Have you ever wondered about the symptoms and diagnosis of heart disease? In this article, we will explore the various signs and indicators that can help you identify this common condition. Understanding the symptoms is crucial for early detection and seeking appropriate medical care. From chest pain to shortness of breath, we will discuss the range of symptoms experienced by individuals with heart disease. Additionally, we will delve into the diagnostic tests and procedures used by healthcare professionals to accurately diagnose this potentially life-threatening condition.
Risk factors for heart disease
Heart disease is a serious condition that can have a significant impact on your health and well-being. Understanding the risk factors associated with heart disease is essential for prevention and early detection. By recognizing these risk factors, you can take proactive steps to protect your heart health.
High blood pressure
High blood pressure, also known as hypertension, is one of the leading risk factors for heart disease. When your blood pressure is consistently high, it puts extra strain on your heart and arteries, increasing the likelihood of developing heart disease. Monitoring your blood pressure regularly and taking steps to keep it within a healthy range is crucial for heart health.
High cholesterol
Having high levels of cholesterol in your blood can lead to the development of plaques in your arteries, a condition known as atherosclerosis. These plaques can restrict blood flow to the heart, increasing the risk of heart disease. It is important to have your cholesterol levels checked regularly and make lifestyle changes or take medications as recommended by your doctor to manage and control your cholesterol levels.
Smoking
Smoking is a major risk factor for heart disease. The chemicals present in tobacco smoke can damage the lining of your arteries, leading to the development of atherosclerosis. Smoking also increases your blood pressure and heart rate, making your heart work harder. Quitting smoking is one of the most significant steps you can take to reduce your risk of heart disease.
Obesity
Being overweight or obese puts extra strain on your heart. It increases the risk of high blood pressure, high cholesterol, and diabetes, all of which are risk factors for heart disease. Maintaining a healthy weight through a balanced diet and regular exercise is essential for reducing your risk of heart disease.
Diabetes
Diabetes is a chronic condition characterized by high blood sugar levels. It significantly increases the risk of heart disease as it can damage blood vessels and nerves that control the heart. Managing diabetes through regular monitoring of blood sugar levels, medication, and a healthy lifestyle can help lower the risk of heart disease.
Family history of heart disease
If you have a family history of heart disease, your risk of developing the condition is higher. Genetic factors can play a role in the development of heart disease. It is important to be aware of your family history and discuss it with your doctor so that appropriate preventive measures can be taken.
Common symptoms of heart disease
Recognizing the symptoms of heart disease is crucial for early detection and prompt medical intervention. While some symptoms may be more subtle or easily mistaken for other conditions, paying attention to any changes or discomfort in your body can help catch potential heart problems early.
Chest pain or discomfort
Chest pain or discomfort, also known as angina, is one of the most common symptoms of heart disease. It may feel like pressure, tightness, squeezing, or a burning sensation in the chest. This pain may also radiate to the arms, shoulders, jaw, neck, or back. If you experience chest pain, it is important to seek medical attention immediately.
Shortness of breath
Feeling breathless or experiencing difficulty breathing, particularly with exertion, can be a symptom of heart disease. This occurs when the heart is unable to pump enough oxygen-rich blood to meet the body’s demands. If you find yourself frequently short of breath, even with minimal physical activity, it is essential to consult a healthcare professional.
Fatigue
Excessive fatigue or a feeling of being extremely tired, even after adequate rest, can be a sign of heart disease. The heart has to work harder when it is compromised, leading to feelings of fatigue or a decrease in energy levels. If you regularly experience unexplained fatigue that affects your daily activities, it is important to discuss this with your doctor.
Dizziness or lightheadedness
Feeling dizzy or lightheaded can be a symptom of heart disease, especially if it occurs suddenly or is accompanied by other symptoms such as chest pain or shortness of breath. This can be due to insufficient blood flow to the brain, causing feelings of dizziness or faintness. It is important to seek medical attention if you experience frequent episodes of dizziness.
Swelling in the legs, ankles, or feet
Swelling, also known as edema, in the lower extremities can be a sign of heart disease. When the heart is unable to pump blood efficiently, fluid can build up in the body, leading to swelling in the legs, ankles, or feet. If you notice persistent or worsening swelling, it is important to bring this to the attention of your healthcare provider.
