Imagine a global community united in the fight against a common enemy: Middle East Respiratory Syndrome Coronavirus (MERS-CoV). As the world grapples with this ongoing outbreak, effective management becomes crucial to ensure the safety and well-being of individuals and communities. With its origins in the Middle East, this highly contagious virus demands swift action and collaboration across borders. This article sheds light on the strategies and measures that can be undertaken to tackle the MERS-CoV outbreak head-on, offering insights into prevention, containment, and treatment that can make a significant difference in curbing its spread and safeguarding lives.
Understanding Middle East Respiratory Syndrome Coronavirus (MERS-CoV)
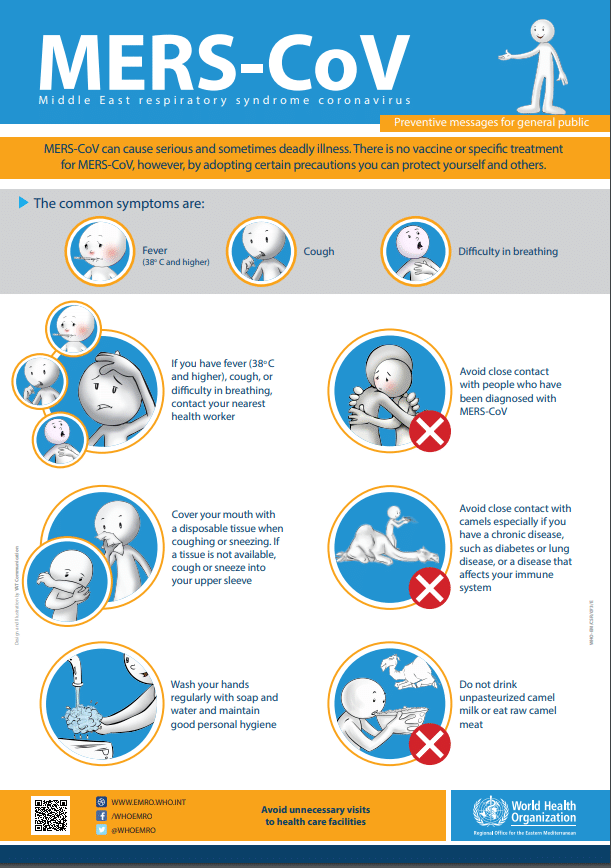
Middle East Respiratory Syndrome Coronavirus (MERS-CoV) is a viral illness that was first identified in Saudi Arabia in 2012. It belongs to the same family as the severe acute respiratory syndrome coronavirus (SARS-CoV) and the novel coronavirus (SARS-CoV-2) that causes COVID-19. MERS-CoV is primarily transmitted from animals to humans, but it can also spread between individuals. Understanding the characteristics, transmission, symptoms, diagnosis, and treatment of MERS-CoV is essential for effective control and prevention strategies.
Overview of MERS-CoV
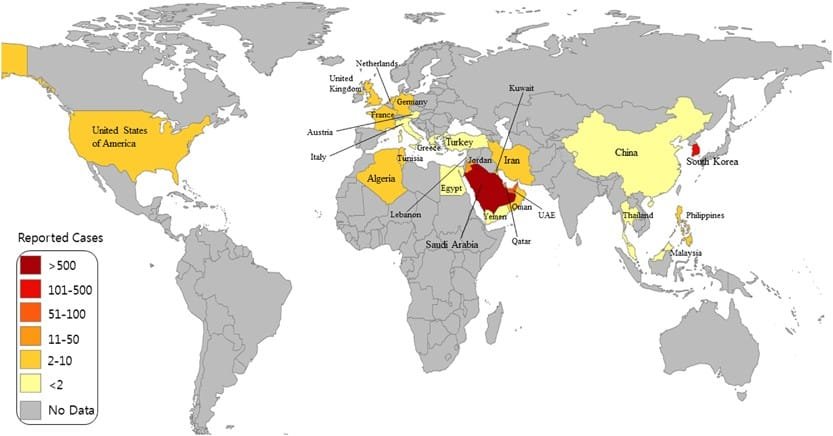
MERS-CoV is caused by a novel coronavirus that primarily circulates in dromedary camels. Humans can contract the virus through close contact with infected animals, mainly through exposure to respiratory droplets. The virus can also spread through human-to-human transmission, usually in close settings such as healthcare facilities. While the majority of MERS-CoV cases have been reported in the Middle East, sporadic cases have been identified in other parts of the world through travel-associated and secondary transmission.
