In this article, you will discover the various treatment options available for bowel cancer. With an estimated 1.8 million new cases reported globally each year, understanding the different treatments can provide valuable insight for those affected. From surgery to chemotherapy and targeted therapy, there are a range of approaches that medical professionals utilize to combat this disease. By exploring these treatment options, you will gain a greater understanding of the resources available to patients and their families, providing hope and support during a challenging time.
Overview of Bowel Cancer
What is bowel cancer?
Bowel cancer, also known as colorectal cancer, is a type of cancer that affects the colon or rectum. It occurs when abnormal cells grow uncontrollably in the lining of these parts of the digestive system. If left untreated, the cancer cells can invade nearby tissues and spread to other parts of the body, making it crucial to detect and treat it early.
How common is bowel cancer?
Bowel cancer is one of the most common types of cancer worldwide. According to the World Health Organization (WHO), it is the third most commonly diagnosed cancer in both men and women. The risk of developing bowel cancer increases with age, with the majority of cases occurring in people over the age of 50. However, it can affect younger individuals as well.
Causes and risk factors
The exact causes of bowel cancer are not fully understood, but certain factors can increase the risk of developing the disease. These include a family history of bowel cancer or certain genetic conditions, such as Lynch syndrome or familial adenomatous polyposis (FAP). Other risk factors include a diet high in red and processed meats, smoking, excessive alcohol consumption, obesity, and a sedentary lifestyle. It is important to note that having one or more risk factors does not necessarily mean that a person will develop bowel cancer, but it does increase the likelihood.
Symptoms of bowel cancer
Several symptoms may indicate the presence of bowel cancer, although they can vary from person to person. Common symptoms include persistent changes in bowel habits, such as diarrhea or constipation, blood in the stool, abdominal pain or discomfort, unexplained weight loss, fatigue, and a feeling of incomplete bowel emptying. It is crucial to consult a healthcare professional if any of these symptoms persist, as they may indicate an underlying issue that requires medical attention.
Diagnosing Bowel Cancer
Initial evaluation
When a person exhibits symptoms that may suggest bowel cancer, their healthcare professional will conduct an initial evaluation. This typically involves a detailed medical history, physical examination, and discussions regarding any potential risk factors. The healthcare professional will also inquire about the duration and severity of symptoms, as well as any relevant family history. This initial evaluation serves as a foundation for further diagnostic tests.
Screening tests
Screening tests are essential for detecting bowel cancer in its early stages, even before symptoms arise. These tests are typically recommended for individuals aged 50 and above, or for those who have an increased risk due to their personal or family medical history. Common screening methods include fecal occult blood tests (FOBT), fecal immunochemical tests (FIT), sigmoidoscopy, and colonoscopy. Regular screenings can help identify precancerous polyps or early-stage bowel cancer, increasing the chances of successful treatment.
Diagnostic tests
When symptoms suggest the presence of bowel cancer, further diagnostic tests may be conducted to confirm the diagnosis. These tests may include imaging studies such as computed tomography (CT) scans, magnetic resonance imaging (MRI) scans, or positron emission tomography (PET) scans. Additionally, a tissue sample may be obtained through a biopsy to examine under a microscope for the presence of cancer cells. The results of these tests will help determine the stage and extent of the cancer, enabling healthcare professionals to develop an appropriate treatment plan.
Stages of Bowel Cancer
Stage 0
Stage 0 bowel cancer, also known as carcinoma in situ, refers to cancerous cells that are confined to the inner lining of the colon or rectum. At this stage, the cancer has not spread into the deeper layers of the bowel or to nearby lymph nodes. Early detection of stage 0 bowel cancer greatly increases the chances of successful treatment, as the cancer is localized and has not yet spread.
Stage I
In stage I bowel cancer, the cancer has grown through the inner lining of the bowel but has not spread beyond the wall of the colon or rectum. Lymph nodes are typically not affected at this stage. With prompt treatment, the prognosis for stage I bowel cancer is generally favorable, as the cancer is still contained within the bowel itself.
Stage II
Stage II bowel cancer is characterized by cancer that has spread through the wall of the colon or rectum but has not yet reached nearby lymph nodes. This stage is further divided into subcategories, depending on the extent of tumor penetration into the bowel wall. Though the cancer has not yet spread to lymph nodes, it is important to consider additional treatment options to minimize the risk of recurrence.