Palpitations
Palpitations refer to an irregular or rapid heartbeat that is noticeable to you. You may feel as though your heart is skipping beats, fluttering, or beating too hard. While palpitations can sometimes be harmless, they can also be a symptom of an underlying heart condition. If you experience frequent or concerning palpitations, it is important to have them evaluated by a healthcare professional.
Fainting or loss of consciousness
Fainting or sudden loss of consciousness can be a serious symptom of heart disease. It occurs when there is a temporary interruption in the blood flow to the brain. If you experience fainting episodes, it is essential to seek immediate medical attention to determine the underlying cause.
Types of heart disease
Heart disease encompasses a range of conditions that can affect the heart and its ability to function optimally. Understanding the different types of heart disease can help you gain insight into how they impact your heart’s health and the potential treatment options available.
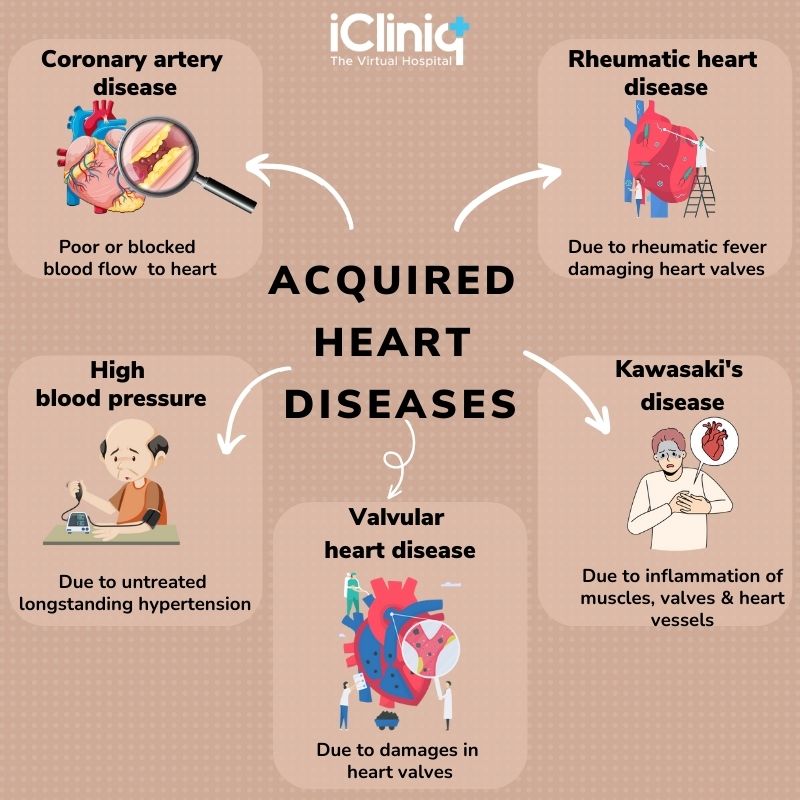
Coronary artery disease (CAD)
Coronary artery disease occurs when the arteries that supply blood to the heart become narrow or blocked due to the buildup of plaque. This limits blood flow to the heart, resulting in symptoms such as chest pain or discomfort (angina) and increasing the risk of a heart attack. Lifestyle modifications, medications, and procedures like stenting may be utilized to manage CAD.
Heart attack
A heart attack, also known as myocardial infarction, occurs when there is a blockage in the coronary arteries, cutting off the blood supply to the heart muscle. This can result in permanent damage to the heart muscle if not treated promptly. Symptoms of a heart attack may include chest pain, shortness of breath, and pain radiating to the arm, shoulder, jaw, neck, or back. Immediate medical attention is necessary in the event of a heart attack to minimize long-term damage.
