Macular Degeneration, a common age-related eye condition, is a topic that demands attention and understanding. This article aims to shed light on the causes, symptoms, and available treatment options for this progressive disease, allowing you to navigate the complexities of Macular Degeneration with confidence. With a friendly tone and clear explanations, it seeks to empower you with knowledge, ensuring that you are equipped to make informed decisions regarding your eye health. So, let’s dive in and unravel the mysteries of Macular Degeneration together!
Causes of Macular Degeneration
Age-related macular degeneration
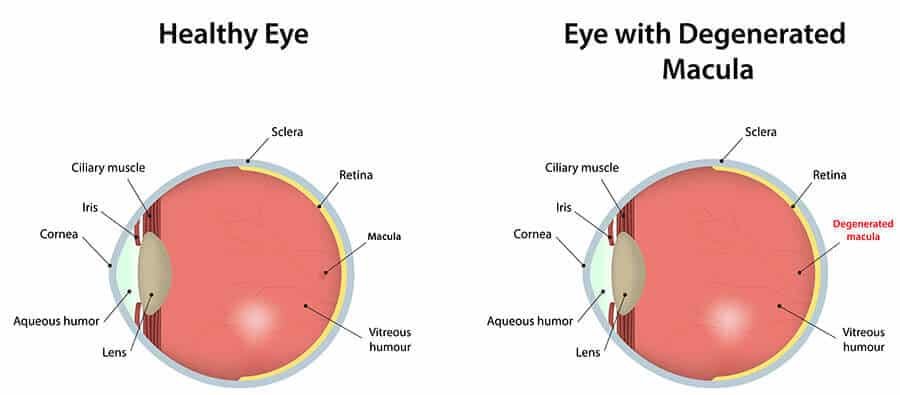
Age-related macular degeneration (AMD) is the most common cause of macular degeneration. As the name suggests, it primarily affects older adults, typically over the age of 50. The macula, a small part of the retina responsible for sharp central vision, begins to deteriorate, causing vision loss. While the exact cause of AMD is unknown, it is believed to be a combination of genetic and environmental factors.
Genetic factors
Genetic factors play a significant role in the development of macular degeneration. Family history of the disease increases the risk of developing AMD. Certain genetic variations and mutations have been identified as potential risk factors. Understanding the genetic basis of macular degeneration can help in identifying those at higher risk and developing targeted treatment strategies.
Smoking
Smoking has been strongly linked to an increased risk of developing macular degeneration. The harmful components of tobacco smoke, such as nicotine and free radicals, can damage the retina and blood vessels in the eye. Smoking also reduces the effectiveness of treatment options for macular degeneration, making it crucial to quit smoking to prevent further vision loss.
Unhealthy diet
A poor diet lacking in essential nutrients can contribute to the development of macular degeneration. Studies have shown that a diet high in saturated fats, cholesterol, and processed foods can increase the risk of AMD. On the other hand, a diet rich in green leafy vegetables, fruits, whole grains, and omega-3 fatty acids can help protect against macular degeneration.