Stage III
At stage III, bowel cancer has spread to nearby lymph nodes but has not yet metastasized to distant parts of the body. This stage is also divided into subcategories depending on the number and extent of affected lymph nodes. Treatment for stage III bowel cancer often involves a combination of surgery, chemotherapy, and potentially radiation therapy to target the cancer cells both locally and systemically.
Stage IV
Stage IV bowel cancer is the most advanced stage, indicating that the cancer has spread to distant organs or tissues, such as the liver, lungs, or other distant lymph nodes. At this stage, treatment aims to manage the cancer and alleviate symptoms, as complete eradication may not be possible. Palliative care, which focuses on improving the patient’s quality of life, becomes a significant component of treatment.
Surgery as a Primary Treatment Option
Surgical removal of the tumor
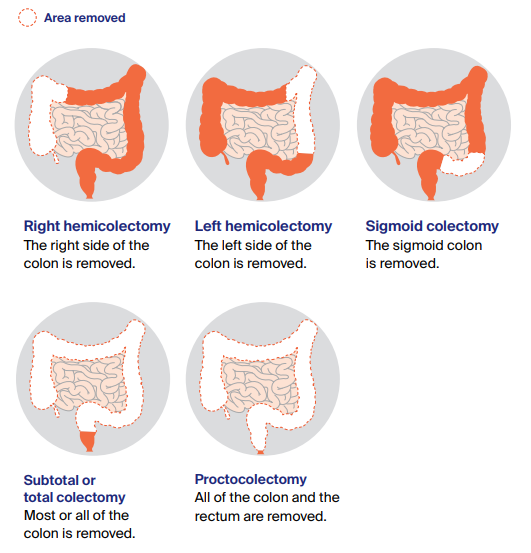
Surgery is often the primary treatment option for bowel cancer, particularly in the early stages. The main goal of surgery is to remove the tumor and any affected neighboring tissues or lymph nodes. The type of surgical procedure performed depends on the location and extent of the cancer. In some cases, a small section of the colon or rectum may be removed, while in more advanced cases, a more extensive surgery, such as a colectomy or proctectomy, may be necessary.
Types of surgery
There are several surgical approaches used to treat bowel cancer. These include open surgery, laparoscopic surgery (minimally invasive), and robotic-assisted surgery. In open surgery, a large incision is made in the abdomen to access the affected area. Laparoscopic surgery involves smaller incisions and the use of specialized tools and a camera, allowing the surgeon to perform the procedure with greater precision. Robotic-assisted surgery combines laparoscopic techniques with robotic technology, providing enhanced visualization and dexterity.
Potential risks and side effects
As with any surgical procedure, there are potential risks and side effects associated with surgery for bowel cancer. These may include infection, bleeding, blood clots, damage to surrounding organs or structures, and adverse reactions to anesthesia. Additionally, common side effects after surgery may include pain, fatigue, changes in bowel habits, and temporary or permanent colostomy or ileostomy (surgically created openings for waste elimination). It is important to discuss these potential risks and side effects with the healthcare team to make an informed decision about treatment.
Radiation Therapy
How does radiation therapy work?
Radiation therapy uses high-energy beams, such as X-rays or protons, to kill cancer cells or prevent them from growing. It is a localized treatment that precisely targets cancer cells while minimizing damage to healthy surrounding tissues. Radiation therapy works by damaging the DNA of cancer cells, leading to their death or impaired ability to divide and multiply. It can be delivered externally (external beam radiation) or internally (brachytherapy).
When is radiation therapy used?
Radiation therapy for bowel cancer is usually recommended as an adjunct to surgery or chemotherapy. It can be used before surgery to shrink tumors and make them easier to remove, or after surgery to destroy any remaining cancer cells. Radiation therapy may also be used to relieve symptoms and improve quality of life in cases where curative treatment is not possible. The decision to include radiation therapy in the treatment plan is based on the individual’s specific cancer stage, location, and overall health.
Types of radiation therapy
There are different types of radiation therapy that may be used for bowel cancer. External beam radiation therapy involves targeting the tumor from outside the body using a machine called a linear accelerator. This is the most common form of radiation therapy. Brachytherapy, on the other hand, involves placing small radioactive sources directly into or near the tumor. This allows for a more precise delivery of radiation, minimizing exposure to healthy tissues.
