Are you curious about the latest research on Dengue Hemorrhagic Fever (DHF)? Look no further! In this article, we will provide you with a concise summary of the most recent findings regarding this serious and potentially fatal disease. With the aim of enhancing your understanding of DHF and providing you with valuable insights, we will explore the key aspects of this research. By the end of this article, you will be equipped with the latest knowledge on DHF and its implications, allowing you to stay informed and potentially contribute to the prevention and management of this global health issue. So, let’s dive into the fascinating world of the latest research on Dengue Hemorrhagic Fever!

Virology of Dengue Hemorrhagic Fever
Dengue Virus Family
Dengue Hemorrhagic Fever (DHF) is caused by the dengue virus, a member of the Flaviviridae family. This family of viruses includes several other important pathogens such as Zika virus and Yellow fever virus. The dengue virus is an RNA virus, which means that its genetic material is composed of ribonucleic acid. There are four serotypes of the dengue virus, known as DENV-1, DENV-2, DENV-3, and DENV-4. Each serotype has distinct characteristics that contribute to the complexity of the disease.
Serotypes of Dengue Virus
The four serotypes of the dengue virus share approximately 65-75% genetic similarity, however, they differ enough to result in distinct immune responses and disease outcomes. This diversity complicates the development of effective vaccines and treatments against dengue virus infection. Additionally, individuals who have been infected with one serotype can still become infected with another serotype, which increases the risk of severe disease and complications.
Genome Structure of Dengue Virus
The genome of the dengue virus is composed of a single-stranded RNA molecule, which encodes for three structural proteins (capsid, envelope, and membrane) and seven non-structural proteins. These proteins play important roles in the virus’s life cycle, replication, and interaction with the host immune system. Understanding the genome structure of the dengue virus is essential for developing targeted treatments and interventions.
Transmission of Dengue Hemorrhagic Fever
Vector-Borne Transmission
The primary mode of transmission of dengue virus is through the bite of infected Aedes mosquitoes, primarily Aedes aegypti. These mosquitoes are commonly found in tropical and subtropical regions, where they breed in clean water sources in and around human habitats. When a mosquito bites a person who is infected with dengue virus, it becomes infected and can transmit the virus to other individuals through subsequent bites. This vector-borne transmission is responsible for the majority of dengue cases worldwide.
Modes of Human-to-Human Transmission
While mosquito bites are the main mode of transmission for dengue virus, there are also rare cases of human-to-human transmission. This can occur through direct contact with infectious blood or bodily fluids, such as mother-to-infant transmission during childbirth or through the use of contaminated needles. However, these modes of transmission are relatively uncommon compared to mosquito-borne transmission.

Clinical Presentation
Symptoms of Dengue Hemorrhagic Fever
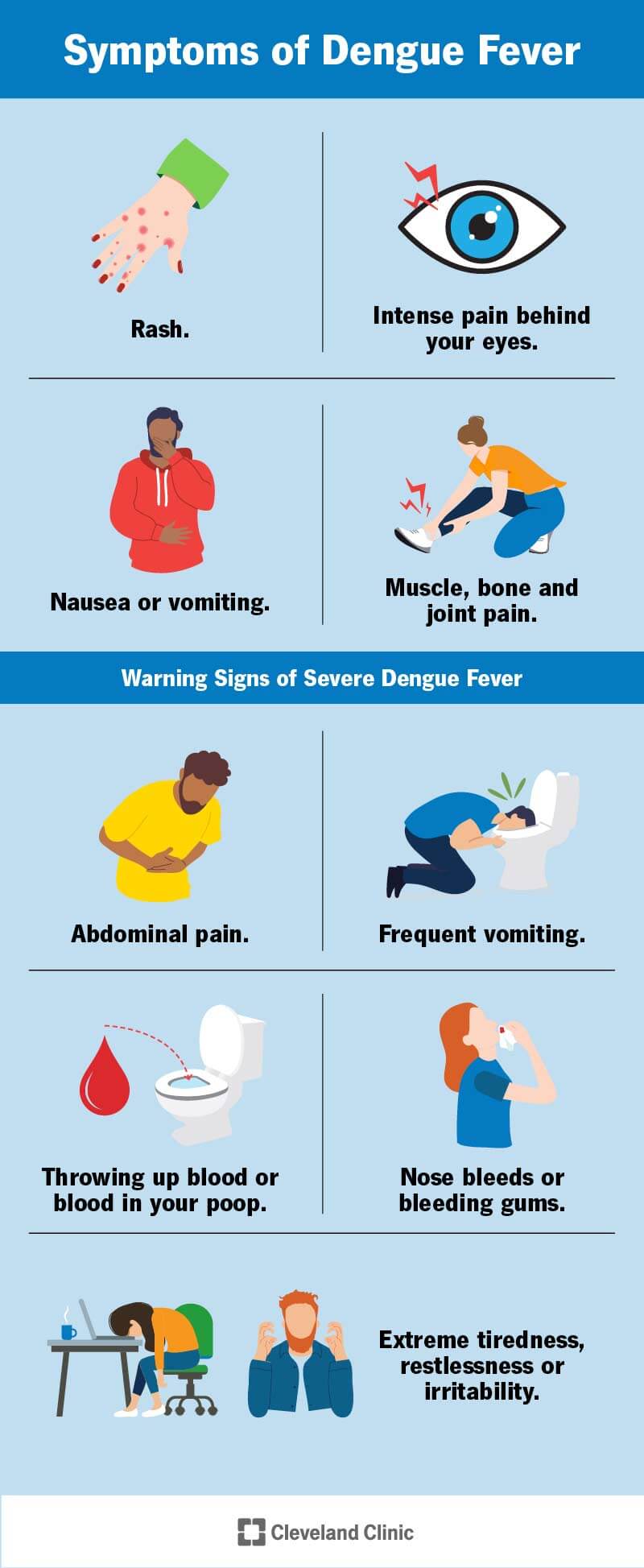
Dengue Hemorrhagic Fever manifests with a wide range of symptoms, ranging from mild to severe. In the initial stages of infection, individuals often experience flu-like symptoms such as fever, headache, muscle, and joint pain, nausea, and rash. These symptoms can last for a few days to a week. However, in some cases, the disease progresses to Dengue Hemorrhagic Fever, characterized by bleeding, organ damage, and severe plasma leakage. Warning signs of severe disease include persistent vomiting, severe abdominal pain, rapid breathing, fatigue, and bleeding from the gums.