Types of Macular Degeneration
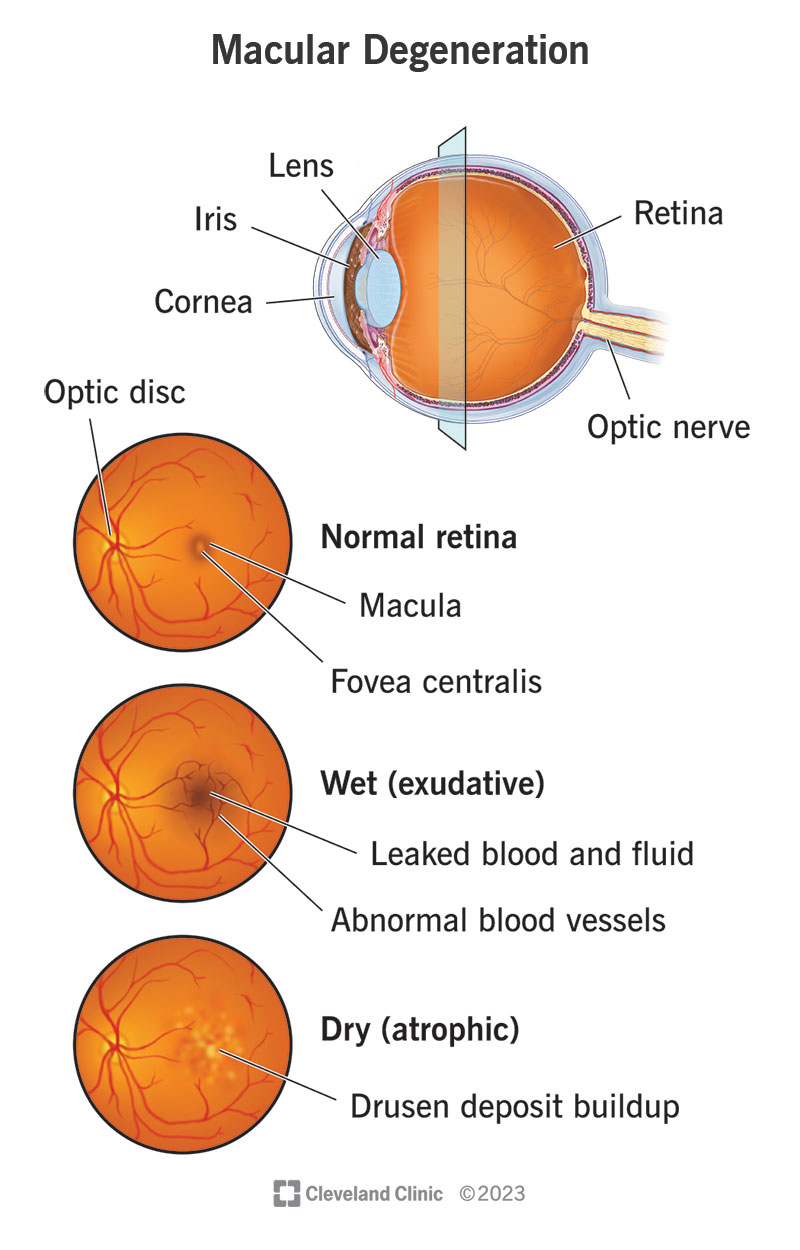
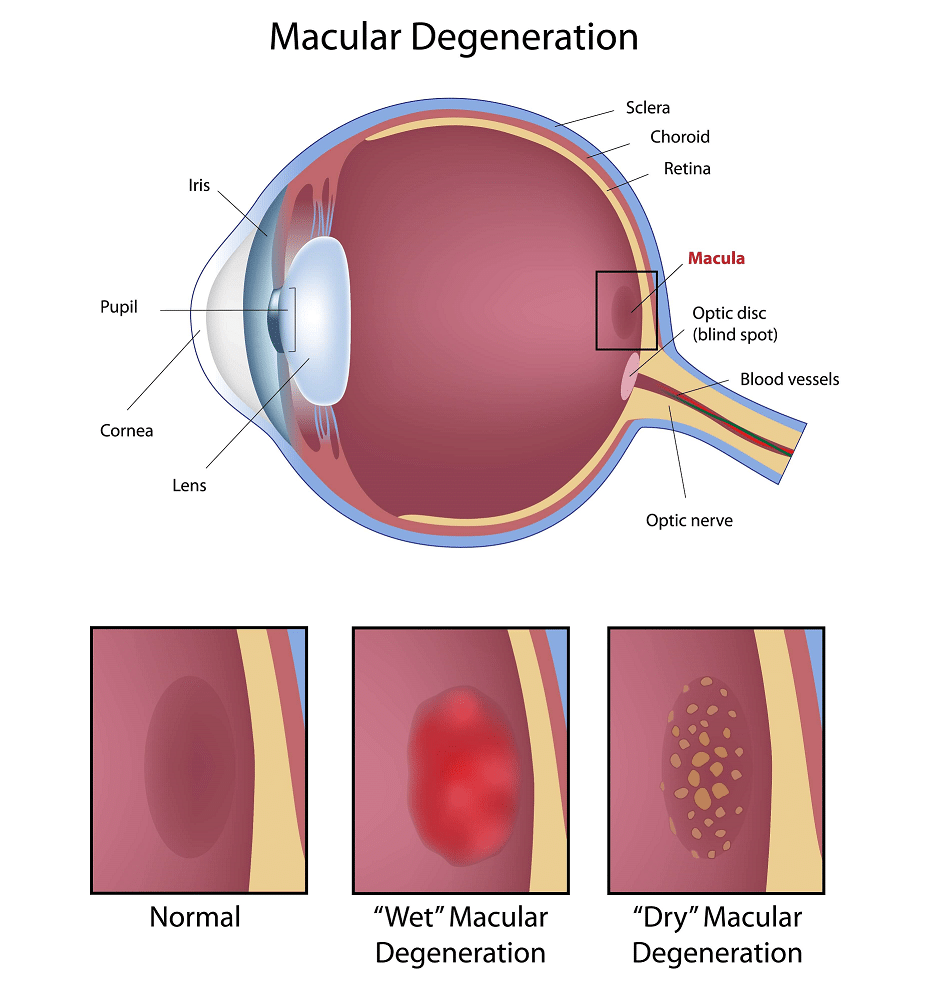
Dry macular degeneration
Dry macular degeneration, also known as non-neovascular or atrophic AMD, is the more common form of macular degeneration. It occurs when yellow deposits called drusen accumulate under the macula, causing it to thin and dry out. This results in a gradual loss of central vision over time. Dry macular degeneration progresses slowly and may not cause noticeable symptoms in the early stages.
Wet macular degeneration
Wet macular degeneration, also known as neovascular AMD, is a more severe and less common form of macular degeneration. It occurs when abnormal blood vessels grow under the macula, leaking blood and fluids that damage the macula. Wet macular degeneration can cause rapid and significant vision loss. Prompt diagnosis and treatment are crucial to prevent further damage and preserve vision.
Risk Factors
Age
The risk of developing macular degeneration increases with age. AMD is most commonly seen in people over the age of 50, and the incidence significantly rises after the age of 65. As the population continues to age, the prevalence of macular degeneration is expected to rise as well.
Family history
Having a family history of macular degeneration increases the risk of developing the disease. Certain genetic variations associated with AMD can be passed down from generation to generation. It is important to be aware of your family’s eye health history and inform your eye doctor to establish personalized prevention and treatment plans.
Smoking
Smoking is a modifiable risk factor that significantly increases the likelihood of developing macular degeneration. The chemicals in cigarettes can damage the retinal cells and blood vessels, accelerating the progression of the disease. Quitting smoking not only benefits overall health but can also help protect against macular degeneration.