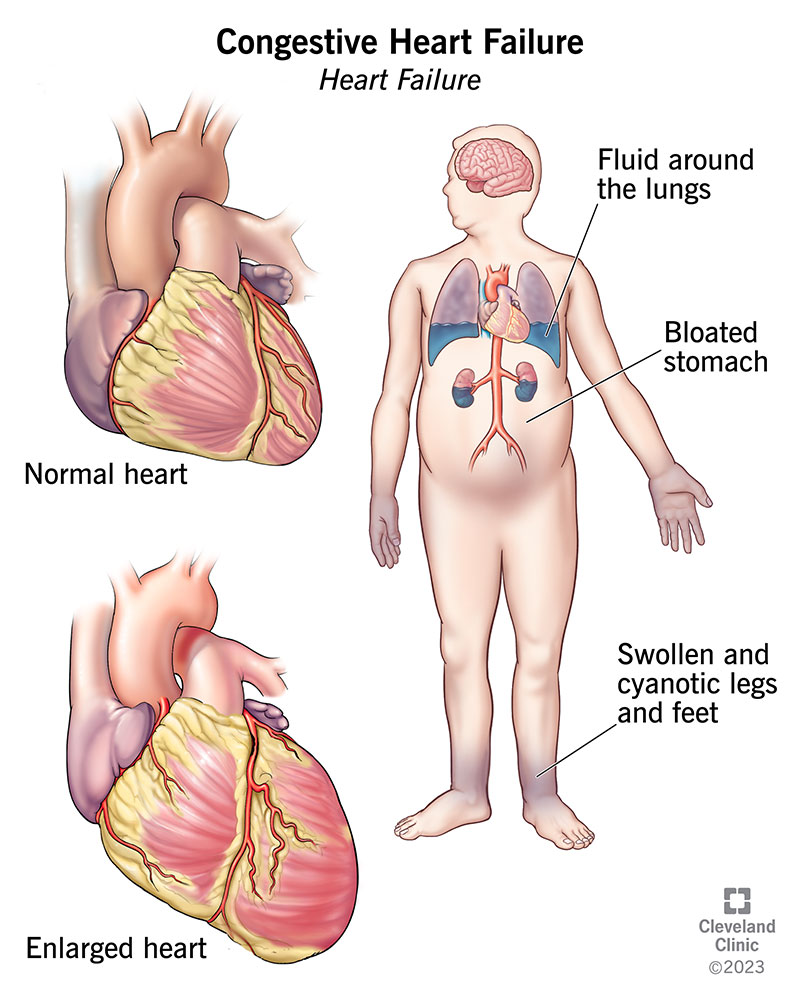
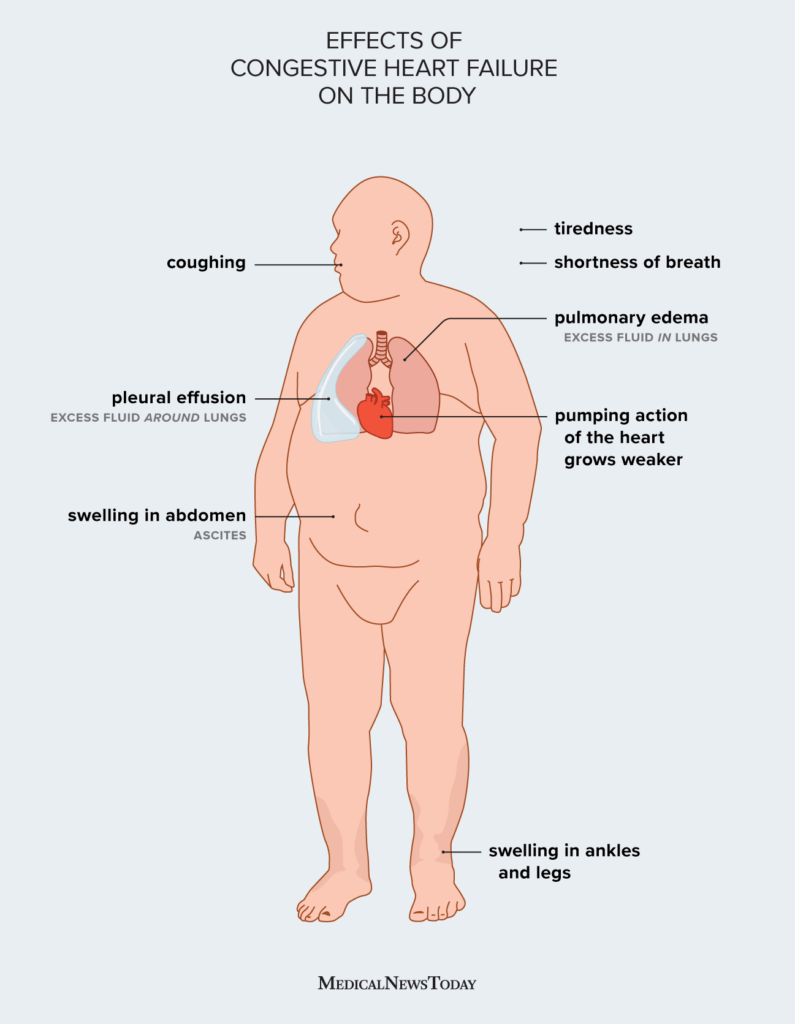
Heart failure
Heart failure refers to a condition in which the heart is unable to pump blood effectively, leading to a reduced supply of oxygen and nutrients to the body’s tissues. This can result in symptoms such as shortness of breath, fatigue, and swelling in the legs and ankles. Treatment for heart failure may involve medications, lifestyle changes, and in some cases, surgical interventions like implantable devices or heart transplant.
