Pregnancy is a beautiful and transformative journey, but it can also bring about various challenges for expectant mothers. One such challenge is anemia, specifically iron deficiency. Anemia during pregnancy can have detrimental effects on both the mother and the developing baby, making it crucial to address this issue promptly. In this article, we will explore the effects of anemia in pregnancy and discuss effective solutions to combat this condition, ensuring a healthy and thriving journey for both mother and child.
Anemia in Pregnancy: Effects and Solutions
Understanding Anemia
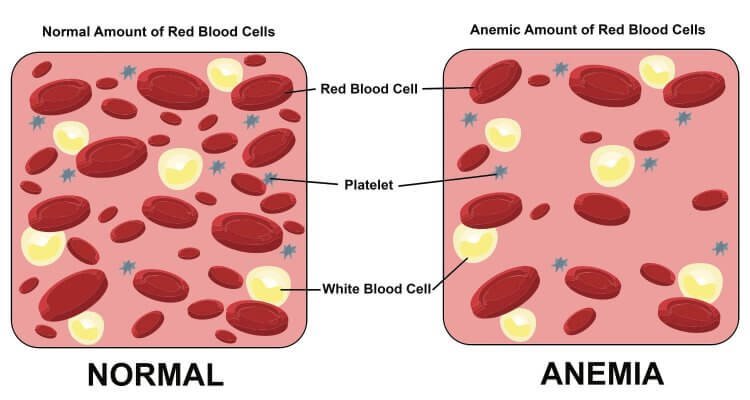
Anemia is a condition characterized by a deficiency of healthy red blood cells or hemoglobin, which are responsible for carrying oxygen to the body’s tissues. During pregnancy, the body requires an increased blood volume to support the growing fetus, making pregnant women more susceptible to anemia.
Prevalence of Anemia in Pregnancy
Anemia is a common condition among pregnant women worldwide. According to global statistics, approximately 38% of pregnant women suffer from anemia. However, the prevalence of anemia varies across regions. Developing countries have higher rates of anemia in pregnancy, reaching up to 57%, while developed countries tend to have lower rates, around 18%.
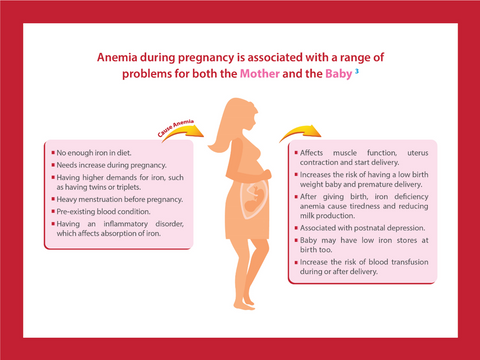
Effects of Anemia on Pregnancy
Anemia in pregnancy can have several negative effects on both the mother and the fetus. Understanding these effects is crucial for ensuring optimal maternal and fetal health.
Complications for the Mother
Women with anemia during pregnancy are more likely to experience fatigue and weakness, making it challenging to cope with the physical demands of pregnancy. Anemic mothers also have an increased risk of infections and are more prone to cardiovascular problems, such as irregular heart rhythms and heart murmurs. Additionally, anemia can aggravate pre-existing conditions, such as diabetes or hypertension, further complicating the pregnancy. Furthermore, postpartum anemia, occurring after childbirth, is more common in women who were anemic during pregnancy.
Complications for the Fetus
Anemia in pregnancy can have severe implications for the fetus. Intrauterine growth restriction, characterized by poor fetal growth, is more prevalent in anemic mothers. The fetus may not receive an adequate supply of oxygen, leading to various organ development issues. This can result in neurodevelopmental delays and an increased risk of infections. Furthermore, studies have shown that infants born to anemic mothers have a higher likelihood of developing anemia in early childhood and later in life.
Diagnosing Anemia in Pregnancy
Diagnosing anemia in pregnancy involves a combination of medical history, physical examination, and routine blood tests. During prenatal care visits, healthcare professionals will assess the woman’s medical history, including any previous instances of anemia or underlying conditions. They will also perform a physical examination, checking for signs such as pale skin, rapid heartbeat, and fatigue. Routine blood tests, including hemoglobin levels, provide further insight into the presence and severity of anemia. Additional tests, such as iron studies or specific genetic testing, may be conducted to determine the underlying cause of anemia.
Causes of Anemia in Pregnancy
Anemia in pregnancy can be attributed to various factors. The most common cause is iron deficiency, which occurs when the body lacks sufficient iron to produce an adequate amount of hemoglobin. Folate deficiency and vitamin B12 deficiency are also prevalent causes of anemia. Genetic disorders, such as sickle cell disease and thalassemia, can lead to anemia in pregnancy. Other genetic disorders affecting the red blood cells or their production may also contribute to anemia.