Transmission of MERS-CoV
The primary mode of MERS-CoV transmission is through direct or indirect contact with infected camels or their bodily fluids. Although the exact mechanism of transmission is still not fully understood, it is believed that the virus may have originated from bats and subsequently transmitted to camels. Human-to-human transmission occurs through close contact, such as caring for an infected individual or through respiratory droplets produced when an infected person coughs or sneezes. The virus does not appear to have sustained human-to-human transmission like COVID-19.
Symptoms of MERS-CoV
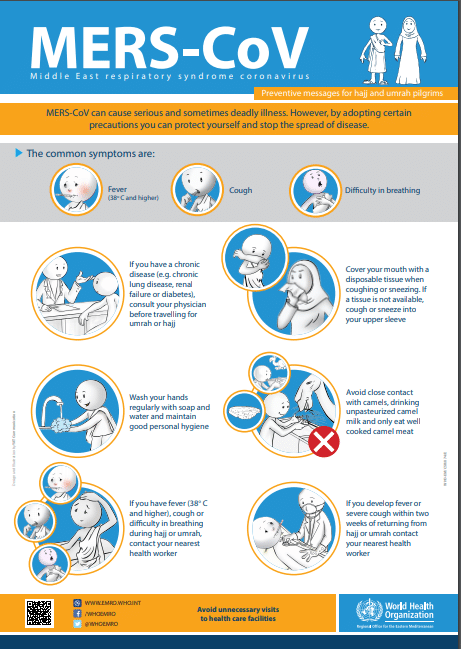
The symptoms of MERS-CoV infection can vary from mild to severe, including fever, cough, shortness of breath, and pneumonia. Some individuals may also experience gastrointestinal symptoms such as diarrhea. In severe cases, MERS-CoV can lead to respiratory failure, kidney failure, and even death. It is important to note that some individuals may be asymptomatic carriers, meaning they show no symptoms but can still transmit the virus to others.
Diagnosis and Treatment of MERS-CoV
Diagnosing MERS-CoV infection involves laboratory testing of respiratory samples, such as a nasopharyngeal swab or sputum. Testing typically involves reverse transcription polymerase chain reaction (RT-PCR) to detect the presence of viral genetic material. Serology tests are also available to detect antibodies specific to MERS-CoV. There is currently no specific antiviral treatment for MERS-CoV, and supportive care is primarily provided to manage symptoms. Severely ill patients may require hospitalization, including the use of ventilators to support breathing.
Preventing the Spread of MERS-CoV
Preventing the spread of MERS-CoV requires a multisectoral approach involving public health measures, community education, improvement of healthcare facilities, and travel restrictions. By implementing comprehensive prevention strategies, the risk of transmission can be significantly reduced.
Public Health Measures
Public health measures play a crucial role in preventing and controlling the spread of MERS-CoV. These measures include early detection and reporting of cases, contact tracing, isolation and quarantine of infected individuals, and implementing infection prevention and control measures in healthcare settings.
Educating the Community
Raising awareness and educating the community about MERS-CoV is essential in promoting preventive behaviors and reducing the risk of transmission. Public health authorities should disseminate accurate and timely information about the virus, its symptoms, and preventive measures through various channels, including media campaigns, educational materials, and community engagement activities.