Arrhythmias
Arrhythmias refer to irregular heart rhythms that can range from harmless to life-threatening. These abnormal heart rhythms can cause symptoms such as palpitations, dizziness, fainting, or shortness of breath. Treatment options for arrhythmias may include medications, lifestyle modifications, implantable devices, or procedures like cardiac ablation.
Valvular heart disease
Valvular heart disease occurs when there is damage or dysfunction of the heart valves, which control the flow of blood through the heart. This can lead to symptoms such as fatigue, shortness of breath, and chest pain. Treatment options for valvular heart disease may involve medication, surgery to repair or replace the damaged valve, or minimally invasive procedures like transcatheter valve repair or replacement.
Cardiomyopathy
Cardiomyopathy is a condition that affects the heart muscle, making it harder for the heart to pump blood effectively. This can result in symptoms such as fatigue, breathlessness, and swelling in the legs and ankles. Treatment for cardiomyopathy may include medications, lifestyle modifications, implantable devices, or, in severe cases, heart transplant.
Diagnostic tests for heart disease
When it comes to diagnosing heart disease, various tests are available to assess the condition of the heart and its function. These diagnostic tests help healthcare professionals accurately determine the presence and severity of heart disease, enabling appropriate treatment and management strategies.
Electrocardiogram (ECG)
An electrocardiogram, also known as an ECG or EKG, is a non-invasive test that records the electrical activity of the heart. It helps identify abnormal heart rhythms, damage to the heart muscle, and other heart-related conditions. During an ECG, electrodes are placed on the chest, arms, and legs, and the electrical signals produced by the heart are recorded.
Echocardiogram
An echocardiogram is a non-invasive test that uses sound waves to create images of the heart. It provides detailed information about the heart’s structure, function, and blood flow. During an echocardiogram, a transducer is placed on the chest, and the sound waves bounce off the structures of the heart, creating images that can be viewed in real-time.
Stress test
A stress test, also known as an exercise stress test or treadmill test, evaluates the heart’s function during physical activity. It helps determine how the heart responds to exertion and can detect abnormalities that may not be noticeable at rest. During a stress test, the patient is asked to walk on a treadmill or pedal a stationary bicycle while being monitored by an ECG.
Cardiac catheterization
Cardiac catheterization, also known as an angiogram, is an invasive procedure that involves the insertion of a thin tube (catheter) into a blood vessel, usually in the groin or arm. The catheter is guided to the heart, and a contrast dye is injected to visualize the coronary arteries. This procedure provides detailed information about blockages or narrowing in the arteries that supply blood to the heart.
Angiogram
An angiogram is a specific type of cardiac catheterization that focuses on visualizing the blood vessels. It is commonly used to evaluate blockages or narrowing in the coronary arteries. By using contrast dye, X-rays are taken to provide a detailed map of the arteries, allowing the healthcare professional to determine the severity and location of any blockages.
Blood tests
Blood tests, such as lipid profiles and cardiac enzyme tests, can provide valuable information about heart health. Lipid profiles measure cholesterol and triglyceride levels, which can indicate the presence of coronary artery disease. Cardiac enzyme tests measure the presence of specific proteins in the blood that are released when there is damage to the heart muscle.

Physical examination for heart disease
A physical examination by a healthcare professional can provide valuable insights into your heart health. During a physical exam, the healthcare provider will assess various factors related to your heart and overall well-being.
Listening to the heart
Using a stethoscope, the healthcare provider listens to your heart sounds. Any abnormalities, such as murmurs or irregular rhythms, can provide clues about possible heart conditions.