Stages and Severity of Disease
Dengue Hemorrhagic Fever can be classified into three stages based on disease progression. The first stage, known as the febrile phase, is characterized by high fever, headache, and body aches. The second stage, called the critical phase, typically occurs around the time of defervescence and is associated with increased vascular permeability, plasma leakage, and potentially life-threatening complications. The third stage is the convalescent phase, where the individual recovers from the acute symptoms and begins the healing process.
Atypical Manifestations of Dengue Hemorrhagic Fever
While the classic symptoms of dengue hemorrhagic fever are well-documented, there are also atypical manifestations that can occur. These can include neurological manifestations, such as encephalitis, meningitis, and Guillain-Barré syndrome. Gastrointestinal symptoms, liver involvement, and kidney dysfunction can also occur. The atypical manifestations of dengue hemorrhagic fever highlight the complexity of the disease and the need for thorough clinical evaluation and monitoring.
Diagnosis
Laboratory Tests for Dengue Hemorrhagic Fever
Diagnosing dengue hemorrhagic fever requires a combination of clinical evaluation and laboratory testing. Laboratory tests commonly used include enzyme-linked immunosorbent assay (ELISA) for detecting dengue-specific antibodies, polymerase chain reaction (PCR) for detecting viral RNA, and viral isolation in cell culture. These tests help confirm the presence of dengue virus and determine the serotype, which can guide treatment decisions and public health interventions.
Importance of Early Diagnosis
Early diagnosis of dengue hemorrhagic fever is crucial for appropriate management and preventing complications. Timely identification of the disease allows healthcare providers to closely monitor the patient’s condition and provide supportive care. Early diagnosis also facilitates the implementation of vector control measures and public health interventions to prevent further transmission of the virus.
Differential Diagnosis
Distinguishing dengue hemorrhagic fever from other febrile illnesses can be challenging due to the similarity of symptoms. Other infectious diseases such as malaria, chikungunya, Zika virus, and influenza can present with similar symptoms. Thorough clinical evaluation, combined with laboratory testing, is required to differentiate dengue hemorrhagic fever from other potential causes of fever and flu-like symptoms.

Pathogenesis of Dengue Hemorrhagic Fever
Immunopathogenesis of Dengue Infection
The pathogenesis of dengue hemorrhagic fever is complex and involves both viral and host factors. Following infection, the dengue virus replicates in various immune cells, leading to the release of pro-inflammatory cytokines and activation of the immune response. In some cases, this immune response becomes dysregulated, leading to excessive production of cytokines and increased vascular permeability. The dysregulated immune response and vascular leakage are key components of the pathogenesis of dengue hemorrhagic fever.
Host Immune Response to Dengue Virus
The host immune response to dengue virus infection plays a crucial role in determining disease severity and outcome. The immune response involves both innate and adaptive immunity. Innate immune cells recognize the presence of the virus and initiate the inflammatory response. Adaptive immune cells produce specific antibodies and T cells that target the virus and infected cells. Understanding the host immune response is essential for developing effective interventions and therapies for dengue hemorrhagic fever.
Risk Factors
Individual Risk Factors
Certain factors can increase an individual’s risk of developing severe dengue hemorrhagic fever. These include age, with young children and older adults being at higher risk, as well as individuals with pre-existing medical conditions such as diabetes, hypertension, or immunosuppression. Additionally, individuals who have been previously infected with one serotype of the dengue virus are at higher risk of severe disease if they are infected with another serotype.
Environmental Risk Factors
Environmental factors also play a significant role in dengue hemorrhagic fever. The presence and abundance of Aedes mosquitoes, particularly in urban areas with inadequate sanitation and water management, increase the risk of transmission. Climate factors, such as temperature and rainfall patterns, also influence mosquito populations and the spread of dengue virus.
