Are you looking for effective strategies and techniques to manage lymphoedema? Look no further! In this article, we will explore various approaches that can help you successfully navigate through the challenges of living with lymphoedema. From simple lifestyle adjustments to specialized therapies, we’ve got you covered. Get ready to discover practical tips and empowering techniques that will empower you to take control of your lymphoedema and live a fulfilling life.

Overview of Lymphoedema
Lymphoedema is a chronic condition characterized by the accumulation of lymph fluid in certain parts of the body, usually the arms or legs. It occurs when the lymphatic system, responsible for draining fluid, is unable to function properly. This can lead to swelling, discomfort, and a range of other symptoms.
Definition of lymphoedema
Lymphoedema is defined as the abnormal accumulation of lymph fluid in the tissues, resulting in swelling and various physical and psychological challenges. It can be categorized as primary or secondary lymphoedema. Primary lymphoedema is caused by a congenital malformation or obstruction of the lymphatic vessels, while secondary lymphoedema results from damage to the lymphatic system, often due to surgery, radiation therapy, or infection.
Causes and risk factors of lymphoedema
There are several factors that can increase the risk of developing lymphoedema. The most common cause is damage or disruption to the lymphatic system. This can occur as a result of surgery, such as lymph node removal in cancer treatment, or radiation therapy. Infections, trauma, obesity, and certain genetic conditions can also contribute to the development of lymphoedema. It’s important to note that not everyone who undergoes these treatments or experiences these risk factors will develop lymphoedema, but it’s important to be aware of the potential risks.
Diagnosis of Lymphoedema
Early diagnosis of lymphoedema is crucial to help manage the condition effectively. Recognizing the signs and symptoms, as well as undergoing diagnostic tests, is essential for a proper diagnosis.
Signs and symptoms of lymphoedema
The key signs of lymphoedema include swelling in the affected area, often accompanied by a feeling of heaviness or tightness. The affected limb may also feel achy or painful, and the skin may appear thickened or hardened. Other symptoms may include reduced flexibility, recurring infections, and difficulty fitting into clothing or wearing jewelry or accessories that were previously comfortable. It’s important to note that these symptoms can vary in severity, and not all individuals with lymphoedema will experience the same symptoms.
Diagnostic tests for lymphoedema
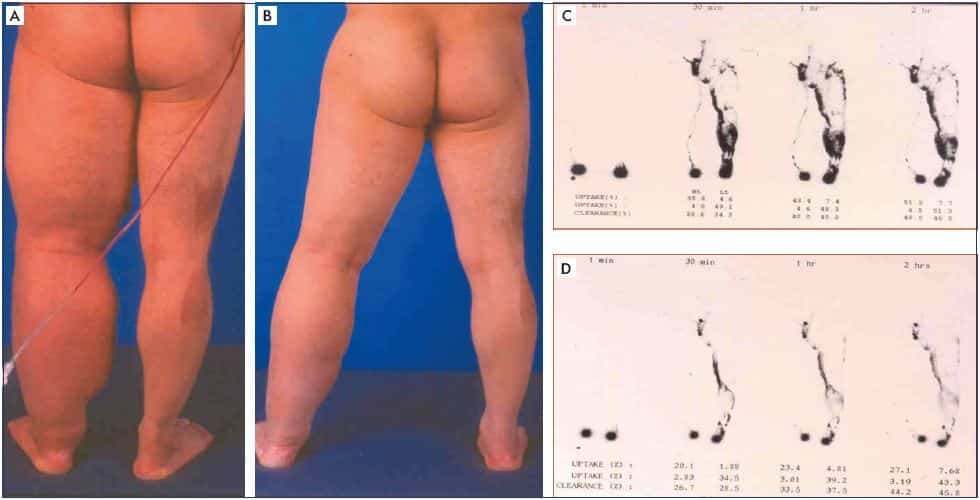
To confirm a diagnosis of lymphoedema, healthcare professionals may perform a variety of tests. These may include a physical examination, where the healthcare provider will assess the affected area for swelling and other characteristic signs. Imaging tests, such as lymphoscintigraphy or lymphangiography, can be used to visualize the lymphatic system and identify any blockages or abnormalities. Additionally, measuring the circumference or volume of the limbs can provide quantitative data to assess the extent of swelling. These diagnostic tests, combined with a thorough medical history assessment, help healthcare professionals accurately diagnose lymphoedema.

Medical Management of Lymphoedema
Medical management plays a crucial role in the treatment and control of lymphoedema. While there is no cure for lymphoedema, various medications and interventions aim to alleviate symptoms and improve quality of life.