Checking blood pressure
A blood pressure measurement is an essential part of a physical examination. High blood pressure is a significant risk factor for heart disease, and regular monitoring is crucial for maintaining heart health.
Feeling pulses
Feeling pulses at various points in the body, such as in the wrists, can help the healthcare provider assess blood flow. Abnormal pulses or discrepancies in pulses between different areas may indicate underlying heart conditions.
Checking for swelling
The healthcare provider will visually inspect your body for any signs of edema or swelling, particularly in the legs, ankles, or feet. Swelling may be an indication of heart failure or other heart-related issues.
Listening to the lungs
By using a stethoscope, the healthcare provider listens to your lung sounds. This helps assess the respiratory system and can provide insights into any potential heart-related complications.
Medical history and risk assessment
A thorough medical history and risk assessment form the foundation for diagnosing and managing heart disease. By discussing your symptoms, evaluating risk factors, and reviewing medical history, healthcare providers can develop an accurate picture of your heart health and devise appropriate treatment plans.
Discussion of symptoms
During a medical evaluation, healthcare professionals will ask you detailed questions about your symptoms. Describing the nature, frequency, and duration of any symptoms you are experiencing can help narrow down potential heart conditions.
Evaluation of risk factors
Understanding and evaluating your risk factors is essential for assessing your likelihood of developing heart disease. Risk factors, such as high blood pressure, high cholesterol, diabetes, obesity, smoking, and family history of heart disease, will be considered to develop a comprehensive plan for prevention and management.
Family history evaluation
Genetic factors play a significant role in heart disease. Providing information about your family’s history of heart disease can help healthcare professionals determine your level of risk and develop strategies for prevention and treatment.
Review of medications and prior medical conditions
Considering your past medical history and medications is crucial for diagnosing and managing heart disease effectively. Certain medications or medical conditions can impact your heart health and need to be taken into account when assessing your overall risk and developing treatment plans.

Coronary angiography for heart disease diagnosis
Coronary angiography, also known as cardiac catheterization, is a diagnostic procedure used to visualize the coronary arteries and evaluate the presence of blockages or narrowing. This procedure provides detailed information about the condition of the arteries and helps guide treatment decisions.
Procedure overview
During coronary angiography, a thin tube called a catheter is inserted into a blood vessel, usually in the groin or arm. The catheter is then guided to the heart, and a contrast dye is injected to make the blood vessels visible on X-rays. This allows the healthcare professional to assess the presence, location, and severity of any coronary artery blockages.
Preparation for angiography
Before undergoing coronary angiography, you will be asked to refrain from eating or drinking for several hours. Medications that may interfere with the procedure may also need to be temporarily discontinued. Your healthcare provider will provide specific instructions on how to prepare for the procedure.
The angiography procedure
During the procedure, you will be awake but given medication to help you relax. The catheter is inserted into the blood vessel, and X-ray images are taken as the contrast dye is injected. You may experience a warm sensation as the dye is administered. The procedure typically takes about 30 minutes to an hour.
Risks and complications
While coronary angiography is generally considered safe, there are risks associated with any invasive procedure. These risks include bleeding, infection, allergic reactions to the contrast dye, blood vessel damage, and irregular heart rhythms. It is important to discuss the potential risks and benefits of coronary angiography with your healthcare provider before undergoing the procedure.
Clotting tests for heart disease diagnosis
Clotting tests are laboratory tests used to assess the ability of blood to clot and detect any abnormalities that may increase the risk of heart disease. These tests play a crucial role in diagnosing and managing certain heart conditions.
Prothrombin time (PT)
Prothrombin time measures how long it takes for blood to clot. It assesses the function of certain clotting factors in the blood, providing information about the body’s ability to form a clot. Abnormal PT results may indicate an increased risk of blood clots or bleeding disorders.
Activated partial thromboplastin time (aPTT)
Activated partial thromboplastin time measures how long it takes for blood to clot in a different pathway than PT. It helps evaluate the function of additional clotting factors, providing a comprehensive assessment of the blood’s clotting ability. Deviations from the normal range may signal an increased risk of bleeding or clotting disorders.
International normalized ratio (INR)
The international normalized ratio is a standardized measure used to interpret PT and ensure consistency across different laboratories. It is commonly used to monitor and adjust the dosage of anticoagulant medications like warfarin. Consistently elevated INR levels may indicate an increased risk of bleeding, while consistently low levels may suggest an increased risk of blood clots.