Socioeconomic Factors
Socioeconomic factors can influence the risk and impact of dengue hemorrhagic fever. Individuals living in low-income, crowded neighborhoods with limited access to healthcare may face additional challenges in preventing and managing the disease. Lack of awareness, poor sanitation, and inadequate vector control measures can contribute to increased dengue transmission and severity in vulnerable populations.

Prevention and Control
Vector Control Measures
Preventing dengue hemorrhagic fever relies heavily on effective vector control measures. These include eliminating mosquito breeding sites by emptying and cleaning containers that collect standing water, using insecticide-treated bed nets, and applying insect repellents. Community engagement and education play a key role in encouraging individuals to adopt these preventive measures.
Vaccines and Immunization Programs
Efforts to develop a safe and effective dengue vaccine have shown promising results in recent years. Vaccination can provide long-term protection against dengue virus infection and reduce the risk of severe disease. Immunization programs targeting high-risk populations, such as children and individuals living in endemic areas, are crucial for preventing and controlling the spread of dengue hemorrhagic fever.
Community Education and Awareness
Raising awareness about dengue hemorrhagic fever is essential for prevention and control. Educating individuals and communities about the symptoms, transmission, and prevention methods can empower them to take necessary precautions and seek early medical care. Community-based initiatives, such as health campaigns and school programs, can contribute to increasing knowledge and promoting behavior change.
Treatment
Supportive Care
There is currently no specific antiviral treatment for dengue hemorrhagic fever. Management primarily involves supportive care to alleviate symptoms and prevent complications. Patients with severe disease may require hospitalization, intravenous fluid replacement, and close monitoring of vital signs. Pain relief medications and rest are important for patient comfort and recovery.
Fluid Management Strategies
Maintaining fluid balance is a critical aspect of managing dengue hemorrhagic fever. Intravenous fluid administration helps stabilize blood pressure, prevent dehydration, and restore electrolyte balance. Doctors closely monitor fluid intake and output to guide fluid management and prevent fluid overload. Early recognition and appropriate fluid management can significantly improve patient outcomes.
Experimental Treatments
Research is ongoing to identify potential antiviral agents and therapeutic interventions for dengue hemorrhagic fever. Some experimental treatments under investigation include antiviral drugs, immunomodulatory agents, and plasma exchange. These treatments aim to target the viral replication and dysregulated immune response associated with severe dengue disease. However, further research is needed to determine their safety and efficacy.
Epidemiology
Global Burden of Dengue Hemorrhagic Fever
Dengue hemorrhagic fever is a global health concern, with an estimated 390 million infections occurring annually. The disease is endemic in over 100 countries, with the largest burden in Asia, the Pacific, and the Americas. Dengue-related complications, including dengue hemorrhagic fever, can cause significant morbidity and mortality, particularly in resource-limited settings without access to adequate healthcare.
Regional Outbreaks and Trends
Dengue outbreaks often occur in a cyclical pattern, with peak transmission during certain seasons. The incidence of dengue hemorrhagic fever can vary within and between regions, influenced by factors such as climate, population density, and vector control measures. Monitoring outbreak patterns and trends is crucial for targeted interventions and allocation of resources to control the spread of the virus.
Seasonality of Disease
Dengue transmission is influenced by seasonal fluctuations in mosquito populations and human behavior. In many regions, dengue cases increase during the rainy season when mosquito breeding sites are more abundant. Increased travel during holidays and festivals can also contribute to the spread of the virus across different regions. Understanding the seasonality of dengue helps guide prevention and control strategies.
Future Directions for Research
Advancements in Vaccine Development
Ongoing research and development of dengue vaccines aim to improve vaccine efficacy and safety. Efforts are focused on developing a tetravalent vaccine that provides protection against all four dengue serotypes. Additionally, studies are being conducted to assess the long-term durability of vaccine-induced immunity and explore the potential for combined vaccinations against multiple flaviviruses.
Understanding Immune Responses
Further research is needed to better understand the immune responses to dengue virus infection and their contributions to disease outcomes. Studies are focused on characterizing the immune responses associated with severe disease, identifying biomarkers for early diagnosis, and exploring host factors that influence susceptibility to dengue hemorrhagic fever. This knowledge will inform the development of targeted interventions.
Improved Diagnostics
Advancements in diagnostic techniques are crucial for early detection and management of dengue hemorrhagic fever. Research is ongoing to improve the accuracy and accessibility of diagnostic tools, such as point-of-care tests and rapid detection methods. These advancements will facilitate timely diagnosis, ensure appropriate patient care, and contribute to effective disease surveillance and control.
In conclusion, understanding the virology, transmission, clinical presentation, diagnosis, pathogenesis, risk factors, prevention, treatment, epidemiology, and future research directions of dengue hemorrhagic fever is essential for combating this global health challenge. Multidisciplinary efforts involving virologists, epidemiologists, clinicians, public health officials, and researchers from various disciplines are crucial for improving prevention, diagnosis, and management strategies to reduce the burden of dengue hemorrhagic fever worldwide.