Obesity
Obesity has been identified as a risk factor for macular degeneration. Excess body weight and an unhealthy body mass index (BMI) can contribute to the development and progression of AMD. Maintaining a healthy weight through a balanced diet and regular exercise can help reduce the risk of macular degeneration.
Hypertension
High blood pressure, or hypertension, is associated with an increased risk of macular degeneration. Uncontrolled hypertension can damage blood vessels throughout the body, including those in the eyes. Managing blood pressure through lifestyle changes and prescribed medications is essential in preventing macular degeneration.
Gender
Although macular degeneration can affect both men and women, studies have shown that women are at a slightly higher risk of developing the disease. The reasons behind this disparity are not fully understood, but hormonal factors and differences in lifestyle choices may contribute to the increased risk among women.
Race
Race or ethnicity can also influence the risk of macular degeneration. Caucasians have a higher prevalence of the disease compared to other racial groups. However, macular degeneration can affect individuals from all racial backgrounds, and early detection and proper management are important for everyone.
High cholesterol levels
Elevated cholesterol levels have been associated with an increased risk of macular degeneration. High levels of LDL cholesterol, also known as “bad” cholesterol, can contribute to the buildup of drusen and the progression of AMD. It is important to maintain healthy cholesterol levels through a balanced diet and medication if needed.