Preventing Anemia in Pregnancy
Prevention is key when it comes to managing anemia in pregnancy. Prenatal care plays a crucial role in identifying and addressing anemia early on. Healthcare providers may recommend iron and nutrient supplementation to meet the increased demands of pregnancy. Additionally, dietary modifications and the adoption of a healthy lifestyle can also help prevent anemia.
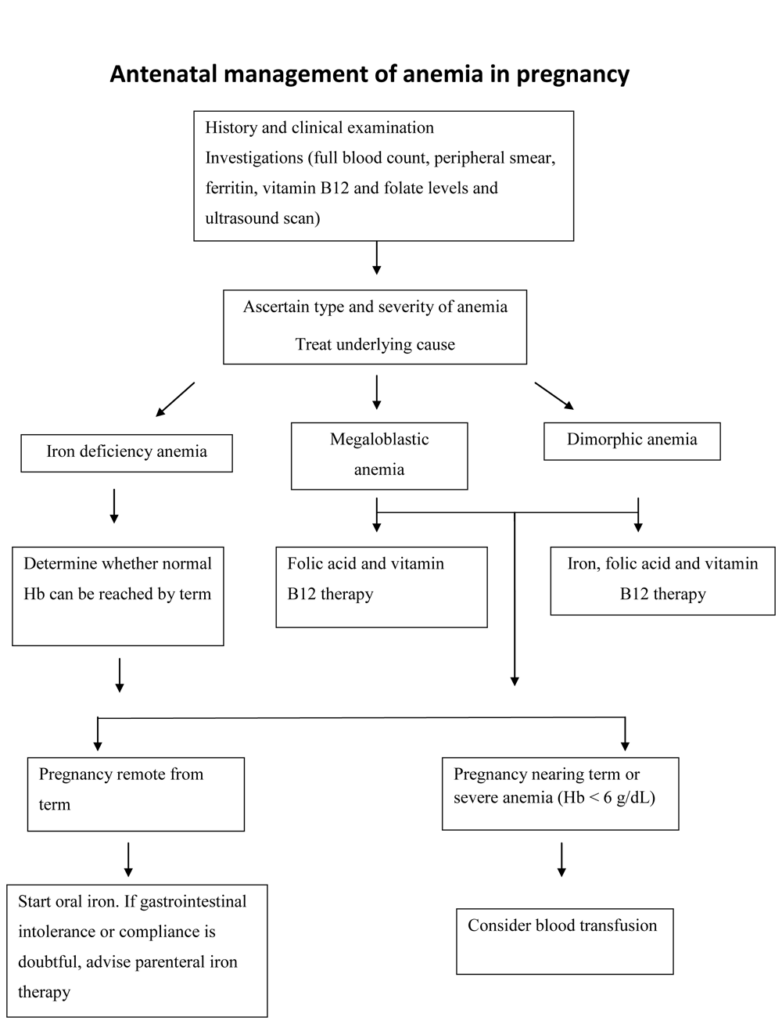
Treating Anemia in Pregnancy
If anemia is diagnosed during pregnancy, prompt treatment is essential to ensure the well-being of both mother and fetus. The primary method of treatment is iron supplementation. Iron supplements help replenish iron stores and aid in the production of healthy red blood cells. In cases where anemia is caused by a deficiency in folate or vitamin B12, appropriate supplementation may be prescribed. Close monitoring of hemoglobin levels is essential to evaluate the effectiveness of treatment.
Dietary Recommendations for Anemia in Pregnancy
A well-balanced diet can significantly contribute to preventing and managing anemia in pregnancy. Incorporating iron-rich foods, such as lean meats, seafood, leafy green vegetables, and fortified cereals, can increase iron intake. Folate-rich foods, including legumes, citrus fruits, and whole grains, are vital for red blood cell production. Vitamin B12 can be obtained from animal products like dairy, eggs, and poultry. Vegetarian and vegan options, such as legumes, tofu, and fortified plant-based milk alternatives, can provide essential nutrients for those following these dietary choices. It is important to avoid foods that inhibit iron absorption, such as tea, coffee, and calcium-rich foods, during meals.
In conclusion, anemia in pregnancy is a prevalent condition worldwide, with various impacts on both the mother and the fetus. Early diagnosis and appropriate treatment are crucial in ensuring a healthy pregnancy and birth outcomes. With proper prenatal care, iron supplementation, and a well-balanced diet, anemia in pregnancy can be effectively managed and prevented, promoting the well-being of both mothers and their children.