Medications for lymphoedema
There are no medications specifically approved for treating lymphoedema. However, healthcare providers may prescribe medication to address underlying conditions, such as infections or inflammation, that can worsen lymphoedema symptoms. Antibiotics may be prescribed to treat or prevent infections, corticosteroids may be used to reduce inflammation, and diuretics may be prescribed to help manage swelling. It’s important to talk to your healthcare provider about any medication options and their potential benefits and risks.
Compression therapy for lymphoedema
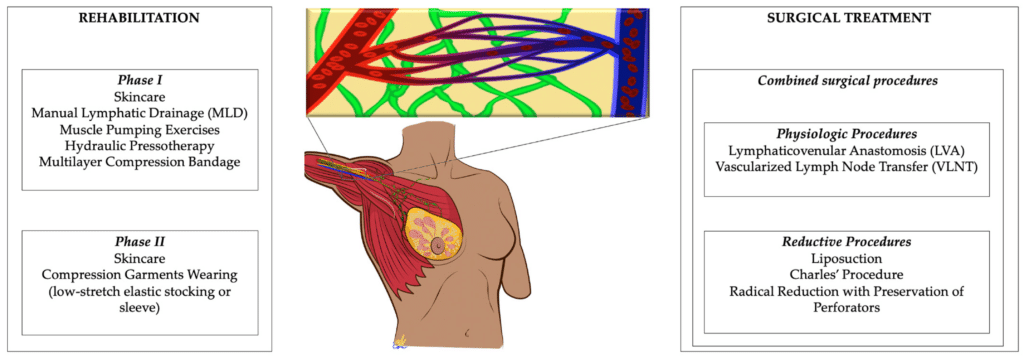
Compression therapy is a cornerstone of lymphoedema management and involves the use of specialized garments or bandages to apply controlled pressure to the affected area. Compression helps reduce swelling, improves lymphatic flow, and maintains the size and shape of the limb. Depending on the severity of lymphoedema, healthcare providers may recommend different levels of compression, ranging from light to heavy compression. It is important to wear compression garments or bandages as prescribed and to follow the healthcare provider’s instructions for proper use and care.
Physical Therapy Treatment for Lymphoedema
Physical therapy plays a vital role in managing lymphoedema, focusing on techniques to reduce swelling, improve lymphatic flow, and enhance overall physical function. A variety of physical therapy techniques are commonly used in the treatment of lymphoedema.
Manual lymphatic drainage
Manual lymphatic drainage (MLD) is a specialized massage technique designed to stimulate lymphatic flow and promote the drainage of excess fluid from the affected area. MLD involves gentle, rhythmic strokes and may be performed by a physical therapist or a certified lymphedema therapist. This technique helps reduce swelling, relieve discomfort, and improve the overall functioning of the lymphatic system. Regular MLD sessions can have a positive impact on managing lymphoedema symptoms.
Exercise for lymphoedema
Regular exercise can be beneficial for individuals with lymphoedema, as it helps improve circulation, reduce swelling, and enhance muscle strength and flexibility. Low-impact activities such as walking, swimming, or cycling are often recommended for individuals with lymphoedema. It’s important to consult with a physical therapist or healthcare provider to develop an exercise program that is safe and suitable for your specific condition. Gradually increasing the intensity and duration of exercise over time can help maximize the benefits while minimizing the risk of overexertion.
Multilayer bandaging
Multilayer bandaging is a technique used to manage lymphoedema by applying a series of specialized bandages to the affected limb. The bandages provide compression and support, helping to reduce swelling and improve fluid drainage. Multilayer bandaging is typically performed by a healthcare professional or a certified lymphedema therapist and may be used as an initial treatment or as part of a maintenance plan alongside compression garments.
Compression garments
Compression garments are specially designed garments, such as sleeves, stockings, or gloves, that apply external pressure to the affected limb. These garments support lymphatic flow, reduce swelling, and help maintain the progress achieved through other treatment techniques. Compression garments come in various sizes, compression levels, and styles, ensuring a proper fit and effective management of lymphoedema. It’s important to wear compression garments consistently and replace them as needed to ensure optimum compression and comfort.

Skin and Wound Care in Lymphoedema
Caring for the skin and preventing wounds in the affected area is crucial for individuals with lymphoedema. Proper skin and wound care help minimize the risk of infection, promote healing, and maintain overall skin health.
Importance of skin and wound care
The accumulation of lymph fluid in tissues affected by lymphoedema can lead to changes in the skin, making it more susceptible to infection, dryness, and other skin-related issues. Regular skincare routines, including keeping the skin clean, moisturized, and protected, are essential to maintain the integrity of the skin and reduce the risk of complications. Maintaining good skin health also helps minimize the risk of secondary infections and improves overall comfort and quality of life.