Symptoms
Central vision distortion
One of the earliest and most common symptoms of macular degeneration is the distortion of central vision. Straight lines may appear wavy or crooked, making it difficult to read or complete tasks that require sharp central vision. This distortion can significantly impact the ability to perform everyday activities.
Difficulty reading or recognizing faces
As macular degeneration progresses, reading becomes increasingly challenging. Words may appear blurry, and it may be difficult to distinguish letters and lines of text. Recognizing faces can also become problematic, as the details and features may appear distorted or indistinct.
Decreased color perception
Macular degeneration can affect color perception, making colors appear dull or faded. It may be challenging to distinguish between shades and hues, and certain colors may be particularly difficult to identify.
Blurred or hazy vision
Blurred or hazy vision is a common symptom of macular degeneration. Objects that were once clear may appear fuzzy or out of focus. This can make it difficult to perform tasks that require sharp vision, such as driving or reading.
Difficulty adapting to low light levels
Macular degeneration can cause difficulties in adapting to changes in light levels. Moving from a brightly lit environment to a dimly lit one may take longer for the eyes to adjust, resulting in temporary vision impairment.

Diagnosis
Visual acuity test
A visual acuity test measures how well you can see at various distances. This test involves reading letters on a Snellen chart or using an electronic visual acuity tester. The results help determine the clarity of your central vision and can indicate any vision loss caused by macular degeneration.
Dilated eye exam
During a dilated eye exam, your eye doctor will administer eye drops to widen the pupils, allowing for a detailed examination of the retinal structures, including the macula. This enables the detection and evaluation of any abnormalities, such as drusen or abnormal blood vessels, associated with macular degeneration.
Fluorescein angiography
Fluorescein angiography is a diagnostic test that involves injecting a special dye called fluorescein into a vein in your arm. The dye travels through the blood vessels in the eyes, highlighting any abnormalities or leaks within the retinal blood vessels. This test helps in identifying and assessing the severity of wet macular degeneration.
Optical coherence tomography
Optical coherence tomography (OCT) uses light waves to create cross-sectional images of the retina. This non-invasive imaging test provides detailed information about the thickness and structure of the macula, allowing for the identification and monitoring of changes associated with macular degeneration.
Treatment Options
Anti-vascular endothelial growth factor (VEGF) injections
Intravitreal anti-VEGF injections have revolutionized the treatment of wet macular degeneration. These injections help reduce abnormal blood vessel growth and prevent fluid leakage. Medications like ranibizumab and aflibercept are commonly used to inhibit the action of VEGF, slowing down the progression of the disease and improving vision in many cases.
Photodynamic therapy
Photodynamic therapy (PDT) is a treatment option for some cases of wet macular degeneration. It involves the injection of a photosensitizing drug into the bloodstream followed by the targeted application of a specific wavelength of light to activate the drug and destroy abnormal blood vessels in the macula.
Laser therapy
Laser therapy can be used to seal or destroy abnormal blood vessels in wet macular degeneration. The laser is targeted at the leaky blood vessels to prevent further damage to the macula. While laser therapy may not restore lost vision, it can help stabilize the condition and prevent further vision loss.
Vitamin supplements
Certain vitamin supplements, known as the AREDS and AREDS2 formulas, have shown promise in slowing the progression of dry macular degeneration. These supplements contain high doses of antioxidants and vitamins, including vitamins C and E, zinc, copper, and lutein. It is important to consult with a healthcare professional before starting any new supplements.

Prevention Strategies
Eat a healthy diet
Maintaining a healthy diet can help reduce the risk of macular degeneration. Include plenty of fruits, vegetables, and whole grains in your meals, as well as foods rich in omega-3 fatty acids, such as fish. Limit the consumption of saturated fats, processed foods, and foods high in cholesterol.
Protect your eyes from sunlight
Excessive exposure to ultraviolet (UV) radiation from the sun can increase the risk of macular degeneration. Wear sunglasses with UV protection and wide-brimmed hats when outdoors, especially during peak daylight hours. This helps to shield your eyes from harmful UV rays and reduces the risk of developing eye-related conditions.