Potential risks and side effects
Radiation therapy can cause certain side effects, although they vary depending on the area being treated and the individual’s overall health. Common side effects may include fatigue, skin changes in the treated area, diarrhea, nausea, and temporary or long-term fertility issues. Bowel and bladder changes, such as increased frequency or urgency, may also occur. The healthcare team will closely monitor these side effects and provide supportive care to manage them effectively.
Chemotherapy
What is chemotherapy?
Chemotherapy is a systemic treatment for bowel cancer that uses drugs to destroy cancer cells throughout the body. Unlike surgery or radiation therapy, which target specific areas, chemotherapy aims to kill or control cancer cells that may have spread beyond the primary tumor. It can be administered orally (tablets or capsules) or intravenously (directly into the bloodstream) and may involve several treatment cycles spaced over weeks or months.
When is chemotherapy used?
Chemotherapy may be recommended at various stages of bowel cancer. When used as adjuvant therapy, it aims to destroy any remaining cancer cells after surgery to reduce the risk of recurrence. In cases where the cancer has spread to lymph nodes or distant organs, chemotherapy is often used as the primary treatment to shrink tumors and slow the progression of the disease. It may also be used to relieve symptoms and improve quality of life in advanced-stage cancer.
Types of chemotherapy drugs
Numerous chemotherapy drugs can be used to treat bowel cancer. Commonly used drugs include fluorouracil (5-FU), capecitabine, oxaliplatin, irinotecan, and combinations of these drugs. The specific drugs and dosages will vary depending on the individual’s cancer stage, overall health, and potential side effects. Chemotherapy is often administered in combination with other treatments, such as surgery or radiation therapy, to maximize its effectiveness.
Potential risks and side effects
Chemotherapy drugs can have various side effects due to their impact on rapidly dividing cells, which can affect normal tissues in addition to cancer cells. Common side effects may include fatigue, hair loss, nausea, vomiting, diarrhea, mouth sores, decreased appetite, and an increased risk of infections. Some chemotherapy drugs may also cause nerve damage, leading to symptoms such as tingling or numbness in the hands and feet. The healthcare team will closely monitor these side effects and provide supportive care to manage them effectively.
Targeted Therapy
What is targeted therapy?
Targeted therapy is a form of treatment that specifically targets certain molecules or pathways involved in the growth and progression of cancer cells. It aims to disrupt the signals that allow cancer cells to grow and divide, while minimizing damage to normal cells. Targeted therapy drugs are designed to interact with specific targets, such as proteins or genetic mutations, that are more commonly found in cancer cells than in healthy cells.
When is targeted therapy used?
Targeted therapy for bowel cancer is typically used in cases where specific genetic mutations or other molecular abnormalities are present. These include mutations in genes such as KRAS, NRAS, BRAF, or HER2. Targeted therapy may be used as a primary treatment option or in combination with other treatments, such as chemotherapy. The decision to use targeted therapy is based on the individual’s specific cancer profile, which is determined through genetic testing or other molecular diagnostics.