Enhancing Healthcare Facilities
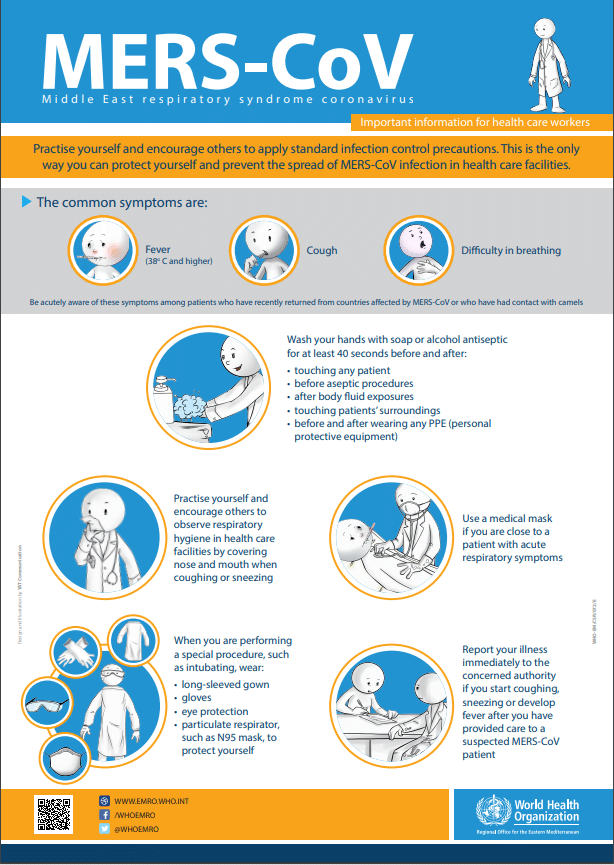
Improving the infrastructure and practices in healthcare facilities is essential for preventing and managing MERS-CoV outbreaks. This involves establishing infection prevention and control measures, ensuring proper ventilation systems, promoting hand hygiene practices, and providing adequate personal protective equipment (PPE) for healthcare workers.
Travel Restrictions and Screening
Implementing travel restrictions and screening measures can play a crucial role in preventing the importation of MERS-CoV cases from affected areas. Travel advisories and guidelines should be provided to individuals and healthcare professionals, highlighting the importance of self-monitoring for symptoms and seeking medical attention if needed.
Preparing Healthcare Systems for MERS-CoV Outbreak
Preparing healthcare systems for MERS-CoV outbreaks involves implementing surveillance systems, training healthcare personnel, ensuring adequate diagnostic capability, and establishing isolation units. These measures are crucial in detecting and responding to MERS-CoV cases effectively.
Implementing Surveillance Systems
Surveillance systems enable the early detection and monitoring of MERS-CoV cases. Healthcare facilities and public health authorities should work together to establish robust surveillance mechanisms to identify and report suspected cases promptly. Surveillance data can also provide valuable insights into the epidemiology and transmission patterns of MERS-CoV.
Training Healthcare Personnel
Proper training of healthcare personnel is essential in effectively managing MERS-CoV outbreaks. Healthcare workers should receive education on infection prevention and control measures, case management protocols, proper use of personal protective equipment, and risk communication strategies. Regular training sessions and simulation exercises can help improve preparedness and response capabilities.
Ensuring Adequate Diagnostic Capability
Rapid and accurate diagnosis is crucial for timely management and control of MERS-CoV outbreaks. Healthcare facilities should have access to reliable diagnostic tools, including laboratory testing capacity and trained personnel. Regular quality assurance programs should be implemented to maintain the accuracy and reliability of diagnostic tests.
Establishing Isolation Units
Isolation units are essential for effectively managing and containing MERS-CoV cases. Healthcare facilities should have designated isolation areas with adequate staff, equipment, and supplies to provide appropriate care to infected individuals while minimizing the risk of transmission to healthcare workers and other patients. Isolation procedures should adhere to strict infection prevention and control guidelines.