Preventing infections
Preventing infections is a crucial aspect of caring for lymphoedema-affected skin. Daily hygiene practices, such as gentle cleaning with mild soap and lukewarm water, can help reduce the likelihood of infection. It is important to avoid harsh soaps, excessive scrubbing, or hot water, as these can further irritate the skin. Keeping the skin well-moisturized with gentle, fragrance-free lotions or creams can also help maintain skin health and reduce the risk of cracking or dryness. Additionally, avoiding exposure to potential sources of infection, such as cuts or insect bites, and promptly seeking treatment for any signs of infection are important preventive measures.
Wound healing techniques
In the event of a wound or skin abrasion in the affected area, prompt attention and proper wound care are essential. For minor wounds, cleaning the area with mild soap and water, applying an appropriate dressing, and monitoring for signs of infection are important steps in the healing process. For more severe wounds or those that do not heal properly, seeking medical attention from a healthcare professional is crucial. They may recommend additional interventions, such as the use of specialized wound dressings, topical medications, or referral to a wound care specialist.
Dietary and Lifestyle Modifications for Lymphoedema
Dietary and lifestyle modifications can play a role in managing lymphoedema and improving overall health and well-being. While these modifications alone may not cure lymphoedema, they can assist in reducing symptoms and supporting overall treatment efforts.
Importance of a healthy diet
Maintaining a healthy diet is important for individuals with lymphoedema, as it helps manage weight, reduce inflammation, and support overall lymphatic function. A balanced diet that includes plenty of fruits, vegetables, lean proteins, whole grains, and healthy fats can assist in maintaining a healthy weight and reducing the burden on the lymphatic system. Limiting processed foods, refined sugars, and excessive salt intake may also help minimize fluid retention and inflammation.
Hydration and lymphoedema
Proper hydration is essential for lymphoedema management. Drinking an adequate amount of water helps maintain the overall health and function of the lymphatic system. It can also help reduce fluid retention and promote the elimination of toxins from the body. While individual water intake needs may vary, a general guideline is to consume at least eight cups (64 ounces) of water per day. However, it’s important to consult with a healthcare provider to determine the appropriate fluid intake for your specific condition.
Lifestyle changes to manage lymphoedema
In addition to dietary modifications, certain lifestyle changes can assist in managing lymphoedema symptoms. Maintaining a healthy body weight through regular exercise and portion control can help reduce the strain on the lymphatic system. Avoiding prolonged periods of inactivity and taking regular breaks to move and stretch can also support healthy lymphatic flow. It’s important to listen to your body and avoid activities that worsen symptoms or cause discomfort. Implementing stress management techniques, such as meditation, deep breathing exercises, or engaging in enjoyable hobbies, can also contribute to overall well-being and help minimize stress-related exacerbations of lymphoedema.
Psychological Support and Coping Strategies
Living with lymphoedema can have a significant psychological impact on individuals, affecting their self-esteem, body image, and overall quality of life. Psychological support, paired with coping strategies, can play a vital role in managing the emotional and psychological aspects of lymphoedema.
Psychological impact of lymphoedema
Lymphoedema can lead to feelings of anxiety, depression, and social isolation. The visible physical changes associated with the condition, such as swelling or skin alterations, can impact body image and self-confidence. Coping with the management of a chronic condition, including the need for ongoing treatments and lifestyle modifications, can also be emotionally challenging. Recognizing and addressing these psychological impacts is important to ensure holistic care for individuals with lymphoedema.
Counseling and support groups
Professional counseling or therapy can provide a safe and supportive space for individuals to navigate the emotional challenges of living with lymphoedema. A licensed therapist can help individuals develop healthy coping strategies, work through body image concerns, and address any underlying issues contributing to emotional distress. Additionally, participating in support groups or connecting with others who have similar experiences can provide a sense of community, understanding, and empowerment. It’s important to research local resources or speak with healthcare providers about available counseling services and support groups in your area.
Stress management techniques
Managing stress is crucial for overall well-being and can contribute to minimizing lymphoedema symptoms. Practicing stress management techniques, such as deep breathing exercises, meditation, mindfulness, or engaging in activities that promote relaxation, can help individuals better cope with the emotional and physical challenges of lymphoedema. It’s important to find techniques that work best for you and incorporate them into your daily routine. Regular self-care and prioritizing activities that bring joy and fulfillment can also support emotional resilience and overall psychological well-being.
Surgical Options for Lymphoedema
In cases where conservative treatment approaches have not provided sufficient relief, surgical interventions may be considered. While surgical options are not suitable for everyone with lymphoedema, they can offer significant improvements in managing the condition.