Exercise regularly
Regular exercise is beneficial for overall health, including eye health. Engaging in physical activity helps maintain a healthy weight, promotes good blood circulation, and reduces the risk of developing conditions like hypertension and diabetes, which can contribute to macular degeneration.
Don’t smoke
Since smoking is a significant risk factor for macular degeneration, quitting smoking is essential in protecting your eyes. Seek support from healthcare professionals, join smoking cessation programs, and explore various strategies to help you quit tobacco use for good.
Manage chronic conditions
Conditions like hypertension, high cholesterol, and diabetes can increase the risk of macular degeneration. It is important to manage these chronic conditions through regular medical check-ups, proper medication, and lifestyle modifications prescribed by healthcare professionals.
Support and Coping Strategies
Vision aids and assistive devices
Visual aids and assistive devices can help individuals with macular degeneration maintain independence and perform daily tasks. Magnifying glasses, telescopic lenses, and electronic magnifiers can assist with reading, while smartphones and tablets with accessibility features can provide enlarged text and audio assistance.
Low vision rehabilitation
Low vision rehabilitation programs offer specialized support and rehabilitation services to individuals with vision loss. These programs may include vision assessments, counseling, mobility training, and assistive device training. Occupational therapists and optometrists often work together to create personalized rehabilitation plans.
Support groups and counseling
Joining support groups or seeking counseling services can provide emotional support and assistance in coping with the challenges of macular degeneration. Sharing experiences with others facing similar hardships can help reduce feelings of isolation and provide valuable insights and strategies for managing the condition.
Adjustment and coping techniques
Learning and practicing adjustment and coping techniques can improve the quality of life for individuals with macular degeneration. Strategies such as task modification, improving lighting conditions, and using contrasting colors can help overcome visual challenges and adapt to changes in everyday life.
Impact on Daily Life
Loss of central vision
Macular degeneration primarily affects central vision, making it difficult to perform tasks that require clear and sharp vision, such as reading, driving, and recognizing faces. The loss of central vision can significantly impact daily activities and overall independence.
Reduced ability to perform daily tasks
As macular degeneration progresses, simple daily tasks like cooking, cleaning, and personal grooming can become more challenging. The need for assistance or the use of adaptive strategies and tools may become necessary to maintain independence.
Dependence on others
The progression of macular degeneration can lead to increasing reliance on others for essential tasks. In some cases, individuals may require help with transportation, reading, and other activities that were once easily done independently.
Emotional impact
Macular degeneration can have a profound emotional impact on individuals. The loss of vision and the challenges associated with the condition can lead to feelings of frustration, sadness, and anxiety. Seeking emotional support, counseling, or joining support groups can help manage these emotions and promote overall well-being.
Research and Future Directions
Stem cell therapy
Stem cell therapy holds promise for the treatment of macular degeneration. Researchers are exploring the potential of using stem cells to regenerate damaged retinal tissue and restore vision. While still in the experimental stage, stem cell therapy could potentially revolutionize the treatment options for macular degeneration in the future.
Gene therapy
Gene therapy aims to correct genetic mutations that contribute to macular degeneration. Scientists are investigating ways to deliver therapeutic genes into the retina to prevent or slow down the progression of the disease. While gene therapy is still in its early stages, it offers hope for individuals with certain genetic forms of macular degeneration.
Artificial retinas
The development of artificial retinas, also known as retinal prostheses, offers immense hope for individuals with advanced macular degeneration. These devices bypass the damaged cells and directly stimulate the remaining healthy retinal cells to restore vision. Ongoing research is focused on improving the effectiveness and accessibility of artificial retinas.
In conclusion, understanding the causes, types, risk factors, symptoms, diagnosis, treatment options, prevention strategies, support, and coping strategies, as well as the impact on daily life, can help individuals recognize the signs of macular degeneration, seek early diagnosis, and adopt appropriate management strategies. While there is currently no cure for macular degeneration, advancements in research and technology offer hope for improved treatment and better quality of life for those affected by this condition. Taking proactive steps to maintain overall eye health, adopting a healthy lifestyle, and staying informed about the latest developments in macular degeneration can contribute to better visual outcomes and overall well-being.