Managing MERS-CoV Outbreak in Hospitals
Managing MERS-CoV outbreaks in hospitals requires a coordinated and systematic approach. This involves identifying and reporting cases, implementing isolation and quarantine procedures, conducting contact tracing, and strengthening infection prevention and control measures.
Identification and Reporting of Cases
Rapid identification and reporting of suspected MERS-CoV cases are crucial in controlling outbreaks. Healthcare workers should be trained to recognize the symptoms and risk factors of MERS-CoV and follow proper reporting protocols. Early identification allows for prompt isolation and initiation of infection control measures.
Isolation and Quarantine Procedures
Isolation and quarantine procedures are essential for preventing the spread of MERS-CoV in healthcare settings. Infected individuals should be isolated in designated isolation units, whereas individuals who have had close contact with confirmed cases should undergo quarantine. Proper adherence to infection prevention and control measures, such as wearing PPE and practicing hand hygiene, should be ensured.
Contact Tracing
Contact tracing plays a vital role in identifying individuals who may have been exposed to MERS-CoV and preventing further transmission. Public health authorities should establish comprehensive contact tracing protocols to identify and monitor individuals who have had close contact with confirmed cases. These individuals should be monitored for symptoms and offered testing if necessary.
Infection Prevention and Control Measures
Stringent infection prevention and control measures should be implemented in healthcare facilities to minimize the risk of MERS-CoV transmission. This includes practicing proper hand hygiene, using appropriate PPE, implementing respiratory hygiene and cough etiquette, ensuring proper disinfection and sterilization protocols, and maintaining a clean and safe environment. Regular training and audits should be conducted to ensure compliance with these measures.
Communication Strategies During MERS-CoV Outbreak
Effective communication is crucial during MERS-CoV outbreaks to address public concerns, disseminate accurate information, and coordinate efforts with health authorities. Different communication strategies should be employed to reach various stakeholders.
Risk Communication to the Public
Risk communication to the public involves providing clear and timely information about MERS-CoV, its transmission, symptoms, preventive measures, and updates on the outbreak. Public health authorities should use various channels, such as social media, websites, press releases, and public service announcements, to ensure accurate information reaches the general population. Communication should be transparent, empathetic, and tailored to the needs of different communities.
Internal Communication within Healthcare Facilities
Internal communication within healthcare facilities is essential for effective coordination and implementation of outbreak response measures. Regular communication channels, such as staff meetings, bulletins, and email updates, should be established to disseminate information about MERS-CoV, infection prevention and control guidelines, and updates on the outbreak situation. Feedback mechanisms should also be in place to address staff concerns and suggestions.
Media Engagement and Crisis Communication
Engaging with the media is important to ensure accurate and responsible reporting during MERS-CoV outbreaks. Public health authorities should establish strong relationships with media outlets and provide regular updates and briefings to journalists. Crisis communication strategies should be developed in advance to effectively manage rumors, address public concerns, and provide timely and accurate information during critical periods of the outbreak.
Coordinating Efforts with Health Authorities
Coordinating efforts with health authorities is crucial for ensuring a cohesive and effective response to MERS-CoV outbreaks. Regular communication channels should be established between healthcare facilities, public health authorities, and other relevant stakeholders to share information, coordinate response activities, and align strategies. Collaboration and information sharing can help strengthen the overall response and improve outbreak control.
Addressing Psychological Impact of MERS-CoV Outbreak
MERS-CoV outbreaks can have a significant psychological impact on individuals and communities. Addressing the psychological well-being of affected individuals is important for their overall recovery and resilience.
Providing Mental Health Support
Provision of mental health support services is essential for individuals affected by MERS-CoV outbreaks. This includes psychological counseling, stress management techniques, and access to mental health professionals. Special attention should be given to healthcare workers and individuals who have been quarantined or isolated.