Types of targeted therapy drugs
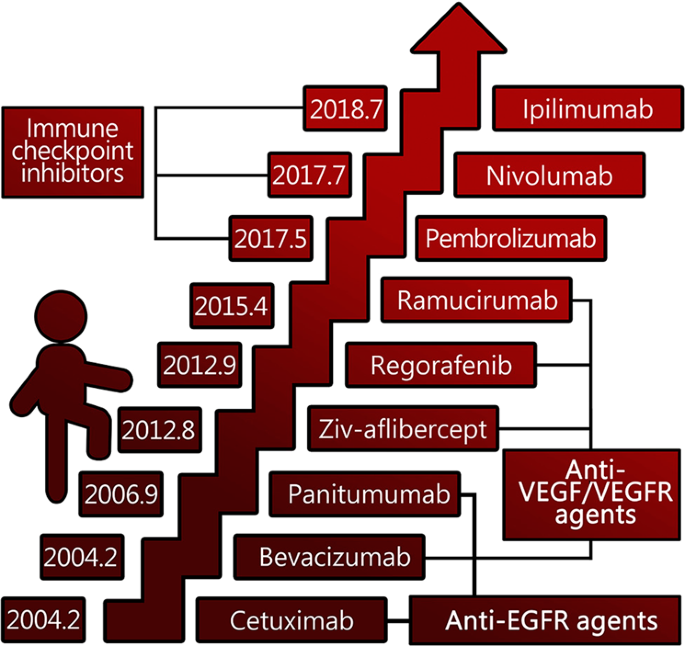
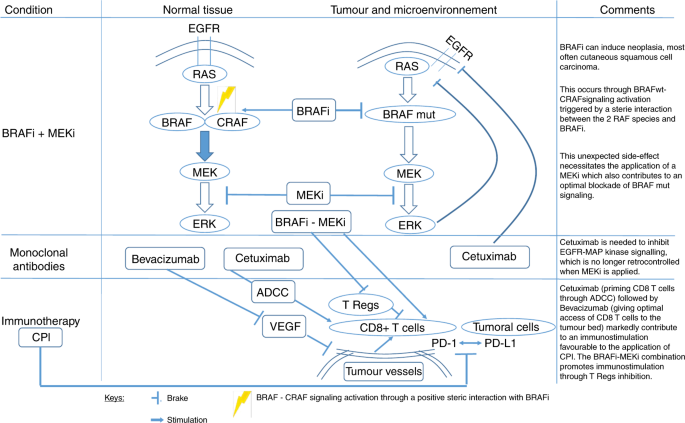
There are several targeted therapy drugs approved for the treatment of advanced bowel cancer. These include monoclonal antibodies, tyrosine kinase inhibitors, and immune checkpoint inhibitors. Monoclonal antibodies, such as bevacizumab and cetuximab, target specific proteins on the surface of cancer cells to prevent them from growing and spreading. Tyrosine kinase inhibitors, such as regorafenib and aflibercept, interfere with the signals that promote cancer cell growth. Immune checkpoint inhibitors, such as pembrolizumab and nivolumab, enhance the immune system’s ability to recognize and destroy cancer cells.
Potential risks and side effects
Targeted therapy drugs may have different side effects compared to traditional chemotherapy drugs, as they are designed to selectively target cancer cells. Common side effects may include diarrhea, skin changes, high blood pressure, liver problems, fatigue, and infusion reactions. The specific side effects and their severity will vary depending on the individual and the targeted therapy drug being used. Healthcare professionals will closely monitor the patient’s response to treatment and manage any side effects that may arise.
Immunotherapy
What is immunotherapy?
Immunotherapy is a type of treatment that harnesses the power of the immune system to recognize and eliminate cancer cells. It works by stimulating or enhancing the body’s own immune response to target and destroy cancer cells more effectively. Immunotherapy drugs, such as checkpoint inhibitors and cytokines, help overcome the immune system’s natural mechanisms that can prevent it from attacking cancer cells.
When is immunotherapy used?
Immunotherapy for bowel cancer may be recommended in specific cases where certain immune-related markers, such as high levels of microsatellite instability (MSI-H) or mismatch repair deficiency (dMMR), are present. These markers indicate that the immune system may be more likely to recognize and attack cancer cells. Immunotherapy is often used in advanced bowel cancer that has not responded to other treatments or has metastasized to other parts of the body. It may also be used as a part of clinical trials to explore its potential benefits.
Types of immunotherapy
Several types of immunotherapy are being investigated for the treatment of bowel cancer. Checkpoint inhibitors, such as pembrolizumab and nivolumab, block proteins that inhibit the immune system, allowing it to recognize and attack cancer cells. Cytokines, such as interleukin-2 and interferon-alpha, stimulate the immune system to enhance its anticancer activity. Various other immunotherapy approaches, such as cancer vaccines and adoptive cell therapy, are also being researched to further improve treatment outcomes.
Potential risks and side effects
Immunotherapy drugs can cause a range of side effects as they enhance the immune system’s activity. Common side effects of immunotherapy may include fatigue, skin rashes, itching, diarrhea, colitis (inflammation of the colon), hormonal imbalances, and flu-like symptoms. In some cases, immunotherapy can trigger an excessive immune response, resulting in more severe side effects known as immune-related adverse events (irAEs). These can include inflammation of organs, such as the lungs or liver, or autoimmune conditions. Regular monitoring is essential during immunotherapy treatment to identify and manage these potential side effects effectively.
