be challenging for both patients and their caregivers. Developing effective coping strategies is crucial to enhance well-being and adapt to the changes and uncertainties that accompany the disease. Strategies such as seeking support from healthcare professionals, participating in support groups, maintaining open communication with loved ones, and engaging in relaxation techniques or hobbies can help patients and caregivers navigate the emotional, physical, and practical aspects of living with leukemia.
Support Networks and Resources
Patients and their families can benefit greatly from the support of networks and resources available to individuals living with or impacted by leukemia. Support networks can include support groups, online communities, or local organizations that offer emotional support, information, resources, and opportunities to connect with others going through similar experiences. Additionally, healthcare institutions and nonprofit organizations often provide educational materials, counseling services, access to financial assistance programs, and other resources to support patients and their families throughout their leukemia journey.