Educating Public on Coping Strategies
Educating the public on coping strategies can help reduce stress and anxiety during MERS-CoV outbreaks. Information on stress management techniques, healthy coping mechanisms, and self-care practices should be provided through various channels, including social media, websites, and community engagement activities.
Reducing Stigma and Discrimination
Promoting understanding and reducing stigma and discrimination associated with MERS-CoV is crucial for fostering social cohesion and supporting affected individuals. Public health authorities should provide accurate information about MERS-CoV transmission and debunk myths and misconceptions that contribute to stigmatization. Community engagement activities can also help promote inclusivity and reduce discrimination.
Community Engagement for Psychological Well-being
Engaging the community in MERS-CoV response efforts can promote a sense of togetherness and resilience. Community leaders, religious institutions, and grassroots organizations should be involved in raising awareness, addressing concerns, and promoting psychological well-being. Encouraging community support networks and social connections can help individuals cope with the psychological impacts of the outbreak.
Research and Development for MERS-CoV
Continued research and development efforts are necessary for improving our understanding of MERS-CoV and developing effective preventive and therapeutic interventions.
Advancing Vaccine Development
Ongoing research is focused on developing a safe and effective vaccine against MERS-CoV. Vaccines are crucial for preventing future outbreaks and reducing the impact of the virus. Collaborative efforts between researchers, regulatory authorities, and vaccine manufacturers are essential for accelerating vaccine development and ensuring its accessibility to populations at risk.
Enhancing Diagnostic Tools
Improving diagnostic tools for MERS-CoV is important for early detection and timely management of cases. Research is ongoing to develop rapid and accurate diagnostic tests that can be easily deployed in healthcare settings. These tools will aid in rapid identification, contact tracing, and implementation of appropriate infection prevention and control measures.
Understanding MERS-CoV Epidemiology
Further research on the epidemiology of MERS-CoV is necessary to better understand its transmission dynamics, risk factors, and geographical variations. Studying the evolutionary patterns and animal reservoirs can shed light on the origins and potential future outbreaks of the virus. This knowledge will facilitate targeted control strategies and surveillance efforts.
Exploring Potential Treatment Options
Research into potential treatment options for MERS-CoV is essential for improving patient outcomes and reducing case fatality rates. Antiviral therapies, immunotherapies, and other novel treatment modalities are being investigated in preclinical and clinical trials. Collaboration between researchers, pharmaceutical companies, and regulatory agencies is vital for advancing these treatment options.
Lessons Learned from Previous MERS-CoV Outbreaks
Drawing lessons from previous MERS-CoV outbreaks is crucial for improving preparedness and response capabilities. Analyzing past outbreaks and patterns can guide the development of robust response plans and the implementation of best practices.
Analyzing Past Outbreaks and Patterns
Analyzing past MERS-CoV outbreaks helps identify common patterns, risk factors, and gaps in the response. This retrospective analysis can provide valuable insights into the effectiveness of preventive measures, surveillance systems, and control strategies. Lessons learned from previous outbreaks can inform future response efforts.
Improving Response Plan and Preparedness
The knowledge gained from previous MERS-CoV outbreaks should be used to enhance response plans and preparedness measures. These plans should incorporate the latest scientific evidence, best practices, and recommendations from national and international health authorities. Regular review, updating, and testing of response plans are essential to ensure their effectiveness.
Implementing Lessons into Current Practices
Lessons learned from previous MERS-CoV outbreaks should be translated into practical actions and integrated into current practices. This may involve revising infection prevention and control guidelines, strengthening surveillance systems, conducting simulation exercises, and addressing training gaps. Continuous feedback and learning loops should be established to ensure ongoing improvement.
Collaboration and Information Sharing
Collaboration and information sharing among countries and international organizations are essential for learning from previous outbreaks and addressing the global threat of MERS-CoV. Sharing experiences, best practices, and research findings help build a collective knowledge base and improve global preparedness and response capacity.