Lymphaticovenous anastomosis
Lymphaticovenous anastomosis (LVA) is a surgical procedure that aims to bypass blocked or damaged lymphatic vessels by connecting them to nearby veins. This allows lymph fluid to flow more freely and reduces swelling in the affected area. LVA is typically performed by a specialized surgeon and may be an option for individuals with primary or early-stage secondary lymphoedema. It’s important to note that LVA is not suitable for all cases of lymphoedema, and eligibility for the procedure should be determined through consultation with a healthcare provider.
Vascularized lymph node transfer
Vascularized lymph node transfer (VLNT) involves the transplantation of healthy lymph nodes from one area of the body to the affected area. This surgical procedure aims to improve lymphatic drainage and reduce swelling. VLNT is typically recommended for individuals with more advanced lymphoedema or those who have not seen adequate improvement with other treatment methods. It requires a highly skilled surgical team and may involve a prolonged recovery period. As with LVA, eligibility for VLNT should be determined through consultation with a healthcare provider.
Self-Care Techniques for Lymphoedema
Self-care techniques are an important part of managing and maintaining lymphoedema treatment progress. These techniques empower individuals to take an active role in their care and promote overall well-being.
Self-massage techniques
Self-massage can be a beneficial technique in managing lymphoedema. It involves gently stimulating the affected area with specific hand movements to promote lymphatic flow and reduce swelling. Self-massage techniques should be learned from a certified lymphedema therapist or physical therapist to ensure they are performed correctly and safely. Self-massage can be done daily or as recommended by healthcare providers, and it can be a comforting and effective way to manage symptoms between professional sessions.
Self-bandaging techniques
Self-bandaging is another self-care technique individuals can learn to manage lymphoedema. It involves applying layers of specialized bandages to the affected limb to provide compression and support. Proper self-bandaging techniques should be taught by a healthcare professional or certified lymphedema therapist to ensure they are performed correctly and safely. Self-bandaging techniques may be recommended as a temporary measure to manage acute swelling or as part of a maintenance plan alongside compression garments. It’s important to follow healthcare provider’s instructions and monitor for any changes in symptoms while self-bandaging.
Skin hygiene practices
Maintaining good skin hygiene is crucial for individuals with lymphoedema. This includes keeping the skin clean, moisturized, and protected to minimize the risk of infections and other skin-related complications. Gentle cleansing with mild soap and lukewarm water, followed by thorough drying and applying an appropriate fragrance-free moisturizer, is important for maintaining the integrity of the skin. Avoiding harsh soaps, excessive scrubbing, or hot water is essential to prevent irritation and damage to the skin. It’s also important to protect the skin from cuts, scratches, insect bites, and other potential sources of infection. Monitoring the skin for any changes, such as redness, warmth, or swelling, and seeking prompt medical attention if any signs of infection arise, are key components of skin hygiene practices.
Preventing Complications of Lymphoedema
Preventing and managing complications is a crucial aspect of care for individuals with lymphoedema. Being aware of potential risks and taking appropriate precautions can help minimize complications and optimize overall management.
Recognizing and managing infections
Infections are a common concern for individuals with lymphoedema, as the accumulation of fluid increases the risk of bacterial or fungal growth. It’s important to be vigilant for any signs of infection, such as increased redness, warmth, or pain in the affected area, as well as fever or flu-like symptoms. Promptly seeking medical attention and initiating appropriate treatment, such as antibiotics or antifungal medications, is crucial to prevent the infection from worsening. Additionally, practicing good skin hygiene, avoiding potential sources of infection, and adhering to recommended skincare and wound care practices can help minimize the risk of infections and their associated complications.
Avoiding injury and trauma
Individuals with lymphoedema should take precautions to avoid injury and trauma to the affected area. Due to impaired lymphatic flow, even minor injuries can lead to complications such as infections, delayed wound healing, or exacerbation of swelling. It’s important to be mindful of activities that may increase the risk of injury, such as contact sports or excessive strain on the limbs. Taking precautions, such as wearing protective clothing or using padding, when engaging in activities that pose a potential risk can help minimize the likelihood of injury. Additionally, avoiding overexertion, maintaining proper body mechanics, and seeking medical attention for any injuries or trauma to the affected area are important steps in preventing complications.
Preventing cellulitis
Cellulitis is a potentially serious bacterial skin infection that can occur in individuals with lymphoedema. To reduce the risk of developing cellulitis, it’s important to maintain proper skin hygiene, avoid injury or trauma to the affected area, and follow recommended skincare practices. Regularly moisturizing and protecting the skin, keeping it clean and dry, and avoiding harsh chemicals or irritants can help minimize the risk of bacterial entry and infection. It’s also important to seek medical attention promptly if any signs or symptoms of cellulitis, such as redness, swelling, warmth, or fever, are observed. Early diagnosis and treatment are essential to prevent the infection from spreading and causing further complications.