D-dimer test
The D-dimer test measures the presence of a substance called D-dimer in the blood. D-dimer is produced when blood clots are broken down. Elevated levels may indicate the presence of a blood clot, as seen in conditions like deep vein thrombosis, pulmonary embolism, or disseminated intravascular coagulation.
Treatment options for heart disease
Heart disease treatment aims to manage symptoms, prevent or control complications, and improve overall heart health. The appropriate treatment options depend on the type and severity of the heart disease and are tailored to each individual’s specific needs.
Lifestyle changes
Making lifestyle changes is a critical component of heart disease management. These changes may include adopting a heart-healthy diet, engaging in regular exercise, quitting smoking, managing stress levels, and maintaining a healthy weight. These lifestyle modifications can help reduce risk factors and improve heart health.
Medications
Medications play a crucial role in managing heart disease. Depending on the specific type of heart disease and individual needs, medications may be prescribed to control blood pressure, lower cholesterol levels, manage arrhythmias, prevent blood clots, or improve heart function. It is important to take medications as prescribed and attend regular follow-up appointments to monitor their effectiveness and adjust dosages if needed.
Angioplasty and stenting
Angioplasty is a minimally invasive procedure used to open narrowed or blocked arteries. During the procedure, a catheter with a balloon on its tip is inserted into the blocked artery. The balloon is inflated to compress the plaque against the artery walls, restoring blood flow. In some cases, a stent, a small mesh tube, may be placed during angioplasty to help keep the artery open.
Bypass surgery
Coronary artery bypass grafting (CABG) is a surgical procedure used to treat severe coronary artery disease. It involves redirecting blood flow around blocked or narrowed arteries by using blood vessels from other parts of the body. This creates new routes for blood to reach the heart muscle, relieving symptoms and improving blood flow.
Heart transplant
In cases of end-stage heart disease, a heart transplant may be considered. This involves replacing a failing heart with a healthy donor heart. Heart transplantation is a complex procedure that is reserved for individuals with severe heart disease who have not responded to other treatment options.
Prevention and management of heart disease
Prevention and management of heart disease are essential for maintaining optimal heart health and reducing the risk of complications. By making lifestyle changes, managing risk factors, and following medical advice, individuals can minimize their chances of developing heart disease and maintain a healthy heart.
Maintaining a healthy diet
A heart-healthy diet focuses on consuming nutrient-rich foods while limiting the intake of saturated fats, trans fats, cholesterol, salt, and added sugars. Prioritizing fruits, vegetables, whole grains, lean proteins, and healthy fats can help lower blood pressure, cholesterol levels, and manage weight.
Regular exercise
Engaging in regular physical activity is crucial for preventing and managing heart disease. Aim for at least 150 minutes of moderate-intensity aerobic exercise or 75 minutes of vigorous exercise each week. Incorporating strength training exercises can further improve heart health and overall fitness.
Quitting smoking
Quitting smoking is one of the most important steps you can take to protect your heart health. Smoking damages blood vessels, increases the risk of atherosclerosis, raises blood pressure, and reduces oxygen levels in the blood. Quitting smoking significantly lowers the risk of heart disease.
Managing stress
Chronic stress can have a negative impact on heart health. Finding healthy ways to manage stress, such as practicing relaxation techniques, engaging in hobbies, spending time with loved ones, or seeking professional support, can contribute to better heart health.
Controlling blood pressure and cholesterol
Monitoring and controlling blood pressure and cholesterol levels are essential for preventing and managing heart disease. Regular check-ups, lifestyle modifications, and medication, if necessary, can help keep these risk factors within a healthy range.
Monitoring diabetes
If you have diabetes, managing your blood sugar levels is crucial for heart health. Regular monitoring, medication, lifestyle modifications, and working closely with healthcare professionals are key to minimizing the risk of heart disease complications.
In conclusion, being aware of the risk factors, symptoms, and types of heart disease is essential for the prevention and early detection of this potentially life-threatening condition. By incorporating lifestyle changes, working closely with healthcare professionals, and following prescribed treatment plans, individuals can maintain a healthy heart and reduce the risk of heart disease and its complications. Prioritizing heart health is a lifelong commitment that can lead to a happier, healthier life.