Global Cooperation in Managing MERS-CoV Outbreaks
Managing MERS-CoV outbreaks requires global cooperation and collaboration among countries and international organizations. By sharing information, supporting affected countries, conducting collaborative research, and building partnerships, the global community can effectively respond to the threat of MERS-CoV.
Sharing Information and Best Practices
Sharing information and best practices between countries experiencing MERS-CoV outbreaks and those without current cases is crucial for promoting preparedness and response. Regular communication and collaboration between public health authorities, researchers, and policymakers facilitate the exchange of knowledge and expertise. This shared information can help countries anticipate and mitigate the impact of MERS-CoV outbreaks.
Supporting Affected Countries
Countries affected by MERS-CoV outbreaks require support from the international community to strengthen their response capabilities. This support may include financial assistance, technical expertise, and capacity building initiatives. Collaborative efforts can help affected countries improve their healthcare infrastructure, surveillance systems, and infection prevention and control measures.
Collaborative Research Efforts
Collaborative research efforts are essential for advancing our understanding of MERS-CoV and developing effective strategies for prevention, diagnosis, and treatment. International research collaborations can facilitate data sharing, joint studies, and clinical trials. These collaborations accelerate research progress and promote the development of innovative interventions.
Building Partnerships for Preparedness
Building partnerships for preparedness involves fostering collaborations among governments, researchers, healthcare providers, and international organizations. These partnerships can support the development and implementation of comprehensive MERS-CoV preparedness plans, joint training programs, and resource sharing. By pooling expertise and resources, countries can enhance their overall preparedness for MERS-CoV outbreaks.
Future Outlook: Mitigating the Threat of MERS-CoV
Mitigating the threat of MERS-CoV requires sustained efforts in improving surveillance systems, strengthening healthcare infrastructure, investing in research and development, and raising awareness and preparedness. By addressing these areas, the global community can minimize the impact of MERS-CoV and better respond to future outbreaks.
Improving Surveillance and Early Warning Systems
Continuous improvement of surveillance systems and early warning systems is crucial for detecting and responding to MERS-CoV outbreaks at an early stage. Investments should be made in strengthening disease surveillance networks, improving laboratory capacity, and ensuring timely reporting of cases. Advanced data analytics and modeling can aid in predicting outbreaks and guiding response efforts.
Strengthening Healthcare Infrastructure
Investments in healthcare infrastructure are necessary to enhance the capacity and resilience of healthcare systems in managing MERS-CoV outbreaks. This includes improving hospital facilities, increasing the number of isolation units, expanding diagnostic capabilities, and ensuring an adequate supply of essential medical equipment and drugs. A robust healthcare infrastructure is vital for effective patient care and outbreak control.
Investing in Research and Development
Continued investment in research and development is crucial for advancing our understanding of MERS-CoV and developing innovative interventions. Funding should be allocated to vaccine development, improving diagnostic tools, studying MERS-CoV epidemiology, and exploring potential treatment options. Well-funded research programs can accelerate progress towards effective prevention and control strategies.
Raising Awareness and Preparedness
Raising awareness and preparedness among healthcare professionals, policymakers, and the general public is essential for reducing the impact of MERS-CoV outbreaks. Educational campaigns, training programs, and simulation exercises should be conducted regularly to ensure a high level of preparedness and adherence to preventive measures. A well-informed and prepared community can effectively contribute to outbreak control efforts.
In conclusion, understanding MERS-CoV and implementing comprehensive control and prevention strategies is crucial for mitigating the threat posed by the virus. By improving surveillance systems, strengthening healthcare infrastructure, investing in research and development, and promoting global cooperation, the global community can effectively respond to MERS-CoV outbreaks and protect public health. Continuous learning from previous outbreaks and sharing of information and best practices will further enhance preparedness and response capabilities. With concerted efforts, we can minimize the impact of MERS-CoV and ensure a safer future for all.