Complementary and Alternative Treatments
Diet and nutrition
Maintaining a healthy diet and proper nutrition is important for individuals with bowel cancer. Consuming a diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can provide essential nutrients and support overall well-being. It is advisable to work with a registered dietitian or nutritionist who specializes in oncology to develop a personalized dietary plan based on individual needs and treatment effects.
Herbal supplements
The use of herbal supplements for the treatment of bowel cancer is not supported by sufficient scientific evidence. While some herbal supplements may have potential health benefits, it is important to consult with a healthcare professional before using any supplements, as they can interact with cancer treatments and have adverse effects. Your healthcare team can provide guidance on safe and appropriate supplement use.
Mind-body therapies
Mind-body therapies, such as meditation, yoga, and relaxation techniques, can help individuals with bowel cancer manage stress, anxiety, and improve overall well-being. These approaches can be a valuable complement to medical treatments but should not be used as a substitute. It is essential to consult with healthcare professionals knowledgeable in mind-body therapies to ensure safety and appropriate guidance.
Acupuncture
Acupuncture is a traditional Chinese medicine practice that involves the insertion of thin needles at specific points on the body to alleviate pain and promote wellness. Some individuals with bowel cancer may find acupuncture helpful in managing treatment-related side effects, such as pain, nausea, and fatigue. It is important to seek acupuncture from a licensed and experienced practitioner who has experience working with cancer patients.
Potential benefits and risks
Complementary and alternative treatments can provide additional support and relief for individuals with bowel cancer. They may help manage symptoms, improve quality of life, and provide a sense of empowerment. However, it is crucial to recognize that these treatments should be used alongside conventional medical treatments, not as replacements. Some complementary or alternative treatments may interact with medical treatments or have adverse effects. It is important to discuss these treatments with the healthcare team and ensure their safety and effectiveness in each individual case.
Discussing Treatment Options with a Healthcare Professional
Importance of open communication
Open and honest communication with a healthcare professional is crucial when considering treatment options for bowel cancer. Sharing concerns, questions, and goals allows for a collaborative decision-making process, ensuring that treatment plans align with the individual’s preferences and values. It is important to express any worries or fears and seek clarifications to make well-informed decisions.
Questions to ask
When discussing treatment options for bowel cancer, it is important to ask relevant questions to gain a comprehensive understanding of the proposed treatments. Some questions to consider asking healthcare professionals include:
- What are the benefits and risks of each treatment option?
- How will this treatment affect my daily life, including work, family, and personal commitments?
- Are there alternative treatments or clinical trials available?
- How long will the treatment last and what can I expect during and after treatment?
- What are the potential short-term and long-term side effects?
- How will the treatment affect my overall quality of life?
- What is the success rate of this treatment option for my specific cancer stage?
These questions can serve as a starting point for an open and informative discussion with the healthcare team.
Second opinions
Seeking a second opinion is a common and encouraged practice when considering treatment options for bowel cancer. It provides an opportunity to gain additional perspectives and insights from different healthcare professionals. A second opinion can help validate the initial diagnosis, explore alternative treatment approaches, and provide peace of mind. It is essential to communicate openly with both the primary healthcare professional and the consulting physician to ensure continuity and coordination of care.
Considerations for decision-making
When making treatment decisions for bowel cancer, it is important to consider various factors. These may include the individual’s overall health, cancer stage, treatment goals, potential risks and benefits, as well as personal preferences and values. Collaborating with healthcare professionals, discussing treatment options with loved ones, and seeking support from cancer support groups or psychologists can assist in making informed decisions that are aligned with individual needs and circumstances.
In conclusion, bowel cancer is a common type of cancer that requires early detection and the appropriate treatment strategy for optimal outcomes. Through a combination of diagnostic tests, surgery, radiation therapy, chemotherapy, targeted therapy, immunotherapy, and complementary treatments, individuals with bowel cancer can receive comprehensive care aimed at controlling the disease, managing symptoms, and improving their quality of life. Open communication with healthcare professionals, discussing treatment options, and considering individual considerations are crucial in ensuring personalized and effective treatment plans. With advancements in medical techniques and ongoing research, the prognosis for bowel cancer is improving, offering hope and better outcomes for those affected by this disease.